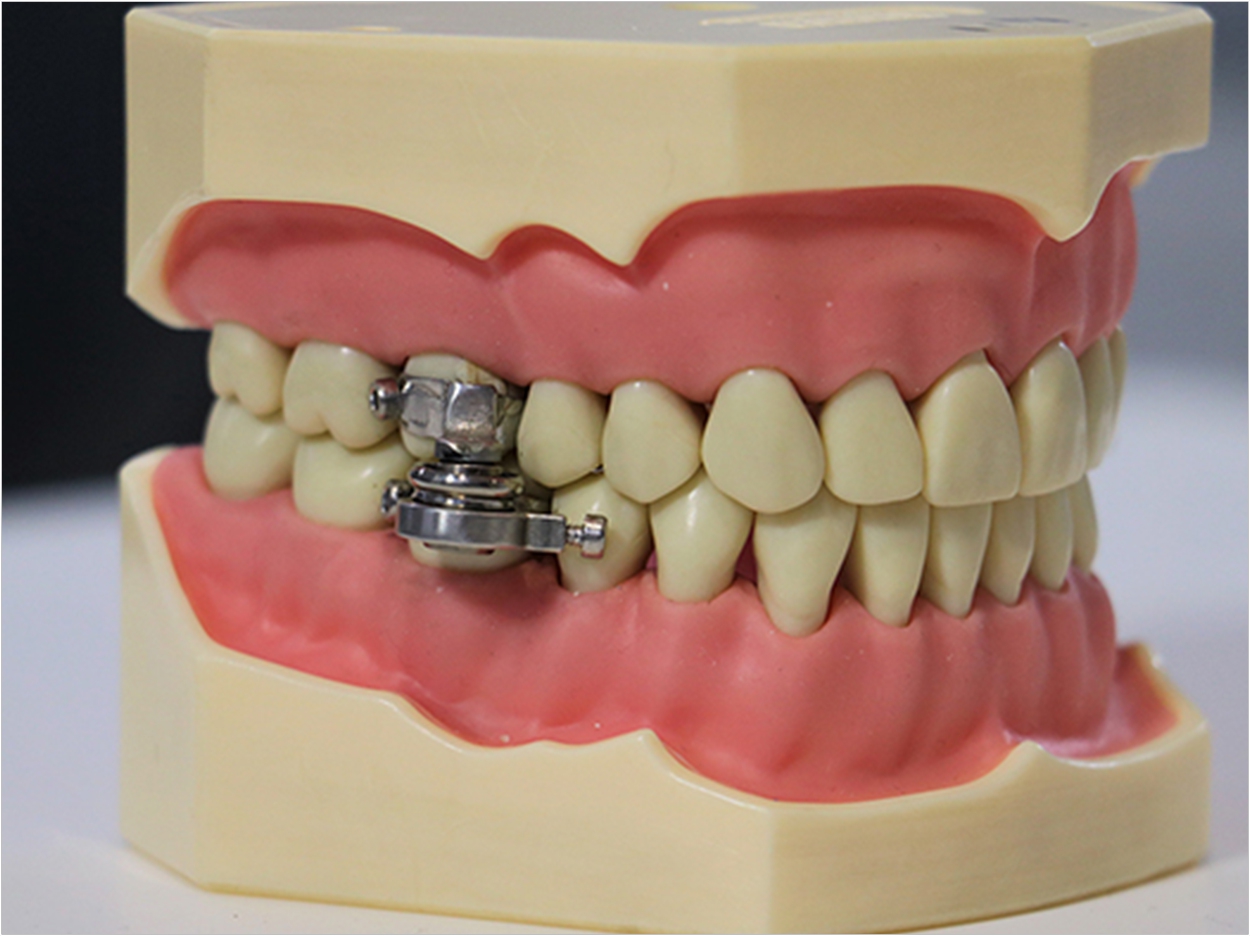
Researchers at the University of Otago and in the United Kingdom have developed an intraoral device designed to help people lose weight.
Fitted by a dental professional to the upper and lower back teeth, the DentalSlim Diet Control uses magnetic devices and unique custom manufactured locking bolts to restrict mouths to a 2-mm opening. Patients will be limited to a liquid diet, but the device doesn’t interfere with speaking or breathing.
Participants in a Dunedin-based trial lost an average of 6.36 kg in two weeks and were motivated to continue with their weight loss journey.
Lead researcher Paul Brunton, pro-vice chancellor with University of Otago Health Sciences, said the device will be an effective, safe, and affordable tool for people battling obesity. Users can release it in case of an emergency, and it can be repeatedly fitted and removed.
“The main barrier for people for successful weight loss is compliance, and this helps them establish new habits, allowing them to comply with a low-calorie diet for a period of time. It really kickstarts the process,” Brunton said.
“It is a noninvasive, reversible, economical, and attractive alternative to surgical procedures,” Brunton continued. “The fact is, there are no adverse consequences with this device.”
The researchers noted recent studies finding that 1.9 billion adults worldwide are overweight, and 650 million are obese. Also, being overweight or obese results in about 2.8 million deaths a year. Approximately 57% of the world’s adult population will be overweight or obese by 2030, the researchers continued.
“In addition, psychological symptoms may be present, including embarrassment, depression, and loss of self-esteem, and obese people may suffer eating disorders together with stigmatization and discrimination,” Brunton said.
The tool could be particularly helpful for those having to lose weight before they can undergo surgery and for diabetes patients for whom weight loss could initiate remission, the researchers said.
Bariatric surgery may play a major role in the management of morbid obesity, the researchers continued, but it cannot be relied upon to manage the global epidemic. It costs about $24,000, and patients “live with the consequences of that for life, which can be quite unpleasant,” Brunton said.
The practice of surgically wiring people’s jaws shut became popular in the 1980s, but it came with risks. Vomiting brought with it the risk of choking, and after nine to 12 months, the patients developed gum disease. In some cases, there were continuing issues with restriction of jaw movement, and some developed acute psychiatric conditions.
“Alternative strategies are required which may obviate surgery, or which reduce weight prior to surgery and so make it easier and safe,” Brunton said.
“The beauty of it is that once patients are fitted with the device, after two or three weeks, they can have the magnets disengaged. They could then have a period with a less restricted diet and then go back into treatment,” Brunton said.
“This would allow for a phased approach to weight loss supported by advice from a dietician allowing long-term weight loss goals to be realized,” he said.
Patients are given a tool to open the device in an emergency, but none of the study participants needed to use it. While they all described the device as tolerable, the design has since been improved, making it smaller to improve functional comfort and aesthetics.
“Overall, people felt better about themselves, they had more confidence, and they were committed to their weight loss journey,” Brunton said.
“It’s hard yards. Patients who really want to do this have to be committed. But for those people who are really struggling, and let’s face it, that’s millions of people across the world, this is a way of getting them back into normal lifestyle diet habits by really pump-priming the process,” said Brunton. “This could actually help a lot of people.”
The study, “An Intraoral Device for Weight Loss: Initial Clinical Findings,” was published by BDJ.
Related Articles
26% of Americans Aren’t Familiar With Obstructive Sleep Apnea
Ultra-Processed Food Reduces Bone Quality
Oral Health, COVID-19, and Systemic Considerations












