Some of the greatest learning at scientific sessions occurs during informal conversations—often in the lobby bar—with my colleagues after the official session is over. One such discussion revolved around the question “What is the most complex restorative challenge for the restorative dentist when providing treatment in the aesthetic zone?” Would it be a single restoration on a natural central incisor, or perhaps the placement and restoration of a single implant to replace either a central or a lateral incisor? What about the added complexity of 2 congenitally missing lateral incisors?
These discussions resulted in the development of a simple systematic approach to treating every aspect of implant restoration in the aesthetic zone. What do we look for and measure in every case so that we don’t miss clinical signs that will result in an aesthetic compromise, especially if they are not addressed at the appropriate step in the case? This treatment approach, as demonstrated in this article, enables the dentist to predictably identify potential problems during the treatment-planning phase so problems are avoided before they occur, resulting in an imperceptible aesthetic result.
CASE REPORT
Diagnosis and Treatment Planning
A 22-year-old female patient presented with congenitally missing right and left lateral incisors (teeth Nos. 7 and 10). She said that she wanted a “natural, beautiful appearance” and requested a minimally invasive solution. Her determination to preserve her natural smile and tooth structure drove the treatment plan and execution to provide the smile she wanted.
 |
 |
| Figure 1. This preoperative photo shows why this patient is high risk for aesthetic treatment: triangular-shaped central incisors, high gingival scallop, high smile line, and the Cupid’s bow upper lip. | Figure 2. The incisal view reveals sufficient alveolar ridge and soft-tissue topography for implant placement to replace teeth Nos. 7 and 10. |
 |
| Figure 3. This fully guided surgical splint was not used, but today it would provide the exact angle, position, and depth of the implant placement during surgical placement. |
She had been referred to our office by her orthodontist. At the initial appointment, she was wearing an Essix appliance with plastic denture teeth inserted to replace the missing lateral incisors.
The initial evaluation involved a detailed analysis of any midline discrepancies, the amount of gingival display, the variation of gingival display in the arch that we were treating, and the location of all the gingival zeniths in the area of treatment. Her dental midline was concentric with her facial midline. Since maximum lip dynamics occur when both the zygomatic major and the orbicularis oculi muscles are engaged, it is important to use the Duchenne smile to assess gingival display.1 She displayed a “Cupid’s bow” gingival smile line, which is defined by the absence of display of the midfacial gingival tissue of the central incisors (ie, a low smile line on teeth Nos. 8 and 9) combined with the display of midfacial zenith gingival tissue on other maxillary teeth in the aesthetic zone (ie, a high smile line on teeth Nos. 3, 4, 5, 6, 11, 12, and 13)2 (Figure 1). This scenario is high-risk, with a poor prognosis for an acceptable aesthetic outcome because everything that needs to be restored is in the visual field. She had a high gingival scallop, and the central incisor zenith and canine zenith were not in the same plane: The canine zenith was positioned 3.0 mm incisal to the central incisor zenith. The central incisors exhibited a triangular tooth shape, and their incisal lengths and embrasures were not symmetrical.
The lateral incisor’s edentulous sites had ideal soft tissue and bone volume. The orthodontic workup included lateral cephalometric tracings (dated September 2010 and July 2016); these tracings were evaluated and compared to confirm that no facial growth had occurred over the observed period. The restorative dentist must evaluate the mesiodistal width of the edentulous areas to determine if they are equal. If not, prior to the surgical consult, the spaces would be equalized, either with direct composite placement or minor orthodontic tooth movement. In this patient’s case, the contralateral spaces were identical, and the patient was referred to the oral surgeon.
