More and more patients in our practice are expressing a strong desire for a “Hollywood” smile. When delivering cosmetic smile enhancements, be it from utilizing minimal-prep porcelain veneers or durable zirconia crowns, there are 3 basic principles to consider: aesthetics, symmetry, and function. Cohesively, these principles ensure mindfulness pertaining to the size, shape, contour, and positioning of teeth. Equally as important is gingival architecture; uniform, pink gums are a sign of a healthy smile and are also highly desirable.
The restorative team, when using these guiding ideologies for each smile makeover, can successfully restore a smile to its proper form, function, and appearance. This article demonstrates the significance of utilizing a prosthetically driven treatment plan when restoring missing teeth in the anterior maxilla with dental implants to achieve an aesthetic smile makeover.
Case REPORT
Diagnosis and Treatment Planning
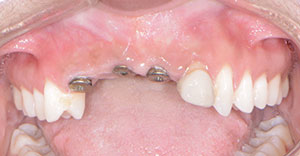
A 36-year-old female patient presented to the practice and expressed dissatisfaction with her smile (Figure 1). This unhappiness was the result of a car accident 7 years prior, during which the patient lost her maxillary anterior teeth (Nos. 6 to 9) and tooth No. 10 was fractured. Restorative dental work included endodontic treatment, followed by a core and crown restoration as well as a removable partial denture in this area of the mouth. Approximately 2 years prior to this initial consultation appointment, another oral health professional had placed 3 dental implants in tooth position Nos. 6, 8, and 9 with the end goal of delivering a fixed partial denture. However, during this process, the dentist was unable to provide a satisfactory fixed provisional restoration, which led the patient to our practice.
Initial diagnostic evaluation consisted of a series of digital images with study casts, a centric relation bite record, and necessary radiographs. The CS 8100 (Carestream Dental) was used to obtain CBCT images to properly evaluate the bone surrounding the previously placed dental implants. Clinical examination revealed good keratinized tissue and bone surrounding the dental implants. However, tooth No. 10 was somewhat flared facially, with recession exposing the gingival margin of the crown restoration. Radiographically, there was a periapical lesion at the apical region of the tooth.
 |
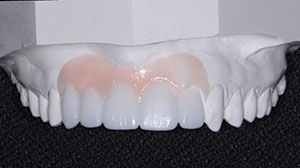 |
| Figure 1. Preoperative retracted view. | Figure 2. Diagnostic wax-up. |
 |
 |
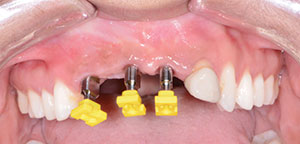
| Figure 3. Implant impression posts. | Figure 4. Impression and bite relations. |
 |
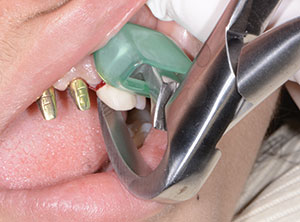 |
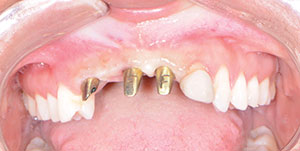
| Figure 5. CAD/CAM abutments. | Figure 6. Atraumatic extraction. |
Considerations regarding the incorporation of tooth No. 10 were discussed with the patient. Respect was also given to its position within the arch, the existing crown restoration, and the failed endodontic treatment. Ultimately, it was recommended that the dental laboratory fabricate a diagnostic wax-up illustrating the result, should tooth No. 10 be removed. This would allow for a 5-unit fixed partial denture (FPD), extending from teeth Nos. 6 through 10 with 3 abutments and 2 pontics. DenMat Dental Lab (Lompoc, Calif) was chosen specifically based on its expertise in anterior aesthetic combination cases.
To develop a treatment plan, full-arch dental impressions (Silginat [Kettenbach LP]) were taken and sent to the dental laboratory. Due to the alveolar defect present in the ridge, it was suggested that the laboratory add pink wax in the gingival area, where it would be replaced with pink porcelain in the final restoration (via FP3). The FP3 dental implant prosthesis, created by Dr. Carl Misch, allows for the re-establishment of proper function, aesthetics, lip support, and phonetics.1 This restoration assists clinicians in achieving their patients’ desired outcomes in the aesthetic zone.
Upon seeing the diagnostic wax-up (Figure 2), the patient was thrilled with the potential outcome of her case. She immediately scheduled her appointment for the recommended treatment.
Starting with three 3.3-mm NC implant (BLT [Straumann]) level impressions (Figures 3 and 4), the technicians virtually extracted tooth No. 10, fabricated custom CAD/CAM abutments (teeth Nos. 6, 8, and 9), and fabricated a polymethylmethacrylate (PMMA) 5-unit fixed provisional restoration. This provisional was designed as an FP1 restoration to determine if it would suffice in the aesthetic zone as well as to try to further enhance tissue contour.2
Clinical Protocol
The patient presented to the office after the abutments and provisional restoration had been delivered from the dental laboratory. Anesthetic was administered (Xylocaine, 1:100,o00 epi), and treatment was initiated.
First, the healing caps were removed from the dental implants and replaced with gold-anodized, CAD/CAM, custom abutments. The abutments were seated and torqued with a torque wrench at 25 Ncm, per the manufacturer’s instructions (Figure 5). Then access openings were sealed with Teflon tape. It is important to note that the dental laboratory designed the abutments so that the facial margins were 0.5 mm apical to the free gingival margin to avoid the display of metal.
