INTRODUCTION
For success with indirect mixed-media cosmetic case preplanning, each case is extremely important to achieve the best results. Using diagnostic records, such as mounted diagnostic cast models, photography, radiography, and diagnostic wax-ups, is important to plan out the case prior to teeth preparation. These cases are much more complex as you are dealing with different types of restorative materials, techniques, and aesthetic protocols. For example, there is a difference in tooth preparations for veneer preps vs crown preps. This difference can affect the internal shade coloration of the tooth preps, the depth of each preparation, and the optical thickness of aesthetic restorative material used for each tooth.
CASE REPORT
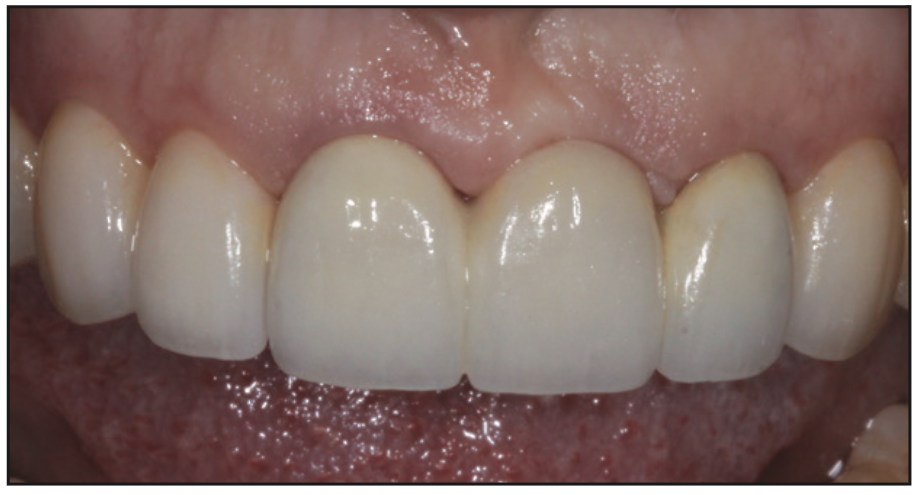
The patient was a 36-year-old female in generally good health. More than 15 years ago, her anterior teeth were corrected with veneers and a resin-based fixed bridge. At presentation, the patient did not like her smile, as it had become aged, worn, and visibly unaesthetic over time (Figures 1 and 2).
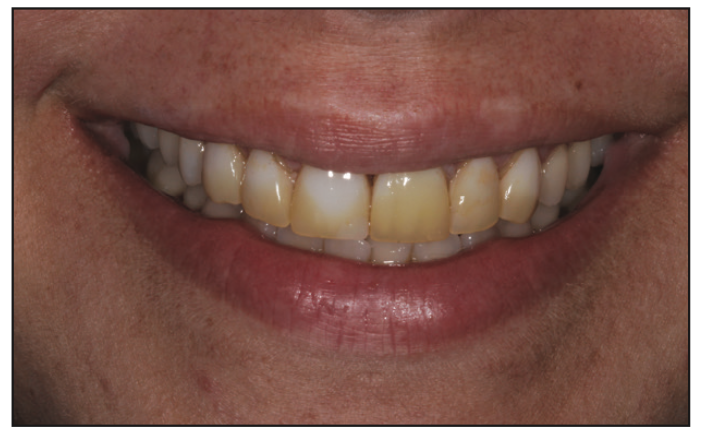
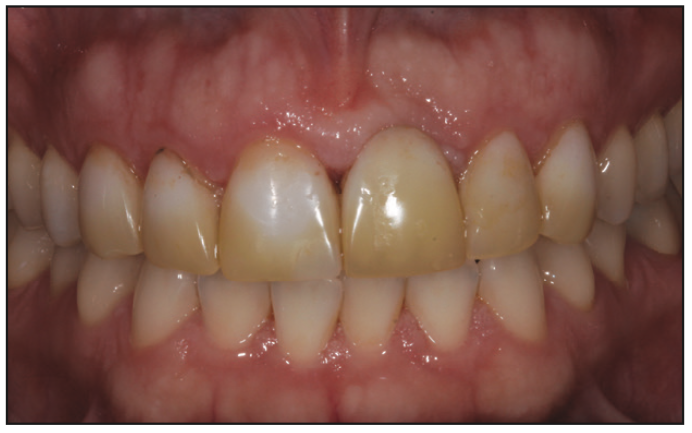
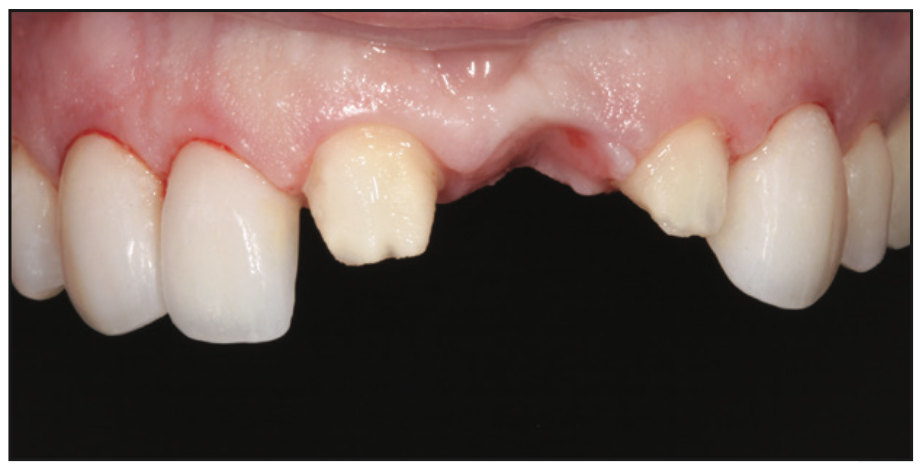
First, a full comprehensive exam and diagnostic work-up were completed. A periodontal exam, aesthetic dental analysis, facial analysis, and full-mouth radiographic series were important to understand the details needed prior to restoring the case. In addition, a comprehensive occlusal analysis was done to ensure a predictable, functional, aesthetic result.1 Although the patient was missing a left central incisor, she was not interested in having a dental implant. So it was determined that the missing tooth would be restored with an anterior