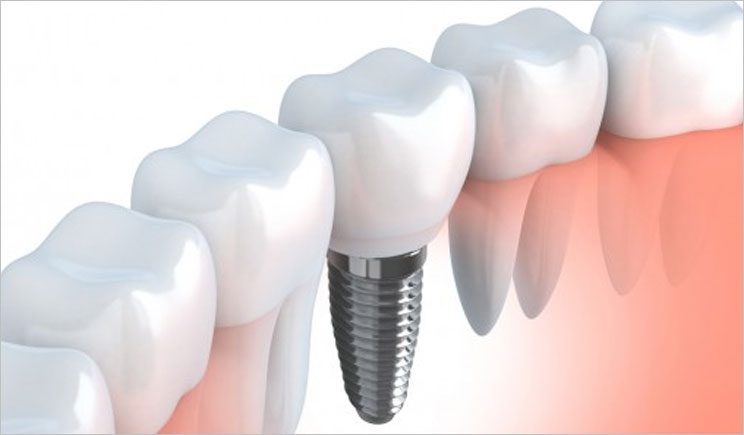
Tooth loss is a global problem that can severely affect overall health and quality of life. In the United States alone, more than 19% of Americans age 65 and older have already lost all their teeth. When it comes to replacing missing natural teeth, there is no option better than dental implants.
However, not all patients are eligible for oral surgery with dental implants, especially those who do not have sufficient volume or jawbone density to support an implant. Thanks to modern dentistry, though, dentists can now restore the jawbone’s optimal volume and strength with bone grafts and enable these patients to receive dental implants.
As the technology advances, newer and improved bone graft materials are being introduced for tooth replacement and for the management of maxillofacial bone defects. That’s why it’s important to determine which materials are most suitable for your patients’ dental needs.
What Is Bone Grafting?
During bone grafting, the dentist will use a section of natural bone from another area of the patient’s body, from another human being or animal, or from a specially prepared synthetic material to repair or replenish diseased or damaged jawbones. A bone graft may be needed to manage jawbone deficiency in cases involving:
- Developmental defects that cause incomplete or insufficient bone formation
- Bone loss due to chronic periodontal disease
- Injury to the face leading to bone damage
- Bone loss as a result of tooth removal or loss
Bone grafts can be broadly classified into two main types: natural and synthetic.
Natural Bone Grafts
Natural bone grafts are derived from natural sources.
Autologous or autogenous bone grafts take the graft from the same individual. Common sites used for obtaining bone grafts include the iliac crest, the mandibular symphysis, and the ramus. Since they originate from the same body, autologous grafts face minimal rejection chances, which is perhaps their most significant advantage. They also offer optimal primary implant stability and osseointegration. However, the process requires two surgical sites: the donor and the recipient site.
Allografts, on the other hand, are obtained from a human being other than the one receiving the graft. They are taken from cadavers who donate their bones, which are kept in a bone bank until a suitable recipient is found.
Since the allografts are also obtained from a human source, they have fewer rejections than synthetic materials. Allografts require sterilization and deactivation of body proteins, though, that may elicit an allergic reaction.
Xenografts are natural grafts are obtained from non-human bovine or porcine sources. Apart from the benefit of being readily available, they are not suitable bone grafting materials for everyone, as they may cause allergic reactions leading to graft rejection.
Synthetic Bone Grafts
Since every patient has unique requirements for bone grafting, synthetic materials that mimic bone tissue have been developed. The most common among them is based on hydroxyapatite, a mineral composed of calcium and phosphate that possesses a mineral-to-organic-component ratio similar to natural bone.
Artificial bone can be prepared from different materials like ceramics, calcium phosphate, bioglass, and calcium sulphate. Each material has its own properties and is selected based on individual patient needs, such as the site of grafting, the number of missing teeth, and the intended use. These materials are combined with bone proteins, growth factors, bone marrow, and ions such as strontium to enhance their biological activity.
The benefits of synthetic bone grafts include their ability to be moulded or modified according to need and elimination of the need for an additional surgical donor site. Synthetic bone graft materials include ceramic-based bone grafts, bioactive glass bone grafts, and polymer-based bone grafts.
Most bone grafts used these days are made from ceramics, owing to their excellent osteointegrative and osteoconductive potential and their safety for use in the oral cavity. But they are generally brittle in nature and are not suitable for grafting at sites where flexibility and resilience are required.
Bioactive glass bone grafts are composed of silicate-based glass such as Bio-Oss and OsteoGraft, which has bioactive properties. The advantages of bioglass include high elastic modulus and excellent biological activity, which promotes implant osseointegration. But, their brittleness precludes them from use in areas where the flexibility of the graft material is desired.
Polymer-based bone grafts with both natural and synthetic polymers are used in dentistry. Uniquely, the degradation rate of polymer-based bone grafts can be controlled. Hence, in cases where a graft is only temporarily required, a degradable polymer graft can be prepared with a degradation rate that can be fine-tuned according to the requirement.
Modern dentistry has now made it possible to prepare unique bone grafts using a combination of synthetic materials. For example, bone grafts are now available that combine the safety of ceramics with the bioactivity of bioglass and the flexibility of polymers. Today, even injectable polymer grafts have become available that are much easier to use and promote optimal bone formation and osseointegration.
Alternatives for Treatment
No matter how severe bone damage is, contemporary bone graft materials can fix virtually any type of bone deficiency. Today, bone grafts are even being used to reconstruct entire faces that were damaged as a result of an accident or oral tumours.
This is good news for patients who were previously unable to get their teeth replaced with dental implants due to insufficient bone density. Now, dentists can fine-tune and customize bone grafts according to every patient’s individual needs, not just to replace missing teeth but also to optimize facial aesthetics and restore optimal dental function.
Dr. Asghar is a dentist, an educator, and a researcher in dental biomaterials. He is currently working as an assistant professor in dental biomaterials at the National University of Medical Sciences, Pakistan, in addition to pursuing a PhD in dental biomaterials. His research interests include silver-based medicaments for dental use, nanoparticles, fiber-reinforced composites, dental polymers, and contemporary dental ceramics. Apart from his professional activities, he loves reading, writing, and working out. He is currently writing for Bond Street Dental as well.
Related Articles
Electrical Bone Mill Unit Regenerates Bone in 8 Minutes
A Conservative Approach to Immediate Bone Grafting
Bone Replacement Procedure Successfully Treats Children With Jaw Tumors











