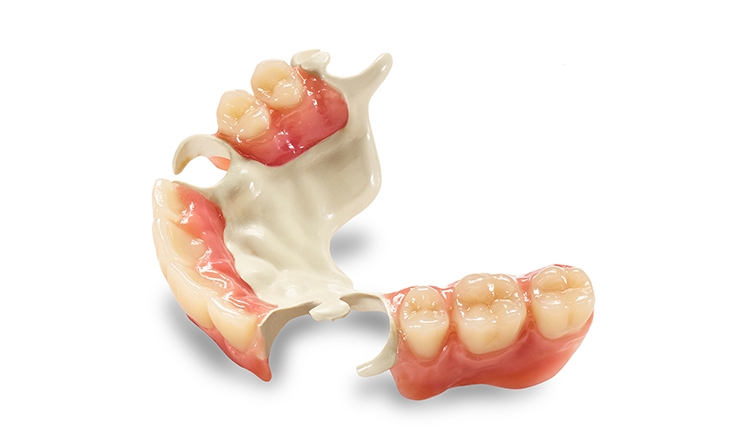
Today, dentures come in a number of forms, from fixed, implanted dentures to removable partial dentures (RPDs). Many denture designs exist, from those that rely on bonding or clasping onto existing teeth to dental implants (fixed prosthodontics) that are permanently affixed within the gums. In any of these cases, the design landscape depends heavily on the nature of the device, as well as the material it’s made from.
Dentures Throughout History
Before diving into present day RPDs, it’s useful to take a look back. Dentures date to as early as 700 BC, when people used human and animal teeth1 to replace missing teeth. These materials remained popular until the 1700s2, with advances in construction and the shaping of ivory.
Wooden teeth were introduced in Japan during the 16th century3. In the 1770s, the first porcelain dentures were introduced4, but they were prone to chipping and appeared to be too white to be aesthetically convincing. Most people still preferred human or even animal teeth. In the 1850s, dentures began being made of Vulcanite, a form of hardened rubber into which porcelain teeth were set4. Following the turn of the 20th century, acrylic resin and other plastics were introduced5.
 |
|
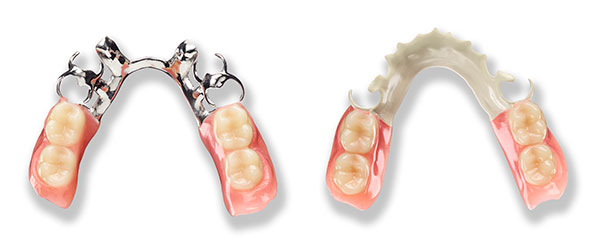
Figure 2. Chrome Cobalt partial denture versus a high-performance polymer partial denture. |
According to “The History of the Characteristic Japanese Wooden Denture” by Moriyama and Hasegawa, the first metal frame dentures were made by Pierre Fauchard in 17283. Since then, there have been significant improvements in RPDs, although the use of metal is still common.
Despite the many advances in healthcare technology, there have not been any significant changes to how RPDs are constructed since the 1950s7. That is to say, after 290 years since that first metal frame denture, innovation in RPDs seems to have halted. This has created an opportunity for a new class of materials to emerge. These materials are changing how patients, clinicians, and dental lab professionals think about RPDs.
A 2017 article in the Journal of Prosthetic Dentistry7 points to the need for innovation in RPDs, highlighting the negative health consequences associated with metal RPDs and the need for advances in both materials and processing for RPDs.
RPDs Today
Unfortunately, while innovation in the RPD space has stalled, the need for removable prosthetics continues to grow at a rapid rate. By 2050, life expectancy is projected to increase by eight years, from today’s 68.6 years to 76.2 years8. As a result, the 65-and-over population is increasing.
According to research from the National Institute on Aging, in the United States alone, this population group is projected to nearly double over the next three decades, from 48 million to 88 million by 20508, meaning the number of individuals in the United States with total or partial edentulism is on the rise9.
