Most temporomandibular joint (TMJ) patients aren’t as obvious as one would think. In fact, many of the symptoms that fall underneath the TMJ disorder umbrella don’t even appear to be associated with a jaw issue, but are a direct result of a destructive bite or poor jaw posture.
We’re taught in dental school to look for clicking or popping in the TMJ and usually only recommend treatment if pain is associated when chewing. Sometimes if we intervene early enough, a properly made occlusal guard to be worn at night can give a patient relief and combat muscular head and neck tension.
But when is a bite guard not enough? Many patients suffer with more severe symptoms like headaches, migraines, neck pain, tinnitus (ear ringing), and even vertigo (dizziness) without theirdentists even being aware of it.These TMJ patients do not believe these symptoms are dentally related, so they never mention them to their dentists.
Not all TMJ patients are the same, and recognizing them can sometimes be quite difficult. However, there are some techniques and approaches to help identify these patients and find them the help they are looking for.
The Case Study
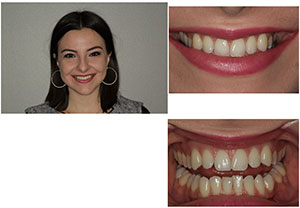
This healthy 24-year-old female patient presented to me for treatment of her potential TMJ disorder (Figure 1).
Despite her healthy dentition, attractive facial appearance, and age, she was suffering from the following:
- Daily headaches
- Migraines once or twice a week
- Severe neck pain
- Ear congestion on the left side, affecting her hearing
- Clicking and popping of her left TMJ
- Continual vertigo episodes
Our diagnostic workup included a comprehensive exam, full-mouth series of x-rays, 3-D CBCT, diagnostic photographs, diagnostic impressions, and a very detailed neuromuscular questionnaire. Based on the patient’s symptoms, lower midline shifted to the left, and depressed curve of spee, we suspected a torqued mandibular position compressing the condyles and resulting in muscular distress.
 |
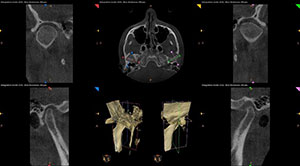 |
| Figure 1. A healthy 24-year-old female presented with severe TMJ symptoms. | Figure 2. The 3-D cone beam view revealed the posteriorized position of both condyles. |
 |
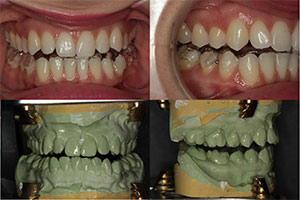 |
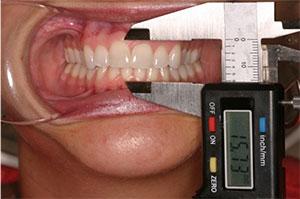
| Figure 3. Shimbashi measurements, noting the distance from the CEJ to the CEJ of the maxillary and mandibular central central incisors, should be between 17 and 21 mm in stable dentitions. | Figure 4. After the bite registration was complete, the case was mounted to the new bite and an anatomically correct orthotic was fabricated to support this mandibular position. |
This posteriorized position of both condyles was confirmed and evident in the 3-D cone beam view (Figure 2).There was also significant beaking of the left condyle that demonstrated the bony changes it has undergone due to its destructive positionand dysfunction.
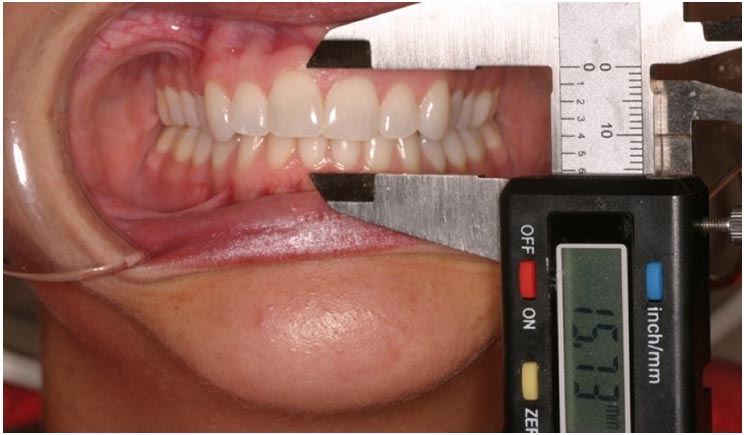
Another measurement that is very helpful in determining the stability of a bite is called the Shimbashi number. This measurement from the CEJ to CEJ of the maxillary and mandibular central incisors in stable dentitions should be between 17 and 21 mm. The Shimbashi number was established to indicate an ideal relationship between the upper and lower jaws.
When there is an optimal position of the lower jaw relative to the upper jaw, the muscles that are connected to them will also be at their optimal length and can function ideally. Any measurement less than 17 mm is considered a deficient vertical dimension (Figure 3). Although our patient did not appear to have a severe overbite, her Shimbashi measurement was only 14.7 mm.
How to Determine a Comfortable Jaw Position
To predictably support the patient in a comfortable and asymptomatic jaw posture, we utilized computerized instrumentation with surface electromyography (EMG). The K7 instrumentation from Myotronics allowed us to establish a baseline to record the location of her habitual bite and indicate where her new mandibular position needed to be according to her physiologic rest position, proper path of closure, and the EMGs of her jaw musculature.
