Dental implants have become a mainstay in the prosthetic rehabilitation of edentulous and partially edentulous patients.1,2 In spite of ongoing improvements in materials, techniques, and implant design, implant failure is a notable problem.3 The 2 most important causes of implant failure are peri-implantitis and a lack of osseointegration.3 There has been an increased incidence of peri-implant inflammations in the last 10 to 12 years, and it is one of the most frequent complications affecting the hard and soft tissues surrounding the implant.4-7 The risk factors for the development of peri-implantitis include smoking, a history of periodontitis, soft-tissue defects, poor-quality soft tissue at the area of implantation (eg, a lack of keratinized gingiva), a history of implant failures, overloading of the implant, faults in materials and techniques (including cementitis), poor bone quality at the implant area, systemic diseases, drug therapies, and improper maintenance (including a lack of compliance and oral hygiene).6-16
A Shift in Focus
In the last decade, there has been a shift in focus from the surgical phase of implant placement to the maintenance phase.7,17-19 With the increasing number of patients receiving implant therapy, it has become critical for the restorative dentist to concentrate on and emphasize the maintenance of complex implant restorations.18,19 Both the restorative dental professional (and his team) and the patients play an important role in the maintenance and long-term success of implants and implant restorations.19 The dental practitioner and his team are responsible for performing regular professional prophylaxis procedures, monitoring the patient, preventing recurrence in previously treated peri-implantitis patients, and locating and treating peri-implant inflammation in a timely manner.19,20 The patient, on the other hand, is delegated the task of daily effective home care.19 The patient should be compliant and motivated, as he or she is vital in the maintenance therapy.19,21
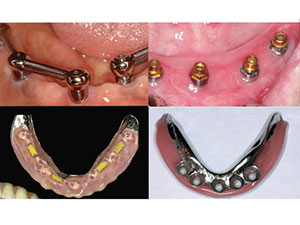 |
| Figure 1. Prostheses and their intraoral counterparts should be self-cleansable or easy to clean. |
Factors Affecting Oral Hygiene Maintenance
The factors that affect oral hygiene maintenance by a patient restored with implant assisted prostheses include the design of the prostheses, the patient’s desire and commitment, patient education, and the instruments and materials made available for cleaning access-challenged areas.22,23 The prostheses should be self-cleansable (Figure 1), they should also have optimal emergence profiles and hygienic contours and be designed according to standard prosthodontic guidelines.22,23 There are several types and designs of implant prostheses, and patients should be educated on how to clean their specific prostheses and oral tissues.23 Patients who are not committed and/or motivated to maintain proper oral hygiene should be educated, and their treatment should be suspended until an improvement in behavior and attitude is noticed (Figure 2).23 The entire dental team, including the dental hygienist, dental assistant, and the restorative dentist, should participate in educating the patient on the oral hygiene regimen.
 |
 |
 |
| Figure 2. (a) Treatment suspended in a patient displaying poor oral hygiene and subsequent poor health of tissues. (b) Improvement in oral hygiene due to patient re-education and suspension of treatment. (c) Improvement in tissue health with proper oral hygiene. |
Choosing Devices and Clinical Care Guidelines to Optimize Oral Hygiene
It is critical to incorporate the most effective oral hygiene devices into each patient’s oral hygiene regimen to optimize oral hygiene maintenance and prevent peri-implantitis.23 Manual and electric toothbrushes (brushing at least twice daily), interproximal brushes, flosses, antimicrobial rinses and gels, and subgingival irrigation systems should be recommended to patients as per their individual needs (Figure 3).24-34 Providing patients with cleaning aids once they accept treatment is particularly advantageous because it saves the patient time and effort, eliminates the possibility of getting a wrong product, and also makes the cleaning aids immediately accessible to the patient. The patient can start using the cleaning aids early in the treatment process, which ensures proficiency by the time the prosthesis is delivered. The entire dental team should ensure that their patients can perform the required skills.22 At each visit, the importance of proper home care practices and a long-term professional recall regimen must be stressed.23
 |
| Figure 3. Various oral hygiene devices are incorporated into a patient’s oral hygiene regimen to optimize oral hygiene maintenance. |
