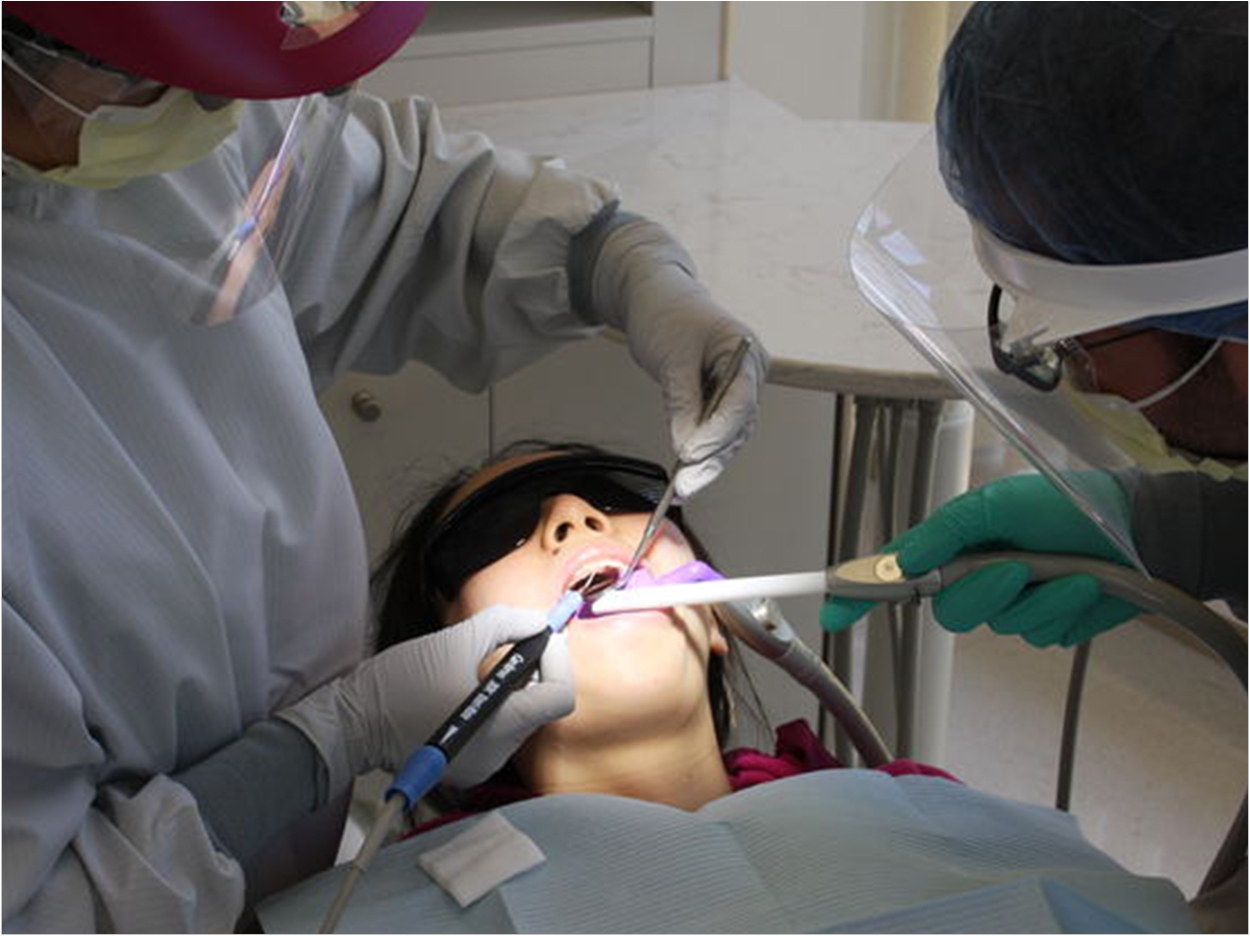
The combined use of a high-volume evacuator (HVE) with an intraoral suction device significantly reduces the amount of microbial aerosols generated during dental cleanings, according to the Loma Linda University (LLU) School of Dentistry, improving safety for patients and dental professionals alike.
Researchers at the school found a threefold reduction in microbial aerosols with the simultaneous use of an HVE plus an additional suction device placed in a patient’s mouth compared to using an HVE only.
The spread of COVID-19 and expanding understanding about its routes of transmission, including airborne respiratory droplets, sparked the researchers’ determination to investigate aerosol dispersion during dental procedures, said Montry S. Suprono, DDS, MSD, director of the LLU Center for Dental Research and the study’s principal investigator.
“Once organizations like the WHO and CDC released reports describing the virus’s modes of transmission, we quickly understood how dentistry would be affected because a number of dental procedures generate aerosols,” said Suprono. “So, we wanted to figure out ways to minimize the risks by decreasing the amount of aerosols that are generated during dental procedures.”
The clinical trial involved more than 90 dental student participants who served as operators and patients at the LLU dental clinic. The researchers collected aerosol samples by placing blood agar plates, which are dishes intended to collect the aerosols, in various zones throughout the clinic such as shelves and patients’ chests for intervals of time before, during, and after dental cleanings.
The procedures were conducted using a split-mouth design. Operators used both the HVE and intraoral suction device on one side of the patient’s mouth during one round of the cleaning and then only the HVE on the other side of the patient’s mouth for the other round. After collecting the aerosols in the various agar plates, samples were incubated for two days, and microbial levels of each sample were measured.
The highest microbial counts came from the plates positioned on patients in the operating zone compared to plates placed on mobile trays and shelves farther away. Also, microbial levels during procedures were highest compared to pre-treatment and post-treatment levels. And compared to using the HVE alone, the combination of the HVE and an intraoral suction device significantly reduced the amount of microbial aerosols generated.
Furthermore, microbial levels before procedures were similar to microbial levels after procedures, meaning that a 30-minute time interval for air change and for the aerosols to settle down on surfaces post-procedure appears to be adequate, the researchers said.
“We now know dental professionals should allow for aerosols to settle for some time before sanitizing the treatment area and that the risk between patients is minimal if time is allowed,” Suprono said.
Suprono hopes the research will inform and guide best clinical practices to enhance safety and hygiene during dental cleanings. There also remains ample opportunity to consider other types of dental procedures or equipment in evaluating aerosol generating, he said. Understanding aerosol dynamics through computerized simulations and modeling constitutes another rapidly developing area of research as well, he added.
The researchers will continue studying personal protective equipment, aerosols, and air quality as it pertains to dental practice, Suprono said.
“These kinds of inquiries and research are critical to evaluate how dentistry currently works now and how it could evolve in the future with the goal of improving the safety for our patients and dental professionals,” said Suprono.’
The study, “A Clinical Investigation of Dental Evacuation Systems in Reducing Aerosols,” was published by the Journal of the American Dental Association.
Related Articles
What in the World Do We Do Now About Masks?
Many AGPs Appear Unlikely to Generate Infectious Aerosol
Suction Significantly Reduces Aerosol Risks in Open Clinic Settings












