Abutment-screw loosening has been shown to be the most common dental implant prosthetic complication, accounting for up to 33% of all post-implant prosthodontic issues.1 The incidence of screw loosening with single implant crowns has been reported as high as 59.6% within 15 years of placement.2 Screw loosening causes many complications that may contribute to crestal bone loss, screw fracture, implant fracture, or implant failure. Although screw loosening may occur in any area of the oral cavity, studies have shown the overwhelming majority of loosened screws occur in the maxillary and mandibular molar areas (~63%) and with single implant crown restorations (~75%).3
ETIOLOGY
To understand why a screw becomes loose, one must understand the engineering principles of a typical screw joint. A screw joint is defined as 2 components that are held together by a screw (ie, an abutment and implant). When a screw is tightened (torque), it will elongate, which produces tension or preload within the screw joint. The preload exerts a force that leaves the screw joint in compression and promotes a spring-like effect. The preload applied also has an associated elastic recovery that is transferred to the abutment and implant, pulling them together and creating a clamping force (ie, equal in magnitude to the elongation and elastic recovery).4 If the elastic recovery of the screw is exceeded (ie, via overtightening or excessive forces), the screw will loosen. The amount of preload force applied to a screw is dependent on screw type, size, material, and manufacturer and is usually recommended to be between 60% to 75% of the yield strength of the screw material.5
For a screw to remain tight, the clamping force must be greater than the separating forces. Most often, these separating forces are in the form of external forces that act on a screw joint. Although these forces are termed joint-separating forces, they are the same forces that place the implant at risk for implant failure, crestal bone loss, and component fracture. When the external joint-separating forces are greater than the force holding the screws together (the clamping force), the screw will become loose. These external forces may result from many factors, including parafunction, excessive crown height, masticatory dynamics, prosthesis position in the dental arch, and opposing dentition (Table 1). In addition, conditions that magnify or increase external forces include cantilevers, angled loads, and poor occlusal designs.
 |
 |
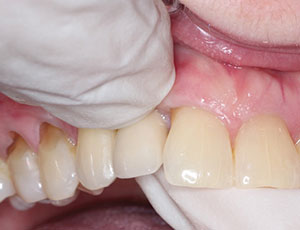
| Figure 1. Buccal-Lingual Plate Compression: To determine implant body mobility, bimanual pressure should be applied over the buccal and lingual cortical plates. | Figure 2. Crown Mobility: To determine if the mobility is originating from the abutment screw, pressure is applied to the crown in a buccal-lingual direction. |
Occlusal forces have been shown to be one of the most common causes resulting in changes of the preload of the abutment screws.6 These forces may result from off-axis contacts, interproximal contacts, and nonpassive frameworks. When these forces exceed the clamping force that holds the screw unit together, screw loosening will likely occur in 2 stages: Initially, slippage of the screw joint occurs, which contributes to the release of the screw’s preload. Secondly, further loosening occurs from a continuous reduction of preload, which results in the complete loss of the screw joint junction (Table 2).
 |
PREVENTION
To maintain the health and longevity of the implant prosthesis, the clamping force must be maintained within the screw joint system. Therefore, to prevent screw loosening, a structured protocol must be adhered to (Table 3). The ideal torque force (preload) applied to an abutment screw varies by manufacturer and may range from 10 to 35 N/cm. This preload is determined by many variables, including the screw material, screw head design, abutment material, and abutment surface characteristics.
Another factor that plays a role in screw loosening is the settling effect. The settling effect results from the non-smooth surfaces (roughness) of the components and is significant in maintaining the stability of the screw. As a result of this inherent roughness, opposing surfaces are never in complete contact. Thus, settling will naturally occur as the rough spots are flattened under pressure, which relaxes the preload. This loss of preload or embedment relaxation has been shown to be approximately 2% to 10% of the initial preload and occurs within the first few seconds or minutes after tightening. To counteract this embedment relaxation, the screw should ideally be retightened after 5 to 10 minutes in order to regain the preload lost due to settling.7
These factors play a significant role in screw tightening a multi-unit fixed implant prosthesis. A proper sequence and technique is crucial to obtain the correct torque and passive prosthesis. The torque should be applied incrementally to all screws, thus avoiding one screw being fully tightened. This is based on the fact that a multi-unit prosthesis is unlikely to be completely passive. A non-ideal tightening sequence will lead to either an insufficient or excessive amount of torque placed onto a specific screw thread.
