INTRODUCTION
Appliance therapy has been a treatment modality for more than 40 years.1,2 “Bite appliances” or “bite planes” were words used interchangeably to describe a retainer-like device designed for one of several purposes. Some for pain relief, others to protect against teeth wear occurring from bruxism, and others aimed at specific therapy for temporomandibular joints (TMJ).3,4 All had differing techniques for construction and adjustment depending on their purpose.5 Rubber-type soft splints had little to adjust, while hard splints demanded excellent equilibration skills to properly deliver and maintain. Each had a design and purpose and therefore could not be used for the same situation.
These drawbacks left many practitioners confused about which appliance to use, and what the appropriate adjustment techniques were for each. Real practice time demands, patient compliance, and confusion over splint therapies have resulted in many dentists not using appliances at all. Yet their value has been proven, and many experts believe appliances should be considered an option for a large percentage of the adult patient population.6
Our access to the “information world” has allowed patients to better understand their problems and to be able to ask questions about the treatments that we are prescribing. More than ever before, this new source of external pressure, and the practitioner’s own internal desire to offer the best treatments possible, serves as genuine motivation to do what is right for all patients.
These pressures and drawbacks to splint use have resulted in a unique system: the E-appliance. Developed and patented by Dr. Jimmy Eubank, this therapeutic appliance is designed to fulfill physiologic criteria while being easy to deliver, monitor, and adjust.7 There is also an advantage not seen in other splints and previous splint therapies: it allows for more control of the bite and teeth stability. The E-appliance is a double-arch appliance: light, thin, and easier for patients to wear than thick single-arch splints. It covers all the teeth, allowing for the complete control of occlusion that anterior appliances cannot provide, and yet it is simple to adjust. It can be used for testing and therapy before definitive restorative treatment, for pain management, and after restorative treatment is completed for stabilization and maintenance.8
This article reports on 2 different case types and describes the versatility of the E-appliance. First, its physiologic benefits will be reviewed to demonstrate how the splint is used in each case.
PHYSIOLOGIC ACTION: JOINTS
One of the primary issues with patients in pain is the source. Most experts suggest the muscles are the cause of pain in more than 90% of the cases we see as dentists.9 Aside from a recent traumatic injury, that has been our experience as well. By using an E-appliance with its anterior bearing point, we can determine the source of pain and use it as a diagnostic tool.10 If true unstable internal derangement exists, there will be an increase in pain from using this type of appliance, thus diagnostic for TMJ damage.11
If there is no joint pain, we can move on to joint position.12,13 This has been another source of controversy with splint use. Capturing the best joint position has been described with several techniques. What’s great about this splint is the practitioner does not need special manipulation skills. By virtue of the splint design, all back teeth contact is removed. With the anterior bearing point and decreased muscle hyperactivity, the joint goes to its most physiologic position without dentist influence.14
If joint health is a question before treatment, this appliance works well to allow stability, disc variation due to remodeling, and determination of a repeatable position before the restorative phase.
PHYSIOLOGIC ACTION: MUSCLES
Muscles are hyper-activated by working and balancing interferences.15 This increases forces on the teeth and perpetuates teeth wear, lateral forces on posterior teeth, and pain in muscles due to lactic acid buildup.16 Single-arch splints designed to help this require precise adjustments so that no posterior tooth contact occurs, other than in an axial direction. Specific jaw manipulation techniques are needed to properly make adjustments so torsionally loading posterior teeth can be avoided.17 The extra manipulation and adjustment skill required results in many splints functioning poorly by leaving both working and balancing interferences “built” into them. Many good dentists, with all the best intentions for their patients, still struggle with appliance problems, and therefore bite stability.
The E-appliance is designed to eliminate posterior contact and let all inter-arch contact be contained on the flat plane area on the upper-arch splint. The full-arch splints essentially “blind” proprioception. When the lower bearing stylus contacts the flat plane, forces are generated in only the anterior portion of the splint; therefore less muscle pressure results.18 Without posterior interferences, the jaw positioning muscle (such as the lateral ptyergoid) decreases activity, letting the jaw seat in a natural position for that joint.19 This allows a release of muscle spasm and results in muscle pain reduction.20,21 The upper plane is designed to be very flat so that even the most muscular bruxer has little resistance when exerting right and left jaw movements. Both the lower stylus and the upper plane are polished acrylic, so the jaw literally slides right out when resistance is applied.
