The number of direct composites being placed by dentists in the United States has climbed rapidly in the last 10 years. According to a 2003 survey, 92% of patients preferred composite resin fillings for aesthetic reasons. In the same survey, 61% of dentists stated that direct composites were preferred because they represented a more conservative restorative choice.1 In May 2002, the American Dental Association reported that 61% of dentists had decreased the use of amalgam.2 Another survey in 2003 put the figure at 71%.1 A report in June 2002 noted that the number of direct composites was eclipsing the number of amalgams being placed in the United States.3
 |
 |
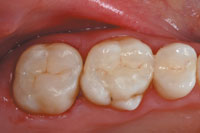
| Figure 1. Indirect composite onlay tooth No. 3 and inlay tooth No. 5 (Concept, Ivoclar Vivadent), 6 years post-op (Courtesy of DH Baker Dental Laboratory, Inc). | Figure 2. Before placement of Concept HP indirect composite restoration. |
 |
 |
| Figure 3. After placement of Concept HP indirect composite restoration (Figures 2 and 3 courtesy of Ivoclar Vivadent; clinical/laboratory procedures accomplished by Dr. Ed Lowe and Nelson Rego, CDT). | Figure 4. Existing amalgam restorations. |
 |
 |
| Figure 5. Teeth prepared for indirect composites. | Figure 6. Postoperative placement of belleGlass restorations (KerrLab; clinical/laboratory procedures accomplished by Dr. David Hornbrook and Douglas Baker, CDT). |
While the use of direct composites has steadily increased, the laboratory industry has witnessed a much slower growth in the use of laboratory-fabricated indirect composite restorations. This is despite positive reports in the literature regarding the clinical performance of certain indirect composites when prescribed for conservative inlays and onlays in patients presenting without serious occlusal pathology4 (Figures 1 through 3). Respected international lecturers have also recognized that indirect composites can be a viable treatment for moderately broken down teeth5 (Figures 4 through 6). Even though there are many clinical situations amenable to the placement of direct composites, we would also expect to see more frequent use of indirect composites when indicated. Why is the growth rate of indirect composites not paralleling that seen with direct composites?
CHOOSING A MATERIAL
Are there misconceptions or preconceived beliefs regarding the best material choice in certain situations? For example, when should one choose a direct composite, an indirect composite, or a porcelain restoration? Consider the following observations in a comparison of direct and indirect composites:
Direct Composites
•Can be the most conservative restoration, when indicated.
•Interproximal contacts are a challenge and their quality is commensurate with operator skill working in the adverse conditions of the oral cavity.
•Aesthetics and occlusion are also commensurate with operator skill working in the adverse conditions of the oral cavity.
•Microleakage with direct composites is still a problem due to polymerization shrinkage (up to 5%), despite a variety of currently proposed clinical steps to reduce this effect.9-11 Polymerization shrinkage becomes a greater problem as the size of the restoration increases. The degree of microleakage is also relative to the bond strength as affected by the position of the cervical margin in relation to the CEJ, and therefore the quality and strength of the enamel and dentin bond to the restorative material.12,13
•Indicated as ideal for incipient to small lesions. Not suitable for moderately to severely broken down teeth that may require coverage of the cusp(s), or in bruxers.
•Lower cost.
Indirect Composites
•Tooth conservation for inlays is less for indirect composites compared with direct composites because of a divergent preparation and other reduction requirements. Conservation of tooth structure is greater with indirect composite onlays than with full-coverage crowns.14
•Interproximal contours are observed to be superior to those created by most clinicians because they are fabricated on removable dies by a skilled dental technician.
•Aesthetics are observed to be superior to those created by most clinicians as they are created outside the oral cavity by skilled dental technicians.
•Compared with direct composites, indirect composites provide superior physical properties (wear, strength, longevity, and margins) and dramatically reduced polymerization shrinkage due to better and more complete curing methods.15-18 The curing methods include a variety of combinations of heat, pressure (in a nitrogen atmosphere, water, etc), light, and vacuum, outside the oral cavity. In most cases, these indirect materials are microhybrid composite variations on proven direct composite resin systems. Examples are Herculite XRV (Kerr) and belleGlass HP (KerrLab).
