Dentists are specialists in diagnosing and treating problems of the stomatognathic system. Typically, we are presented with problems that can be defined as a subset of an anatomic issue, such as a toothache resulting from pulpitis or a cracked tooth. This problem-focused diagnosis is the “bread and butter” of general dental practice. When examining a patient, we are taught to examine for oral cancer, occlusal problems, periodontal or endodontic issues, caries, etc. However, when multifactorial problems exist, we must creatively present plans that will address disease processes while honoring a patient’s chief complaints, concerns, and financial limits.1
This case study will serve to highlight issues clinicians face daily that involve when to extract teeth and place implants, how long to treat periodontally challenged teeth, and how to improve aesthetic difficulties in a patient with severe occlusal disharmonies.
CASE REPORT
Diagnosis and Treatment Planning
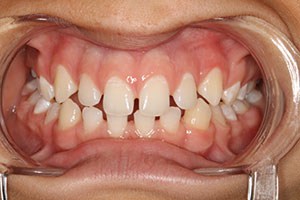
This patient presented with chief complaints of pain when chewing and dissatisfaction with her smile. In examining her dentition, it was noted that she had a blocked lateral incisor in linguoversion; a Class II malocclusion with a deep bite that resulted in her biting her incisive papillae during normal chewing; a severely canted occlusal plane; and severe fremitus with localized, severe type IV periodontitis, according to the ADA and American Academy of Periodontology (AAP) classification of periodontal disease. In discussing her treatment wishes, she expressed the desire to have us “pull her teeth and give her implants.” There was Class III mobility of teeth Nos. 6, 10, 12, and 23 to 26, along with several posterior molars.
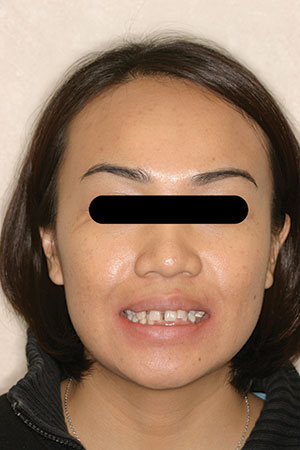 |
| Figure 1. Preoperative full-face photo. |
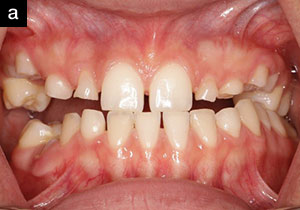
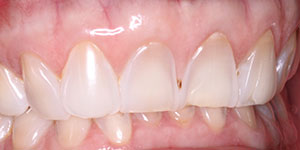
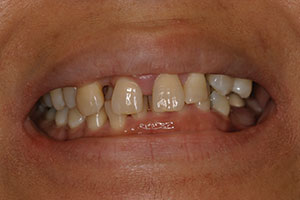
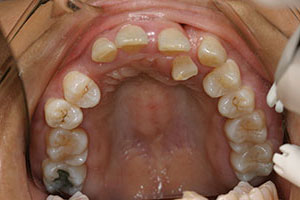
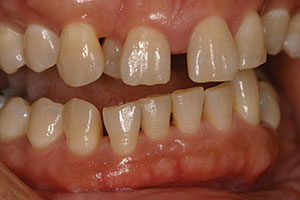
Her full-face smile photo revealed a large 3.0-mm diastema with a rotated canine and a slight grimace in maximum intercuspation position (Figure 1). In relaxed smile position, it was noted that the lower anteriors were in contact with her incisive papillae (Figure 2). Upon slight opening of her dentition and in the occlusal photograph, a canted occlusal plane with super eruption of tooth No. 22 into the missing tooth No. 11 site was noted, highlighting the reasons for her occlusal traumatism and fremitus (Figures 3 and 4). There was a stippled appearance to her gingiva, but a loss of interdental papillae in the mandibular anterior was representative of her bone loss. The patient had undergone periodontal surgery 4 years prior. The left lateral view showed a super-eruption of tooth No. 22 to the crestal ridge where tooth No. 11 had been removed, and the “step” between teeth Nos. 21 and 22 was significant and was the etiology for mobility of teeth Nos. 10 and 12 (Figure 5). The right lateral view revealed that tooth No. 10 was angled and tooth No. 6 had super-erupted (Figure 6).