PHYSIOLOGIC ACTION: TEETH
Another advantage of the E-appliance is that it doesn’t have to be extra tight. Any action on the splint only serves to seat the appliance. No crossover can occur, so there is no need for tight splints to resist that type of jaw movement. When the splint is not as tight as previous single arch appliances, we see better patient compliance. Since the splint covers the entire arch, no one area of the teeth receives excessive pressure from bruxing like some anterior limited-coverage systems. By covering all the upper and lower teeth, mobility and teeth movement are eliminated, and so is orthodontic relapse.22 This will also limit furcation bone loss, diagnosed by periodontists as a condition of periodontal disease often complicated by secondary occlusal trauma.
Dentists have been told if the bite balancing is done right, the teeth will stay in position. Yet that has not been the experience of even the most skilled practitioners. Some patients do not stay balanced; with an E-appliance, the teeth will stay where you have adjusted them over time.
Because the appliance covers all the teeth, wear from clenching is controlled, and complex restorative work is protected.23 Aesthetic reconstruction can be done on some of the most abusive bruxers if they are wearing this appliance; a small price to pay for controlling the breakdown caused by such damaging jaw movements.24
CASE 1
E-appliance for Holdover Therapy and Pain Management
 |
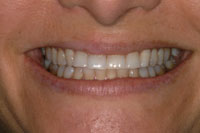 |
| Figure 1. Preoperative f ull-face. |
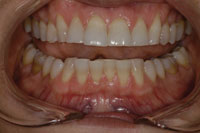
Figure 2. Pre-op. Anterior teeth look age-worn. |
 |
 |
| Figure 3. Pre-op. Worn anteriors flat posteriors. |
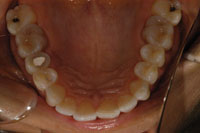
Figure 4. Pre-op. Occlusal view of fractured premolar. |
This 35-year-old female was unhappy with her smile. She had suffered jaw muscle pain for several years and believed that she was grinding her teeth at night. The initial exam revealed worn anterior and posterior teeth; tooth No. 4 had the lingual cusp fractured and required endodontic therapy. The masseter temporalis and lateral ptyerigoid jaw muscles were sore and tender, although no pain was evident in the jaw joints on loading (Figures 1 to 4).
During the initial interview, she reported being previously advised to have a full-mouth reconstruction done, and she was simply not ready to invest that much money. She was looking for an alternative to help her jaw problems, and to also look more attractive.
fter a complete work-up, we agreed to a plan of transitional therapy using composite resin to re-establish harmonious bite function while creating a more attractive smile. Tooth No. 4 needed endodontic treatment and a post-and-core restoration. Splint therapy, using the E-appliance during sleep, was agreed to in this case.
The patient wore an anterior deprogrammer the night before her bite balancing. She then reported for an all-day appointment, consisting of bite balancing, composite additions to teeth Nos. 6 to 11 (covering the middle and incisal two thirds of these anteriors), and rebuilding of tooth No. 4. Hybrid composite was used in all areas since strength was an emphasis during this transitional treatment. Upon completion, full-arch impressions were done for the E-appliance using crown and bridge impression materials. When balancing the bite, we eliminated working and balancing interferences, and therefore reduced forces during the day. The new anterior teeth not only looked better, but also helped establish the anterior guidance lost as a result of tooth wear. The E-appliance was used to keep the teeth from moving in both the upper and lower arches. With the splint’s anterior bearing point, we could reduce nighttime forces, protect all the teeth, and distribute clenching pressure all at the same time, with little adjustment. Her muscle tension and pain decreased during the day, and the E-appliance kept her jaw comfortable and without pain upon waking each morning.
