|
||||||||||||||||||||||||||||||||
|
INTRODUCTION
The aesthetic restoration process often requires a multidisciplinary approach. Successful rehabilitation requires methodical integration among dental professionals to achieve an aesthetic, functional, and healthy restorative and periodontal interface. This meticulous process requires clearly defined objectives and many levels of professional collaboration.1-4
Periodontal disease prevalence has been estimated to affect up to 85% of the US adult population.5 General dentists and periodontists are both engaged in diagnosing, treating, and maintaining a healthy restorative and periodontal interface. Achieving good oral health may or may not require a multidisciplinary approach. However, many complex treatment plans often require comanagement and intercommunication between a general dentist and specialist to achieve optimal oral health, function, and aesthetics. Once periodontal health has been established, a restorative clinician and periodontist may successfully begin the restorative phases of treatment.
Periodontal treatment modalities often include establishing a healthy periodontium. Today, however, more periodontal plastic surgical procedures are being employed to facilitate an increasing demand for aesthetic restorative treatment. These may include subepithelial connective grafts, gingival recontouring, and, more frequently, aesthetic clinical crown lengthening, or a “smile lift surgery.”
Frequently, a patient’s chief complaint will be “I have short teeth” or “I have a gummy smile.” A diagnosis of altered passive eruption (APE) is a common etiology that is often underdiagnosed and treated by prosthodontic means.6,7 Short crowns usually fall in one of 2 categories: coronal destruction resulting from traumatic injury, incisal attrition, abrasion, or corrosion; and a coronally situated gingival complex resulting from tissue hypertrophy or APE.
APE can also be confused with other conditions; eg, vertical maxillary excess, vertical maxillary rotation, and hyperactive lip translation when smiling8—all should be considered as part of the differential diagnoses. If APE is found or the diagnosis needs to be confirmed, conferring with a specialist or periodontist to join the team is a prudent decision for patient and clinician success.
Despite the progression of periodontal disease or the complexity of prescribed treatment, following the fundamentals of collaborative patient care typically ensures better patient outcomes and mutual success for the referring general practitioner and periodontist. Ongoing communication between both the general dentist and periodontal specialist are paramount to success, and the lines of communication need to be defined and remain open throughout treatment. In order for the general practitioner and periodontist to function as a cohesive team, both professionals need to have a thorough understanding of the treatment modalities, processes, and desired treatment outcomes. Equally important to the collaborative relationship is a sharing of treatment philosophies.
Establishing an Interdisciplinary Team
A multidisciplinary approach will mean establishing a relationship with a specialist. Avenues to pursue a specialist or periodontist may be through the obvious channels, ie, phone calls, letters, Internet searches, and geographic location. However, education and sharing practice philosophies are tried and tested methods in forming and maintaining successful professional relationships.
Although education may seem like the obvious answer to many, the best clinicians admit that this will provide a more stable fundamental structure for a team approach and patient care. Specialists should also be proactive in educating other clinicians in their area through local study clubs and pursuing higher levels of continuing education (CE) seminars. This provides an opportunity to share your unique talents or special interests within your dental community and scope of practice.
If you are experienced and proficient at placing implants or are adept at periodontal plastic procedures, let that be known through these avenues. Opening your practice with a specific vision and goals will provide any clinician with better focus for professional accomplishments, patient care, and a rewarding career.
“As a general practitioner, when I’m establishing a referral relationship, I look for a periodontist that has a vision for seeing things from a restorative and aesthetic standpoint as well,” states Dr. Green. “Likewise, I believe it is beneficial for periodontists to find dentists who have a strong focus on establishing periodontal health at a truly optimal level before moving into the restorative phase of treatment.”
Learning is Lifelong
“Consistent and focused CE is imperative to optimal treatment outcomes for patients. Learning is truly life-long. The more knowledge people have and the more they know and accept their limits in terms of what they can and can’t do, the more they will know when to refer. Ultimately, the goal is to ensure the patient receives excellent treatment and results,” says Dr. Green.
Congruent Patient Care
A collaborative treatment concept begins the moment the general practitioner consults with a periodontist. This communication must remain open from the initial patient presentation, diagnostic, and treatment and maintenance phases of therapy. “If there is a patient I’m referring to Dr. Pulliam who has restorative needs as well as periodontal needs, I will e-mail photos, a full set of radiographs, and study models if the complexity of the case warrants it. We meet to discuss the patient’s case in person (or over the phone), once he has all the necessary patient information in hand,” continues Dr. Green.
“Dr. Pulliam’s restorative perspective, the diagnostic information, and our discussion will help to focus periodontal treatment planning; therefore, it is imperative that diagnostic information be shared through interoffice communiqué (Table 1). This process must include staff education and proficiency in transferring data and patient records. This may include electronic and traditional methods. Patients will perceive this and have a greater appreciation when clinicians discuss treatment options and before scheduled examinations (Table 2).”
