Experiencing our profession as a doctor-technician liaison is like looking through a unique, interdisciplinary window into our complex technological and relationship-based professions. This has allowed me to have an insider’s look at many of the current “realities” in both dentistry and dental technology. In this journey I have been able to make many interesting observations and identify some of the defining challenges facing our interdependent industries. Without a doubt, we are in demanding professions that require careful examination and thoughtfulness in everything we do. Consequently, some of my observations may seem a bit critical at first glance. However, I report them with a sincere and passionate desire to positively impact how we practice dentistry and how we relate to one another. Only by acknowledging the existence of our challenges can we become empowered to visualize, create, and implement solutions in coordination with our entire professional team.
HIGH OCCLUSION: SHARING IN THE RESPONSIBILITY?
 |
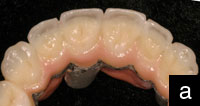
| Figure 1. A complex anterior restorative case being done on a simple, hinged ìarticulatorî that is not matched for the task. Note the degree of wear on the mandibular anterior teeth and lack of restorative space. Consider the resulting challenges and limitations that the dental technician will face in fabricating this case. (The anterior teeth in function are the principal determinant of occlusal form and function, according to Dr. P.E. Dawson and others.2) |
During the time I have served as a doctor-technician liaison, doctors have understandably shared both their positive and negative experiences in working with their dental laboratories. One topic that seems to be a repeated concern is the frustration inherent in delivering restorations that require major occlusal adjustments, with a corresponding significant loss of valuable chair time and elevation of stress levels. According to a recent survey, one of the most common problems doctors reported with their dental laboratory work was poor/high occlusion.1 This is a legitimate problem and can definitely be a result of a number of technical errors in the laboratory. Much of the problem could even be related to the articulation devices that our laboratories select and use in creating restorations for us. This is a topic that deserves a deeper look, and we will explore it later in this article when we examine what is going on inside our dental laboratories.
With regard to high occlusion, many doctors tend to “correct” this problem by asking their dental technicians to compensate in advance for any potential occlusal errors. Fabricating restorations out of occlusion often becomes the prescribed solution. I have personally observed many cases that dental technicians created with arbitrary amounts of visible space between the restorations and opposing teeth in an attempt to avoid adjustment at the seating appointment. This can also be how a technician unilaterally solves the problem. Perhaps it is done because the technician and/or doctor may not fully understand how to fabricate and deliver restorations with correct interocclusal relationships. Unfortunately, out-of-occlusion cases are often delivered despite the knowledge that the teeth (restored and opposing) can potentially erupt, drift, and/or rotate into functional disharmony.
When asked about this problem, dental technicians tell us that they are often expected to work with poorly executed, dual-arch tray impressions that may have been used in contraindicated situations. Sometimes these cases present with only a few teeth in occlusion. Bite registrations, if taken, have usually been done after the patient has been anesthetized and worked on for various lengths of time, thus directly affecting the accuracy of the recorded bite. Consequently, the dental technicians often find themselves taking their best guess to articulate models with the ìrightî relationship. Add to this the impact that untreated (not diagnosed?) occlusal pathology/neuromuscular disharmony can have on the task of achieving occlusion with proper function on a simple, nonadjustable “articulator” (Figure 1). This can be further complicated when a technician attempts to relate incomplete portions of a patientís dental arch together.
WHAT CAN WE DO DIFFERENTLY?
Fallout from this kind of approach to care takes a heavy toll on our profession both financially and psychologically. According to the aforementioned survey,1 73% of doctors stated that they use 3 to 5 dental laboratories; 28% of respondents stated that they have changed laboratories in the past 2 years. Of these doctors, 66% cited inconsistent quality as a factor. These statistics are really just symptoms of underlying technical, business, and relationship challenges that most often require a multilevel team approach for solutions.
We should address the myths, misunderstandings, and other barriers that are halting us from moving in a positive way toward viable solutions. We need to minimize any excuses and rediscover the motivating factors for uncompromising dentistry. Too many times we look exclusively for quick technical fixes to our challenges. To initiate long-lasting changes in our technical and business behaviors, it is prudent to look at our current belief systems to understand why we do what we do, and why we are not doing what we could be doing.
SIMPLE, HINGED “ARTICULATORS”: WHY SO LOW-TECH IN SUCH A HIGH-TECH PROFESSION?
I recently wrote articles about the role of accurate preparations and impressions to help our dental technicians give us the best possible fit, function, and aesthetics.3,4 While these are important areas to consider, there is another vital topic that deserves our consideration. Why is the vast majority of restorative work in our dental laboratories being done with low-tech articulation instrumentation in an otherwise increasingly high-tech field of dentistry? Why are almost all face-bows and semiadjustable articulators put into storage upon our graduation from dental school? What is the dental technicianís role in this? Why should we change? How?