•Indicated for the moderately broken down tooth where the lesion is too large or the restoration will be under too great an occlusal load for a direct composite (or nonsupporting amalgam), yet the placement of a full-coverage crown is considered too aggressive.19 Not indicated for incipient lesions, severely broken down teeth, or in bruxers.
•Higher cost. (Two visits required, plus laboratory fees.)
WHAT ABOUT PORCELAIN INLAYS AND ONLAYS?
When comparing wear of the opposing enamel between indirect composites and porcelain, indirect composites hold a definite advantage.23 Some studies suggest that indirect composite inlays and onlays also hold the edge with respect to the long-term quality of margins. Margins are still one of the keys to restorative success. The longevity of indirect restorations of any type depends on the integrity of the margins at placement, despite the intoxicating temptation that can be found in a short-term “cover-up” of deficiencies with the use of resin cements. In a recent 8-year in vivo study of fired ceramic inlays, the margins were observed to have 22% visual microfractures and 77% microfractures under scanning electron microscope (SEM).24 Another study of pressed-glass ceramic inlays and onlays, after 6 years in vivo, showed 94% with margin deficiencies.25 In contrast, the margins of indirect composites seem to be faring much better. In 1992, Van Meerbeek et al26 reported in a 5-year in vitro wear study under SEM that 60% of indirect resin margins are gap-free. In 1996, Van Dijken and Horstedt27 reported that 84% of indirect resin inlays were gap-free at 5 years in vivo. A recent 3-year study, reported in the Journal of the American Dental Association in 2000, compared direct composites with indirect composites. It concluded that the margins of indirect composites were “rated consistently higher than direct composites.”18
CONCLUSION
The indirect composite restoration can be an excellent choice for our patients when indicated. For optimal success, it is vital to choose a laboratory that creates the restoration with aesthetic and functional excellence. Ideally, in the spirit of teamwork, the laboratory should be willing and capable of giving the doctor a level of technical support commensurate with their level of knowledge and experience. Treatment plans should reflect the differences in individual clinician’s abilities as well as the patient’s varying aesthetic desires, and functional needs.
Because there is no ideal “one-fits-all restorative system” that can be successfully applied to every clinical situation, it continues to be the doctor’s responsibility to select the appropriate materials and techniques for each patient after a thorough exam, diagnosis, and co-discovery process. This holds true for indirect composites as it does for any other class of dental materials. There is a time and place for any well-done direct or indirect composite, gold, PFM, all-ceramic, or amalgam restoration. Choose wisely to maximize the benefits for the patient, and everyone involved will succeed.
References
1. Goff S. What about amalgam? 600 GPs respond to usage survey. Dental Products Report. 2003;37:124-126.
2. Dental Practice (table). ADA News. 2002; 33(10):4
3. Berthold M. ADA News. 2002;33:1,10-11.
4. Donly KJ, Jensen ME, Triolo P, et al. A clinical comparison of resin composite inlay and onlay posterior restorations and cast-gold restorations at 7 years. Quintessence Int. 1999;30:163-168
5. Jackson RD. Indirect resin inlay and onlay restorations: a comprehensive clinical overview. Pract Periodontics Aesthet Dent. 1999;11(8):891-900.
6. Adams D. Know the CDT4 code changes for indirect composite resin restorations. Dental Insurance Today. 2003;16(2):3.
7. Suzuki S, Nagai E, Taira Y, et al. In vitro wear of indirect composite restoratives. J Prosthet Dent. 2002;88:431-436.
8. Miller M. Resin cements. Reality Now. 2003;153:1-2.
9. Davidson CL, Feilzer AJ. Polymerization shrinkage and polymerization shrinkage stress in polymer-based restoratives. J Dent. 1997;25:435-440.
10. Russell RR, Mazer RB. Should flowable composites be used as liners for Class II restorations? J Dent Res. 1999;78:389. Abstract 2266.