Diagnostic Phase: New Patient
“When patients present at my office, the first thing I do is conduct a new patient interview with them. If the patient is a minor, I will have the parent or guardian also present for the interview,” states Dr. Green. “Before I do a clinical examination, we need to know patients’ goals and desires pertaining to their overall oral health and aesthetics. This entails asking them where they have been, from a dental standpoint, and where they see themselves in 5 or 10 years. This information helps to define and establish expectations at the very beginning.”
Depending on the complexity of the treatment plan, a joint meeting between the patient and both doctors may be necessary. In this way, both doctors can review their roles and responsibilities in treating the patient at the same time. Sending the patient back and forth between both offices is not only an inconvenience for the patient, but can lead to confusion. The fewer meetings the patient has to attend not only promotes more efficiency, but also engages the patient in the treatment planning process. Additionally, we have found there is a direct correlation in the levels of patient communication, education, understanding, and motivation, to that of treatment acceptance (Figure 1).
CASE REPORT
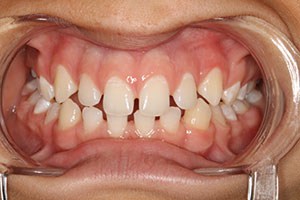
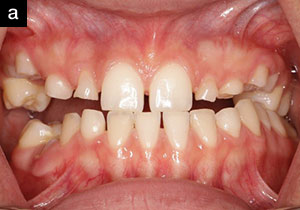
In December of 2009, a 17-year-old male presented to Dr. Green’s office with a chief complaint of: “I have a gummy smile and wide spaces between my upper and lower teeth” (Figures 2a and 2b). During the initial examination, which included his parents, it was noted that prior orthodontic treatment had been completed approximately 2 years ago with an overall improvement, but without full resolution of interdental spacing due to tooth size and contour discrepancies. This was confirmed with a set of pre- and postorthodontic panoramic radiographs sent to Dr. Green by the treating orthodontist (Dr. Arthur Anderson, Nashville, Tenn). A comprehensive examination was conducted at this time, including intraoral and extraoral photos, alginate impressions for study models, and face-bow transfer (Artex [Jensen Dental]).
 |
 |
| Figure 1. Aesthetic outcomes have direct correlation to doctor collaboration and patient education. | Figure 2a. Initial patient presentation. |
 |
 |
| Figure 2b. Preoperative smile. | Figure 3. Photoshop modification to approximate potential treatment outcome. |
 |
 |
| Figure 4. Free-hand composite buildup as a diagnostic aid and patient preview. | Figure 5a. Surgical flap reflected shows bone at the cementoenamel junction (CEJ) and confirms diagnosis of altered passive eruption. Ostectomy is indicated. |
 |
 |
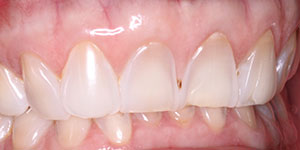
| Figure 5b. Ostectomy and osteoplasty establish proper osseous contour to CEJ relationship (~1.5 to 2 mm). Clinical crown length is 10.5 mm, which maintains gingival position and crown length (prevents gingival rebound posthealing). | Figure 6a. Final restorations and resulting smile; 8 all-ceramic veneers on teeth Nos. 5 to 12. |
 |
 |
| Figure 6b. Final smile: right profile. |
Figure 6c. Final smile: left profile. |
Patient Consultation
The patient and his mother returned to Dr. Green’s office a week later to review the findings and discuss the treatment options. The photographs and study models were reviewed, as well as the treatment challenges, which were both aesthetic- and occlusion-related.
Dental imaging software or Photoshop are valuable tools for patient education, and also provide a blueprint to determine the next restorative or periodontal treatment step. “Photoshop is a useful imaging tool for patient education and treatment planning,” notes Dr. Green (Figure 3). “This will often help the dentist and patient realize the aesthetic potential and limitations. Many times, the patient does not realize what a difference treatment will make without some form of dental imaging. Once the patient can visualize the end result—that’s the ‘A-ha!’ moment for him or her, and a pivotal moment in patient education.”
A composite mock-up was completed on teeth Nos. 5 through 12. A composite mock-up is another practical tool providing valuable insight for patient understanding and education, and often enhances case acceptance (Figure 4). Additional photographs were taken after the placement of the composite. After reviewing the Photoshop images and the composite mock-up, the patient was anxious to begin treatment, and was asked to return to the office in a week, at which time a comprehensive treatment plan and timeline would be discussed further.
