INTRODUCTION
Gummy smile (excessive gingival display) is a condition in which a high lip-line exposes an abnormal amount of gingival tissue. Several potential factors could contribute to a gummy smile. For example, the muscle controlling the movement of the upper lip could be hyperactive, resulting in an upper lip that rises higher than normal. When this occurs, more of the gingival tissue is exposed when smiling. Other factors can include, but are not limited to, delayed passive eruption and factors related to the dentogingival complex.1-3
The smile-line is determined by the shape and size of the lips, the facial muscles, shape and size of the teeth, and the gingival tissue. Ideally, an aesthetic smile line should reveal the least amount of gingival tissue possible. Gum tissue present in the smile-line should exhibit balance with the contours in harmony with the upper lip. Since a gummy smile can have a negative affect on the aesthetics of a smile, one needs to consider various treatment options available to correct the condition when desired by the patient. One such option is the use of the soft-tissue diode laser treatment; this article will serve to explain and demonstrate the use of this treatment modality to aesthetically improve smiles that exhibit excessive gingival display.
CASE REPORT
Diagnosis and Treatment Planning
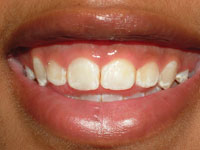
A 20-year-old female presented with the desire to improve the appearance of her gummy smile (Figure 1). Although she had undergone previous orthodontic therapy, she was still dissatisfied with her smile. The patient stated that she was often teased by her friends about having “baby teeth” (small teeth). The patient’s periodontal status was normal, and her medical history revealed that she was in good health with no significant findings.
Proper diagnosis is vital to the success of every potential aesthetic case. In this case specifically, the patient’s dental diagnosis was delayed passive eruption. The aesthetic issue was not a tooth problem, but a periodontal (gum) problem that had to be approached employing a periodontal treatment plan.
Clinical Protocol
The patient underwent a smile assessment and revealed 5 mm of gingival exposure when smiling (Figure 2). First, access and isolation were effectively achieved using a comfortable latex-free lip and cheek retractor (OptraGate [Ivoclar Vivadent]) (Figure 3). Tooth No. 8 measured only 8.9-mm long (Figure 4); the normal length of this tooth is between 10.5 mm to 11 mm.
 |
 |
| Figure 1. Preoperative views of the patient’s smile, revealing excessive gingival display. | Figure 2. The patient’s preoperative gummy smile was measured, revealing 5 mm of exposed gingival tissue. |
 |
 |
| Figure 3. Isolation and access was achieved with a latex-free lip and cheek retractor (OptraGate [Ivoclar Vivadent]). | Figure 4. The patient’s teeth and tissue were measured. The length of tooth No. 11 was 8.9 mm. |
 |
| Figure 5. After local anesthetic was administered, a periodontal probe with a 3-mm marking was used to sound to bone to determine the location of the osseous crest. |
Once local anesthetic was administered, a periodontal probe (Hu-Friedy) with a 3-mm marking was used to sound to bone to determine the location of the osseous crest (Figure 5) in all the anterior teeth to be treated. It was determined that the bone and cemento-enamel junctions were in the proper biological positions. Therefore, 2 mm of gingival tissue could be removed while maintaining the proper biological width for all the teeth involved in the procedure. The digital Boley gauge (Erskine Dental) was set to the determined length of the central incisor, and the gingival tissue was marked.
All proper laser hygiene protocols were followed, per the manufacturer, and the laser settings used were as per the manufacturer (eg, preset gingivectomy setting). The pre-measured and carefully planned tissue removal was carried out with the laser (Odyssey Diode Laser [Ivoclar Vivadent]) starting first on Tooth No. 8 (Figures 6a to 6d). The bone was again sounded with the periodontal probe to verify that a proper biological width had been established (Figure 7). Once treatment of tooth No. 8 was completed, tooth No. 9 was treated next in the same manner. Then, teeth Nos. 7 and 10 were treated. Once completed, final measurements were recorded. The immediate postoperative results were in line with the aesthetic treatment goals and patient goals to eliminate her gummy smile (Figures 8 and 9).
