|
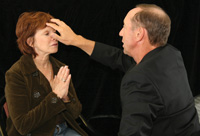
| Figure 1. Acquiring thought of event and emotional context for 30 to 40 seconds. |
Every dentist has been confronted with the challenge of the anxious or phobic patient. Recent literature describes several approaches to making these individuals more comfortable and easier to treat. Those papers focus on the anxiety itself and attempt to down-regulate the fear response. Currently, 3 approaches are routinely used to address the concerns of the patient. First are the talk therapies, such as Cognitive Behavioral Therapy.1 This approach involves an interaction and a relationship between a trained therapist and a client. Second is Systematic Desensitization/Exposure, where the individual is slowly introduced to the feared situation.2 Third, medication can be used to alter the brain’s neurochemical response to the exposure.3
This paper introduces a new therapeutic modality and suggests a neurobiological mechanism for its effectiveness. We call this Havening Therapy, as in “find a safe haven.” This approach utilizes the extrasensory aspect of touch to alter pathways that create distress.
WHAT IS A PHOBIA AND WHY DO SOME PEOPLE HAVE THEM?
A phobia (from Greek: phobos, “fear”) is generally defined as “an irrational, intense and persistent fear of certain situations, activities, things or persons.”4 Phobic anxiety is distinguishable from other forms of anxiety only in that it occurs specifically in relation to a certain object or situation. Anxiety is a physiological and psychological state characterized by cognitive, somatic, emotional and behavioral components. The physiological symptoms of fear include a rapid pounding heartbeat, widening of the eyes, pupil dilation, peripheral muscle activation and increased respiration.5 These symptoms are the observed responses to a complex neurobiological event generated within the mind of an individual.
This response, produced involuntarily by the brain, has only one objective: to flee from or defend against a fearful object or situation. These primitive responses were needed to increase muscle strength, increase blood flow and decrease the experience of pain. Over millions of years, evolution has perfected a cascade of neurochemicals such as norepinephrine, epinephrine, dopamine, and cortisol that are released into our bodies to prepare for flight or fight.6
For nonprimates, where predator and prey battle, there are 2 options: escape or die. In the primate/human species, a third option exists. Survive and not escape (abused child, traumatic dental experience). This third outcome can, for some people, become encoded as a phobia, which is one type of traumatization. Phobias are the response to a perceived encoded threat. How they form is beyond the scope of this paper, but suffice it to say that certain criteria must be met.
The most critical of these requirements is that escape is not to be perceived as possible. Without escape, there is no closure on the event. Cues and content by overlapping with the original event can reactivate feelings (ie, white coat syndrome). A stimulus that reactivates the emotional (fear) component of the traumatic event does so as if it were being experienced for the first time. This response to a previous event provides the opportunity to de-link the emotional component and find a safe haven.
| Table. Havening Sequence | |||||||||||||
|
When a nonhuman escapes a predator, the brain is flooded with serotonin.7 This primitive neurochemical allows for the brain to become calmer and inhibits a fear response, thus allowing for normative behavior. In humans, rising serotonin (meaning a safe place is found) on recall of the trauma allows for a disconnect between the emotions and memory. Thus, serotonin extinguishes the phobia.
HAVENING
Havening makes it possible to alter the response to a stimulus that would normally generate a fear response by using the extra sensory aspects of touch. It is well known that touch increases serotonin in the brain.8 Swedish massage has been shown to create physically and mentally relaxed states by increasing serotonin and dopamine. It is this connection between serotonin and touch that forms the basis for treatment.
ACTIVATION AND DISPLACEMENT OF THE PHOBIA/ANXIETY
History taking is the key to removing the unwanted traumatically encoded pathway. Early traumas set the stage for current circumstances. To start the displacement, the initial sensitizing event must be found and activated. In dental phobias, the event quite often occurs at a fairly young age. Usually the patient can give a narrative of the experience and can see quite clearly the whole context of the event. The fact that the memory is still so significant after so many years speaks to the high emotional content at the time of encoding.
PREHAVENING PROTOCOLS
If the patient cannot bring to mind a specific event, then have the patient focus on the current situation and feelings.
Have the patient bring to mind the entire circumstance involved with the memory or moment. The sights, sounds and smells should fill the subject’s mind until she approaches being in that moment. The patient’s eyes should be closed (Figure 1). The patient should also experience the emotional content of the moment. The “experience of fear” is the response to an unresolved trauma.
HAVENING PROCEDURES
Allow 30 to 40 seconds to have the patient recall and “feel” the moment with eyes closed. Request a subjective unit of distress (SUD), which is a number from zero to 10 which the patient will indicate the degree of “being in the moment.” Ten represents being right there; zero represents its disappearance. She should open her eyes and write down the number that she feels. The sequence that I find effective is found in the Table.
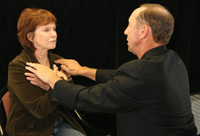
During this process I use an unmodulated, somewhat monotonous voice that is never hurried. I am always encouraging and never correcting when simple mistakes are made (Figure 2). I say, “Listen to the sound of my voice.” Additionally, phrases in the same unmodulated tone, such as, “Almost home,” and “You are excellent at this,” are interjected while other sensory components are being stimulated.
This process is called havening. It includes kinesthetic components (touch and posture) that raise serotonin, as well as the distractive elements (humming, counting, eye rolling, and so on9) that cause displacement of the thought (emotional core).
