Acute pain is the most common complaint that causes patients to seek help from healthcare professionals. Pain management remains an important consideration in dental care and patient management. Although utilized for acute pain control, analgesics provide significant anti-inflammatory effects. Anti-inflammatory analgesics are available both over-the-counter (OTC) and by prescription. Since analgesics are widely used in dentistry and by patients for other medical indications, the dentist should be knowledgeable in their pharmacology. This article thoroughly reviews these drugs including mechanisms of action, indications, dosage regimens, and drug interactions. A suggested pain management plan is provided.
DEFINING PAIN
Pain, as defined by the International Association for the Study of Pain, is “an unpleasant sensory and emotional experience associated with actual or potential tissue damage or described in terms of such damage.”1
Pain is not a single entity; it is part of the entire inflammatory process and one of the clinical signs of inflammation. Pain can be described as (1) acute, (2) chronic and associated with malignant disease, or (3) chronic and not associated with malignant disease. The duration of acute pain is usually hours to days, while chronic pain can last months to years and have associated problems of depression and anxiety.
UNDERSTANDING ACUTE PAIN
Oral pain is associated with pulpitis, periodontitis, pericoronitis, abscesses (endodontic/periodontal), trauma, and other conditions including temporomandibular disorders (TMDs) and masticatory muscle disorders. Dental procedures also can have pain as a sequela with more invasive procedures increasing this likelihood. Pain is provoked when a variety of inflammatory mediators such as bradykinin, histamine, leukotrienes, and prostaglandin E2 are released into the tissues. These pain-inducing substances can be produced and released from cell membranes by trauma (eg, mechanical trauma to the soft tissues and bone during periodontal surgery), infection, and allergenic reactions. Therefore, part of the successful management of pain requires blocking or managing the development of inflammation.
ACUTE PAIN MANAGEMENT
The majority of dental pain is an acute response to inflammation. The acute pain associated with dental trauma, infection, or surgery is usually predictably managed pharmacologically. The key to pharmacologically managing pain is to provide a sufficient dose of a particular drug to minimize pain onset and give the patient comfort. The drug should be administered frequently to prevent the pain from becoming severe. The most effective way to maintain analgesia is to administer doses on a regularly scheduled basis for a specified period after the trauma. For example, after periodontal surgery, inflammation and pain usually peak 48 hours later. Thus, postoperative analgesic medication can be administered on a regular schedule, depending on the half-life of the drug (eg, every 4 hours), for 48 hours, then given as necessary (prn).
CLASSIFICATION OF ANALGESICS
Analgesics are classified as antipyretic analgesics, nonselective nonsteroidal anti-inflammatory drugs (NSAIDs), cyclooxygenase-2 (COX-2) selective NSAIDs, and opioids.
Antipyretics
Acetaminophen is an antipyretic analgesic with no real attributable anti-inflammatory effect. Its mode of action has never been totally determined. It is provided as an oral or rectal dose form. Although acetaminophen is eliminated through the kidneys, part of the therapeutic dose is broken down in the liver. However, doses in the excessive range of 10 g can cause hepatic damage. Also, consumption of alcohol and acetaminophen can cause liver damage. Overdosing is not difficult, as the patient may not be cognizant that other OTC products contain acetaminophen. The maximum recommended dose is 2 to 4 g daily.
Acetylsalicylic acid (ASA) or aspirin in doses of more than 4 g/d can provide an anti-inflammatory effect. Nevertheless, it is usually administered for its antipyretic and analgesic actions. These actions are a consequence of ASA’s irreversible inhibition of cyclooxygenases through covalent binding of the acetyl residue. Although all NSAIDs have a structure related to ASA, their inhibition of cyclooxygenase is reversible.
Therefore, ASA will have a more profound effect on platelet function inhibiting aggregation and prolonging bleeding time. This, combined with gastric mucosal irritation as a result of the inhibition of prostaglandin synthesis, often contraindicates ASA after many intraoral surgical procedures.
