Control of the root surface environment has been an essential component of periodontal therapy for at least 1,000 years, when a Middle Eastern healer named El Zahwari (Albucassis) wrote in his treatise that “ye shall remove the encrustations on the teeth lest they be lost.”1 We have come a long way since then, but the basic requirements for periodontal health have not changed. Mechanical and chemical control of the root surface in order to achieve an environment compatible with the health of the supporting tissues remains the essence of periodontal management.2,3 However, with our current level of knowledge and understanding, we now have to consider the “big picture.”
 |
|
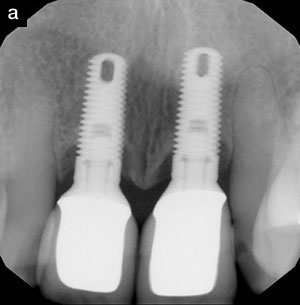
Figure 1. Chronic refractory periodontitis. |
SYSTEMIC MULTISYSTEM INVOLVEMENT
With its entire attendant ramifications related to its onset and ongoing inflammatory response, periodontal disease is associated with many issues of considerable concern. In addition to soft-tissue deformities, attachment loss and destruction of the osseous supporting structures of the teeth has historically been of concern (Figure 1).
BACTERIAL CONTROL
The rationale for bacterial control is supported by very solid evidence in the literature that has gradually allowed us to better understand the mechanisms involved in the pathogenesis of periodontal diseases. Anti-infective therapy can be divided into 3 components: biofilm control, adjunctive antimicrobial therapy, and, in many cases, surgical and restorative procedures to redefine soft and hard tissues for more efficient maintenance.
 |
|
Figure 2. PerioPath report showing high pathogen levels. |
 |
| Figure 3. PerioPath report after scaling and root planing and targeted antibiotic therapy. |
QUANTITATIVE DNA ANALYSIS
Knowing that the periodontal diseases are infections, it is appropriate to consider the medical model, whereby specific knowledge of the causative organisms can be used to plan a more guided approach to therapy. With the advent of quantitative DNA analysis of the pocket flora using polymerase chain reaction technology, we now have a simple way to determine not only the pathogens present in the pockets but their levels above threshold, and the ratios of organisms to each other. Using this information we can select the antibiotics or combination of antibiotics most suitable for the specific situation, based on well-documented published studies.21-26 A major step forward for the clinical implementation of this concept is the recent introduction of a salivary-DNA test for periodontal pathogens. This noninvasive test uses an oral rinse which is sent to the laboratory for analysis. The results (Figure 2) include a detailed analysis of the pathogens present in bar graph format, divided into the high-, medium-, and low-risk groups. Based on the patients medical history and their periodontal charting the reports include treatment considerations for more directed adjunctive therapy. Post-treatment testing approximately 6 weeks after completion of therapy shows the microbiological results (Figure 3).
USE OF SALIVA FOR DIAGNOSIS
 |
|
Figure 4. PerioPath report using sulcular fluid collection. |
 |
|
Figure 5. PerioPath report using saliva collection. |
The use of oral fluids, especially saliva for diagnosis, is an emerging tool, made possible by the increasingly sophisticated, sensitive, and accurate use of DNA analysis using polymerase chain reaction (PCR) technology.27,28 Analysis of oral fluid or saliva is currently used for the diagnosis of infectious and malignant diseases, hereditary disorders, autoimmune and endocrine disorders as well. It contains plasma electrolytes and many other metabolites, enzymes, and both bacterial and human DNA.
LONG-STANDING THERAPEUTIC GOAL?
The importance of the microbial activation of the destructive inflammatory response is borne out by the known association of combinations of pathogens associated with measures of periodontal inflammation, as shown in Figures 2 to 5. This highlights the so-called high- (red complex), medium- (orange complex) and low-risk groups39 (Figure 5). These associations are well documented40 and relate, as well, to many systemic diseases, most notably coronary heart disease.41 The link between all of these oral and systemic manifestations is inflammation.