 |
 |
| Figure 4. Impression copings were placed for the fixture-level impression. | Figure 5. The screw access for the left lateral incisor extends to the incisal facial of the provisional restoration. |
 |
 |
| Figure 6. The Essix retainer, with a window cut out to allow for maturation of tissue while retaining the correct tooth position. | Figure 7. This photo demonstrates the uneven location of the lateral incisor gingiva, with the zenith of tooth No. 10 positioned 1.5 mm incisal to that of tooth No. 7. |
 |
 |
| Figure 8. The facial emergence profile is flattened and under-contoured subgingivally when the free gingival margin needs to be moved incisally. | Figure 9. This case required augmenting the facial emergence profile with composite to move the free gingival margin apically. |
 |
 |
| Figure 10. The bulkier facial contour of the provisional creates blanching of the facial tissue, which disappears within a few minutes. | Figure 11. Flowable composite resurfaced and polished the provisional. |
The oral surgeon believed there was adequate bone volume and architecture as well as adequate soft-tissue thickness at the transmucosal connection (thick tissue biotype) (Figure 2). A vacuum-formed surgical guide (pilot guide) was fabricated by the restorative dentist to aid in proper implant positioning. However, a pilot guide does not guide the surgeon toward obtaining the exact angle and depth of the implant. Implant complications occur 48% of the time because the implant is placed with a poor angulation, and, 25% of the time, the complication occurs because the implant is placed in the wrong location. In contrast, a fully guided surgical splint is created by syncing the CBCT scan of the maxillary arch with the scanned model. Implants are placed virtually in the software. After the surgeon verifies and approves this placement, a surgical guide is printed. This guide provides the exact angle, position, and depth of the implant during surgical placement. A CBCT scan has zero distortion (Figure 3).
Treatment Phase: Surgical Phase and Transitional Prosthesis
A bone-level, 4.1- × 10-mm Straumann SLActive implant was selected. The rough, osseoconductive surface with a horizontal offset and the platform shift design at the neck is felt to be the most effective design to maintain the marginal bone level against functional load. The implants were placed toward the palatal aspect of the maxillary alveolus at a 15° inclination. A healing abutment was placed.
A transitional prosthesis allows both the patient and dentist to preview and correct any tooth form, length, or incisal and facial embrasures that do not meet their expected aesthetic vision. It also allows the dentist to groom the soft tissue by subtracting or adding composite to the provisional. Since the interproximal bone levels on the adjacent teeth dictate the interproximal papillary height, grooming occurs on the facial.3 Impression copings were placed, and a fixture-level impression was taken (Figure 4).
 |
 |
| Figure 12. Patient approval of the provisional smile, including tissue contours, tooth shape, and incisal embrasures, is confirmed with a signature. | Figure 13. The photographs are taken with the shade sample in the same plane as the tooth and include a detailed description: “distal and gingival third BL4 stain, middle and body shade BL3.” |
 |
| Figure 14. Flowable composite is injected into the sulcus and light cured, ready for the fixture-level impression. |
A transitional screw-retained composite prosthesis was created, followed by an evaluation of soft-tissue heights and grooming of the soft tissue.4
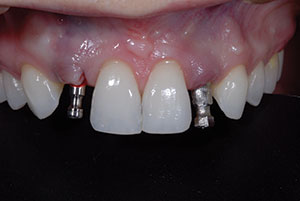
When the case was returned from the ceramist, it was noted that the screw access of the left lateral incisor protruded out of the incisal facial of the composite prototype (Figure 5). As previously mentioned, almost half of implant complications are the result of an implant placed with poor angulation. In this case, the final porcelain crown would need to be cemented over a custom abutment in order to avoid the screw access being placed on the facial of the restoration.
The patient returned for the fabrication of the transitional prosthesis. The healing abutment was removed, a reverse torque test at 20 Ncm verified integration, and the impression coping was screwed into place. A radiograph was taken to verify complete seating of the coping. Shade photos were taken, followed by a fixture-level impression, and then the laboratory-team-prepared, provisional, screw-retained composite crown (Sinfony [3M]) was fabricated.
