As practicing dentists, we are continually bombarded with a plethora of decisions to make. These decisions can range from the simple and easy (Do I want to attend the local dental society’s evening dinner meeting next week?) to the complex, difficult, and time-consuming (Is it time to add some major new technology or equipment to the office?) Many times just the thought of making a major decision is so daunting that it is easier to procrastinate or ignore it and hope that it will go away. The decision may go away for awhile, but the consequences will not. The sheer quantity of choices, added to the fear of making a bad decision, often prevents us from making any decision at all, often with financial or professional consequences.
When making decisions that impact my practice, I use a flow chart I have developed that gives me the clarity, confidence, and guidance to make a wise choice, be it very minor or very complex and major. It starts with the most important question: What will the impact be on patient care…how will the decision to add this new technology, material, technique, or system affect the patients on a day-to-day basis in the practice? As healthcare professionals, our primary consideration should always center on patient care, safety, and benefit.
 |
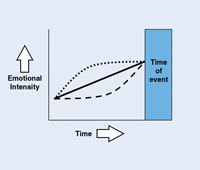
When taking the patient into consideration, the result of the decision can only be one of 3 possibilities: positive, neutral, or negative (Chart). Let’s use the example of deciding to shorten all recare visits to no more than 20 minutes, even for periodontal patients. When the implications for the patient are analyzed, it is obvious that many patients would be shortchanged and would receive inadequate or incomplete treatment. It may be good for the bottom line of the practice, but with the benefit to the patient being the overriding factor, the decision is easy: stop. If the decision you are trying to make does not benefit the patient, then you should go no further.
If the result of the decision would be positive for the patient, such as using a stronger cement to cement crowns and bridges, or neutral for the patient, such as using a different color patient bib, we take one step further down the decision tree and look at the effect the decision would have on the practice. As noted previously, there can be only one of 3 options: positive, neutral, or negative.
Once it is determined that the new, stronger cement is good for the patient, determine the effect on the practice. Will it take more time to use or less? Is it encapsulated to minimize the potential for mixing errors and ensure better properties? Does it cost more or less than the present cement? If the determination is that it is positive for the practice (faster, cheaper, easier to use), then the decision again is an easy, absolute yes. If it is neutral for the practice (no difference in cost or procedure) but still beneficial for the patient (stronger), then the answer again is yes; implement the decision. If it is negative for the health of the practice, but positive for the patient, then continue to evaluate the cost/benefit ratio to reach a final decision.
When the decision is a non-issue for the patient (the color or brand of the patient bib), then the effects on the practice take full priority in the decision-making process. If it is cheaper or more convenient for the practice, then make the decision to change. If it is more costly, then don’t. If the cost is the same, then it does not matter. Do not agonize over it.
With these examples, it should now be easy to start at the top of the decision tree, follow the flow down, and come to a quick, confident, and rational decision. This framework will work with decisions of any complexity, will simplify your life, and will help you make better decisions and be more in control of your practice and your life.
It is obvious how this works when the decisions seem relatively minor. How does it work with very large, important decisions that will have a tremendous impact on your practice profitability and growth, as well as your satisfaction with your career choice of being a clinical dentist? Let’s take digital radiography, a very hot topic in dentistry today, and follow it through the decision tree to see if it works.
The first consideration again is the patient. How would the decision to add digital radiography to the practice affect the patient? Will it be a good thing for the patient, neutral for the patient, or even bad for the patient? The first step is to gather and analyze this type of data.
From the information presently available, we know that digital radiography requires less radiation than most film-based methods. It also requires less time to acquire because it eliminates the processing steps, resulting in less chair time for patients, which they appreciate. The radiographs are more diagnostic because they are viewed in a much larger size on a computer monitor, and computer enhancements allow for different positions to aid in analysis and diagnosis. The size also now enables the patients actually to see what the dentist sees on the x-rays, which promotes understanding of the problems and ultimately treatment acceptance. The above attributes certainly add up to moving to the positive benefits for the patient on the decision tree.
The next step is to look at how the addition of digital radiography will affect the practice. Again, this can be positive, negative, or neutral. The effects on the dental practice are also easy to glean from the many articles written on digital radiography and by questioning those dentists who are presently using it. The first benefit is the better diagnostic information that is available from the digital radiographs, once more because of their larger viewing size and computer enhancements. These allow manipulation, which enables the dentist to focus on different considerations and locations, such as periodontal views, endodontic PA views, and DEJ operative views. Better diagnosis can lead to earlier and more complete treatment. In addition, Kodak Dental Systems has an analytical way (the Logicon Software system) to examine radiographs for caries, which adds confidence, clarity, and credibility for the dentist and the patient.
The next benefit for the practice is the time saved by using digital radiography. The image is captured and filed in the patient’s chart within 2 to 3 seconds. Contrast this to the several minutes it takes to reach the same point in traditional, film-based radiography, and the amount of time saved is enormous. This translates into enabling the hygienists to see an additional patient each day, and even more time saved with endodontic and emergency patients for the doctor. Often the time savings alone will more than pay for the system.
Another benefit is the cost savings of no longer having to buy and inventory film, mounts, and processing chemicals. There are no more smelly and toxic chemicals to work with. Compare the number of films taken every month with what a monthly payment would be for purchasing a digital radiographic system and analyze the savings for the practice.
Once it is obvious that the decision to purchase digital radiography is beneficial for the patient and the practice, the only logical choice is to make the decision to proceed and make it a reality in your practice.
CONCLUSION
The process described in this article also works if you put it through the practice first, and then the patient. The result should be the same. I choose to put it through the patient consideration first, so I am not tempted to do something strictly because it is good for the practice.
Dr. Dykstra started his solo dental practice in 1978 in Hudsonville, a small town in western Michigan. His original office was expanded 3 times, and in 1994 he built his dream office with just more than 3,800 square feet of working room. Dr. Dykstra’s practice is in the top tier of production and collection of dental practices in the United States. He went paperless in the fall of 2002 and has successfully incorporated total electronic records with digital clinical charting, digital radiography, digital intraoral and extraoral photography, and digital imaging. He added a laser to his practice in 2003. In addition to working full time in his practice, he does speaking and consulting work through Anchor Dental Consulting, which he founded to help dentists successfully integrate technology into the dental office. He can be reached at
info@anchordentalconsulting.com.
Disclosure: Dr. Dykstra receives an honorarium from the Kodak Company when lecturing on digital radiography.