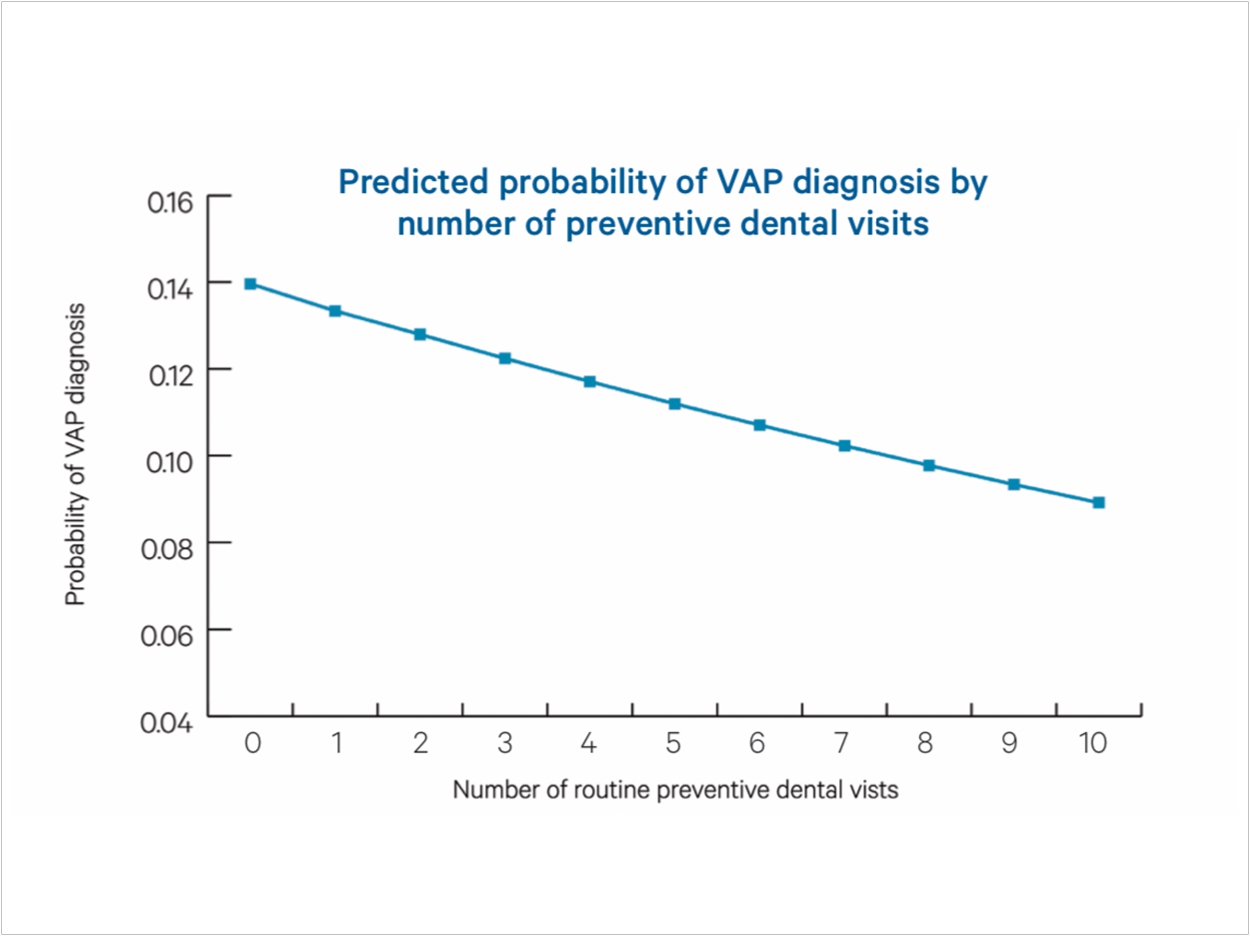
Good oral health reduces the chances of acquiring ventilator-associated pneumonia (VAP), according to DentaQuest.
The company examined administrative claims data in the IBM Watson MarketScan Medicaid Database for 9,279 patients admitted to an intensive care unit in 2016 and 2018 who received invasive mechanical ventilation for 48 hours or more. It also analyzed dental claims data and Current Dental Terminology codes to identify patients who had received a dental examination, prophylaxis, or preventive visits within three years prior to hospitalization.
Approximately 14% of Medicaid patients on mechanical ventilation had a VAP diagnosis. However, preventive dental visits decreased the likelihood of acquiring VAP, and at least one visit within three years reduced the likelihood of a VAP diagnosis by 22%. Each additional routine dental visit during the three years prior to being put on a ventilator decreased the probability of a VAP diagnosis by 5%.
VAP is the second most common hospital-acquired infection (HAI) and the leading cause of HAI deaths among critically ill patients, DentaQuest said. VAP commonly occurs when patients are connected to mechanical ventilation and bacteria travel from the oral cavity or breathing equipment and into the lungs. The airway tube disrupts the natural defenses that maintain a healthy oral microbiome.
In fact, DentaQuest said, VAP is likely to occur in 10% to 20% of patients who are mechanically ventilated for 48 hours or more. And with the pandemic producing record numbers of patients requiring mechanical ventilation to survive, DentaQuest said, more people are at risk of acquiring VAP and facing adverse outcomes including death than ever before.
However, risks vary among different populations. For example, Black patients on mechanical ventilators for 48 hours or longer were 39% more likely than White people to be diagnoses with VAP. Also, males were 20% more likely to be diagnosed than females. Patients with one comorbidity were 73% more likely to be diagnosed with VAP than those with none. And, patients with two or more comorbidities were 98% more likely than those with none.
These differences are particularly concerning, DentaQuest said, as COVID-19 disproportionately affects people of color and low-income communities, especially counties with higher proportions of Black people. These counties account for 52% of COVID-19 diagnoses and 58% of COVID-19 deaths in the United States.
Also, other DentaQuest data shows that Black adults are 22% less likely to have had a routine dental visit in the past year and 68% more likely to have unmet dental needs that White adults, making them not only more likely to acquire the coronavirus but also VAP from poor oral health and mechanical ventilation.
VAP adds approximately $40,000 and seven days to a single hospital stay, DentaQuest said, so improved oral health could have a significant impact in reducing its burden on the healthcare system while ensuring resources are available for other critically ill patients. The company also said that its findings emphasize the need to mitigate the inequalities now afflicting oral healthcare to reduce the risks of illness and death from COVID-19 and VAP.
DentaQuest recommends a three-step strategy for preventing VAP. First, effective oral healthcare and behaviors should be promoted in the community. Second, the healthcare system should be attuned to historic disparities to improve effective oral healthcare for patients in anticipation of VAP. Finally, DentaQuest recommends fully implementing oral care management protocols for all ventilated patients.
Related Articles
Oral Healthcare Program Reduces Pneumonia Rates in Nursing Homes
Poor Oral Health Linked to Death by Pneumonia in the Elderly
Dental Visits Can Prevent Pneumonia