After establishing the baseline, a Myotronics Myomonitor ulf-TENS unit was used to pulse her muscles into a more relaxed, un-torqued state to establish the physiologic rest position of her mandible. At this point, the proper path of closure was established using the computerized mandibular scanning jaw-tracking capabilities of the K7 with simultaneous monitoring of the patient’s EMGs.
 |
 |
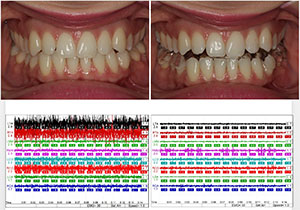
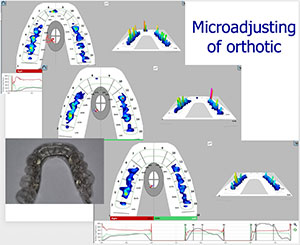
| Figure 5. Surface electromyography in the patient’s habitual occlusion was compared to her surface electromyography occluding in her orthotic after the second adjustment. | Figure 6. The patient’s overall bite into her orthotic became more uniform and balanced during the course of treatment. |
 |
 |
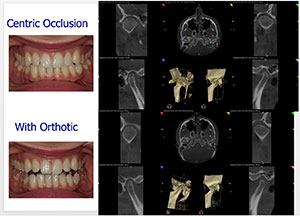
| Figure 7. After resolution of symptoms to the patient’s satisfaction, verification of stability of path of closure, and calm facial musculature, the patient had completed this phase of treatment. | Figure 8. A 3-D cone beam scan with the patient in occlusion with her orthotic was taken to compare the final condylar position in the glenoid fossa to her habitual centric occlusion. |
Once this jaw position was determined, this ideal maxillary-mandibular relationship was registered with Kettenbach’s Futar rigid bite material. After the bite registration was complete, the case was mounted to the new bite and an anatomically correct orthotic was fabricated to support this mandibular position (Figure 4).
For phase 1 therapeutic treatment in our TMJ cases, this mandibular repositioning orthotic is worn 24 hours a day, including eating with it, for a minimum of four months. During this time, healing of facial and neck muscles will occur, inflammation of the TM joints will be reduced, and the body will adapt to this comfortable jaw posture. This step is critical to stabilize the patient and ensure the patient is symptom-free before moving on to any phase 2 definitive treatment.
All treatment performed in phase 1 orthotic therapy is completely reversible. Patients are given the opportunity to either continue with the orthotic as a nighttime device and limited daytime use as needed, or consider a permanent orthodontic or restorative change in their dentition.
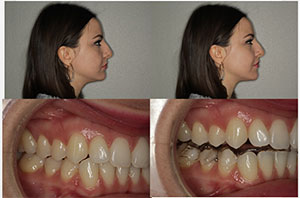 |
| Figure 9. Treatment resulted in improvements in her profile, lower facial height, and improved head posture. |
Letting the Body Guide Orthotic Adjustments
Over the next four months, three coronoplasty adjustments were performed with TENS on the removable mandibular orthotic. As the body unwinds, and the jaw musculature relaxes, the mandible is allowed to stabilize as interferences are removed in the orthotic.
The K7 instrumentation was used at all adjustment appointments to ensure there was no increase in EMGs when the patient was biting into her orthotic. Chew cycle recordings were also made to identify and remove any working or balancing interferences during function.
Figure 5 shows the comparison of surface electromyographyin the patient’s habitual occlusion versus occluding in her orthotic after the second adjustment.As can be seen, the patient’s musculature is significantly calmer in her orthotic position, resulting in continued reduction of her symptoms by 50% at the second month.
Final Stabilization of the Patient
At her fourth and final adjustment appointment, we utilized TekScan Digital Bite Analysis instrumentationfor micro adjustment of her orthotic.The “T Scan” shows prematurities throughout the occlusion at the 20-µm level. (Articulating paper is limited at about the 80-µm level.)This coronoplasty is truly considered “micro-adjusting,” and many times it is essential for honing in a very difficult TMJ patient.See the scans in Figure 6 as the overall bite into the patient’s orthotic became more uniform and balanced.
After less than five months, the patient reported all symptoms reduced 90% to 100%. Her left TMJ popping and clicking were gone while she wore the orthotic, she had no migraines or vertigo episodes,and she stated she felt great.After resolution of symptoms to her satisfaction, verification of stability of path of closure (Figure 7), and calm facial musculature, the patient had completed this phase of treatment.
At the end of orthotic therapy, we took a 3D cone beam scan with the patient in occlusion with her orthotic to compare final condylar position in the glenoid fossa to her habitual centric occlusion (Figure 8). With the orthotic in place, you can see how decompressed the condyles are, allowing proper functional space for the articular disc and associated structures.
Knowing Who We Can Help
Proper identification of candidates for this treatment and utilizing the latest dental technology and techniques not only results in a successful outcome, it also minimizes patient time and maximizes patient results.
This treatment is extremely predictable due to the objective data the K7 computerized jaw tracking and surface electromyography provides. It allows us to recognize patients who may not have the standard TMJ occlusal signs and head and neck characteristics we usually see in TMJ disorders.
And although this patient appears to fall within the normal limits of a stable dentition and facial appearance, you can even see the improvement in her profile, lower facial height, and head posturewith her orthotic(Figure 9).
Many patients do not realize what “healthy” is or what comfort feels like until we introduce them to a relaxed head and neck posture. They may be suffering from myriad symptoms that are the result of an undiagnosed TMJ disorder. Taking the time to ask the right questions, listening to our patients, and using diagnostic technologies available to us could help give these patients solutions for relief.
Dr. Haddad received his BA in psychology from the University of Michigan in 1997. He completed his dental education at the University of Michigan in 2001. He is a fellow of the Las Vegas Institute for Advanced Dental Studies. He is also an independent consultant reviewing new products and technology for Dental Advisor. Dr. Haddad lectures nationally on cosmetic dentistry, TMJ and sleep disorders, and practice marketing. If you have any questions or would like further information, contact him at drhaddad@rochesteradvanceddentistry.com or (248) 656-2020.
Related Articles
TMD Treatment May Alleviate Meniere’s Disease











