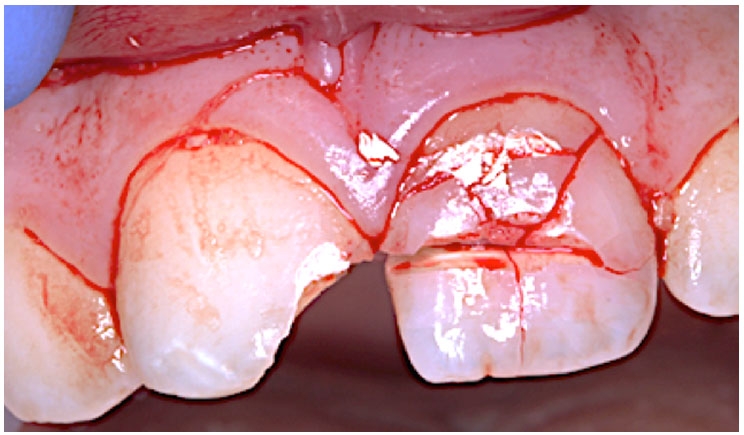
Trauma involving the dentoalveolar region is a frequent occurrence that can result in fractures and displacement of teeth, crushing and/or fractures of bone, and soft tissue injuries including contusions, abrasions, and lacerations. For many traumatic dental injuries (TDIs), immediately provided treatment has a major influence on the prognosis.
Any collision between the face and almost any object can result in a TDI. While many injuries do not need immediate treatment, most patients present as emergencies in dental or medical offices, or at emergency departments. Dentists can improve outcomes for TDI patients by following useful guidelines in assessing them and establishing a treatment plan.
After taking a brief medical history including information on tetanus immunization:
- Assess the patient for any potential head and/or neck injuries.
- Control bleeding, which can usually be controlled by applying pressure. Bleeding from gingival tissues can be controlled if tissues are repositioned and held in place for a few minutes.
- Provide positive reassurance, good anesthesia, and cleansing and debridement of soft tissues. Wipe and rinse soft tissues with water or chlorhexidine.
- Avulsed teeth can sometimes be replanted without causing too much discomfort. If possible, this should be done at the site of the injury as an emergency procedure. Search for the tooth, briefly rinse it in saline, and replant it into its socket. Then seek care with a dental professional.
- A bleeding socket is by far the best storage media. If immediate replantation is not possible or impractical, teeth should be immediately placed in Hanks Balance Salt Solution (HBSS) or milk, and the patient should be rushed to seek professional care for replantation and stabilization.
- Immediately after emergency aid is carried out, it is essential to assess whether serious injuries, including neck and head injuries, have occurred. More specifically, the head and brain should be evaluated for concussion and recorded, and a referral should be arranged for medical treatment if considered appropriate.
Other areas of concern when assessing the patient include determining whether:
- The patient remembers the accident;
- There was a period of unconsciousness;
- The patient has a headache or has had a headache since the accident;
- A headache is worsening over time;
- There has been nausea or vomiting;
- There has been a noticeable behavior change, such as irritability;
- The patient is confused or drowsy;
- There is blurred vision or limited eye movement;
- Pupils are of equal size;
- Speech is slurred;
- Breathing is irregular;
- Fluid is leaking from the ears or nose.
Positive responses need to be noted, and a referral needs to be made immediately for neurological screening. Treatment for shock must also be considered, as well as the possibility of aspiration of teeth or tooth fragments. Also, be sure to check:
- How the injury occurred: TDIs can occur from myriad causes. A moving object can damage the dentition, or the patient can collide with a stationary object. Trauma can occur directly (direct trauma), where an object directly strikes the teeth. Depending on the size and composition of the impacting object, trauma may not necessarily be restricted to the teeth that are obviously affected. Assessment and review of adjacent teeth are recommended and necessary. Compounding and coexisting factors influence the type of trauma sustained and the severity and extent of an injury. None act independently. The injury is a result of the summative effect of these many interrelated factors. While some of these factors may not be applicable to all injuries, it is important to understand the nature of the injury to understand treatment options and the prognosis.
- Whether contact was made with an object or the ground: This is especially important when considering the need for tetanus boosters or antibiotic therapy. If a clean object caused the TDI, the risk of contamination is considerably less than if the injury were sustained by contact with the contaminated ground. The environment where the TDI was sustained is thus important, particularly where soft tissue injuries and avulsions are considered. If soft tissues are contaminated, the tetanus status must be assessed and administration of antibiotics must be considered.
- The type of injury the patient has suffered: Each TDI has its own individual complications and treatment priorities. Some injuries constitute real dental emergencies while others do not. Identifying the injury type and understanding the individual management of each type of injury is one of the first goals in the overall management. Being able to diagnose and use the same classification of dental injuries is critical to determine the most appropriate treatment plan.
- Whether there were any previous injuries to the teeth: Many patients who suffer a dental injury have had trauma previously. If there was previous injury or damage, get details including what treatment was carried out and whether clinical and radiographic records can be retrieved for comparison with current recordings.
- Whether missing teeth or fragments have been identified or recovered: Patients should bring displaced teeth or fragments with them. Re-attachment of the fractured fragment followed by a coronal reconstruction is a clinically acceptable procedure with a good prognosis.
- Whether the tooth color has changed: Color changes may occur in traumatized teeth, so it’s important to note any color changes post-injury.
- Tooth response to sensitivity tests such as hot or cold stimuli: Pulp sensibility testing should be performed at each appointment to determine if an individual tooth response has changed. Even though immature teeth might not respond initially to pulp testing, baseline tests are important for follow-up examination.
- Tenderness to percussion: Percussion testing is a reliable way to assess damage to supporting tissues.
- Whether the tooth should be splinted: As a general rule, all teeth that have been luxated, displaced, or avulsed require a stabilization period. What matters most is that the splints should allow physiological movement of teeth and should be easy to remove. If available, wire and nylon splints have the advantage that small corrections in the occlusion can be made if the teeth are not repositioned exactly in the right position.
- Any orthodontic considerations: When an injury occurs during orthodontic treatment, movement should be delayed or suspended to allow healing of the periodontium. For minor injuries, a period of 3 months is recommended. For more severe injuries involving root fractures, avulsions, intrusions, and lateral luxations, a longer period of waiting is recommended.
Following an injury, it is essential to accurately evaluate all injured tissues and teeth before providing treatment. Poor treatment protocols can have very unsatisfactory outcomes for both patients and practitioners. With proper knowledge and careful examination and treatment, TDIs can be properly treated to preserve children’s smiles. Moreover, with proper education, most injuries can be prevented!
Adapted from: Moule, AJ and Cohenca, N. “Emergency assessment and treatment planning for traumatic dental injuries,” Australian Dental Journal 2016: 61 (suppl 1); 1-18.
Alex Moule, BDSc, PhD, FADI, FICD, FPPS, FIADT, is an endodontist and an associate professor at the School of Dentistry, the University of Queensland, Australia. He is a past president of the Australian and New Zealand Academy of Endodontists. Also, he has been a member of the Australian Society of Endodontology for more than 35 years.
Nestor Cohenca, DDS, FIADT, is an endodontist and a leading expert in dental trauma and pediatric endodontics. He is in private practice at Lakeside Endodontics, Everett, Wash. Also, he is an affiliate professor with the Department of Pediatric Dentistry at the University of Washington School of Dentistry and with Seattle Children’s Hospital. He provides online coursework for dental professionals seeking CE hours as well.
Related Articles
How to Spot Child Abuse Among Your Patients
Exploding E-Cigarette Causes Mouth Injuries
Emergency Room Visits on the Rise for Dental Patients











