The aesthetically acceptable replacement of natural teeth is dependent on a variety of factors. Of critical importance is the natural appearance of the soft tissues. Patients desire for natural-appearing tooth replacements has prompted the development of various techniques designed to achieve a natural appearance of the soft tissues.1 Specifically, use of the ovate pontic2 is among the most versatile and effective means for obtaining the desired results.
 |
 |
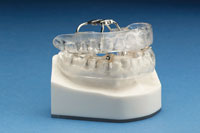
| Figures 1a and 1b. Ovate pontic design (arrow indicates the root form of the pontic.) |
The ovate pontic design refers to a prosthesis with an anatomically shaped clinical crown in which a root form profile is incorporated (Figure 1a and 1b). This configuration (in both the provisional and final restorations) promotes and maintains the development of aesthetically correct soft tissues after an extraction, implant placement, and in preparation of a long edentulous ridge prior to implant or partial denture placement.3 This versatility makes the concept of the ovate pontic an extremely useful tool in achieving proper gingival form. This is achieved by appropriate management of tissue maturation.
Since it was first detailed in 1933, the ovate pontic concept has been successfully used in conjunction with fixed and removable partial denture treatment as well as with implant placement.4-6 Although some have questioned its viability,7 histological study has not revealed any clinically significant problems with this design when appropriate oral hygiene is maintained.8 This article will discuss patient evaluation and clinical techniques for ovate pontics.
EVALUATION AND REQUIREMENTS FOR SUCCESSFUL TREATMENT
Certain factors must be carefully considered when attempting to use the ovate pontic technique. The dimensions of the soft tissues, atraumatic oral surgery (when applicable), and ridge preservation or enhancement techniques are essential. Use of functionally suitable and aesthetically acceptable provisional restorations, such as transitional fixed or removable partial dentures, is also important.
When a single tooth requires extraction, the proximal contacts of the provisional prosthesis (whether fixed or removable) should be positioned immediately above the interproximal papillae of the adjacent natural teeth to promote retention of gingival form. This will also help to limit loss of tissue, which can cause the appearance of dark interdental areas (black triangles). The gingival form developed during tissue maturation in the area of the ovate pontic would degenerate quickly without an adequate scaffold of supporting tissue. If the measurement from the superior aspect of the adjacent interproximal papillae to the crest of the underlying crestal bone at the extraction site reveals a distance of more than 5 mm, collapse of the soft tissue will occur. This will not be influenced by the location of the interproximal contacts. This measurement can be established with a periodontal probe under local anesthesia through a process called sounding.9 In these cases, thick and flat gingiva is more favorable than thin and scalloped tissue. The former is less prone to recession.10 Clearly, if periodontitis and bone loss are present about the tooth to be extracted or adjacent teeth, chances for success are compromised.
An atraumatic extraction technique is also critical to achieve the ideal outcome. Laceration or piercing of the gingival margin in the area of the extraction site may compromise healing and result in unacceptable discrepancies in tissue contours following healing. Traumatic loss of alveolar bone during tooth removal can also result in aesthetic failure, as support of the soft tissues is contingent upon the integrity of the underlying crestal bone. Gingival tissue will collapse into any flaw or defect on the buccal or facial walls of an extraction site. Even if the periodontal tissues at an extraction site remain essentially intact as a result of an atraumatic extraction, extensive remodeling of the alveolus (with a concomitant reduction in volume) can be anticipated with healing unless steps are taken to control this undesirable outcome.
A bone grafting procedure known as ridge preservation11 can help to preserve the underlying alveolar form in the area of the ovate pontic. This procedure obturates the socket after the extraction and removal of granulomatous tissue. Different types of graft materials can be used. Particulate synthetic bone, bioactive glass, demineralized bone allograft, as well as polylactide and polyglycolide fillers are among the materials that have been used for this purpose.12-14 Chairside, with the exception of the fillers, such materials are transferred from their vials into a sterile vessel, saturated with a sterile solution (such as saline or even local anesthetic), and then loaded into the extraction site (eg, using an amalgam carrier). Polylactide and polyglycolide sponges do not require the latter steps for placement. The socket should be filled to the level of the crestal bone with the graft material. A barrier membrane may also be required.15 This material will buttress the extraction site and appreciably reduce the amount of alveolar resorption that may subsequently occur. Such steps help sustain the osseous profile necessary to support the soft tissue that will, in turn, frame the final restoration in an aesthetically desirable fashion.
OVATE PONTIC TECHNIQUE
The site is now ready to accept an ovate pontic as either a fixed or removable provisional prosthesis prior to fabrication of the final restoration, or a removable partial denture when a denture tooth is being immediately added to the prosthesis to replace an extracted tooth. A fixed or removable provisional with ovate pontic design could be used in anticipation of a fixed prosthesis (ie, an implant and crown or a fixed partial denture).