Next, tooth No. 10 was extracted using Physics Forceps (GoldenDent) (Figure 6). By using these forceps and the associated technique, tooth No. 10 was extracted with great care, so as not to disrupt the surrounding tissues (Figure 7). A curette (Hartzell [DenMat]) was used to debride granulation tissue from the socket. An alloplastic material (OsteoGen [Impladent Ltd]) was then inserted and packed into the socket (Figure 8), ensuring that it was in tight contact with bony walls. Then the PMMA provisional restoration (Figure 9) was cemented with a temporary cement material (ETC Temporary Cement [Parkell]), and the patient was instructed on how to care for it during the 3-month healing period (Figure 10).
 |
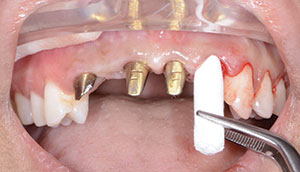 |
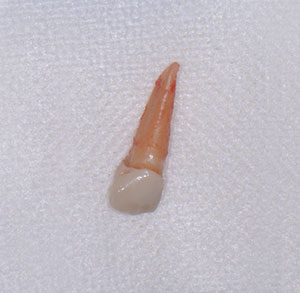
| Figure 7. Extracted tooth. | Figure 8. Socket preservation. |
 |
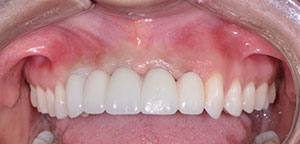 |
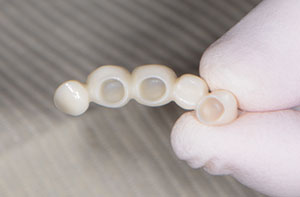
| Figure 9. Provisional restoration. | Figure 10. The provisional, seated. |
 |
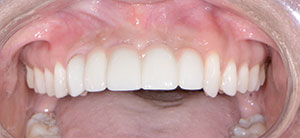 |
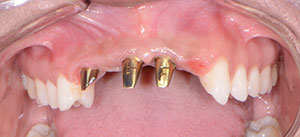
| Figure 11. Abutments and the healed extraction site. | Figure 12. Postoperative retracted view. |
Upon satisfactory healing, the patient returned to the dental practice 3 months later to capture impressions for the definitive FPD restoration. Using a vinyl polysiloxane material (Panasil [Kettenbach LP]), a full-arch impression was taken of the maxillary arch using a traditional crown and bridge technique. This impression, along with bite relations and the opposing model, were forwarded to the dental laboratory team with instructions to fabricate the FPD restoration with LumiZir (DenMat Dental Lab) zirconia due to its aesthetics and strength.3-5 LumiZir full-contour crowns are fabricated from the strongest, most translucent zirconia on the market and offer more than 1,150 MPa flexural strength. Thanks to these features, this restoration offered the benefits of unmatched strength and lifelike aesthetics.
Laboratory Considerations
After reviewing the digital clinical images, the diagnostic wax-up, and the patient’s feedback, it was determined that the definitive restoration would be much more aesthetic if it were designed as an FP3 restoration (similar to the wax-up). This would ensure that pink porcelain would be used to fill in the gingival embrasures, thereby creating a more natural appearance.
DenMat Dental Lab is a specialized dental laboratory that’s completely focused on anterior aesthetic cases. The lab is equipped with the latest CAD/CAM technology and employs a team of highly trained dental technicians who consult with the dental professional at each phase of treatment. This leads to highly predictable and aesthetic outcomes, no matter how complex the case.
Delivery Appointment
Before try-in of the definitive restorations to verify fit, function, and aesthetics, the provisional restorations were removed using an Easy Pneumatic Crown and Bridge Remover (Dent Corp). Remaining cement was cleaned off the abutments (Figure 11), and the FPD was tried in for evaluation. Using retractors first, the patient was shown the retracted view, followed by a full-face view, for acceptance of the definitive restoration.
With the patient’s approval, the cementation process was initiated. Implant cement (Infinity SE [DenMat]) was used to cement the FPD restoration (Figure 12).
Closing Comments
In cases such as this, it is important to look at the entire smile when restoring it to proper aesthetics, form, and function. The process should begin with a diagnostic wax-up, which is an invaluable tool for planning and communicating with patients about the proposed treatment plan. As dental providers, our goal should be to first listen to our patients’ needs and then to guide them to the appropriate solution using our knowledge and experience.
Acknowledgment:
Special thanks to Randy Berry and his team of dental technicians at DenMat Dental Lab, Lompoc, Calif.
References
- Misch CE. Contemporary Implant Dentistry. 3rd ed. St. Louis, MO: Mosby Elsevier; 2007:97-101, 147-159.
- Nash RW. Treatment planning with modern materials. Compend Contin Educ Dent. 1997;18:1064-1071.
- McLaren EA. All-ceramic alternatives to conventional metal-ceramic restorations. Compend Contin Educ Dent. 1998;19:307-310.
- van Dijken JW. All-ceramic restorations: classification and clinical evaluations. Compend Contin Educ Dent. 1999;20:1115-1124.
- Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing; 1994:108.
Dr. Nazarian maintains a private practice in Troy, Mich, with an emphasis on comprehensive and restorative care. He is a Diplomate in the International Congress of Oral Implantologists, and his articles have been published in many of today’s popular dental publications. Dr. Nazarian is the director of Ascend Dental Academy. He has conducted lectures and hands-on workshops on aesthetic materials and dental implants throughout the United States, Europe, New Zealand, and Australia. He can be reached at (248) 457-0500 or via the website aranazariandds.com.
Disclosure: Dr. Nazarian reports no disclosures.
Related Articles
Implementing a Systematic Digital Workflow
Predictably Achieving Aesthetics and Strength
Systematic Approach to Full-Mouth Reconstruction