One could probably sum up what many are thinking like this: “Give me a break! Itís overkill to start using face-bows and articulators for all my simple (CO) cases. This really does not apply to me because I am doing just fine with my current techniques. Furthermore, all this stuff is expensive, time-consuming, and way too complicated.”
With all due respect, with our emphasis in the last few years beginning to refocus on the importance of considering both aesthetics and function to ensure patient comfort and restorative longevity, it is crucial that we challenge the status quo governed by our commonly held beliefs regarding the use, or lack of use, of more accurate articulation systems.
SOME POSITIVE MOTIVATION FOR CHANGE!
Before we go any further, let’s consider a patient-centered point of view. Within the best of our abilities and available technology we should complete all dental work with functional correctness regardless of the number of teeth to be restored. We have all seen and treated patients who belong to the “crown-of-the-month”club, who have been restored tooth by individual tooth into functional and aesthetic disharmony. Imagine how different their outcomes could have been with proper time given to diagnosis and treatment planning that considers function, aesthetics, and desired longevity. Think about it. If we were the patient, within what degree of occlusal accuracy and comfort would we like to be able to function?
WHAT’S GOING ON IN OUR LABORATORIES?
 |
 |
| Figures 2 and 3. Examples of simple, nonadjustable, hinged “articulators” currently in use in many dental laboratories. |
Make it a point to visit your dental laboratory sometime soon if you do not already do so on a regular basis. Check out the usual methods of articulation being used. What kind of “articulators” do you see in the case pans? Are they matched appropriately to the level of complexity of the cases? How many semiadjustable or fully adjustable articulators are in use? Are they clean and fully functional? Are the dental technicians trained in how to use these instruments? Are they being used regularly, or are they gathering dust on a storage shelf in the laboratory?
What you will find in the vast majority of labs, small and large alike, are triple-tray (dual-arch) cases being routinely fabricated on various simple, hinged devices that manufacturers, technicians, and doctors refer to as ìarticulatorsî (Figures 2 and 3). These ìarticulatorsî should be more accurately called “hold-the-case-together” devices. Why? Because that is all these basic, hinged devices are capable of doing! They cannot replicate anything close to the human movements of the jaws and teeth. What could be more ironic than one manufacturer claiming to have better quality of function over a competitor with these simple “articulators”? Since they are disposable, they are no doubt extremely profitable for the companies producing them. As a result, there is no financial incentive for “hold-the-case-together” device manufacturers to initiate or desire changes that support a higher level of patient care. Furthermore, most of us do not consider the real cost of disposable “articulators.” Be-cause the cost of these is passed on (hidden or buried costs) from the laboratory to the doctor, they are not really a focus of attention. Combine these hidden and repeated expenses with the loss of chair time due to greater inaccuracy, and the cost is staggering over a practice lifetime. This is especially true in comparison to owning one quality, interchangeable, semiadjustable articulator.
What, then, are the requirements that determine acceptability of an instrument capable of producing consistent and predictable end results? Dr. Peter E. Dawson5 states, “The single most important purpose of an articulator is to relate the lower cast to the upper cast in centric relation. To accomplish this relationship and maintain it during any change of vertical dimension, both casts must have the same relationship to the horizontal axis on the articulator that the dental arches have to the condylar axis on the cranium. So the first requirement for acceptability of an articulator is that it must accept a face-bow mounting. Reproducing the horizontal axis is the essential first requirement because the accuracy of all other relationships depends on a correct starting point.”
In my opinion, it cannot be said any better or with more clinical and academic experience than that. So why are we routinely using inferior disposable devices and associated techniques that do not incorporate any of the above principles?
BUSTING THE MYTHS!
 |
 |
 |
| Figures 4 to 6. Examples of quality, semiadjustable articulator systems that allow the operator to easily and quickly accomplish face-bow recordings. Each system can be accurately calibrated to allow multiple cases to be done on the same articulator utilizing magnetic mountings. Figure 4 is the Artex Carbon (arcon) Articulator System (Jensen Industries); Figure 5 is the Stratos Articulator (shown with a calibration device in place) by Ivoclar Vivadent; and Figure 6 is the SAM 3 Articulator (Great Lakes Orthodontics). |
Letís address the myths behind the common reasons that we fail to use more accurate articulator systems. We need to re-examine part of the statement quoted earlier in this article: “…all this stuff is expensive, time-consuming, and way too complicated.”