THE KINESTHETIC COMPONENT (TOUCH AND POSTURE)
The touch is meant to be comforting, soothing, gentle, supportive, and produces a dramatic surge of serotonin in the brain. Light touch is best and the movements should create a bond between the doctor and the patient. The patient should always be seated in a comfortable position. During the therapy, one can use different hand and arm positions such that it appears that the patient is either praying (Figure 3) or hugging oneself gently (Figure 4). During the havening touch component, the patient should be encouraged to allow the shoulders to drop and the jaw to become slack. This postural approach is useful for calming both the body and the mind. Light, sensitive stroking of the arms, hands, and head is the somatic aspect of the havening (Figures 5 and 6).
THE DISTRACTIVE COMPONENT
At the same time, distracting thoughts and tasks are introduced to the moment displacing the present mindset. Try it yourself. Hum “Happy Birthday” out loud and count backwards from 20 in your mind. So only one thought can exist at a time! Eye rolling, humming a tune, counting backwards by multiple numbers causes an intense focus on the task at hand and slowly displaces the originally held thought. Sit with the patient for 10 seconds with palms up and your hand on top of palms (Figure 7). Repeat the process 3 times and obtain the SUD after the third round. After 3 rounds say “when you are ready, open your eyes.”
This combination of activation of the memory and its emotional core, along with the increase in serotonin, creates the window for disrupting the linkage which has been encoded at the time of traumatization. The distraction displaces the thought from working memory and inhibits further responsiveness. Since the exact circumstances of the previous traumatizing moment cannot be replicated, the memory fades and becomes a simple memory without emotional context and is unable to produce a fear response.
After havening, the patient feels calm. Following the havening process to ensure the memory and the stimulating cues are removed, the patient is asked to attempt to recapture the same feelings she had at the start of the process. Invariably, the patient will be unable to recall the previously thought experience and may present in one of 3 ways: (1) the thought is gone, (2) the thought is looked at from above with no emotional content, or (3) the thought is fuzzy. The patient finds a safe haven. When this is accomplished, the phobia disappears forever.
It is the authors’ experience that these techniques work extremely well when used with patients who present with varying degrees of anticipatory anxiety. Most of the therapy can easily be done in the dental chair using the above protocol. You will find that the patient is more relaxed and ready to accept care. One or 2 repetitions should be sufficient to achieve significant results. After years of experience this nondrug therapy has been shown to be safe and effective. For further information, scientific foundation, and testimonials visit healingthemind.net.
CONCLUSION
A technique has been demonstrated that utilizes the patient’s thoughts, emotions, and the extrasensory components of touch to modify encoded pathways to disrupt and eliminate unwanted responses from previous traumatic experiences.
References
- Choy Y, Fyer AJ, Lipsitz JD. Treatment of specific phobia in adults. Clin Psychol Rev. 2007;27:266-286.
- Marks I. Exposure therapy for phobias and obsessive-compulsive disorders. Hosp Pract. 1979;14:101-108.
- Tolksdorf W, Siefert S. Drug-related methods for alleviation of stress in dentistry. Anesth Pain Control Dent. 1992;1:34-40.
- Bourne EJ. The Anxiety & Phobia Workbook. 4th ed. Oakland, Calif: New Harbinger Publications; 2005.
- Seligman MEP, Walker EF, Rosenhan DL. Abnormal Psychology. 4th ed. New York, NY: WW Norton and Co; 2000.
- Fellous J-M, Arbib MA, eds. Who Needs Emotions? The Brain Meets the Robot. New York, NY: Oxford University Press; 2005.
- Weisstaub NV, Zhou M, Lira A, et al. Cortical 5-HT2A receptor signaling modulates anxiety-like behaviors in mice. Science. 2006;313:536-540.
- Field T, Hernandez-Reif M, Diego M, et al. Cortisol decreases and serotonin and dopamine increase following massage therapy. Int J Neurosci. 2005;115:1397-1413.
- Shapiro F. Efficacy of the eye movement desensitization procedure in the treatment of traumatic memories. Journal of Traumatic Stress. 1989;2:199-223.
Dr. Steven Ruden graduated from New York University in 1971. He is the director of the Sea Cliff Health Center. His education includes 2 years of training in periodontics at Albert Einstein College of Medicine, advanced studies at The LD Pankey Institute, and continuing education at Lund University in Malmo, Sweden. As director of the dental implant program at Nassau University Medical Center (1986 to 1998), he created and developed many of the procedures in use today and trained a generation of implant dentists. Dr. Ruden is a certified hypnotherapist, which enables him to address many phobias that interfere with patients’ ability to accept optimal dental treatment. He can be reached at drruden@seacliffdentist.com.
Dr. Ronald Ruden started his academic career in 1971 when he earned his PhD in organic chemistry. He then joined Nobel Laureate E.J. Corey at Harvard where they developed new advanced synthetic methods and pioneered computer modeling in chemical synthesis. Two years later, he was asked to join the faculty of Rutgers University. At Rutgers, he became interested in medical research and received his MD from Mt. Sinai School of Medicine in 1979. He took a Fellowship in Nutrition at Sloan Kettering Cancer Center, and during his first year he chaired an international symposium on cancer and nutrition. He is a published author, and his first book, The Craving Brain, is in its second edition and addresses issues pertaining to addiction and obesity. Dr. Steven Ruden is the contact author for this article.
Disclosures: Drs. Steven and Ronald Ruden report no conflicts of interest.