TREATMENT
Initially, when confronted with a mobile prosthesis, it is imperative to determine if the mobility is a result of screw loosening or the actual implant being mobile (implant failure).
Implant Movement
Mobility of the implant indicates failure of the implant and necessitates immediate removal. A diagnostic test should include compression of the buccal and lingual cortical plates to determine the presence of pain (Figure 1). If pain is present, it is most likely a nonintegrated implant. Radiographic evaluation should be completed to look for signs of failure.
Abutment Screw Movement
To verify if the abutment screw is loose, 2 diagnostic tests may be used (Figure 2). When the crown is moved in a buccal-lingual position, if no pain is present, this most likely is the result of the abutment screw being loose. If pain does exist, it is most likely the non-integration of the implant that is the origin of the discomfort. If this occurs, further evaluation should be completed to rule out tissue impingement, which could be conclusive for abutment screw loosening.
In most cases, an abutment screw loosening may be corrected without doing irreversible damage to the existing prosthesis. Caution should be exercised in attempting to remove a cemented crown from a mobile abutment with conventional crown-removal techniques (eg, with a crown bumper or by sectioning the crown). The impact force that is applied to the mobile crown is dissipated because of the loose screw. This may result in damage to the internal threads of the implant body. Additionally, in poorer bone densities, overzealous use of a crown remover may result in a loss of bone-implant interface.
 |
When cutting off the crown, one needs to be careful, as, in most cases, it is difficult to determine the cement location because sectioning the crown too deep may cause damage to the abutment, abutment screw, or implant body. The safest and most predictable treatment option to correct abutment screw loosening and retain the existing crown is accomplished by making an occlusal access and transforming the cement-retained crown into a screw-retained crown via an occlusal access hole (Figure 3) (Table 4). In situations where the access hole is through the facial aspect of the prosthesis (ie, anterior crowns), the crown will need to be removed and a new crown fabricated.
CLOSING COMMENTS
Screw loosening is a recognized complication in implant dentistry. The reliability and stability of the abutment-implant screw joint connection is an essential prerequisite for long-term success of the implant and prosthesis. This is a complication that most implant clinicians will be confronted with in their careers. By having a strong understanding of the biomechanical principles responsible for this complication, the clinician will be able to prevent and effectively manage screw loosening.
References
- Kourtis SG, Sotiriadou S, Voliotis S, et al. Private practice results of dental implants. Part I: survival and evaluation of risk factors—Part II: surgical and prosthetic complications. Implant Dentistry. 2004;13:373-385.
- Jemt T. Single implants in the anterior maxilla after 15 years of follow-up: comparison with central implants in the edentulous maxilla. Int J Prosthodont. 2008;21:400-408.
- Kirov D, Stoichkov B. Factors affecting the abutment screw loosening. Journal of IMAB–Annual Proceeding (Scientific Papers). 2017;23:1505-1509.
- Marinucci T. Influence of Repeated Tightening and Loosening of the Prosthetic Screw in Micromovements Abutment/Implant [master’s thesis]. Coimbra, Portugal: University of Coimbra; 2013.
- Bickford JH. Introduction to the Design and Behavior of Bolted Joints: Non-Gasketed Joints. 4th ed. Boca Raton, FL: CRC Press; 2008:137-169, 293-352, 391-421.
- Breeding LC, Dixon DL, Nelson EW, et al. Torque required to loosen single-tooth implant abutment screws before and after simulated function. Int J Prosthodont. 1993;6:435-439.
- Winkler S, Ring K, Ring JD, et al. Implant screw mechanics and the settling effect: overview. J Oral Implantol. 2003;29:242-245.
Dr. Resnik is a leading educator, clinician, and researcher in the field of prosthodontics and oral implantology. He is a graduate of the University of Pittsburgh, with a specialty degree in prosthodontics, a surgical fellowship in oral implantology, and a master’s degree in radiology. He is a clinical professor of oral implantology at Temple University in Philadelphia, a clinical professor at the University of Pittsburgh (Graduate Prosthodontics), a staff member at Allegheny General Hospital in Pittsburgh, and surgical director at the Misch International Implant Institute in Taylor, Mich. He maintains a private practice in Pittsburgh limited to oral implantology. He can be reached via email at resnikdmd@gmail.com.
Disclosure: Dr. Resnik reports no disclosures.
Related Articles