At the provisional crown try-in appointment, it was noted that an excess of facial gingival tissue was present. To create an ideal smile design, the zenith of the canines and the centrals should be on the same plane, and the zenith of the lateral incisors should be 0.5 to 1.0 mm incisal to a line drawn from the centrals to the canines. Her smile presented with the zeniths of the centrals being 3.0 mm higher than the canines. Since the goal was to create a harmonious smile, the zenith of the laterals needed to be positioned at the midpoint between the canine and central incisor gingival zeniths. The facial gingiva was probed to the head of the implant, and a gingivectomy was planned that would leave a 4.0-mm zone of facial gingiva as measured from the crest of the implant.5
 |
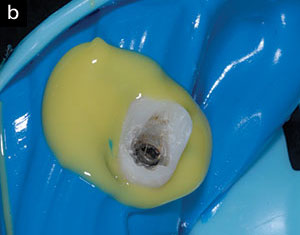 |
| Figure 15. Seating the tissue-bearing side of the prototype into the light-body vinyl polysiloxane impression. |
 |
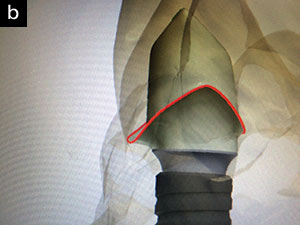 |
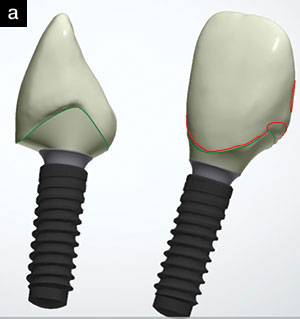
| Figure 16. The zirconia abutment with titanium was designed digitally. |
A diode soft-tissue laser (Gemini 810 + 980 diode laser [Ultradent Products]) was used to remove the excess gingival tissue via a scalloped design. Extreme care was taken to preserve the interproximal papilla. The diode laser can be used in the presence of metal, implants, and pacemakers, while an electrosurgery unit cannot. A laser cut creates a zone of necrosis 3 to 5 cells thick, which is thinner than a human hair. Superficial coagulation occurs with no edema. An Essix retainer was fabricated with a window cut out in the gingival to middle third of the lateral incisors to both maintain the tooth position and allow healing of the facial and interproximal tissue (Figure 6).
 |
 |
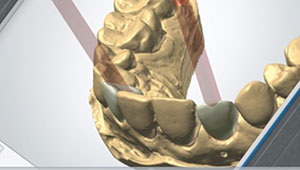
| Figure 17. Digital verification that a screw-retained design could not be utilized. | Figure 18. Zoom day white 14% (Philips Oral Healthcare) was placed in at-home bleaching trays to brighten the natural dentition and improve the color match with the porcelain crowns. |
 |
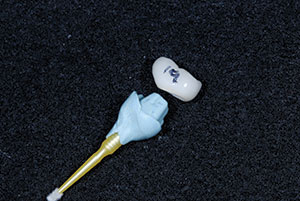 |
| Figure 19. The abutments were inserted in a wet environment and torqued to 35 Ncm to secure the new, never-before-used, titanium abutment screws. | Figure 20. An analog of the abutment was created to minimize any excess cement that would be trapped subgingivally on the implant. |
 |
 |
| Figure 21. The final lithium disilicate (IPS e.max [Ivoclar Vivadent]) (HTBL2 ingot) restorations have proper aesthetic emergence profiles, contours, and color and healthy interproximal papillary form. |
Three weeks following the gingivectomy, the facial and interproximal tissue heights were evaluated. The desired gingival architecture was evaluated by drawing a horizontal line between the height of the facial gingival zenith of the lateral incisors. In this case, the maxillary left central incisor zenith was 1.5 mm incisal to the right lateral incisor (Figure 7). The provisional facial contour is contoured to be flat up to 1 mm of the proposed free gingival margin. The subgingival emergence profile can be altered by manipulating the facial soft tissues, which will adapt to compression from the provisional. If the facial tissue at the height of the contour on the free gingival margin needs to be moved incisally, the composite prototype is flattened under the zenith (Figure 8).6 If the tissue at the zenith needs to be moved apically, a flair or bulge is created at this point, and the tooth form will apically position the tissue. The tissue is shaped by the manipulation of concavities and convexities in the provisional restoration. Since we needed to move this zenith apically, the restoration was unscrewed, and flowable composite was added and highly polished (Figure 9). The restoration was screwed back into the implant and torqued to 15 Ncm. Any blanching of the facial tissues that occurs when the provisional is seated disappears within a few minutes (Figure 10). The provisional composite aesthetics on the right central incisor were unacceptable. The color was monochromatic and too opaque, which did not blend with the patient’s translucent, natural dentition. A medium coarse diamond (KSOF diamond [Brasseler USA]) was used to remove 0.5 mm of facial composite. A flowable composite (Beautifil Flow Plus [Shofu Dental]) was placed and contoured with a wax spatula. This extra step only took 5 minutes and created a composite prototype that blended imperceptibly into her smile (Figure 11). All the surfaces were polished (Astropol [Ivoclar Vivadent]), and then a final finishing glaze (LuxaGlaze [DMG America]) was applied and light cured for 10 seconds. Correct occlusal clearance to prevent overload in maximum intercuspation and chewing cycle were confirmed.