The combination of the expanding partially edentulous patient population and the material drawbacks of current denture materials is a call to arms to the dental community to address the complications of current RPDs, low patient satisfaction, and lack of compliance. There is a clear need for a prosthodontic frame solution that supports oral health and encourages patient compliance, resulting in overall better health outcomes after tooth loss or absence.
It’s true that patients now have more options for RPDs than they did generations ago. But to date, none of the available choices has offered a hassle-free solution. Here’s a look at the pros and cons of some of the most popular alternatives on the market:
- Metals: RPD frames have traditionally been constructed of metal alloys6. These frames use metal clasps or supports that secure to existing teeth and ultimately hold the dentures in place. Although it’s a viable and common restoration option, patients with metal frames may experience problems with fit and function, comfort, aesthetics, and/or hygiene. Metal frames can leave a metallic taste and appear aesthetically undesirable for many, which often results in a lack of compliance from patients who don’t like to wear them or take care of them properly7. More critically, they can cause sensitivity and inflammation within the gums, resulting in poor oral hygiene or further tooth loss for patients7. Furthermore, dentist feedback indicates metal RPDs can slowly torque teeth out of the mouth, leading to more tooth loss for the patient, an increased expense, and further restorations10.
- Flexibles: Flexible dentures offer a solution for patients that can be more comfortable, aesthetic, and less invasive than dentures that require metal clasps, adhesive, or implants. In contrast to metal clasps, flexibles cling to the gums on their own with clear material that allows the natural gum color to show through. While more elastic in nature, they can be prone to bacteria buildup11 and require careful daily maintenance. Flexible denture materials also have the drawback of generally low strength11 and creep resistance relative to high-performance polymers. Creep resistance is a material’s ability to withstand deformation or damage under constantly applied stress. The combination of low strength and low creep resistance renders materials typically used for flexible dentures more easily deformed under typical stresses seen in the mouth over long-term use. The consequences of this can lead to poor retention due to clasp or general frame deformation, which can ultimately lead to low patient compliance or the need for another restorative option.
- Acrylic: Acrylic dentures offer a lower-cost RPD solution12. However, they can be easier to damage and more uncomfortable than flexibles, and they can result in sore spots in the mouth. The damage and discomfort of RPDs made from acrylic materials stem from their mechanical properties, a similar issue seen with metals and flexibles for RPDs. To compensate for their low impact strength, acrylic dentures are made thicker in sections, making them bulky12. Although generally stronger than flexibles, acrylic systems don’t have the ideal combination of strength or elasticity to simultaneously provide mechanical stability of the framework and patient comfort, both during insertion and removal and during use.
- High-performance polymers: High-performance polymers are polymer systems designed for very unique application environments, typically those needing materials that have high strength and toughness, high dimensional stability, stable surface properties, and high chemical resistance7. Given the needs of dental devices, high-performance polymers can solve a lot of the issues associated with today’s materials. Specifically for RPDs, these materials can hit the “sweet spot” between metals and flexibles more effectively than acrylic. Metals are too rigid and flexibles are too flimsy, but high-performance polymers are custom-formulated to provide the best of both qualities.
The only high-performance polymer currently on the market specifically indicated for removable partial dentures is Ultaire AKP from Solvay Dental 360. It is 60% lighter than typical metal RPDs13, and this decrease in weight can result in more comfort and improved patient compliance (Figures 1 and 2).
The product is also biocompatible. It is a non-irritant. It is non-pyrogenic, non-mutagenic, and non-catatoxic. And, it does not leach in water ethanol or hexane. Overall, Ultaire AKP is designed to enhance the rigidity of the polymer to be supportive and have a very long lifetime, but at the same time, have some flexibility and elasticity.
One perceived drawback of high-performance polymers may be their relative newness. Many dentists are just learning about the role of high-performance polymers, so their use is not yet widespread. Because of this, many dentists erroneously confuse high-performance polymers with flexibles.