This brings us back to the observations made so many centuries ago. Control the root surface and pocket environment and the tissues heal. This has always been, and continues to be our therapeutic goal in managing periodontal disease, and, apparently, reducing the risk of systemic sequellae. The inception of accurate, reproducible, salivary diagnostics for the clinician puts us much closer to the goal of predicting therapeutic outcomes, and disease activity.42
References
- Hamareh S K. In: Hayes JR, ed. The Genius of Arab Civilization: Source of Renaissance. 2nd ed. London, England: Eurabia Publishing; 1983:198-200.
- Zionts D: Surgical vs non-surgical techniques in periodontal therapy: A literature review. Penn Dent J. 1985;86:21-24.
- Beirne P, Forgie A, Worthington HV, et al. Routine scale and polish for periodontal health in adults. Cochrane Database Syst Rev. 2005;CD004625.
- Offenbacher S, Katz V, Fertik G, et al. Periodontal infection as a possible risk factor for preterm low birth weight. J Periodontol.1996;67(suppl 10):1103-1113.
- Kuula H, Salo T, Pirilä E, et al. Local and systemic responses in matrix metalloproteinase 8-deficient mice during Porphyromonas gingivalis-induced periodontitis. Infect Immun. 2009;77:850-859.
- Listgarten MA. Pathogenesis of periodontitis. J Clin Periodontol. 1986;13:418-430.
-
Kinane DF, Shiba H, Hart TC, et al. The genetic basis of periodontitis. Periodontol 2000. 2005;39:91-117.
- Hujoel PP, Löe H, Anerud A, et al. The informativeness of attachment loss on tooth mortality. J Periodontol. 1999;70:44-48.
- Reddy MS, Geurs NC, Jeffcoat RL, et al. Periodontal disease progression. J Periodontol. 2000;71:1583-1590.
- Hallmon WW, Rees TD. Local anti-infective therapy: mechanical and physical approaches. A systematic review. Ann Periodontol. 2003;8:99-114.
- Yukna RA, Vastardis S, Mayer ET. Calculus removal with diamond-coated ultrasonic inserts in vitro. J Periodontol. 2007;78:122-126.
- Chapter 8. Non-Surgical Therapy. Periodontal Literature Reviews. 1996;1:136-144.
- Bader H. Scaling and rootplaning: evolution or revolution? Dent Today. 1991;10:56-57.
- Rosen PS, American Academy of Periodontology—Research, Science, and Therapy Committee. Treatment of plaque-induced gingivitis, chronic periodontitis, and clinical conditions. Pediatr Dent. 2008-2009;30(suppl 7):253-262.
- Lang NP, Tan WC, Krähenmann MA, et al. A systematic review of the effects of full-mouth debridement with and without antiseptics in patients with chronic periodontitis. J Clin Periodontol. 2008;35(suppl 8):8-21.
- Petersilka GJ, Ehmke B, Flemmig TF. Antimicrobial effects of mechnical debridement. Periodontol 2000. 2002;28:56-71.
- Offenbacher S, Barros SP, Beck JD. Rethinking periodontal inflammation. J Periodontol. 2008;79(suppl 8):1577-1584.
- Offenbacher S, Barros SP, Singer RE, et al. Periodontal disease at the biofilm-gingival interface. J Periodontol. 2007;78:1911-1925.
- Socransky SS, Haffajee AD, Cugini MA, et al. Microbial complexes in subgingival plaque. J Clin Periodontol. 1998;25:134-144.
- Adriaens PA, De Boever JA, Loesche WJ. Bacterial invasion in root cementum and radicular dentin of periodontally diseased teeth in humans. A reservoir of periodontopathic bacteria. J Periodontol. 1988;59:222-230.
- van Winkelhoff AJ, Winkel EG. Microbiological diagnostics in periodontics: biological significance and clinical validity. Periodontol 2000. 2005;39:40-52.
- Haffajee AD, Teles RP, Socransky SS. The effect of periodontal therapy on the composition of the subgingival microbiota. Periodontol 2000. 2006;42:219-258.
- Beikler T, Prior K, Ehmke B, et al. Specific antibiotics in the treatment of periodontitis—a proposed strategy. J Periodontol. 2004;75:169-175.
- Herrera D, Alonso B, León R, et al. Antimicrobial therapy in periodontitis: the use of systemic antimicrobials against the subgingival biofilm. J Clin Periodontol. 2008;35(suppl 8):45-66.