Clinical care guidelines recommend the use of electric toothbrushes for implant-supported removable and fixed restorations.35 Electric toothbrushes with a wide variety of brush attachments may be advantageous for maintaining the oral hygiene of implant-supported prostheses and preserving the health of the peri-implant-supporting tissues.23 Electric toothbrushes are recommended because of their unique mechanical interaction with contaminated tooth surfaces.36,37 Patients are more compliant and motivated to use electric toothbrushes due to the psychological “high-tech” effect and also because they are often recommended by their dental practitioners.23,38 Electric toothbrushes are easy and convenient to use because the user just needs to appropriately position the bristles on the various tooth surfaces for an adequate amount of time and not worry about performing brushing motions.23 Hence, they are especially indicated for the elderly and young children because of their limited motor skills and dexterity.29,39 Systematic reviews and many studies comparing manual toothbrushes with powered (electric) toothbrushes conclude that there is an improvement in oral health with powered toothbrushes compared to manual toothbrushes.40-45
 |
 |
| Figure 4. Oral-B electric toothbrush (Oral-B Genius 8000 [Procter & Gamble]). | Figure 5. The FlossAction (interproximal) brush head. |
 |
 |
| Figure 6. (a) The CrossAction toothbrush head. (b) The CrossAction toothbrush head was used in cleaning the locator abutment. |
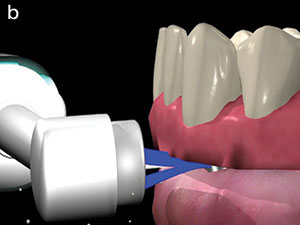
The Oral-B electric toothbrush (Oral-B Genius 8000 [Procter & Gamble]) (Figure 4) is the first to have been accepted by the ADA.46 Its 3-D Cleaning Action technology safely and effectively removes plaque and helps prevent plaque-related oral diseases. It is a smart toothbrush.47 By connecting a smartphone and the Oral-B app, it uses facial recognition technology to guide user brushing, zone to zone.47 It has pressure sensors: It visually alerts the user when brushing is too hard.47 The rounded brush head surrounds each tooth for a more thorough clean. The built-in timer alerts the user when they have brushed for the right amount of time. Several types of attachments (brush heads) are available to be used with it, as per the user needs, including Pro Gumcare, CrossAction, Precision Clean, Sensitive Clean, Deep Sweep, FlossAction, Ortho Care, 3D White, and Dual Clean (Oral-B). The FlossAction and CrossAction toothbrush heads are best indicated for implant prostheses. The FlossAction has micro pulse bristles and a cone-shaped brush head 6 mm in diameter at the base of the brush and tapering to approximately 4 mm at the apex, providing superior interdental cleaning (Figure 5). The CrossAction is an oval, multi-tufted toothbrush head approximately 15 mm × 13 mm in diameter (Figure 6).47 Its CrissCross bristles are set at a 16° angle to effectively clean along the gingival margin and interdental areas. Indicator bristles fade as a sign to replace the toothbrush head for a better clean. Both brush-head attachments can be used interchangeably to access most surfaces of hygienically designed implant-supported prostheses (Figure 7).47
 |
 |
 |
 |
| Figure 7. Both brush-head attachments are used interchangeably for cleaning implant-supported prostheses. |
CLOSING COMMENTS
Both professional maintenance and optimal personal oral hygiene are essential for the long-term success and the proper and comfortable function of dental restorations involving dental implants.22 Patients invest a lot of money and time in rehabilitations with implant-assisted prostheses; hence, most patients are motivated to maintain oral hygiene when educated regarding the same. It is the responsibility of the entire dental team to educate the patients and make available hygiene devices that can be easily used by patients and can thoroughly clean all the surfaces of dental implant restorations.
References
- Bryant SR, MacDonald-Jankowski D, Kim K. Does the type of implant prosthesis affect outcomes for the completely edentulous arch? Int J Oral Maxillofac Implants. 2007;22(suppl):117-139.
- Sadowsky SJ. Treatment considerations for maxillary implant overdentures: a systematic review. J Prosthet Dent. 2007;97:340-348.
- Kate MA, Palaskar S, Kapoor P. Implant failure: a dentist’s nightmare. Journal of Dental Implants. 2016;6:51-56.
- Zitzmann NU, Berglundh T. Definition and prevalence of peri-implant diseases. J Clin Periodontol. 2008;35(suppl 8):286-291.
- Roos-Jansåker AM, Renvert H, Lindahl C, et al. Surgical treatment of peri-implantitis using a bone substitute with or without a resorbable membrane: a prospective cohort study. J Clin Periodontol. 2007;34:625-632.
- Smeets R, Henningsen A, Jung O, et al. Definition, etiology, prevention and treatment of peri-implantitis—a review. Head Face Med. 2014;10:34.
- Atieh MA, Alsabeeha NHM, Faggion CM Jr, et al. The frequency of peri-implant diseases: a systematic review and meta-analysis. J Periodontol. 2013;84:1586-1598.
- Charyeva O, Altynbekov K, Zhartybaev R, et al. Long-term dental implant success and survival—a clinical study after an observation period up to 6 years. Swed Dent J. 2012;36:1-6.
- Heitz-Mayfield LJ. Peri-implant diseases: diagnosis and risk indicators. J Clin Periodontol. 2008;35(suppl 8):292-304.
- Gruica B, Wang HY, Lang NP, et al. Impact of IL-1 genotype and smoking status on the prognosis of osseointegrated implants. Clin Oral Implants Res. 2004;15:393-400.