Periodontal Exam and Consultation
Drs. Green and Pulliam reviewed the diagnostic radiographs, models, and photographs to make a tentative periodontal diagnosis and treatment plan. A periodontal examination would confirm good periodontal health and consider aesthetic periodontal plastic surgery options to enhance restorative and aesthetic outcomes.
Dr. Pulliam, Dr. Green, the patient, and his parents were present during the next treatment consultation. It is sometimes necessary to meet as a collective group to really ensure optimal communication. Oftentimes, a family member or doctor may not be present for the treatment discussion and will miss critical information needed for treatment success.
The periodontal exam revealed that gingival reshaping, or a “smile lift,” was indicated. A description of the procedure, how long it would take, and why it was necessary in order to achieve an optimal final result for the patient was provided. Both doctors explained each phase of treatment to the patient and his parents, beginning with the diagnostic phase, and continuing on through the restorative, temporization, and final restorative phases. By doing so, the patient and his family would have a complete understanding of the recommended treatments, along with a timeline for each milestone in the treatment plan. The periodontal and restorative treatment plan was accepted, and the patient was scheduled to return to Dr. Green’s office a week later to begin preliminary treatment.
Preliminary Restorative Phase
Composite resin (Renamel Microfill [Cosmedent]) was performed on teeth Nos. 22 to 27 to close diastemas and to open the vertical dimension of occlusion. In addition, composite resin (Venus [Heraeus Kulzer]) was bonded on the mandibular molars and premolars to provide a balanced occlusion. Two weeks later, new impressions were taken and poured in stone. Diagnostic wax-ups were done on the new models and these models were shared with Dr. Pulliam. “The wax-ups Dr. Green sent me were extremely important, because knowing the intended length and shape of the teeth to be restored helped me determine precisely how much gingival tissue to remove during gingivectomy aesthetic crown-lengthening surgery.”
Surgical Phase
The patient presented to Dr. Pulliam’s office for periodontal surgery (Figures 5a and 5b). Aesthetic crown lengthening was indicated to establish appropriate clinical crown length and gingival position. All diagnostic materials and data were available during surgery, including wax-ups provided by Dr. Green, pre-op photographs, radiographs, and Photoshop images. A stent was also fabricated to duplicate ideal wax-up, ensure proper crown length, and biologic width dimensions during surgery. This provided the blueprint necessary to establish proper dental, gingival, and osseous relationships.
Upon surgical exploration, a confirmation of short clinical crowns and APE was made. The primary goal for this procedure was to establish the correct osseous crest to cementoenamel junction (CEJ) relationship. Gingival recontouring for ideal position was completed. A full-thickness mucoperiosteal flap was reflected and the osseous crest was found adjacent to the CEJ, confirming a diagnosis of APE6—some references consider this altered active eruption9 (Figure 6a). Approximately 1.5 to 2 mm of ostectomy and/or osteoplasty was performed using rotary instruments and diamond burs (Henry Schein) to establish the desired osseous crest to CEJ relationship6 (Figure 6b). This will: ensure and maintain (1) proper osseous contours for a stable and healthy dentogingival complex; (2) provide an additional 1.5 to 2 mm of clinical tooth structure necessary for proper restorative space; (3) establish desired crown length of 10.5 mm;10 and (4) prevent gingival rebound and chronic gingival inflammation. A vertical mattress suturing technique (5-0 gut sutures [Henry Schein]) was used for proper flap adaptation. A surgical report and photographs were prepared by Dr. Pulliam and forwarded to Dr. Green to facilitate temporization.
Temporization Phase
The patient returned to Dr. Green’s office for immediate healing temporaries of teeth Nos. 5 to 12. Knowing that the final restorations would not be placed for another 14 to 16 weeks, the teeth were prepared as minimally as possible to receive the temporary veneers. This allowed sufficient time for the patient’s gingival structures to fully heal and mature to a point of stabilization, at which time final restorations could be accomplished with a successful treatment outcome. Provisionals were fabricated with a layering technique utilizing a bis-acryl material (Integrity [Dentsply Caulk]) and composite resin (Venus [Heraeus Kulzer]).
Final Restorative Phase
Preparation refinements were accomplished. Maxillary and mandibular vinyl polysiloxane impressions (Imprint 3 [3M ESPE]), centric relation bite registration (Blu-Mousse [Parkell]), face-bow transfer, and photographs of the preparations and provisionals were sent to the dental ceramist. Feldspathic porcelain veneers (Ceramco 3 [Vident]) were fabricated for teeth numbers 5 through 12. Three weeks later, and nearly 5 months since the initial patient consultation, the veneers arrived at Dr. Green’s office. At this time, the patient returned for try-in and final cementation (Figure 6c). The patient approved all aesthetic aspects of the veneers. The veneers were cleaned and silanated (Clearfil Ceramic Primer [Kuraray]). The veneers were bonded utilizing primers/adhesives, and resin cements (Choice 2 Veneer cement [BISCO Dental Products] was used for teeth Nos.7 to 10, and Panavia F Light [Kuraray] for teeth Nos. 5, 6, 11, and 12). Currently, the patient is in the planning stage of the second phase of his restorative plan, which entails the possibility of orthodontic treatment on the mandibular incisors to close remaining spaces before final restorative work is complete.