Nonselective NSAIDs
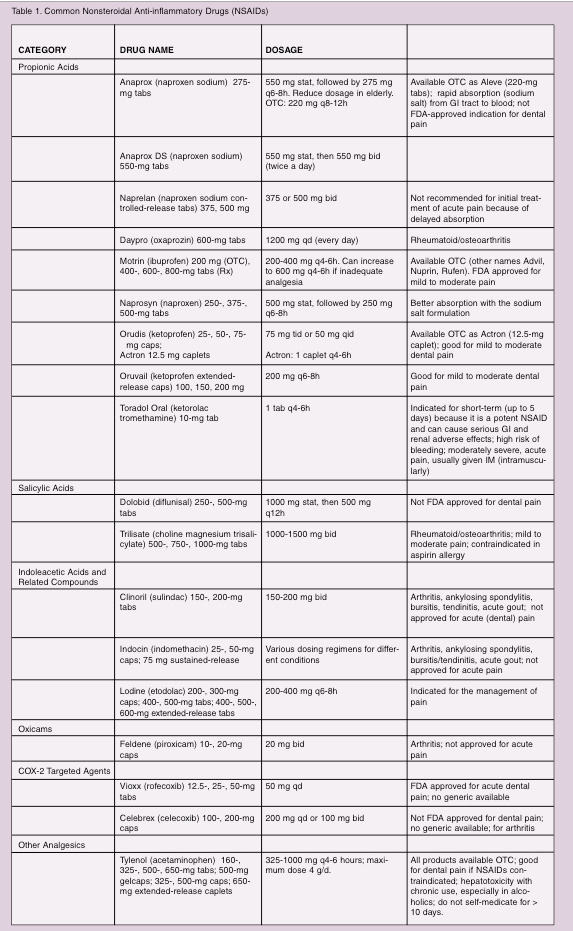
The nonselective NSAIDs (Table 1) have been utilized as analgesics for the treatment of both acute and chronic pain since the 19th century. All nonselective NSAIDs have the same mechanism of action and similar pharmacokinetics. The decision regarding which one to use depends on the convenience of the dosing regimen, adverse or undesired side effects, the patient’s clinical needs, previous experience with the drug, and cost. Some NSAIDs are more potent, have specific indications, or have improved adverse side-effect profiles. Patients who do not respond with one type of NSAID may respond to another. NSAIDs provide anti-inflammatory, analgesic, and antipyretic properties. FDA indications include acute (mild to moderate) pain (including dental), chronic pain (osteoarthritis or rheumatoid arthritis), ankylosing spondylitis, bursitis/tendinitis, and menstrual pain. Dental pain is not an FDA-approved indication for all NSAIDs.
 |
The analgesic potency of a NSAID is largely related to its ability to inhibit prostaglandin synthesis. NSAIDs block prostaglandin production by the inhibition of the COX enzyme in the arachidonic acid pathway. Two forms of COX have been identified. The constitutive form (COX-1), which is present in most tissues, including the gastrointestinal (GI) tract, kidneys, and platelets, plays a protective role in these organs. The inducible form (COX-2) is found in small amounts in inflammatory cells (macrophages), endothelial cells, synovial cells, and chondrocytes (unless an inflammatory process is occurring).2 Inhibition of COX-2 in these tissues is probably responsible for the anti-inflammatory effects of NSAIDs. Each NSAID inhibits COX-1 and COX-2 to varying degrees. The inhibition of COX-1 causes undesirable effects including gastric complications, depression of renal function, and inhibition of platelet aggregation. This inhibition of platelet aggregation is dose/drug dependent. Aspirin and nonselective NSAIDs exert their antiplatelet effect by inhibiting COX which blocks the formation of thromboxane A2. When a NSAID comes into contact with the platelet cell membrane, it binds to and inhibits the release of COX, thereby altering platelet function. The antiplatelet effect of aspirin is irreversible, lasting for the half-life of the platelet (approximately 7 days). However, NSAID derivatives reversibly bind to the platelet membrane causing a transitory antiplatelet effect. Recovery of platelet function may occur within 1 to 4 days after discontinuation of the drug.
