INTRODUCTION
Diode lasers have been utilized in dentistry for many years now as an effective means to help manage gingival tissues during restorative procedures. Prior to the development of diode lasers, electrosurgery (radiosurgery) was used for many of the same soft-tissue management indications. While there are still some procedures for which electrosurgery technology is useful, there are limitations to its use because of the extensive amount of tissue damage (necrosis) that it can cause. The zone of tissue necrosis around an electrosurgery cut is 3 to 5 times wider than the same zone seen when using a diode laser. Also, electrosurgery devices cannot be used safely around metal dental restorations or titanium implants. Since many restorative dentists are placing and/or restoring dental implants, it is important to remember that the use of electrosurgery around them is strictly contraindicated.
The main objection that clinicians have had with diode lasers is that they feel lasers are slower to cut. This is probably due to the limits on the power (watts) they have in order to minimize collateral thermal damage. As a result, these diode lasers are typically used in “continuous wave” mode to cut faster, but the constant energy can result in more tissue damage (necrosis) than desired, although not nearly as much as with electrosurgery. It is imperative that the clinician understand periodontal tissues, biotypes, and crestal bone position relative to restorative margin position before performing any soft-tissue laser procedure; that said, better control of cutting, as well as less peripheral tissue damage, is the clinical objective as advances in laser technology become incorporated into the newest diode lasers on the dental market.1
“Super Pulsed”—The Latest in Diode Laser Technology
Super pulsed diode lasers are the latest offering in soft-tissue lasers. One of the first of this type specifically designed for dentistry is the Gemini Laser (Ultradent Products). Existing diode lasers on the market are either 810- or 980-nm wavelength. The chromophores that these laser photons seek in the tissue are hemoglobin (pigment) and water; 810-nm-wavelength diodes are better suited for coagulation (hemostasis), while 980-nm wavelength diodes are more efficient at tissue ablation (cutting). The Gemini Laser combines 810- and 980-nm wavelengths in one unit to enhance both coagulation and ablation performance. However, the main difference seen by combining wavelengths is the ability to achieve 20 W of peak power (most diodes are in the 2- to 5-W peak power range) over an extremely short duty cycle (the time the laser energy is actually firing). Therefore, the amount of thermal relaxation that is achieved between pulses allows the tissues to cool to such a degree that the necrosis (collateral tissue damage) is drastically reduced. The clinical result means cleaner cuts (little to no charring), faster healing times, more operator control, and less patient discomfort both during and after the procedure. The extent of collateral thermal effects can be decreased by a factor of 2 to 3 for the super pulsed mode when compared to continuous wave mode from an older diode laser. Comparable incisions in depth can be made more quickly and efficiently with less energy when using a super pulsed diode laser. Optimal clinical results with the least risk of thermal damage are achieved with very short pulses (duty cycles) at the highest peak power possible using super pulsed technology. And, since super pulsed lasers have such low heat output, they are extremely safe to use around metallic restorations and implant components—for example, to uncover implant platforms to place impression copings during the impression phase of treatment.2
A Useful Everyday Tool for Better Restorative Outcomes
Most of the time, diode lasers are marketed to be used to trough the gingival tissue prior to taking a final physical or digital impression in lieu of using a traditional approach for tissue management by packing gingival retraction cords for crown and bridge impressions. While troughing can be useful when judiciously used, it is not the only clinical application for this wonderful tool. This article will explore other clinical procedures where having a diode laser can make the difference between a simple, successful outcome and struggling to control the soft-tissue environment during a procedure.