11. Hilton TJ, Ferrance JL. Cavity preparation factors and microleakage of Class II composite restorations filled at intraoral temperatures. Am J Dent. 1999;12:123-130.
12. Fitchie JG, Roberts B, Anderson L, Puckett A. Radioisotope and dye microleakage evaluation of three single bottle adhesives [abstract]. J Dent Res 1999; 12:154 Abstract 391.
13. Haak R, Losche G, Roulet J. Bond strength of composite resin to cervical enamel and dentin [abstract]. J Dent Res 1996;75:41. Abstract 190.
14. Dietschi D, Spreafico R. Adhesive Metal-Free Restorations: Current Concepts for the Esthetic Treatment of Posterior Teeth. Carol Stream, Ill: Quintessence Pub Co; 1997;79-99.
15. Ferracane JL, Condon JR. Post-cure heat treatments for composites: properties and fractography. Dent Mater. 1992;8(5):290-295
16. Cook WD, Johannson M. The influence of post-curing on the fracture properties of photo-cured dimethacrylate based dental composite resins. J Biomed Mater Res. 1987;21(8)979-989
17. Bennett ME, Puckett AD, Parsell DE, Roberts SB, Conversion of a heat and pressure cured composites [abstract]. J Dent Res.1996; Abstract 2188.
18. Manhart J, Neuerer P, Scheibenbogen-Fuchsbrunner A, et al. Three-year clinical evaluation of direct and indirect composite restorations in posterior teeth. J Prosthet Dent. 2000;84:289-296.
19. De Moor RJ, Verbeeck RM, De Maeyer EA, Fluoride release profiles of restorative glass ionomer formulations. Dent Mater. 1996;12:88-95
20. Strang R, Whitters CJ, Brown D, et al. Dental materials: 1996 literature review. J Dent. 1998;26:191-207.
21. Morin D, De Long R, Douglas WH. Cusp reinforcement by acid-etch technique. J Dent Res. 1984;63:1075-1078.
22. Van Meerbeek B, Perdigao J, Lambrechts P, et al. The clinical performance of adhesives. J Dent. 1998;26:1-20.
23. Hayashi M, Tsuchitani Y, Kawamura Y, et al. Eight-year clinical evaluation of fired ceramic inlays. Oper Dent. 2000;25:473-481.
24. Frankenberger R, Petschelt A, Kramer N. Leucite-reinforced glass ceramic inlays and onlays after six years: clinical behavior. Oper Dent 2000;25:459-465.
25. Suzuki S, Suzuki SA, Kramer C. Enamel wear against resin composite and ceramic C&B materials [abstract]. J Dent Res. 1997;76. Abstract 2454.
26. Van Meerbeek B, Inokoshi S, Willems G, et al. Marginal adaption of four tooth-coloured inlay systems in vivo. J Dent. 1992;20(1):18-26.
27. Van Dijken JW, Horstedt P. Marginal breakdown of 5-year-old direct composite inlays. J Dent. 1996;24(6):389-394.
Dr. Adams is an assistant professor at Medical College of Ohio, Division of Dentistry, Department of Otolaryngology, in Toledo, Ohio. He has lectured both nationally and internationally for many dental organizations and dental laboratories. In addition to Dr. Adams’ years in private practice, he has had the opportunity to serve as the doctor/technician liaison for DH Baker Dental Laboratory in Traverse City, Mich, for nearly 8 years. This unique combination of experiences has enabled Dr. Adams to bring clinically relevant discussions and practical solutions to the challenges facing the entire dental and laboratory team. Dr. Adams recently presented one of his seminars, “Indirect Composites: Dentistry’s Best Kept Secret!,” at the 2003, AGD Annual Meeting in Nashville, Tenn. He has also written or contributed to articles on insurance and clinical topics related to indirect composites for Dental Insurance Today, published by Atlanta Dental Consultants. Dr. Adams is listed in Dentistry Today’s 6th Annual Leaders in Continuing Education. He may be contacted for comments or seminar information at 800-946-8880 or damona@dhbaker.com.