 |
 |
|
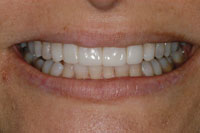
Figure 5. Postoperative at 2 years. |
Figure 6. Post-op, 2 years. Stable and attractive with composite resin. |
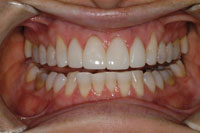 |
 |
| Figure 7. Post-op, 2 years. No breakdown occurring. |
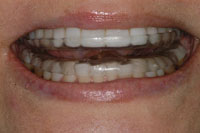
Figure 8. Post-op with E-appliance in place. |
These 2-year post-op photos show the improved appearance and the stability the E-appliance can help patients achieve (Figures 5 to 8). The additional height of the bearing point is required to account for her increased curve of Spee. This enables her to freely move her jaw at night and avoid any posterior contact.
At a recent hygiene appointment, she reported being ready to begin reconstruction with porcelain; she’s hoping to do this in phases. With this system and the E-appliance stability, we can easily meet her requests.
CASE 2
E-appliance for Stabilizing Full-Mouth Rehabilitations/Occlusions Over Time
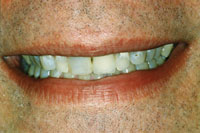
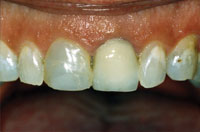
Any full-mouth reconstruction comes with a set of complications unique to each case. This 41-year-old male complained about his age-worn smile, jaw pain, and some fractured fillings. Repeated repairs had this patient wondering if there was another and better way. He felt his smile looked bad and that it detracted from his overall appearance; a better-looking smile was a primary concern (Figures 9 to 13).
 |
 |
|
Figure 9. Preoperative full-face. |
Figure 10. Pre-op. Worn and discolored. |
 |
 |
|
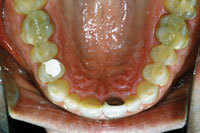
Figure 11. Pre-op. Uneven anterior wear patterns. |
Figure 12. Pre-op. Cracked and worn posteriors. |
 |
|
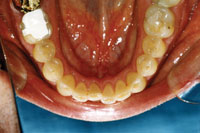
Figure 13. Pre-op. Wear rates increase with dentin exposure. |
His initial exam revealed many old fillings in various stages of disrepair. Tooth wear, cracks, and temporary patching were also evident in his posterior teeth. He acknowledged that he may clench his teeth, and that he had awakened on some mornings with jaw soreness.
After a comprehensive bite and aesthetic workup, we agreed to restore all the upper and lower teeth. During the work-up process, we found his periodontal health to be quite good. The breakdown was occurring with his occlusion and the restorations designed to protect and restore the teeth.
Laboratory construction of the restorations on precise articulators using specific guidelines requires close communication and common principles understood by both the clinician and the dental laboratory technician. The guidelines for full-mouth rehabilitation cases involve certain preparation, prototypes, and bonding techniques. Each stage was aimed at resolving the aesthetic and occlusal problems. Building the anteriors to look good and also protect the posterior teeth in ecce
ntric movements was the goal of this segment of treatment. Posteriors that contact evenly and at the same time were also important criteria. No contacts should be on slopes so we could avoid hyperactivating jaw muscles. All centric stops were to be in harmony with the patient’s natural jaw joint position. All these goals are common with many cases; yet, on delivery and subsequent follow-up, it is difficult to keep the occlusions stable and functioning exactly where we intend. That is where the E-appliance plays a major role.