CASE REPORTS
Case 1: Operative Dentistry—Class II, III, and V Restorations
Most every restorative dentist provides direct restorative services to his or her patients that include composite (resin-bonded) restorations that can extend near or below the gingival tissue due to the extent of decay or a previous subgingival restorative margin placement. Since the 2 main enemies of adhesive dentistry are blood and saliva, any hemorrhage of the gingival tissues during the adhesive process can compromise the final result. Many times, when replacing an old restoration, an improper proximal contour can be enough to cause chronic gingival irritation that can stimulate bleeding when etching near the tissue or placing a matrix and wedge prior to placement of the restorative material. Some clinicians will pack a retraction cord in an effort to control bleeding in the restorative area; however, it can often get caught up and cured in the composite after placement or stimulate even more bleeding. The use of chemical astringents (hemostatic agents) may also interfere with the bonding process if not completely removed prior to performing the adhesive steps. The use of a diode laser in these instances solves the problem immediately. The restorative margin, in many instances, can be made to be supragingival by the removal of a small amount of tissue and, at the same time, achieve hemostasis for the restorative procedure.
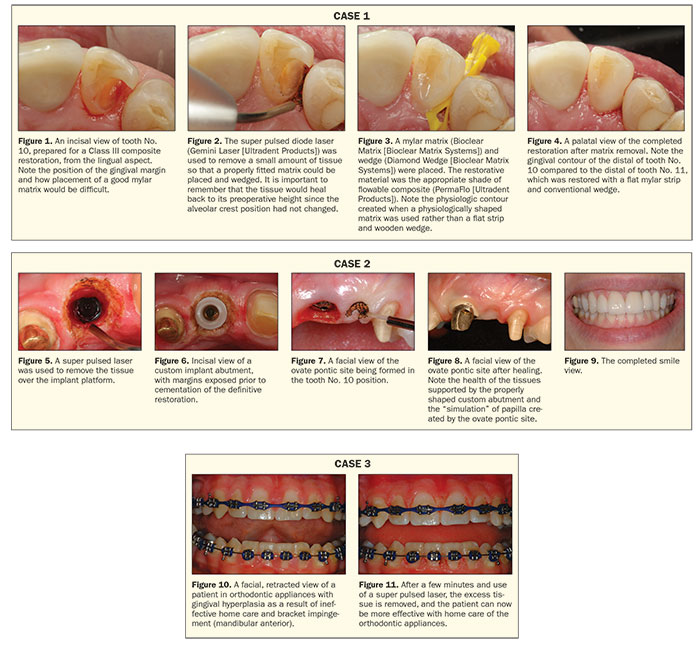 |
Figure 1 is a lingual view of a Class III preparation in tooth No. 10 after removal of the recurrent decay, old restorative material, and tooth preparation. The super pulsed diode laser (Gemini Laser) was used from the lingual aspect to perform a “mini” gingivectomy and create a supragingival margin to the preparation (Figure 2); a matrix could then be more easily placed, and there was tooth surface apical to the restorative margin to support the proximal wedge without indenting the matrix, which could negatively affect the contour (Figure 3). Also, placement of the wedge was now less likely to stimulate further bleeding while the restorative procedure was being completed. Figure 4 shows the completed Class III composite restoration after removal of the matrix and wedge and after polishing procedures have been completed.
Case 2: Implant Dentistry—Uncovering Platforms for Restorative Component Placement
Another common procedure performed by restorative dentists in practice today is the restoration of dental implants. Managing the gingival tissues during impressions, abutment placement, and delivery of the definitive restoration can be challenging, particularly if the tissues are overgrown around the healing abutment or if they creep over the platform when a healing abutment is loose.