However, the clasp design is different. It’s shorter and thicker, and it’s purposely designed to engage the undercuts. These polymers are bone-like and tooth-supported7, which can be a paradigm shift for many clinicians unwilling to adopt more progressive dental product solutions.
The Future of RPDs
It’s not news that digital dentures are here to stay and will continue to grow in popularity. The material properties of dental devices directly dictate how they can be manufactured or processed. In this context, the drawback of metal frames goes beyond their poor experience for patients, as they are also dramatically inefficient to produce, requiring an immense amount of manual labor (and thus time and money). In contrast, high-performance polymers bring high value to the lab, in addition to their advantageous properties for patients.
High-performance polymers drop seamlessly into the current trend of CAD/CAM resources in dentistry7, resulting in high-quality RPDs that can be efficiently designed and manufactured to meet the precise needs of the patient. More and more labs and clinicians are embracing the streamlined digital denture process to benefit all involved parties. By making the switch, clinicians can provide high-quality RPDs for high-quality patient outcomes.
Although high-performance polymers have been utilized for years in a wide variety of industries like aerospace, automotive, electronics, and healthcare, the realized value of high-performance polymers for the dental industry is currently in its infancy. The true potential of these materials to revolutionize restorations has yet to be fully experienced.
The chemical zoology of high-performance polymers is broad. Chemistries can be used alone or in conjunction with various fillers, which can provide needed functionality to the formulation. This combination of chemical breadth and depth creates a true formulation landscape that has the potential to unlock unique design features that could lead to improved patient oral health, while also further increasing efficiencies to manufacture these devices through streamlined workflows.
The key attributes of high-performance polymers—lightweight, strong, durable, tough, and providing ease of manufacturing—address many of the needs of the dental industry, benefitting both clinicians and patients. These polymer systems are only the tip of the iceberg in terms of innovation in the dental space for the foreseeable future.
References
1. Donaldson JA. The use of gold in dentistry: an historical overview. Part I. Gold Bulletin. 1980;13:117-124.
2. Waterloos and its dental legacy. Br Dent J. 2015; 218(12).
3. Moriyama N, Hasegawa M. The history of the characteristic Japanese wooden denture. Bull Hist Dent. 1987;35:9-16.
4. Wynbrandt J. The Excruciating History of Dentistry: Toothsome Tales & Oral Oddities from Babylon to Braces. New York, NY: St. Martin’s Griffin; 2000.
5. Eden SE, Kerr WJ, Brown J. A clinical trial of light cure acrylic resin for orthodontic use. J Orthod. 2002;29:51-55.
6. Becker CM, Kaiser DA, Goldfogel MH. Evolution of removable partial denture design. J Prosthodont. 1994;3:158-166.
7. Campbell SD, Cooper L, Craddock H, et al. Removable partial dentures: the clinical need for innovation. J Prosthet Dent. 2017;118:273-280.
8. He W, Goodkind D, Kowal P; US Census Bureau. An Aging World: 2015. International Population Reports. Washington, DC: US Government Publishing Office; 2016.
9. Levin L. Dealing with dental implant failures. J Appl Oral Sci. 2008;16:171-175.
10. Dula LJ, Ahmedi EF, Lila-Krasniqi ZD, et al. Clinical evaluation of removable partial dentures on the periodontal health of abutment teeth: a retrospective study. Open Dent J. 2015;9:132-139.
11. Vojdani M, Giti R. Polyamide as a denture base material: a literature review. J Dent (Shiraz). 2015;16(suppl 1):1-9
12. Wilson VJ. Acrylic partial dentures—interim or permanent prostheses? SADJ. 2009;64:434-440.
13. Solvay (data on file).
Dr. Murphy is a technology manager at Solvay Dental 360. He began his career at the Solvay Group in 2009 and joined Solvay Dental 360 in January 2017. He received his doctorate in 2007 from the Polymer Science and Engineering department at the University of Massachusetts, Amherst. In his work at Solvay Dental 360, he is at the forefront of researching and developing new solutions for dental labs, dentists, and patients.
Related Articles