Periodontal therapy was instituted with scaling and root planing, and a periodontal consultation was done. The patient had stable periodontium but understood that, even though there was not active bleeding upon probing and her oral hygiene was adequate, several teeth would be lost due to severe mobility from chronic periodontal disease and concomitant occlusal disease. Her participation in ongoing periodontal therapy and maintenance was required prior to initiating orthodontics and restorative prosthetics.
 |
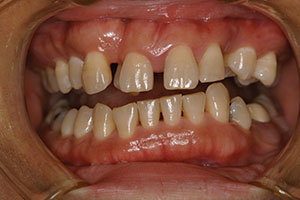 |
| Figure 2. Pre-op relaxed-smile photo. | Figure 3. Pre-op retracted photo with patient in slight disclusion. |
 |
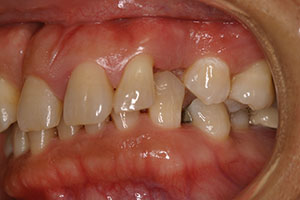 |
| Figure 4. Pre-op occlusal view, showing missing tooth No. 11 and tooth No. 7 in linguoversion. | Figure 5. Pre-op left lateral view, showing super-eruption of tooth No. 22. |
 |
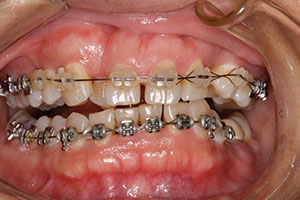 |
| Figure 6. Pre-op right lateral view. | Figure 7. Interim orthodontic photo. |
 |
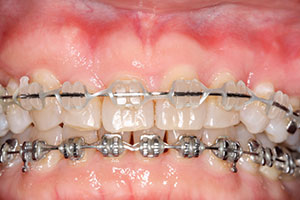 |
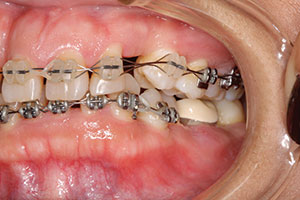
| Figure 8. Left lateral view in braces. | Figure 9. Frontal view near the end of orthodontic treatment. |
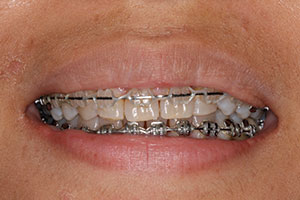 |
| Figure 10. Smile display at the completion of orthodontic treatment. |
To plan a comprehensive solution, while allowing for restoratively driven implant placement, a diagnostic wax-up would be required. Even with the most thoughtful planning, placing implants to replace her mobile teeth would require proper mesial-distal and occlusal vertical space. It would also require canine guidance, which would be protective for implant placement and the stability of her remaining dentition.
If teeth Nos. 7 to 10 and 22 to 26 required extraction with implant replacement, would there be enough space for all of her teeth to be placed in the available arch form? How much osteoplasty would be required in the areas of teeth Nos. 22 to 26 to level the bone and, thus, to level her curves of Spee and Wilson?
The complicated nature of anticipating the final occlusal construct necessitated orthodontic intervention to “set the stage” for proper implant placement.2 But how could orthodontics be treatment planned where there was ADA AAP type IV localized severe periodontal disease? Is that irresponsible? Would participating dentists get sued for tooth loss caused by orthodontic intervention?
To answer these questions, the following scenario can be evaluated: If a tooth is broken and extraction is inevitable, is it OK to use orthodontics to erupt this tooth to bring the bone down with the root prior to extraction? Can we use terminal teeth to help us achieve our goals? Of course, the answer is yes, and—if informed consent is discussed and documented and the patient understands that teeth will be lost either during or post orthodontic care to achieve idealized results—then the use of compromised dentition as anchorage units to achieve goals is warranted.3,4
 |
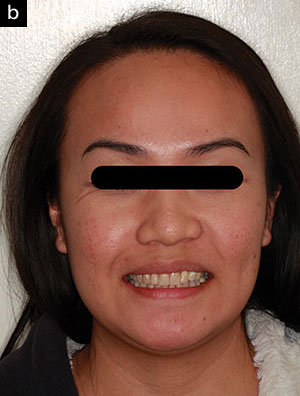 |
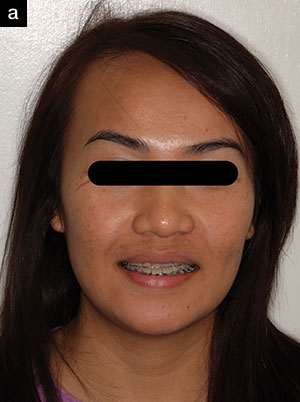
| Figure 11a. Full-face photo near the end of orthodontics. | Figure 11b. Full-face photo after removal of orthodontic appliances. |
The Use of Orthodontics
The use of orthodontics to facilitate a stable, aesthetic, implant-protected occlusion with idealized space creation and bone leveling is not only responsible, it is justifiable.
Orthodontics was prescribed by the general practitioner with specific instruction to align and correct rotated teeth, distalize the upper left quadrant of teeth, level the occlusal plane, intrude tooth No. 22, harmonize both arches, level the CEJs, bring tooth No. 7 into the arch in harmony with tooth No. 10, and achieve canine protected occlusion by using tooth No. 12 to mimic tooth No. 11 by placing it strategically into the No. 11 site and tipping it to look and act like a canine.