 |
| Figure 22. The postoperative full-face photo demonstrates that the implant restorations blended perfectly with the natural dentition. |
At this point in the process, patients often become impatient to get their real tooth/teeth. Together, we review the importance of achieving ideal tooth and tissue contours and outlines. The patient’s approval of the provisional is recorded along with his or her signature.
Once the provisional and tissue contours are ideal, impressions are taken for the final restoration. The impression technique described below is necessary to ensure that the ceramist has the road map to predictably design and create a definitive porcelain restoration that duplicates the now-accepted provisional aesthetics. This is the predictability piece that is paramount to the success of the buy-in from the patient.
Impression Technique
Two weeks later, patient approval was confirmed with a signature (Figure 12), and she returned for the final impression. Shade selection was done at the beginning of the appointment. Natural teeth easily become dehydrated and appear whiter, so accurate shades are best taken as soon as the patient is seated. The photographs are taken in the same plane as the facial surface of the tooth being used for comparison. Shooting in RAW format and using a gray card in the photo helps the ceramist with color calibration. A written color description of what is being seen and in what areas of the tooth also aids the ceramist with color matching and mapping of the tooth (eg, distal and gingival third BL4 stain, middle and body shade BL3) (Figure 13).
Custom Impression Copings: Preservation and Duplication of the Tissue-Bearing Area
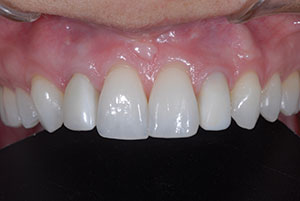
The subgingival envelope of the provisional must be reproduced so the ceramist can duplicate it in the final restoration. One technique is to duplicate this area using a customized impression coping. The provisional, screw-retained composite crown is removed, and an impression coping is screwed into place. The flowable composite is immediately extruded and injected into the sulcus and light cured. This prevents collapse of the tissue (Figure 14). A radiograph is taken to verify the complete seating of the coping. An alternative technique involves fabricating an impression of the tissue side of the provisional and seating the tissue-bearing side of the prototype into the light-body vinyl polysiloxane (VPS) impression (Figure 15). This provides an actual cast of the soft-tissue emergence profile, which shows the exact support of soft tissue needed to replicate the papillary and free gingival margin height and contours.7,8
A fixture-level, full-arch impression (Honigum [DMG America]); face-bows (Panadent); opposing impressions (AccuDentXD [Ivoclar Vivadent]); and bites (Virtual CADbite [Ivoclar Vivadent]) were recorded. A zirconia abutment with titanium inserts, chosen due to its aesthetics and strength, was designed digitally (Figure 16). A lithium disilicate (IPS e.max [Ivoclar Vivadent]) HTBL1 ingot was selected for the crowns due to its aesthetic properties and high flexural strength (approximately 500 MPa). A screw-retained design would have been selected for ease of retrievability and a decreased risk of subgingival cement retention. However, the implant angle was skewed, forcing the screw channel opening to be directed through the facial incisal edge (Figure 17).
At the following appointment, the screw-composite prototypes were removed, and the abutments were screwed in, followed by crown try-in and evaluation. The crown shades were too light, so photographs with shade tabs next to the restorations were taken, and a detailed color map was sent that asked for a more superficial
stain. At the next appointment, the restorations were tried in. The crown color was very close but still slightly too light. The patient liked the lighter porcelain color and reported that she had not whitened her natural teeth for 3 months. Custom at-home trays were fabricated over the non-cemented crowns, and whitening gel was dispensed (Zoom day white 14% [Philips Oral Healthcare]) (Figure 18). Two days later, she approved the shape, form, and color of the final restorations.
