
Most advertising has the same basic strategy—convince consumers that they have a problem, and then offer a product to solve it. Whitening toothpaste is an example of how solutions sometimes make things worse.
I frequently see patients who inadvertently remove significant amounts of enamel by using toothpaste with an unnecessarily high relative dentin abrasivity (RDA). It’s tough to blame them for choosing a high-RDA toothpaste because few consumers know that the scale exists, and even when they do, manufacturers rarely publicize their figures.
The ADA recommends using toothpastes with an RDA value of no more than 250. Toothpaste manufacturers do not readily provide the RDA on the label of the tube of toothpaste. It is actually difficult to get it from their salespeople. They say that it is being changed all the time. Clinical studies may have the data, but there is no search engine that does an exhaustive comparison.
Many dental offices have put together their own information about RDA and have posted it to their websites. Some of the data may be a little outdated, but it is helpful in giving patients the general idea of how abrasive the toothpaste can be. Examples include:
- satyen.com/toothpastes.shtml
- healingteethnaturally.com/toothpaste-abrasiveness-index.html
- dendds.com/uploads/RDA_index.pdf
People typically choose their toothpaste on their own and then decide how to use it on their own. Their dentists and hygienists can help them avoid enamel loss and other unintended consequences by educating them about the RDA, the amount of toothpaste to use, and how to apply the right amount of pressure when brushing.
More ≠ Better
To patients, the concept of whitening seems so straightforward: more = better. More paste than necessary. More pressure than necessary. Commercials and print ads typically show the brush head completely covered with paste, which fuels the perception that more is better.
The initial result usually is noticeably whiter teeth. Patients take that as proof that they’re doing what they should and that the toothpaste is working as advertised. Some patients also reason that because they’re getting good results on their own, there’s no need to pay more for professional whitening. Dental-phobes often use this positive experience as another excuse to avoid the dentist.
But at this point, the flawed logic of more = better starts to kick in. The combination of high-RDA paste, aggressive brushing, and too much paste starts to remove enamel, revealing the dentin. This part of the tooth is naturally darker than enamel, so when patients start to notice shades of yellow or gray, they compensate by brushing even more aggressively.
Unless the enamel loss is so great that it causes sensitivity, patients won’t realize the problem they’re creating. They also may not understand the problem when their dentist notices it at their next cleaning.
Seeing is Believing
One way to get patients to appreciate the damage, and stop creating more, is by taking videos or still photos using a microscope, an intraoral camera, or even a digital single-lens reflex (SLR) camera. Regardless of the technology used, it’s important to shoot both the damaged areas and spots with ample enamel, typically between teeth. That way, patients can see the difference—and damage—for themselves (Figure 1).
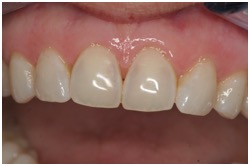 |
| 1. Abrasive toothpaste removed the enamel from these front teeth. |
 |
 |
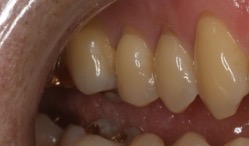
| 2. Excessive brushing or possibly bruxism caused this abrasion. |
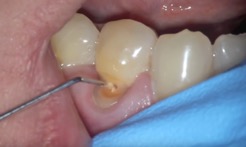 |
| 3. A cervical lesion can bring the pulp chamber close to the surface. |
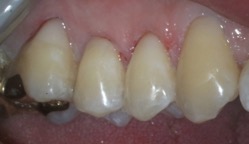
High-resolution photos or videos are useful for helping patients understand other types of damage caused by DIY whitening: grooves by the gumline and noncavity lesions (Figure 2). These problems often are accompanied by sensitivity. Switching to a low-RDA toothpaste helps because these products are formulated for sensitive teeth.
Many people are afraid to go to the dentist. Type A individuals, who are driven to succeed in whatever they do, often choose to overbrush to compensate for not going to the dentist. This past month, I have seen a CEO of a multinational company and an investment banker. They were terrified about going to the dentist.
The CEO had someone put him to sleep 10 years ago to do all his dental work at once. He had not been to the dentist since. He had removed the enamel and caused divots in the dentin for 12 of his teeth. The investment banker had the exact same issue with similar tooth loss. In both cases, they thought they were using the “right technique” in their brushing habits.
The noncarious lesions are a “Catch 22” if left alone. The dentin is more susceptible to decay if not adequately cleaned, while brushing too hard will remove the softer dentin faster. The more abrasive toothpastes can make the condition even worse by removing the tooth structure faster. The nerves of the teeth are closer to the cervical surface of the tooth, and an exposure of the pulp chamber can occur. This is a difficult situation to restore and may end up with tooth loss (Figure 3).
The earlier that dental professionals alert their patients about these problems, the better because if they advance, the restoration is expensive, including veneers and root canals. Patients are shocked when they learn that something as seemingly simple as DIY whitening can, and often does, cause major problems.
Ideally, dentists and hygienists should educate every new patient about how to choose a toothpaste, how to determine the right amount, and how much pressure to apply. Damage caused by DIY whitening is yet another example of how most people think they know how to care for their teeth and gums, but actually don’t. By the same token, this is an opportunity for dentists and hygienists to educate their patients on how to improve their hygiene and appearance in a safe manner.
Craig S. Kohler, DDS, MBA, MAGD, has been practicing on the North Shore of Chicago for more than 30 years. After completing his residency, he earned his Fellowship and master’s from the AGD by completing 1,600 hours of continued education. Dr. Kohler mentors at Evanston Hospital and is a visiting faculty member at the Spear Institute. He is the inventor of Prophix, the world’s first video toothbrush.
Related Articles
Dangers Lurk in the Illegal Tooth Whitening Market
Overcome the Barriers of Teaching Your Patients About Oral Hygiene
Use Video to Educate Your Patients and Keep Them Loyal