This statement typifies what many of us have heard expressed so repeatedly and by so many over time that it has become a belief statement. If we look more closely, it really sums up the 3 reasons (cost, time, fear) that most doctors and their dental technicians avoid more accurate articulator systems for routine use in their diagnostic and restorative care. To challenge this thinking, letís ask some basic questions related to the tri-part essence of the statement:
- Cost. If the one-time cost of a quality semiadjustable articulator system is considered over the lifetime of your practice, does that make the amount seem more palatable in comparison to other expenditures, including thousands of disposable ìarticulatorsî? What if you could find an articulation system with which you need to own only one articulator to accomplish multiple, simultaneous cases? One that utilizes dependable calibration and a magnetic mounting system that allows you and your laboratory technician to transfer cases from one instrument to another (interchangeable) without sacrificing accuracy? If you could achieve better precision, thereby increasing the level of your work and reputation (referrals!), how would this affect your perception of cost versus the return on investment? Over the life of your practice, how much does it cost you to perform all the extra and unnecessarily difficult occlusal adjustments at seating appointments with restorations fabricated via low-tech “articulators”? (Solving this with an out-of-occlusion approach is not considered an acceptable treatment standard.) Is accuracy more than just a cost benefit to you, your team, and your patients?
- Time. Do you believe that time is money? Did you know that a face-bow can be completed in as little as 5 minutes by a dental assistant who is trained in these concepts and procedures? Is it worth it to take a little up-front time to relate dental casts together properly on a horizontal axis and an initial arc of rotation that is at least much closer to that of the patient? (Clinical Tip: When using semiadjustable articulators with arbitrary, aesthetic plane of occlusion face-bows, cases should be mounted with a bite registration taken as close to the same OVD to which the case is to be restored. This is to ensure the best possible accuracy as it relates to the initial arc of rotation as recorded in a nonhinge axis recording.)
- Fear. If you and your team are well-trained in face-bow and mounting procedures and find them understandable and simple to accomplish, would you still have fear and anxiety of the unknown? Is the only thing we have to fear, fear itself?
So what is the bottom line? All 3 of the aforementioned reasons for avoiding better articulation technology will quickly evaporate if you and your team are willing to make a commitment to change. High-quality articulator systems are on the market that will make it easier than you think to accomplish restorations with both better occlusion and aesthetics. The Artex Carbon Articulator available in arcon and non-arcon versions (Jensen Industries), SAM 3 Articulator (Great Lakes Orthodontics), Stratos Articulator (Ivoclar Vivadent), Panadent Articulator (Panadent), and the Whip Mix 2000 Series Articulator (Whip Mix) are a few examples of cost-effective instrumentation that will make a noticeable difference in how well you and your dental technicians will be able to accomplish diagnostic and restorative procedures (Figures 4 to 6).
CONCLUSION
If we are not vigilant, any of us can find ourselves practicing day-in and day-out with techniques that are in serious need of improvement without really noticing or challenging the “way weíve always done it.” We must learn to work closely together with our laboratory technicians in order to accomplish the best in form, function, and aesthetics in our indirect restorative work. This involves gaining more knowledge than we left dental or dental technology school with, by listening to and learning from everyone on our team. We must be willing to reach out and support one another through the decisions and learning curves faced when we introduce better articulation systems into our practices and dental laboratories. With relatively minor changes and sound investments that return positive rewards, we have the ability to improve the quality of our services dramatically. Letís work together to challenge and improve upon the status quo!
References
- Dental Products Report 2003 Communications Survey, mailed December 2004.
- Dawson PE. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd ed. St Louis, Mo: Mosby-Year Book; 1989:274-297.
- Adams DC. The ten most common all-ceramic preparation errors: a doctor/technician liaison’s perspective. Dent Today. Oct 2004;23:94-99.
- Adams D. Impression distortion-only a technical problem? A doctor/technician liaisonís perspective. Dent Today. Dec 2005;24:66-70.
- Dawson PE. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd ed. St Louis, Mo: Mosby-Year Book; 1989:206, 274.
Suggested Reading
Ahlers MO. Simulation of Occlusion in Restorative Dentistry. Hamburg, Germany: dentaConcept; 2000. Available by calling Jensen Industries Inc, 800-243-2000.
Dawson PE. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd ed. St Louis, Mo: Mosby-Year Book; 1989: chap 12, 13, and 16.
Dr. Adams, a graduate of the University of Michigan, is an assistant clinical professor at the University of Toledo College of Medicine, Division of Dentistry. He presents seminars and workshops internationally that are primarily devoted to doctor-laboratory/techno-clinical issues and to improving doctor-technician relationships. He is listed in Dentistry Todayís Annual Top Clinicians in CE and is also a Contributing Editor for Dentistry Today. Dr. Adams can be reached at (231) 642-7785 or damona11@hotmail.com.
Disclosure: Dr. Adams has no financial interest in any of the companies mentioned in this article.