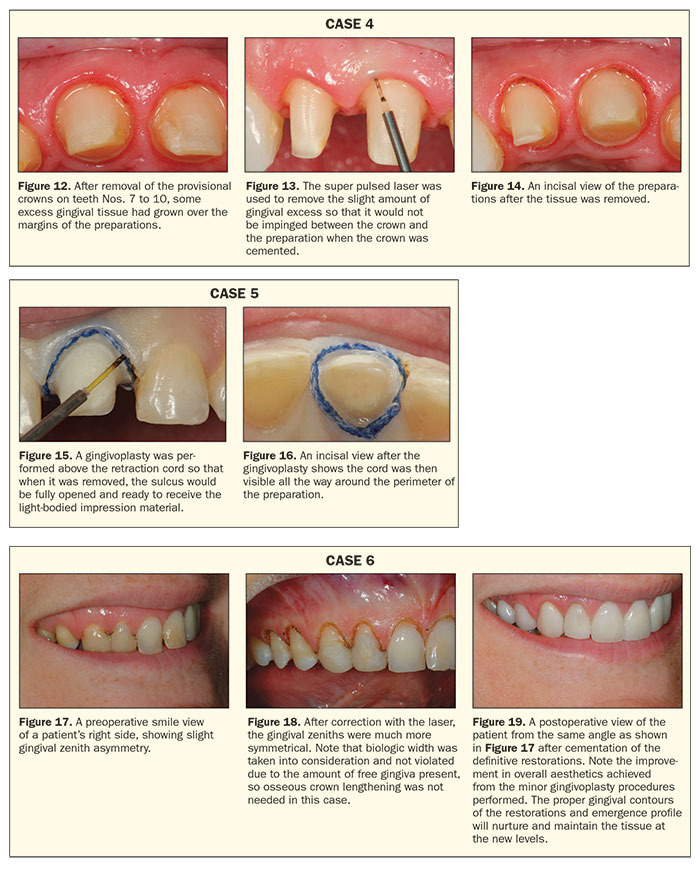
Figure 5 shows the clearing of the platform of an internal hex implant so that the impression coping can be placed without interference from the excess tissue that had creeped in under a loosened healing abutment. Without a fully cleared implant platform, there is always a danger that the impression coping will not fully seat. This will cause an improper fit to any restoration that is fabricated from that impression. A super pulsed diode laser is also useful when placing custom implant abutments prior to delivery of the implant crown. After the custom abutment is placed and complete seating is verified by radiograph, it is necessary to visually see all of the margins of the custom abutment just as if it were a prepared tooth. If any gingival tissue covers the abutment margin, it is not likely that the cementation process will “push” the tissue out of the way. It is more likely that the tissue will prevent full seating of the restoration. So, in a case like this, the laser is used around the periphery of the custom abutment after placement to ensure full seating of the crown when it is cemented (Figure 6). Figure 7 shows a fixed-implant case where a diode laser was used to remove the excess tissue around the healing abutment in the tooth No. 9 position. Note that the gingival tissue surrounding the healing abutment was “flared” to more adequately reflect the diameter of a central incisor root so that the custom abutment would properly support the gingival tissues with a natural physiologic contour. If a pontic site has adequate keratinized tissue present, a diode laser can also be used to create an “ovate pontic site” so that the pontic will have the appearance of “emerging” from the gingival tissues rather than sitting in front of them as with a typical “ridge-lap” design. Figure 8 shows the tissue healed prior to delivery of the definitive restorations. Note how well the custom abutment supports the gingival tissue and “simulated” papillae as well as the ovate pontic site and the simulated papilla between the site and the adjacent maxillary canine preparation. Figure 9 is a full-smile view of the fixed-implant case at the 10-year followup.
Case 3: Orthodontic Tissue Management During Bracket Placement and Treatment
Diode lasers are becoming a useful tool in the management of orthodontic cases with fixed appliances. Often with ineffective oral hygiene, coupled with the added difficulty of maintenance while wearing fixed orthodontic appliances, clinicians can struggle with gingival tissues making proper bracket placement difficult, as well as encounter the same difficulties while bonding the brackets to place that restorative dentists face (namely blood contamination). Since super pulsed lasers, such as the Gemini Laser, have such a short duty cycle that allows for thermal relaxation of tissue, the minor gingivoplasty procedures required for the purposes mentioned above can often be performed without local anesthesia. This is a definite advantage for the busy orthodontic practice (Figures 10 and 11).
 |
Case 4: Crown and Bridge—During Crown Cementation
Many provisional crowns do not fit the margins of the preparations very well, and this can lead to excess temporary cement in the gingival crevice or marginal gaps and openings between the provisional restoration and the tooth. The result can be chronic inflammation and ingrowth (proliferation) of gingival tissue over the preparation margin (Figure 12). Again, if the definitive restoration is to be placed with an adhesive protocol, this can present a potential contamination problem. Also, regardless of cement protocol, excess tissue over the preparation margins can prevent the crown from fully seating during the cementation process. A super pulsed laser is ideal for clearing the excess tissues away, often without the use of local anesthesia, so that the crown can be fully seated (Figure 13). Figure 14 shows the cleared crown margins prior to cementation of the definitive restoration.