- Huynh-Ba G, Lang NP, Tonetti MS, et al. Association of the composite IL-1 genotype with peri-implantitis: a systematic review. Clin Oral Implants Res. 2008;19:1154-1162.
- Lagervall M, Jansson LE. Treatment outcome in patients with peri-implantitis in a periodontal clinic: a retrospective study. J Periodontol. 2012;84:1365-1373.
- Linkevicius T, Puisys A, Vindasiute E, et al. Does residual cement around implant-supported restorations cause peri-implant disease? A retrospective case analysis. Clin Oral Implants Res. 2013;24:1179-1184.
- Vervaeke S, Collaert B, Cosyn J, et al. A multifactorial analysis to identify predictors of implant failure and peri-implant bone loss. Clin Implant Dent Relat Res. 2015;17(suppl 1):e298-e307.
- Renvert S, Aghazadeh A, Hallström H, et al. Factors related to peri-implantitis—a retrospective study. Clin Oral Implants Res. 2014;25:522-529.
- Ferreira SD, Silva GL, Cortelli JR, et al. Prevalence and risk variables for peri-implant disease in Brazilian subjects. J Clin Periodontol. 2006;33:929-935.
- Silverstein LH, Kurtzman GM. Oral hygiene and maintenance of dental implants. Dent Today. 2006;25:70-75.
- Kanathila H, Pangi A, Benakatti V, et al. Maintenance of dental implants: A way to long term success: A review. Int J of Appl Dent Sci 2018; 4(2): 104-107.
- Gulati M, Govila V, Anand V, et al. Implant maintenance: a clinical update. Int Sch Res Notices. 2014;2014:908534.
- Cohen RE; Research, Science and Therapy Committee, American Academy of Periodontology. Position paper: periodontal maintenance. J Periodontol. 2003;74:1395-1401.
- Garg AK, Duarte F, Funari K. Hygienic maintenance of dental implants: the key to long-term success. J Practical Hygiene. 1997;6:13-20.
- Piermatti J, Barndt P, Thalji G. American College of Prosthodontists position statement. Maintenance of full-arch implant restorations. October 2016. https://www.prosthodontics.org/assets/1/7/Maintenance_of_Full-Arch_Implant_Restorations.pdf. Accessed August 19, 2019.
- Cagna DR, Massad JJ, Daher T. Use of a powered toothbrush for hygiene of edentulous implant-supported prostheses. Compend Contin Educ Dent. 2011;32:84-88.
- de Araújo Nobre M, Cintra N, Maló P. Peri-implant maintenance of immediate function implants: a pilot study comparing hyaluronic acid and chlorhexidine. Int J Dent Hyg. 2007;5:87-94.
- Humphrey S. Implant maintenance. Dent Clin North Am. 2006;50:463-478, viii.
- Renvert S, Lessem J, Dahlén G, et al. Topical minocycline microspheres versus topical chlorhexidine gel as an adjunct to mechanical debridement of incipient peri-implant infections: a randomized clinical trial. J Clin Periodontol. 2006;33:362-369.
- Horwitz J, Machtei EE, Zuabi O, et al. Amine fluoride/stannous fluoride and chlorhexidine mouthwashes as adjuncts to single-stage dental implants: a comparative study. J Periodontol. 2005;76:334-340.
- Sarment DP, Peshman B. Manual of Dental Implants: A Reference Guide for Diagnosis & Treatment. Hudson, OH: Lexi-Comp; 2004:70-73.
- Tawse-Smith A, Duncan WJ, Payne AG, et al. Relative effectiveness of powered and manual toothbrushes in elderly patients with implant-supported mandibular overdentures. J Clin Periodontol. 2002;29:275-280.
- Truhlar RS, Morris HF, Ochi S. The efficacy of a counter-rotational powered toothbrush in the maintenance of endosseous dental implants. J Am Dent Assoc. 2000;131:101-107.
- Vandekerckhove B, Quirynen M, Warren PR, et al. The safety and efficacy of a powered toothbrush in patients with implant-supported fixed prostheses. Clin Oral Investig. 2004;8:206-210.
- Wolff L, Kim A, Nunn M, et al. Effectiveness of a sonic toothbrush in maintenance of dental implants. A prospective study. J Clin Periodontol. 1998;25:821-828.
- Felo A, Shibly O, Ciancio SG, et al. Effects of subgingival chlorhexidine irrigation on peri-implant maintenance. Am J Dent. 1997;10:107-110.
- Ciancio SG, Lauciello F, Shibly O, et al. The effect of an antiseptic mouthrinse on implant maintenance: plaque and peri-implant gingival tissues. J Periodontol. 1995;66:962-965.