- Cionca N, Giannopoulou C, Ugolotti G, et al. Amoxicillin and metronidazole as an adjunct to full-mouth scaling and root planing of chronic periodontitis. J Periodontol. 2009;80:364-371.
- Ramseier CA, Kinney JS, Herr AE, et al. Identification of pathogen and host-response markers correlated with periodontal disease. J Periodontol. 2009;80:436-446.
- Saiki RK, Gelfand DH, Stoffel S, et al. Primer-directed enzymatic amplification of DNA with a thermostable DNA polymerase. Science. 1988;239:487-491.
- Bartlett JM, Stirling D. A short history of the polymerase chain reaction. Methods Mol Biol. 2003;226:3-6.
- Boutaga K, Savelkoul PH, Winkel EG, et al. Comparison of subgingival bacterial sampling with oral lavage for detection and quantification of periodontal pathogens by real-time polymerase chain reaction. J Periodontol. 2007;78:79-86.
- Paju S, Pussinen PJ, Suominen-Taipale L, et al. Detection of multiple pathogenic species in saliva is associated with periodontal infection in adults. J Clin Microbiol. 2009;47:235-238.
- Cortelli SC, Feres M, Rodrigues AA, et al. Detection of Actinobacillus actinomycetemcomitans in unstimulated saliva of patients with chronic periodontitis. J Periodontol. 2005;76:204-209.
- Sawamoto Y, Sugano N, Tanaka H, et al. Detection of periodontopathic bacteria and an oxidative stress marker in saliva from periodontitis patients. Oral Microbiol Immunol. 2005;20:216-220.
- Kulekci G, Leblebicioglu B, Keskin F, et al. Salivary detection of periodontopathic bacteria in periodontally healthy children. Anaerobe. 2008;14:49-54.
- Feng XH, Zhang L, Meng HX, et al. Detection of 3 anaerobic microorganisms in saliva and subgingival plaque of patients with periodontitis [in Chinese]. Beijing Da Xue Xue Bao. 2009;41:44-48.
- Könönen E, Paju S, Pussinen PJ, et al. Population-based study of salivary carriage of periodontal pathogens in adults. J Clin Microbiol. 2007;45:2446-2451.
- Greenstein G, Hart TC. A critical assessment of interleukin-1 (IL-1) genotyping when used in a genetic susceptibility test for severe chronic periodontitis. J Periodontol. 2002;73:231-247.
- Kornman KS, di Giovine FS. Genetic variations in cytokine expression: a risk factor for severity of adult periodontitis. Ann Periodontol. 1998;3:327-338.
- Nikolopoulos GK, Dimou NL, Hamodrakas SJ, et al. Cytokine gene polymorphisms in periodontal disease: a meta-analysis of 53 studies including 4178 cases and 4590 controls. J Clin Periodontol. 2008;35:754-767.
- Teles RP, Haffajee AD, Socransky SS. Microbiological goals of periodontal therapy. Periodontol 2000. 2006;42:180-218.
- Socransky SS, Haffajee AD, Smith C, et al. Microbiological parameters associated with IL-1 gene polymorphisms in periodontitis patients. J Clin Periodontol. 2000;27:810-818.
- Geismar K, Enevold C, Sørensen LK, et al. Involvement of interleukin-1 genotypes in the association of coronary heart disease with periodontitis. J Periodontol. 2008;79:2322-2330.
- Giannobile WV, Beikler T, Kinney JS, et al. Saliva as a diagnostic tool for periodontal disease: current state and future directions. Periodontol 2000. 2009;50:52-64.
Dr. Bader practices periodontics and implant dentistry in Cape Cod and Plymouth, Mass. He is a graduate of NYU College of Dentistry, and in 1966 completed a residency in periodontology at the Harvard School of Dental Medicine, where he currently serves as lecturer in postgraduate periodontology. He is a Fellow of the American College of Dentists, International College of Dentists, and a Diplomate of the American Academy of Osseointegration. He has been published in the Journal of Dental Research, Journal of Periodontology, Journal of Clinical Periodontology, and the American Journal of Dentistry. He can be reached via e-mail at redabsr@aol.com.
Disclosure: Dr. Bader is on the Scientific Advisory Board of OralDNA Labs, Inc (A Quest Diagnostics Company).