For example, a provisional fixed partial denture with an ovate pontic could be inserted after a hopeless tooth has been extracted, ridge preservation has been performed, and the adjacent teeth have been prepared as abutments. The ovate pontic that is in the position of the extracted tooth contacts the graft material that has been placed within the socket, displacing a portion of the graft. The footprint of the ovate pontic should be slightly larger than the socket opening after the extraction in order to stabilize the wound and help retain the graft material in place. The displacement of the graft material corresponding to the apical aspect of the ovate pontic will aid in the development of appropriate tissue form. After healing and tissue maturation is complete, a final fixed partial denture can be fabricated, with the pontic corresponding to the gingival form that has been created. This will also maintain the natural emergence profile at the site of the extracted tooth.
 |
| Figure 2. A Monodont Bridge in the area being developed for an ovate pontic. |
 |
| Figure 3. The final implant-retained crown. Tissue maturation is complete. |
 |
| Figure 4. An acrylic transitional removable partial denture, also called a flipper, replacing tooth No. 9. |
In implant cases, either a fixed or removable provisional prosthesis may be used. The former may be a single-unit provisional fixed partial denture, and the Monodont Bridge (Eastflex Corp) system can be utilized. This system resembles a Maryland bridge in function (Figures 2 and 3). Alternatively, an acrylic transitional removable partial denture commonly called a flipper (Figure 4), or a retainer-like device called an Essix appliance, can be employed.16 Most patients prefer a fixed provisional prosthesis.
In instances where a natural tooth has been extracted and a denture tooth is being added to an existing removable cast partial denture, the sequence is much the same.6
 |
 |
| Figure 5. After tooth extraction (No. 5), the removable partial in place with an ovate pontic. | Figure 6. The tissue contour of the same patient one week after extraction. |
After the area has been evaluated and either found to be adequate or require correction, the tooth in question is removed atraumatically and ridge preservation is performed. The final removable partial denture, with the ovate pontic denture tooth added, is immediately inserted. The properly formed tissue is observable at placement, and over time, for the restoration (Figures 5 and 6).
It is important to inform patients that they should not remove the prosthesis for 3 consecutive days and nights after tooth removal, so the prosthesis can act as a wound dressing. After that time, the restoration should only be removed for oral hygiene and at night for sleeping. In the authors experience, keeping the removable partial denture (whether provisional or final) in the mouth for the first 72 hours after tooth extraction is essential both to maintain the ridge preservation material within the socket and to form the desired profile in the healing gingival tissue. Thereafter, failure to use the prosthesis for any significant period of time (other than during the night) carries a high risk of losing the developed form.
In cases involving replacement of multiple, contiguous teeth that require extraction, a somewhat different approach is required. First and foremost, the residual osseous crest must be evaluated. If ridge preservation was not performed, or the teeth were not removed atraumatically, extensive osseous defects may be present, and the remaining edentulous ridge may be inadequate to allow the use of ovate pontics. In these cases, ridge augmentation procedures must be performed before the ovate pontics are employed. Several techniques are available to accomplish this augmentation, with guided bone regeneration and distraction osteogenesis chief among them.17,18
 |
| Figure 7. Implant crowns in the Nos. 29 and 30 positions. |
As discussed previously, sounding is an important step when a single tooth is to be replaced. When multiple missing teeth are involved, typical papillary form will only be present for the teeth framing the edentulous space, and sounding will only be needed in these areas. In posterior regions of the mouth where aesthetic considerations are not critical, natural papillary contours are not essential (Figure 7).
To foster the generation of soft-tissue contours that are natural in appearance, careful execution of the flap procedure or use of the so-called punch technique19 (when sufficient attached gingiva is either present or added) is critical if ovate pontics are to be used. The punch technique is preferable in cases where the treatment plan calls for partial dentures (fixed or removable). The punch technique is a procedure whereby a tissue punch is used (without raising a full thickness flap) to core the tissue over an edentulous ridge. Such a site would also be produced in an implant case when a flap procedure is used during placement, with the choice of these 2 methods of entry being determined by the implant surgeon. Establishment of ovate pontic sites on a long edentulous ridge should only be undertaken after any corrective regenerative procedures have healed (in the case of partial denture placement), or when grafting is contemplated at the time of implant placement (as may be a consideration in some cases with extremely porous bone at the surgical site).
Once the hard and soft tissues of the edentulous ridge have been assessed and modified as needed, and an ovate pontic site has been created, the provisional prosthesis can be inserted. Again, after the soft tissue has matured, final partial dentures with pontics or denture teeth with an ovate pontic design can be inserted, and implants can be restored with crowns mimicking the contours of natural crowns. All these clinical restorations will maintain the soft tissue.