It is imperative that all treating doctors can communicate and offer insights to appreciate optimal multidisciplinary care. In this case, the dictates of future prosthetic rehabilitation required skilled orthodontic movement to ensure proper foundational support for implants, with minimal bone grafting needs post orthodontics. Without using orthodontic movement of teeth, bone grafting may have been required for the bony cleft present over tooth No. 7, the loss of bone width in the No. 11 site, and in areas of anticipated extraction due to bone loss and mobility.
Orthodontic treatment took 18 months and successfully achieved the outlined goals as delineated (Figures 7 to 10).
Upon the removal of brackets, there was a noted cosmetic improvement in smile display, the occlusal plane was normalized, buccal corridor symmetry was improved, and canine guidance was established.
 |
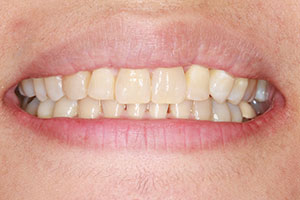 |
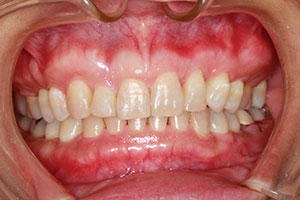
| Figure 12. Retracted view at 8 years postoperatively. | Figure 13. Smile view at 8 years post-op, with no implant placed to date. |
Optimal Results!
Debonding revealed occlusal stability, lack of mobility, lack of fremitus, lack of pain on closure in maximum intercuspation, and no pain in protrusive or excursive border movements. The resolution of occlusal disharmony and optimization of occlusal vertical dental positioning led to resolution of the symptoms for which she had sought treatment. Simply put, no pain, no mobility, and no implants.
While this patient understands that perhaps some of the bone loss on posterior molars may require further treatment in the future, the use of a Talon appliance (Space Maintainers Laboratory [Van Nuys, Calif]) to optimize her occlusion and treat her nocturnal bruxism, along with a conscientious periodontal maintenance program, is all that may be needed to maintain long-term stability.
The postoperative photos taken at an 8-year recall appointment demonstrate this stability and periodontal health (Figures 11 to 13).
References
- Winter R. Upgradeable dentistry: Part 1. Dent Today. 2009;28:82-87.
- Kois DE, Kois JC. Comprehensive risk-based diagnostically driven treatment planning: developing sequentially generated treatment. Dent Clin North Am. 2015;59:593-608.
- Feu D, Menezes FC, Augusto Mendes Miguel J, et al. Orthodontic treatment in the severely compromised periodontal patient. J Orthod. 2012;39:303-313.
- Cho YD, Kim S, Koo KT, et al. Rescue of a periodontally compromised tooth by non-surgical treatment: a case report. J Periodontal Implant Sci. 2016;46:128-134.
Additional Reading
Johal A, Ide M. Orthodontics in the adult patient, with special reference to the periodontally compromised patient. Dent Update. 1999;26:101-108.
Kokich VG. Managing complex orthodontic problems: the use of implants for anchorage. Semin Orthod. 1996;2:153-160.
Mankoo T, Frost L. Rehabilitation of esthetics in advanced periodontal cases using orthodontics for vertical hard and soft tissue regeneration prior to implants—a report of 2 challenging cases treated with an interdisciplinary approach. Eur J Esthet Dent. 2011;6:376-404.
Nemcovsky CE, Beny L, Shanberger S, et al. Bone apposition in surgical bony defects following orthodontic movement: a comparative histomorphometric study between root- and periodontal ligament-damaged and periodontally intact rat molars. J Periodontol. 2004;75:1013-1019.
Ong MA, Wang HL, Smith FN. Interrelationship between periodontics and adult orthodontics. J Clin Periodontol. 1998;25;271-277.
Panwar M, Jayan B, Arora V, et al. Orthodontic management of dentition in patients with periodontally compromised dentition. J Indian Soc Periodontol. 2014;18:200-204.
Dr. Winter, a 1988 graduate of the University of Minnesota School of Dentistry, maintains a private practice in Milwaukee, Wis. He is a Master in the Academy of General Dentistry, a Diplomate in the American Board of Oral Implantology/Implant Dentistry, a Fellow in the American Academy of Implant Dentistry, and a Diplomate in the International Congress of Oral Implantologists. He lectures on the topics of upgradeable dentistry, advanced treatment planning, and general dentistry as a specialty. He can be reached vai email at rick@winterdental.com.
Disclosure: Dr. Winter reports no disclosures.
Related Articles
Maxillo-Mandibular Atrophy: Success Through Interdisciplinary Planning