- Bidra AS, Daubert DM, Garcia LT, et al. Clinical practice guidelines for recall and maintenance of patients with tooth-borne and implant-borne dental restorations. J Prosthodont. 2016;25(suppl 1):S32-S40.
- Robinson PG, Deacon SA, Deery C, et al. Manual versus powered toothbrushing for oral health. Cochrane Database Syst Rev. 2005;(2):CD002281.
- Lea SC, Khan A, Patanwala HS, et al. The effects of load and toothpaste on powered toothbrush vibrations. J Dent. 2007;35:350-354.
- Hellstadius K, Asman B, Gustafsson A. Improved maintenance of plaque control by electrical toothbrushing in periodontitis patients with low compliance. J Clin Periodontol. 1993;20:235-237.
- Davidovich E, Ccahuana-Vasquez RA, Timm H, et al. Randomised clinical study of plaque removal efficacy of a power toothbrush in a paediatric population. Int J Paediatr Dent. 2017;27:558-567.
- Yaacob M, Worthington HV, Deacon SA, et al. Powered versus manual toothbrushing for oral health. Cochrane Database Syst Rev. 2014;(6):CD002281.
- Rosema NA, Timmerman MF, Versteeg PA, et al. Comparison of the use of different modes of mechanical oral hygiene in prevention of plaque and gingivitis. J Periodontol. 2008;79:1386-1394.
- Kurtz B, Reise M, Klukowska M, et al. A randomized clinical trial comparing plaque removal efficacy of an oscillating-rotating power toothbrush to a manual toothbrush by multiple examiners. Int J Dent Hyg. 2016;14:278-283.
- Kulkarni P, Singh DK, Jalaluddin M. Comparison of efficacy of manual and powered toothbrushes in plaque control and gingival inflammation: a clinical study among the population of East Indian region. J Int Soc Prev Community Dent. 2017;7:168-174.
- Jain Y. A comparison of the efficacy of powered and manual toothbrushes in controlling plaque and gingivitis: a clinical study. Clin Cosmet Investig Dent. 2013;5:3-9.
- Allocca G, Pudylyk D, Signorino F, et al. Effectiveness and compliance of an oscillating-rotating toothbrush in patients with dental implants: a randomized clinical trial. Int J Implant Dent. 2018;4:38.
- American Dental Association. Oral-B power toothbrushes to receive ADA Seal of Acceptance [press release]. September 18, 2017. https://www.ada.org/en/press-room/news-releases/2017-archives/september/oral-b-power-toothbrushes-to-receive-ada-seal-of-acceptance. Accessed August 19, 2019.
- Oral-B. Oral-B Genius. https://oralb.com/en-us/products/compare/genius. Accessed August 19, 2019.
Dr. Massad is an associate professor in the department of graduate prosthodontics at the University of Tennessee Health Science Center (UTHSC) College of Dentistry in Memphis; an associate faculty at the Tufts University School of Dental Medicine in Boston; an adjunct associate faculty of the department of comprehensive dentistry at the University of Texas Health Science Center at San Antonio (UT Health San Antonio) School of Dentistry; and an adjunct professor in the department of restorative dentistry at Loma Linda University in Loma Linda, Calif. He has a private practice in Tulsa. He can be reached at joe@joemassad.com.
Disclosure: Dr. Massad is a consultant for Proctor & Gamble. He did not receive compensation for this article.
Dr. Verma is the vice chancellor of Guru Gobind Singh Indraprastha University, Delhi and former director-principal, Maulana Azad Institute of Dental Sciences, New Delhi, India. He is a past president of the Indian Dental Association, the Indian Prosthodontics Society, and the International College of Dentists and Member, Service Committee FDI. He is a recipient of the Padma Shri, the fourth highest civilian award in India. He holds many fellowships viz FDSRCS (England), FDSRCS (Edinburgh), FDSRCPS (Glasgow), FACD, Associate Fellow of AAID and numerous other awards and positions. He can be reached at dpmaids@gmail.com.
Disclosure: Dr. Verma reports no disclosures.
Dr. Ahuja graduated with a BDS from Nair Hospital Dental College in 2002 and an MDS and certificate in prosthodontics from UTHSC in 2009. She was as an assistant professor in the department of prosthodontics at UTHSC, where she worked for 3 and a half years, teaching and treating complex restorative cases. Currently, she is a consultant for several private dental clinics in Mumbai, India, and also for NYU Langone in New York. She has lectured nationally and internationally on various prosthodontic topics. She has been published in multiple peer-reviewed national and International journals and is the co-author of the textbook, Applications of the Neutral Zone in Prosthodontics. She can be reached at swatiahuja@gmail.com.
Disclosure: Dr. Ahuja reports no disclosures.
Related Articles
Treating a Patient With Inadequate Restorative Space
Cameograms: A New Technique for Prosthodontic Applications