At the 6-week postoperative follow-up appointment, the patient stated that her adult teeth were finally in and that healing was completed in about a week. She was very pleased with the final result (Figure 10) and reported that she had not required any pain medications after the procedure. The final healed length of tooth No. 8 was 10.2 mm, and the healed length of tooth No. 9 was 8.6 mm. These final numbers are in line with the golden proportion commonly used in restorative dentistry.
DISCUSSION
 |
 |
 |
 |
| Figures 6a to 6d. Beginning with tooth No. 11, the laser tip (Odyssey Diode Laser [Ivoclar Vivadent]) was appropriately placed and the excess gingival tissue was removed according to previous preplanned measurements. |
The diode laser was ideal in this case because no osseous contouring was required. However, if the CEJ and the level of bone had been coincident, then traditional flap surgery and osseous contouring would have been required. These procedures can be done with minimal discomfort (often painlessly), fast, and with no sutures or packing required. In addition, no analgesics were required. In this 20-year-old patient who had presented with a gummy smile, this was the minimally invasive treatment method of choice to achieve an excellent aesthetic result.
Soft-Tissue Diode Lasers
Today, soft-tissue lasers are easy to use, portable, and affordable. These lasers (such as the Odyssey Diode Laser illustrated in this article, or ezlase (BIOLASE Technology), or Zap SoftLase Pro [Discus Dental], or Sirona SIROLaser Advance [Sirona Dental Systems]) are used for facilitating treatment of certain periodontal diseases, gingivectomy, gingivoplasty, tissue retraction, and other soft-tissue applications.
Soft-tissue diode lasers can help clinicians enhance their aesthetic dentistry procedures. Some models provide other conveniences such as: battery operation, light weight, and easy-to-use features, a clear and concise push-button control panel, LED screen display that indicates Continuous or Pulse output mode, and power (Watt) settings. It is also important to note that a soft-tissue diode laser’s consistent output ensures smooth and clean cutting.
| Lasers—It’s a Technique, Not a Procedure | ||||||||||||||||||||||||||||||
| Tom M. Limoli, Jr Code D7465 is the one and only procedure code that is specifically technique sensitive to the use of the laser. Rather than being surgically removed, a pathologic lesion is simply obliterated. The code definition and descriptor for this procedure simply reads: destruction of lesion(s) by physical or chemical method, by report. Examples include using cryo, laser, or electro surgery. For all other procedures where the laser is used, report the code that most accurately describes the intended procedure. For a frenectomy, the code is D7960. For a gingivectomy, the code is either D4210 (4 or more teeth per quadrant) or D4211 (one to 3 teeth per quadrant). For laser curettage, the incidental removal of soft tissue is part of D4341 and D4342 scaling and root planning—never to be confused or coded as D4260 osseous surgery. Simple bacteria reduction with the laser is part of D1110 prophylaxis and can only be accurately coded following scaling and polishing. We must remember that a laser is nothing more than an adjunctive instrument that is utilized to complete a more definitive procedure. You would not explain on the claim form that you used a No. 11 or No. 15 Bard-Parker blade. The carrier accepts no additional liability for the use of a laser or the use of a curved or straight blade. The code on dental procedures and nomenclature identify procedures, not specific techniques. The separate unbundled fee for the use of the laser is never appropriate as the technique is simply part of rendering the completed coded procedure. |
||||||||||||||||||||||||||||||
|
When clinicians consider purchasing a soft-tissue diode laser, it will behoove them to investigate a laser’s feature that can make its use easier and highly flexible. For example, some soft-tissue diode lasers have a touch-screen monitor with an intuitive design and navigation ability for simple and easy program selection and activation; an ergonomic handpiece; a wireless foot pedal or finger switch for easy activation; and unit-dose (disposable) fiber tips, so there is no need to cleave/strip the fiber prior to use.