DISCUSSION
Use of ovate pontics with fixed or removable partial dentures does require that patients exercise special care with oral hygiene and other oral functions. As noted, it is important that patients with removable partial dentures use these appliances consistently to preserve the soft-tissue contours that have been developed. Home care for fixed partial dentures demands that cleansing of the pontic area is accomplished without trauma, ie, flossing should not traumatize or disrupt the soft tissues. There may be some differences on a histological level between the mucosal surface under an ovate pontic and the mucosa under a ridge lap or sanitary pontic associated with a fixed partial denture. Nevertheless, these differences are not clinically significant and have no bearing on whether or not to create an ovate pontic when periodontal conditions are otherwise normal.8
CONCLUSION
In the past, the clinical crowns or pontics of the primary types of prosthetic devices were aesthetically acceptable, but the supporting soft-tissue architecture often was not. Patients have now come to expect that implant crowns, the pontics associated with a fixed partial denture, and even the denture teeth of removable prostheses will demonstrate emergence angles and soft-tissue profiles that match those associated with natural teeth. The ovate pontic method, when properly performed, will fulfill these expectations in a simple and predictable manner.
References
1. Langer L. Enhancing cosmetics through regenerative periodontal procedures. Compend Suppl. 1994;(18):S699-S705.
2. Miller MB. Ovate pontics: the natural tooth replacement. Pract Periodontics Aesthet Dent. 1996;8:140.
3. Kinsel RP, Lamb RE. Development of gingival esthetics in the edentulous patient prior to dental implant placement using a flangeless removable prosthesis: a case report. Int J Oral Maxillofac Implants. 2002;17:866-872.
4. Dylina TJ. Contour determination for ovate pontics. J Prosthet Dent. 1999;82:136-142.
5. Kois JC, Kan JY. Predictable peri-implant gingival aesthetics: surgical and prosthodontic rationales. Pract Proced Aesthet Dent. 2001;13:691-698.
6. McArdle BF. Enhancing the esthetics of teeth added to cast partial dentures. Contemp Esthet Restor Pract. 2003;7(8):44-48.
7. Johnson GK, Leary JM. Pontic design and localized ridge augmentation in fixed partial denture design [published correction appears in Dent Clin North Am. 1993;37(1):vii]. Dent Clin North Am. 1992;36:591-605.
8. Zitzmann NU, Marinello CP, Berglundh T. The ovate pontic design: a histologic observation in humans. J Prosthet Dent. 2002;88:375-380.
9. Greenberg J, Laster L, Listgarten MA. Transgingival probing as a potential estimator of alveolar bone level. J Periodontol. 1976;47:514-517.
10. Sanavi F, Weisgold AS, Rose LF. Biologic width and its relation to periodontal biotypes. J Esthet Dent. 1998;10:157-163.
11. Ashman A. Postextraction ridge preservation using a synthetic alloplast. Implant Dent. 2000;9:168-176.
12. Murray VK. Anterior ridge preservation and augmentation using a synthetic osseous replacement graft. Compend Contin Educ Dent. 1998;19:69-78.
13. Serino G, Biancu S, Iezzi G, et al. Ridge preservation following tooth extraction using a polylactide and polyglycolide sponge as space filler: a clinical and histological study in humans. Clin Oral Implants Res. 2003;14:651-658.
14. Froum S, Cho SC, Rosenberg E, et al. Histological comparison of healing extraction sockets implanted with bioactive glass or demineralized freeze-dried bone allograft: a pilot study. J Periodontol. 2002;73:94-102.
15. Bartee BK. Extraction site reconstruction for alveolar ridge preservation. Part 2: membrane-assisted surgical technique. J Oral Implantol. 2001;27:194-197.
16. Moskowitz EM, Sheridan JJ, Celenza F Jr, et al. Essix appliances. Provisional anterior prosthesis for pre and post implant patients. N Y State Dent J. 1997;63(4):32-35.
17. Fugazzotto PA. Guided bone regeneration for enhanced esthetics: edentulous ridge contours beneath pontics and hard tissue repair of postoperative ridge defects. J Esthet Dent. 1994;6:103-108.
18. Papageorge MB. Distraction osteogenesis for augmentation of the deficient alveolar ridge. J Mass Dent Soc. 2002;51(1):24-30, 51.
19. Auty C, Siddiqui A. Punch technique for preservation of interdental papillae at nonsubmerged implant placement. Implant Dent. 1999;8:160-166.
Dr. McArdle graduated from Tufts University School of Dental Medicine in 1985 and has been practicing general dentistry on the New Hampshire seacoast ever since. He has served on the active medical staff in dentistry of Concord Hospital in Concord, NH, and on the board of directors of Priority Dental Health, Inc (prioritydental.com), the New Hampshire Dental Society’s Direct Reimbursement entity. He currently serves on the editorial committee of The Granite State Dentist, the newsletter of the New Hampshire Dental Society, and is a co-founder of the Seacoast Esthetic Dentistry Association (SEDA) (dentalesthetics.org). Dr. McArdle
(mcardledmd.com) can be reached at (603) 430-1010, drmcardle@mcardledmd.com, seda@dentalesthetics.org, or drmcardle@digitaldental.net.