COX-2 NSAIDs
The most recent advances in NSAIDs have been the development of selective COX-2 inhibitors. An advantage of these NSAIDs is a more favorable GI, renal, and platelet side-effect profile. Rofecoxib (Vioxx) is FDA approved for acute pain (including dental pain) in adults, primary dysmenorrhea, and osteoarthritis.3 Celecoxib (Celebrex) is only FDA approved for the long-term treatment of osteoarthritis and rheumatoid arthritis and not for acute dental pain. Thus, rofecoxib is a good choice for patients with prior or present GI problems.
ADVERSE SIDE EFFECTS/CONTRAINDICATIONS TO NSAID USE
Because serious GI effects have been associated with nonselective COX inhibitors, these medications should be avoided in patients who present with a history of peptic ulcer disease or GI bleeding. Additionally, all NSAIDs are highly protein-bound and have the potential to displace coumadin and potentiate its anticoagulant effect.
NSAIDs, including COX-2 inhibitors, are contraindicated in patients who have experienced bronchospasms, angioedema, and allergic reactions to aspirin. Since NSAIDs do not cross the blood-brain barrier, sedation is not a side effect.
A number of drug/drug interactions caused by NSAIDS have been documented.4 Consumption of antacids may decrease the absorption of NSAIDs. The concurrent use of cortico-steroids may increase the risk for NSAID-induced gastropathy. The actions of lithium when taken with NSAIDs may be increased due to decreased renal clearance of the drug. The effects of oral hypoglycemic agents and phenytoin may be increased due to the high protein binding of NSAIDs. NSAIDs may cause fluid retention and therefore increase the potential to exacerbate congestive heart failure. Additionally, these agents may elevate blood pressure or reduce the effects of antihypertensive drugs.5 Renal function should be monitored in patients who take both a NSAID and a diuretic or angiotensin-converting enzyme inhibitor [eg, enalapril (Vasotec), lisinopril (Zestril)].5
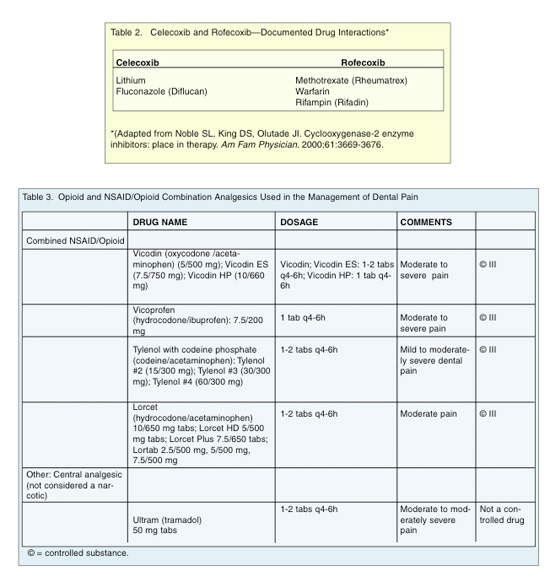
Because celecoxib is metabolized by the enzyme cytochrome P450-2C9 in the liver, drugs that inhibit cytochrome P450-2C9 have the potential to increase serum concentrations of celecoxib. The hepatic cytochrome P450 system has a minor role in the metabolism of rofecoxib. Rofecoxib is not recommended for use in patients with moderate to severe hepatic damage. Celecoxib is not recommended in patients with severe hepatic damage. Generally, no dosage adjustments are needed in the elderly, however, they are not recommended for use in patients younger than 18 years of age. Known drug interactions for celecoxib and rofecoxib are listed in Table 2.6
OPIOID ANALGESICS
For moderate pain that is not relieved by NSAIDs, opioid analgesics are generally the agents of choice. Opioids alter the patient’s perception of the pain in the brain. Both endogenous opioids (enkephalins, endorphins) and the exogenous opioids (morphine) bind to and activate receptors in the brain. There are three opioid receptors belonging to the group of G-protein coupled receptors. Pain relief is also provided through inhibition of nociceptive impulsive transmission in the spinal medulla. Table 3 lists common opioids used in dental pain management.