 |
 |
|
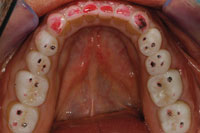
Figure 14. Post-op at 7 years. Maintained posterior stops over time. |
Figure 15. Post-op, 7 years. The E-appliance eliminates posterior interferences. |
 |
 |
|
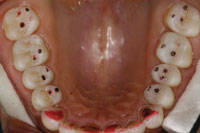
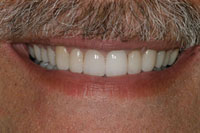
Figure 16. Post-op at 7 years. |
Figure 17. Post-op, 7 years. Attractive and stable rehab. |
 |
|
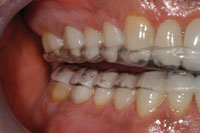
Figure 18. E-appliance, showing posterior separation. |
Once the case was completed and the bite appropriately balanced, the E-appliance was delivered as usual. Wearing this device will turn off muscle activity and allow the joint to fully seat each night. Avoiding muscle hyperactivity means pain-free jaws in the morning. The splint also keeps the teeth from shifting; therefore occlusal contacts not appropriate for an individual tooth can be easily detected and removed. As a result, daytime occlusal management can be done more simply. At times in the past, we chased around occlusal stops, adjusting and hoping some stable place would finally be achieved. If patients felt good and nothing was breaking, we called this an occlusal “success.” Now, we can apply exacting accuracy by checking for stable tooth contacts, and working and balancing interferences, at hygiene intervals. By using the E-appliance, we have found our patients’ occlusions to be very stable.
The 7-year post-op photos shown in Figures 14 and 15 indicate the absence of eccentric contacts in the posterior, yet solid centric stops remain. This patient has been very comfortable and stable with his occlusion. Unlike before, the treatment that we provided, which included use of the E-appliance, resulted in occlusal stability, thus obviating the need for continual and repeated repairs/patching (Figures 16 to 18). There really was another outcome possibility that proved both predictable and stable!
|
Appliance Therapy: Treating the Joint, Muscle, Teeth, Bone…
Or Simply the Patient? |
|||||||||||||||||||||||||||||
|
Tom M. Limoli, Jr
|
DISCUSSION
Patient Advantages
Any device that relieves pain is always popular with patients. With the E-appliance, pain reduction is a strong benefit. In our experience, we have also noted that compliance is much better than found with many single-arch (“thick”) systems. Tooth pain and temperature sensitivity resulting from excessive forces is also improved or eliminated. Adults completing orthodontics or complex restorative (as in Case 2) will not experience relapse by using an E-appliance.
The E-appliance system is also helpful when used with restorative treatment. By stabilizing the damaging occlusal conditions, it allows patients to spread out their treatment in phases (as in Case 1). When faced with complex treatment, some patients cannot afford to proceed at all. The E-appliance can prevent further damage from bruxism until they are ready. When combined with preventive hygiene and caries removal, this works well as a “holdover option” for those who desire it.
Doctor Advantages and Protocol
The E-appliances are easy for offices to deliver, since all the design and fabrication of the patented splint is done by Esthetics Unlimited Laboratory. Bite recordings are simple to do; no special manipulation is needed to properly fabricate the double-arch appliance. Curve of Spee is accounted for by the vertical dimension of the splint so that all jaw movements result in posterior separation. In the 2 cases presented here, the stylus and height were adjusted for us by the dental laboratory technician for exactly that reason.
Many doctors have delegated the records and delivery to auxiliary team members. Patients should bring their appliances to hygiene appointments for cleaning and evaluation.
Since the E-appliance is self-adjusting, the follow-up is very easy. Without the stress of precise manipulation, doctors are able to know the best muscle/joint position for the patient with much less effort. Because the design of the E-appliance separates joint pain from muscle pain, it is a very useful tool for dentists to help determine if they should treat the patient or refer to the TMJ specialist.
CLOSING COMMENTS
We have been using the E-appliance in our office for more than 8 years. Since its introduction, it has been retooled and improved over time. In the author’s opinion, appliance therapy for most patients has never been easier.
References
- Dyer EH. Importance of a stable maxillomandibular relation. J Prosthet Dent. 1973;30:241-251.
- Beard CC, Clayton JA. Effects of occlusal splint therapy in TMJ dysfunction. J Prosthet Dent. 1980;44:324-335.
- Burns R, McKinney J, Chase D, Anderson D: Occlusal splint therapy for treatment of internal derangements: retrospective study. J Dent Res. 1983; 62: Abstract No. 1215.
- Magnusson T, Carlsson GE. Recurrent headaches in relation to temporomandibular joint pain-dysfunction. Acta Odontol Scand. 1978;36:333-338.
- Quayle AA, Gray RJ, Metcalfe RJ, et al. Soft occlusal splint therapy in the treatment of migraine and other headaches. J Dent. 1990;18:123-129.