Case 5: Crowns and Bridges as an Adjunct to Cord Packing
Many clinicians use a 2-cord retraction technique when taking master impressions. The most incisal (occlusal) cord is placed at the level of the restorative margin. Ideally, the dentist should see the entire top cord around the length of the margin so that when it is removed, a fully patent sulcus will be present for the injection of light-bodied impression material. Often, a localized area of a preparation may have a tissue prolapse over the cord, making it not visible. This is common in interproximal areas where the gingival tissues (papilla) may be slightly enlarged. It is not recommended to simply hope that the heavy-bodied tray material will push the tissue out of the way to let the light-body material access the crevice. Figure 15 shows the super pulsed diode laser performing a gingivoplasty above the top cord—in this case, the No. 1 retraction cord—prior to removal and injection of the light-body impression material. Figure 16 shows the preparation of tooth No. 8 from the incisal view. The entire blue cord (Ultrapak No. 1 [Ultradent Products]) can be seen 360° around the tooth. When the cord was removed, an impression of the margin was taken, including 0.5 mm of tooth/root surface apical to the margin so that the emergence profile of the tooth was included.
Case 6: Crown and Bridge—Aesthetic Gingivectomy Prior to Definitive Restoration
Aesthetic gingivectomies can be performed to create symmetrical gingival levels when performing crown and bridge procedures as long as biologic width3 is not encroached upon. When there is adequate amount of free gingiva present (one must leave a minimum of 1.0 mm of sulcus depth), a super pulsed diode laser is the perfect tool to refine the gingival aesthetics of a case. Figure 17 shows a preoperative smile view of the maxillary left side. One of the goals of treatment was to balance the gingival zeniths as much as possible without necessitating bony crown lengthening, which was declined by the patient. Once the gingivectomy procedure was performed (Figure 18), the teeth were prepared, and provisional restorations were placed. After approximately 12 weeks of healing, the master impression was made, and the case was completed. Figure 19 shows the same smile view of the patient’s right side after delivery of the definitive restorations. Note the subtle difference that balancing gingival heights can have on the outcome of a case.4
IN SUMMARY
Several clinical examples have been shown using a super pulsed diode laser in the everyday practice of restorative dentistry. The chair time and dollars saved, along with the optimal results achieved utilizing this technology to its fullest, make the use of a soft-tissue diode laser an indispensable part of the clinician’s armamentarium.
References
- Goharkhay K, Moritz A, Wilder-Smith P, et al. Effects on oral soft tissue produced by a diode laser in vitro. Lasers Surg Med. 1999;25:401-406.
- Borchers R. Comparison of diode lasers in soft tissue surgery using CW and superpulsed mode: an in vivo study. International Journal of Laser Dentistry. 2011;1:17-27.
- Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol. 1961;32:261-267.
- Kois JC. Altering gingival levels: The restorative connection Part 1: biologic variables. J Esthet Restor Dent. 1994;6:3-7.
Dr. Lowe received his DDS degree from the Loyola University School of Dentistry in 1982. He previously taught at the Loyola University School of Dentistry while building a private practice in Chicago. Dr. Lowe currently maintains a full-time practice in Charlotte, NC. He can be reached at boblowedds@aol.com.
Disclosure: Dr. Lowe receives honoraria from Ultradent Products, Inc.
Related Articles
The Bulk-Fill Class II Composite Restoration
Complete Oral Rehabilitation: A Case Report: Using a Combined Surgical/Ceramic Approach