SUMMARY
Considering the ever increasing demand for youthful and attractive smiles, collaborative patient care among restorative clinicians and periodontists is paramount. Successful aesthetic rehabilitation often demands a multidisciplinary approach and requires more than a prescribed treatment plan.
“Beginning with the end in mind” not only helps the patient actualize treatment possibilities—thus making them a part of and engaged in their dental care from the start—but also provides clinicians with the appropriate data vital to accomplishing any required surgical and restorative procedure.
Conjoint treatment planning will help each clinician accomplish treatment objectives more effectively while achieving a functional and aesthetic outcome for optimal patient care. The lines of communication between clinicians must remain open and accessible at all times. As demonstrated, many practitioners involved with complex dental treatment will utilize many levels of education, communication, and treatment philosophies in achieving long-term success.
Acknowledgement
Dr. Green would like to acknowledge Mr. Alan Wollmam, Clearview Dental Arts, for his excellent ceramic work and collaboration on this case.
References
- Lee EA, Jun SK. Aesthetic design preservation in multidisciplinary therapy: philosophy and clinical execution. Pract Proced Aesthet Dent. 2002;14:561-570.
- Terry DA, McGuire M. The perio-aesthetic-restorative approach for anterior reconstruction—Part I: Evaluation and periodontal surgery. Pract Proced Aesthet Dent. 2002;14:283-292.
- Almog DM, Meitner SW, Even-Hen N, et al. Use of interdisciplinary team approach in establishing esthetic restorative dentistry. N Y State Dent J. 2005;71:44-47.
- Ohyama H, Nagai S, Tokutomi H, et al. Recreating an esthetic smile: a multidisciplinary approach. Int J Periodontics Restorative Dent. 2007;27:61-69.
- Brown LJ, Oliver RC, Löe H. Periodontal diseases in the U.S. in 1981: prevalence, severity, extent, and role in tooth mortality. J Periodontol. 1989;60:363-370.
- Dolt AH III, Robbins JW. Altered passive eruption: an etiology of short clinical crowns. Quintessence Int. 1997;28:363-372.
- Evian CI, Cutler SA, Rosenberg ES, et al. Altered passive eruption: the undiagnosed entity. J Am Dent Assoc. 1993;124:107-110.
- Ezquerra F, Berrazueta MJ, Ruiz-Capillas A, et al. New approach to the gummy smile. Plast Reconstr Surg. 1999;104:1143-1150.
- Chu SJ, Karabin S, Mistry S. Short tooth syndrome: diagnosis, etiology, and treatment management. J Calif Dent Assoc. 2004;32:143-152.
- Wheeler RC, Ash MM. Wheelers’s Dental Anatomy, Physiology, and Occlusion. 6th ed. Philadelphia, PA: Saunders; 1984:120.
Dr. Pulliam completed his undergraduate work at the University of Mississippi School of Pharmacy, and after completing 2 years as a clinical hospital pharmacist in Tuscaloosa Ala, he earned a DMD at the University of Alabama at Birmingham School of Dentistry. He later earned a certificate and MS in periodontics at The University of Texas Health Science Center San Antonio, Tex. He is a Diplomate of the American Board of Periodontology. He is an active member of ADA, American Academy of Pediatrics, Southern Academy of Periodontology, Texas Dental Association, and Nashville Dental Society. Dr. Pulliam maintains a private practice in Nashville, Tenn with an emphasis on aesthetic and implant dentistry. He has published articles and provides continuing education in periodontics and implant dentistry. He can be reached at (615) 297-8973.
Disclosure: Dr. Pulliam reports no disclosures.
Dr. Green maintains a private practice in Nashville, Tenn, with an emphasis on restorative and aesthetic care. Since graduating from The University of Louisville School of Dentistry in 1998, he has completed numerous continuing education courses, including The Louisiana State University Cosmetic Dentistry Continuum, Essential and Advanced Occlusion with Dr. Jimmy Eubank, restorative and aesthetic courses with William C. Strupp, and graduated from the Schuster Center for Professional Development. He can be reached at (615) 383-8213 or at green465@bellsouth.net.
Disclosure: Dr. Green reports no disclosures.