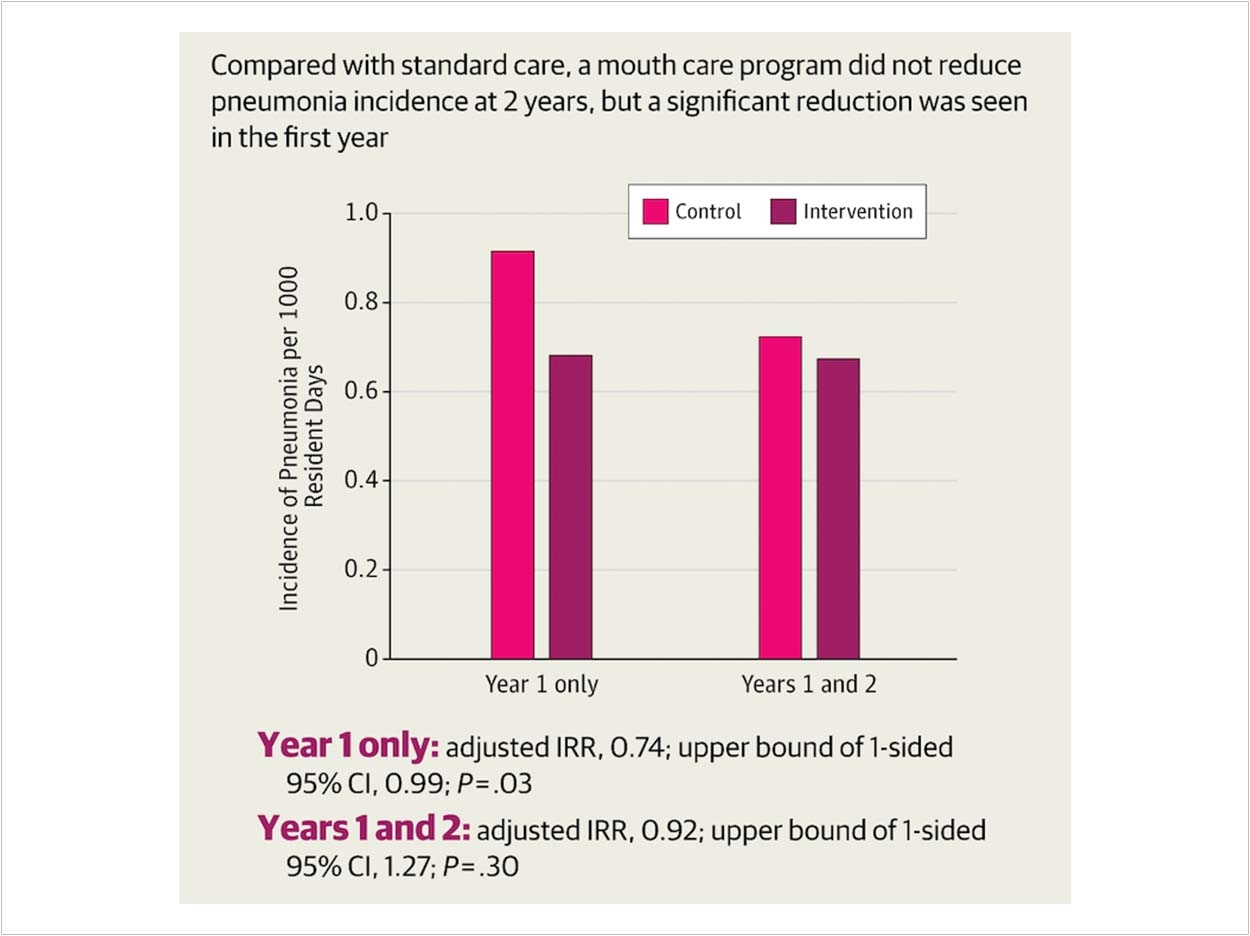
Nursing homes that implemented an oral healthcare program for their residents saw a statistically significant 31% reduction in pneumonia cases compared to facilities that did not use the program, according to the Cecil G. Sheps Center for Health Services Research at the University of North Carolina at Chapel Hill.
While numerous previous studies have demonstrated an association between oral healthcare and pneumonia, the researchers said, the latest work is the first to examine whether a pragmatic program of brushing, flossing, and gum care provided by nursing home staff such as their Mouth Care Without a Battle approach reduces pneumonia.
“We’re building a compelling case to show that mouth care is healthcare, that poor oral hygiene can lead to more serious health concerns, and that nursing home staff can play a key role to interrupt that cycle,” said Sheryl Zimmerman, PhD, Sheps Center program codirector and distinguished professor of social work and public health.
“By implementing an evidence-based, compassionate approach like Mouth Care Without a Battle, nursing homes can take a meaningful step to evolve care practices. This program has incredible potential to help individuals in a variety of supportive care settings, including those living at home or in assisted living communities,” said Zimmerman.
Nearly two-thirds of nursing home residents have Alzheimer’s disease or a related dementia, the researchers said. When these residents resist care, their caregivers often lack the knowledge or skills to properly clean their teeth, the researchers added. As a result, 84% of dependent long-term care residents don’t receive oral care.
Building on its growing body of evidence-based training, including the nationally adopted Bathing Without a Battle program, the Sheps Center Program on Aging, Disability and Long-Term Care designed Mouth Care Without a Battle to remove common barriers to oral care. In addition to learning about new products and techniques, staff learn individualized care practices that improve their confidence and the care they provide.
“Many nursing home communities may not connect the dots between mouth care and pneumonia, but the results from the program speak for themselves,” said Michelle Strickland, licensed nursing home administrator at Brian Health & Rehabilitation in Wilson, North Carolina.
“We saw a noticeable reduction of residents being hospitalized with pneumonia, and the program continues to empower our staff and residents,” said Strickland.
A lack of significant results in the second year of the study, however, raises questions about the sustainability of interventions in long-term care.
“It’s one thing to train your staff on a new procedure, and another to establish a new best practice in the long term,” said Philip Sloane, MD, MPH, Sheps Center program codirector and distinguished professor of family medicine. “We recommend putting safeguards in place, such as hiring an oral care aide, to help sustain a high level of oral healthcare.”
“This study is an exciting step forward in translating evidence into daily care practice,” said Robyn Stone, PhD, senior vice president of research at LeadingAge. “While most frontline caregivers intuitively know that oral health is important, these findings bring the issue into focus in a way that’s practical, actionable, and patient-centric.”
The study, “Effectiveness of a Mouth Care Program Provided by Nursing Home Staff Vs. Standard Care on Reducing Pneumonia Incidence,” was published by The JAMA Network Open.
Related Articles
Poor Oral Health Linked to Death by Pneumonia in the Elderly
Seniors Need Effective Dental Care Too
Chronic Health Conditions Associated With Greater Risk of Tooth Loss