The combined use of a NSAID with an opioid produces a synergistic effect so that a lower dose of opioid can be used. Opioids alone are not prescribed for the management of acute dental pain because too high a dose would be needed. The adverse side effects would not be acceptable.
Along with the analgesic effects, all opioids have similar profiles of toxic side effects, which should be considered when prescribing these medications. Respiratory depression may occur in a patient taking an opioid for the first time. Tolerance to opioids can develop over time so that regular increases in the dosage may be required in order to provide a sustained analgesic effect. However, side effects will continue to occur including constipation, sexual impairment, and nausea. Opioids can create a physical dependence and addiction, which is termed a psychological loss of control resulting in compulsive use. Opioids may cause sedation and/or drowsiness.
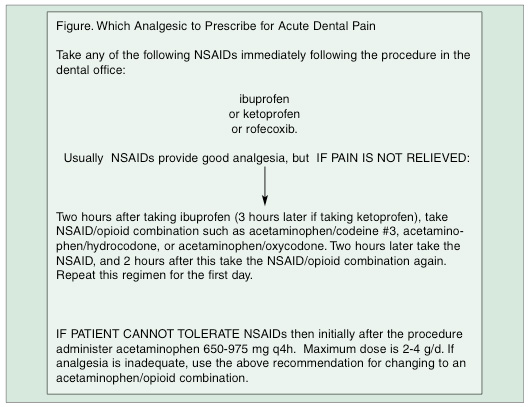
SELECTION CRITERIA: DECISION TREE FOR MANAGEMENT OF ACUTE PAIN
A decision tree (Figure) is proposed for the management of acute dental pain. Initially, a maximally effective dose of a NSAID should be prescribed, (eg, rofecoxib, ibuprofen, or acetaminophen), with the patient ingesting the loading dose in the office.
If the patient does not show improvement within a few hours either switch to another NSAID or add a combined NSAID/opioid (eg, Vicoprofen or acetaminophen with codeine phosphate). If the patient was taking acetaminophen initially, substitute the combination opioid. Adding on another more potent drug allows the second drug to be absorbed from the GI tract while the other drug is at its peak therapeutic plasma level. Thus, there is a continuous level of analgesic in the blood. Initially, nonopioid analgesics should not be prescribed “prn” because analgesics are more effective if peak therapeutic plasma levels are maintained.
There are shorter-acting (4 to 6 hours and 6 to 8 hours) analgesics (eg, ibuprofen, ketoprofen, naproxen sodium), and long-acting (half-life of 17 hours) analgesics (eg, rofecoxib). Rofecoxib has been documented to provide analgesia up to 24 hours after surgery.7 Ibuprofen plasma levels peak at 1 to 2 hours. Celecoxib plasma levels peak at 3 hours and rofecoxib peaks at 2 to 3 hours. Since the clinical differences between the nonselective NSAIDs and selective COX-2 inhibitors are small, the decision to use the more expensive COX-2 inhibitors should be based on the patient’s risk of GI tract bleeding and peptic ulcer disease.
Studies have suggested that NSAIDs may be a better choice than opioid combinations following most dental and medical outpatient surgery.8 Patients receiving NSAIDs will have fewer undesirable side effects such as nausea and somnolence. Opioid analgesics are usually not needed after outpatient surgery.9 Dosing with 600 mg ibuprofen either immediately before or immediately after periodontal surgery significantly delays the onset of pain as compared with placebo. However, studies have shown the onset of pain is delayed longer when dosing immediately postsurgically as compared with dosing presurgically for a combined 8-hour period after surgery.10 Other studies have found when ibuprofen was taken 30 minutes before the removal of impacted third molars, there was a delay in onset and diminished intensity of postoperative pain, whereas dosing immediately after surgery significantly delayed the onset of pain.11 Another advantage to dosing after an invasive procedure is to avoid the effects of inhibition of platelet aggregation.