In general, soft-tissue diode lasers promote less postoperative discomfort for the patient, and there is virtually no collateral damage to healthy tissue. Because soft-tissue lasers can cut and coagulate simultaneously, they contribute to immediate hemostasis with less tissue charring. Diode lasers, used in dentistry for soft-tissue surgical procedures, can range from 805 nm to 1064 nm. In studies conducted to determine the efficacy of a diode laser in reducing the bacteria that cause periodontal disease, one report (that focused on the use of diode lasers as an adjunct to conventional scaling and root planning) found that bacterial reduction was enhanced, bleeding on probing improved, and periodontal indices improved remarkably when the diode laser was used.4
 |
 |
| Figure 7. Once the laser excision of the excess tissue for each tooth was completed, the periodontal probe was then used again to sound to bone to verify that the proper biological width was established. | Figure 8. Postoperative retracted photo immediately after completion of laser treatment. |
 |
 |
| Figure 9. Full smile, immediately after laser treatment. | Figure 10. Retracted view showing the healed tissues at 6 weeks postoperatively. The final healed length of tooth No. 8 was 10.2 mm, and the healed length of tooth No. 9 was 8.6 mm. |
Interesting for practitioners using the diode laser for aesthetic gingival contouring applications, in another study that examined the use of a diode laser as an adjunct to conventional periodontal surgery, investigators studied such factors as pain scale assessment, pain medication, tissue edema, and tissue color—among other parameters—at 6-week and 5-month intervals.5 In this specific study, the researchers concluded that the use of the diode laser as an adjunct to periodontal surgery provided less postoperative pain and tissue edema and was safe for oral tissues.5
CONCLUSION
This article demonstrates that patients who present with excessive gingival display can be safely, easily, and effectively treated (when indicated) with minimal to no discomfort in the dental office with diode laser technology and proper training.
References
- Robbins JW. Differential diagnosis and treatment of excess gingival display. Pract Periodontics Aesthet Dent. 1999;11:265-272.
- Kois JC. Altering gingival levels: The restorative connection part 1: biologic variables. J Esthet Dent. 1994;6:3-7.
- Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11:29-38.
- Moritz A, Schoop U, Goharkhay K, et al. Treatment of periodontal pockets with a diode laser. Lasers Surg Med. 1998;22:302-311.
- Sanz Moliner J, Ciancio S. A diode laser as an adjunct to periodontal surgery. J Dent Res. 2009;88. Abstract 847.
Dr. Marangos is a graduate of the University of Toronto, Faculty of Dentistry, Canada and a graduate of the postgraduate program in aesthetic dentistry from State University of New York in Buffalo. He completed a general practice residency at Mount Sinai Hospital in Toronto. Dr. Marangos maintains a private practice in Toronto. He is the principal doctor at the Yorkville TMJ Centre. His professional affiliations and memberships include: Fellow of the American Academy of Craniofacial Pain (AACP), the International Academy of Dental Facial Aesthetics, and the Academy of Dentistry International; he is a Diplomate of the American Board of Craniofacial Pain, the American Academy of Pain Management, the American Academy of Orofacial Pain, the American Academy of Dental Sleep Medicine, the International Association for Orthodontics, the American Academy of Functional Orthodontics, the Canadian and Ontario Dental Associations, the American Academy of Cosmetic Dentistry, and the Toronto Academy of Cosmetic Dentistry. He is the immediate past-president of the AACP, Canadian Chapter. Dr. Marangos has written many articles. He was guest editor for Oral Health Journal’s edition devoted to TMJ disorders and craniofacial pain. Dr. Marangos has lectured for groups and study clubs. Dr. Marangos can be reached at (416) 465-9343 or via e-mail at dmarangos@rogers.com.
Disclosure: Dr. Marangos is a certified Ivoclar speaker and lectures on behalf of Ivoclar Vivadent.