New, never-used titanium abutment screws were torqued at 35 Ncm torque force in a wet environment to secure the custom zirconia abutments. Ten minutes later, the screws were torqued again to 35 Ncm (Figure 19) to minimize the risk of screw loosening. The access opening was covered with plumber’s tape and then composite.
A custom analog of the abutment was fabricated by injecting a VPS bite registration material (O Bite [DMG America]) inside the crown and placing a stick into the VPS material. Using this replica will minimize or prevent cement retention subgingivally along the implant. At cementation, a self-adhesive resin cement (TheraCem [BISCO Dental Products]) was chosen because it contains MDP, which is basic and releases calcium and fluoride. Then the crown was quickly placed over the replica so that all excess cement remained on the replica. The crown was then quickly removed from the replica and seated over the zirconium abutment in the mouth (Figure 20).
The incisal edges of the central incisors were leveled with a medium sandpaper disc (Sof-Lex [3M]). The screw-retained composite provisional and the implant models were archived in her records box, although we always hope they will never be needed again.
CLOSING COMMENTS
The technique utilized in this case provides a system for designing the composite prototype and fabricating the definitive porcelain restoration while eliminating guesswork on shape and form for the ceramist. For patients with significant gingival display, the gingival shape, position, and contour are just as important as the crown shape, position, and contour in achieving aesthetic success. The pink soft tissue is the backdrop of the smile and, therefore, must be assessed preoperatively to determine what changes may be required (Figures 21 and 22). Surgical guides, created from CBCT scans easily and economically, allow virtual placement of implants. These guides are precise and standardize the size, angle, and depth of placement, eliminating a majority of possible implant complications. This technology was in its infancy when this case was being restored. Many excellent surgeons and general dentists have not adapted this technology for single-tooth implants and immediate extractions. There are flaws in every technique, but can we accept the errors of not using digital design in 2019 and into the future? The preciseness and predictability of this technology may lead us to using fully guided surgical splints as the standard of care.
Acknowledgments:
The concepts shown here are the teachings of the Kois Center in Seattle, the American Academy of Cosmetic Dentistry, and Catapult Education. The author would like to thank Dr. Karel DeLeeuw for his surgical expertise; Rick Durkee, Matt Roberts, and Tom Dippel for their laboratory work and support; and Dr. Jean Martin for her editing expertise.
References
- Duchenne GB. The Mechanism of Human Facial Expression. New York, NY: Cambridge University Press; 1990.
- Hochman MN, Chu SJ, Tarnow DP. Maxillary anterior papilla display during smiling: a clinical study of the interdental smile line. Int J Periodontics Restorative Dent. 2012;32:375-383.
- Choquet V, Hermans M, Adriaenssens P, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72:1364-1371.
- Leziy SS, Miller BA. Aesthetics in implant therapy: a blueprint for success and change. Ann R Australas Coll Dent Surg. 2010;20:28-35.
- Kois JC. Predictable single-tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2001;22:199-206.
- Phillips K, Kois JC. Aesthetic peri-implant site development. The restorative connection. Dent Clin North Am. 1998;42:57-70.
- Neale D, Chee WW. Development of implant soft tissue emergence profile: a technique. J Prosthet Dent. 1994;71:364-368.
- Jemt T. Restoring the gingival contour by means of provisional resin crowns after single-implant treatment. Int J Periodontics Restorative Dent. 1999;19:20-29.
Dr. Bassett practices comprehensive restorative and aesthetic dentistry in Scottsdale, Ariz. She is an Accredited Fellow of the American Academy of Cosmetic Dentistry and served as president from 2015 to 2016. Dr. Bassett is a Kois clinical instructor, a member of the Academy of Fixed Prosthodontics, a Diplomate of the American Board of Aesthetic Dentistry, a Fellow in the AGD, an associate member of the American Academy of Esthetic Dentistry, and a member of the Catapult Education Speakers’ Bureau. She can be reached via email at [email protected] or via the website drbassett.com.
Disclosure: Dr. Bassett receives honoraria for podium lectures from BISCO, DMG America, and Ivoclar Vivadent. She did not receive compensation for this article.
Related Articles
Predictable Tooth Replacement in the Aesthetic Zone
Bassett and Calvo Take Home AACD Evy Awards
Strategies for Consistent Aesthetics and Function