If NSAIDs are contraindicated (eg, patients with ulcers or asthma and patients taking coumadin or antihypertensives, phenytoin, coumadin, corticosteroids, oral hypoglycemic agents, or lithium), acetaminophen can be prescribed. NSAIDs and short-acting opioids should generally be avoided for chronic daily use because of the side effects of NSAIDs and potential opioid tolerance.10 Dosage adjustment must be made in the elderly or debilitated and if there is liver or kidney disease. Use of these drugs during pregnancy and lactation must be discussed with the patient’s physician.
Instructions to the patient include taking all medications with a full glass of water, to stay upright for 15 to 30 minutes, and not to take medication at bedtime. This will minimize chances of esophageal irritation and enhance absorption in the duodenum. These medications can also be taken with a small amount of food or milk to minimize GI upset (eg, GI ulceration or bleeding). All NSAIDs have a ceiling effect, whereby administration of a higher dose than prescribed will not provide additional analgesic effects.
DISCUSSION
The management of acute dental pain due to inflammation is a common clinical problem. Effective pain management depends on an accurate diagnosis. The decision to use a NSAID or a combination NSAID/opioid depends on the severity of the pain. Opioid analgesics are controlled substances and have many adverse side effects. Thus, most acute dental pain can be managed with the proper NSAID. Although NSAIDs and short-acting opioids may be helpful in relieving acute pain, they should not be used on a daily basis for chronic pain. The chronic use of NSAIDs may be associated with significant side effects, including renal disease.
References
-
Mersky H. Pain terms: a list with definitions and notes on usage, IASP Subcommittee on Taxonomy. Pain.
-
Fu JY, Masferrer JL, Seibert K, et al. The induction and suppression of prostaglandin H2 synthase (cyclooxygenase) in human monocytes. J Biol Chem. 1990;265:16737-16740.
-
Matheson AJ, Figgitt DP. Rofecoxib: a review of its use in the management of osteoarthritis, acute pain and rheumatoid arthritis. Drugs. 2001;61:833-865.
-
Ament PW, Bertolino JG, Liszewski JL. Clinically significant drug interactions. Am Fam Physician. 2000;61:1745-1754.
-
McEboy GK, ed. AHFS Drug Information 2001. Bethesda, Md: American Society of Health-System Pharmacists; 2001.
-
Noble SL, King DS, Olutade JI. Cyclooxygenase-2 enzyme inhibitors: place in therapy. Am Fam Physician. 2000;61:3669-3676.
-
Moore PA, Hersh EV. Celecoxib and rofecoxib. The role of COX-2 inhibitors in dental practice. J Am Dent Assoc. 2001;132:451-456.
-
Agency for HealthCare Policy and Research. Acute Pain Management in Adults: Operative Procedures. Rockville, Md: Department of Health and Human Services, Agency for Health Care Policy and Research; 1992: AHCPR Publication no. 92-0019.
-
Carpenter RL. Optimizing postoperative pain management. Am Fam Physician. 1997;56:835-844, 847-850.
-
Vogel RI, Desjardins PJ, Major KVO. Comparison of presurgical and immediate postsurgical ibuprofen on postoperative periodontal pain. J Periodontol. 1992;63:914-918.
- Dionne RA, Cooper SA. Evaluation of preoperative ibuprofen for postoperative pain after removal of third molar. Oral Surg Oral Med Oral Pathol. 1978;45:851-856.
Dr. Weinberg is clinical associate professor of periodontics and director of the second-year periodontic program at New York University College of Dentistry, David B. Kriser Dental Center in New York. She is a member of the American Dental Association. Dr. Weinberg can be reached at (212) 998-9506 or maw2@nyu.edu.
Dr. Fine is presently associate professor of clinical dentistry and postdoctoral director of the Division of Periodontics at the School of Dental and Oral Surgery of Columbia University and associate attending dental surgeon on the Presbyterian Hospital Dental Service. He is a diplomate of the American Board of Periodontology. Dr. Fine has served on the Research, Science, and Therapy Committee of the American Academy of Periodontology, and has been the recipient of several teaching awards and fellowships. He has authored or coauthored numerous articles in the periodontal literature, and was an author of the text, Clinical Guide to Periodontics. He can be reached at ms14@columbia.edu.