- Kampe T, Tagdae T, Bader G, et al. Reported symptoms and clinical findings in a group of subjects with longstanding bruxing behaviour. J Oral Rehabil. 1997;24:581-587.
- Eubank JB. Phased treatment for complete dentistry. Dent Today. 2008;27:68-73.
- Wichelhaus A, Hüffmeier S, Sander FG. Dynamic functional force measurements on an anterior bite plane during the night. J Orofac Orthop. 2003;64:417-425.
- Mongini F. Assessment of craniofacial pain and dysfunction: a multidisciplinary approach. Cranio. 1990;8:183-200.
- Bell WE. Temporomandibular Disorders: Classification, Diagnosis, Management. Chicago, IL: Year Book Medical Publishers; 1986.
- Wabeke KB, Hansson TL, Hoogstraten J, et al. Temporomandibular joint clicking: a literature overview. J Craniomandib Disord. 1989;3:163-173.
- Ito T, Gibbs CH, Marguelles-Bonnet R, et al. Loading on the temporomandibular joints with five occlusal conditions. J Prosthet Dent. 1986;56:478-484.
- May BM, Garabadian C. Reducing condylar compression in clenching patients. Crit Rev Biomed Eng. 2000;28:389-394.
- Manns A, Miralles R, Valdivia J, et al. Influence of variation in anteroposterior occlusal contacts on electromyographic activity. J Prosthet Dent. 1989;61:617-623.
- Mahan PE, Wilkinson TM, Gibbs CH, et al. Superior and inferior bellies of the lateral pterygoid muscle EMG activity at basic jaw positions. J Prosthet Dent. 1983;50:710-718.
- Steele JG, Lamey PJ, Sharkey SW, et al. Occlusal abnormalities, pericranial muscle and joint tenderness and tooth wear in a group of migraine patients. J Oral Rehabil. 1991;18:453-458.
- McKee JR. Comparing condylar positions achieved through bimanual manipulation to condylar positions achieved through masticatory muscle contraction against an anterior deprogrammer: a pilot study. J Prosthet Dent. 2005;94:389-393.
- Manns A, Rocabado M, Cadenasso P, et al. The immediate effect of the variation of anteroposterior laterotrusive contacts on the elevator EMG activity. J Cranio. 1993;11:184-191.
- Belser UC, Hannam AG. The influence of altered working-side occlusal guidance on masticatory muscles and related jaw movement. J Prosthet Dent. 1985;53:406-413.
- Shupe RJ, Mohamed SE, Christensen LV, et al. Effects of occlusal guidance on jaw muscle activity. J Prosthet Dent. 1984;51:811-818.
- Kerstein RB, Wright NR. Electromyographic and computer analyses of patients suffering from chronic myofascial pain-dysfunction syndrome: before and after treatment with immediate complete anterior guidance development. J Prosthet Dent. 1991;66:677-686.
- Parfitt GS. Measurement of the physiologic mobility of individual teeth in an axial direction. J Dent Res. 39:68,1960.
- Kydd WL, Daly C. Duration of nocturnal tooth contacts during bruxing. J Prosthet Dent. 1985;53:717-721.
- Grippo JO. Abfractions: a new classification of hard tissue lesions of teeth. J Esthet Dent. 1991;3:14-19.
Dr. Orser graduated Loyola University with a BS in psychology, Loyola Dental School with a DDS, and completed a general practice residency from Rush Medical Center. He is a member of the American Equilibration Society and the ADA, and he is an accredited member of the American Academy of Cosmetic Dentistry. He teaches at the Eubank Teaching Institute and is founder and senior partner of Arlington Adult Dentistry in Arlington Heights, Ill. He is a past reviewer of cosmetic articles for the ADA Journal and has previously published in the Journal of Cosmetic Dentistry and Dental Economics. He can be reached at [email protected].
Disclosure: Dr. Orser has no financial interests in, or benefits from the owners and developers of the E-appliance.
If you are interested in utilizing the E-appliance as a part of your patients’ treatment, contact Esthetics Unlimited Laboratory at (972) 596-1811 or send e-mail to [email protected].


