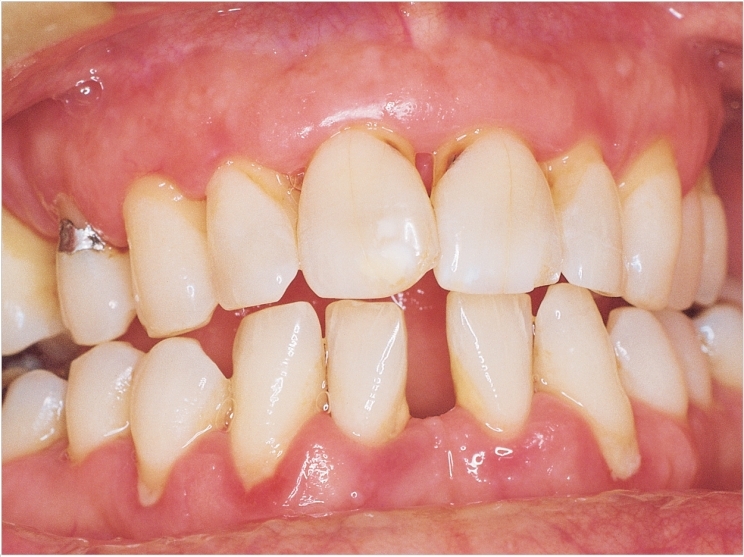
An imbalance between the body’s oxygen-producing free radicals and its antioxidant cells could be why gum disease and chronic kidney disease (CKD) affect each other, according to a study led by the University of Birmingham.
Previous studies have shown a link between the severe oral inflammation caused by gum disease and CKD demonstrating that those with worse inflammation of the gums have worse kidney function.
Also, previous research has shown that patients with CKD and periodontitis experience a drop in survival rates, similar in magnitude to if they had diabetes instead of gum inflammation, suggesting that gum inflammation may casually affect kidney function.
In the latest study, more than 700 patients with chronic kidney disease were examined using detailed oral and full-body examinations including blood samples. The aim was to test the hypothesis that periodontal inflammation and kidney function affect each other and to establish the underlying mechanism that may facilitate this relationship.
The results showed that just a 10% increase in gum inflammation reduces kidney function by 3%. In this group of patients, a 3% worsening in kidney function would translate to an increase in the risk of kidney failure over a five-year period from 32% to 34%. Results also showed that a 10% reduction in kidney function increases periodontal inflammation by 25%.
In contrast to current beliefs that inflammation is the link between periodontitis and other systemic diseases, the researchers found for the first time that, in this group of patients, the effect was caused by a biological process called oxidative stress, or an imbalance between reactive oxygen species and the body’s antioxidant capacity that damages tissues on a cellular level.
“This is the first paper to quantify the casual effect of periodontitis on kidney function and vice versa as well as the first to elucidate the pathways involved,” said lead author Praveen Sharma of the Periodontal Research Group at the University of Birmingham School of Dentistry.
“It showed that even a modest reduction in gum inflammation can benefit renal function. Given the relative ease of achieving a 10% reduction in gum inflammation, through simple measures like correct brushing techniques and cleaning between the teeth, these results are very interesting,” Sharma said.
“We hope that this research paves the way for further studies to see if improvements in kidney function, following periodontal care, translate to longer, healthier life for patients with chronic kidney disease. We would also hope that the hypothesis we have identified could be tested in other groups,” Sharma said.
The study, “Oxidative Stress Links Periodontal Inflammation and Renal Function,” was published by the Journal of Clinical Periodontology.
Related Articles
Periodontitis Linked to Higher Kidney Disease Mortality
Fluoride Linked With Diminished Kidney and Liver Function in Adolescents
P Gingivalis Borrows Growth Molecules from V Parvula to Cause Gum Disease