fixed bridge. Also, porcelain veneers would replace the existing, very stained veneers (Figure 3). Traditionally, this case might have been approached with full crowns instead of porcelain veneers due to the difficulty of matching veneers to fully prepped teeth for the bridge. However, preserving natural dentition with veneer preparations was more desirable for minimally invasive purposes despite the increase in difficulty.
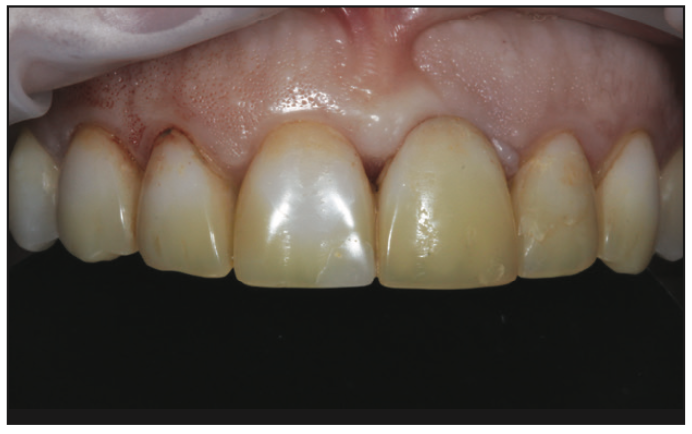
It is important to note that the clinician must understand the diagnostic criteria, treatment planning process, and biological parameters involved in attaining predictable outcomes when treating the aesthetic zone.2 After mounting diagnostic models on a semi-adjustable articulator (Denar [Whip Mix]), a diagnostic wax-up was completed to reflect the new contours and proportions in the new aesthetic arrangement. To maximize facial aesthetic beauty, it is important to customize the smile design to create the best results.3-5
Mixed-Media Treatment With Porcelain Veneer Preparation and an Aesthetic Anterior Bridge
Using a diamond prep depth guide bur (Porcelain Veneer Kit [Komet USA]), the old porcelain restorations along Nos. 6, 7, and 11 and the existing anterior bridge from Nos. 8 to 10 were removed. For the porcelain veneer preparations, light chamfer margins were placed slightly under the free gingival margin. A clear matrix was used to verify the clearance needed for 0.5-mm porcelain veneers.6 The teeth preparations were finished and marginated with tapered chamfer diamond burs (850.FG.014 [Komet USA]). Whenever possible, it is good to leave enamel intact for optimal porcelain-to-tooth bonding, as this helps increase the long-term success of bonded porcelain veneers.
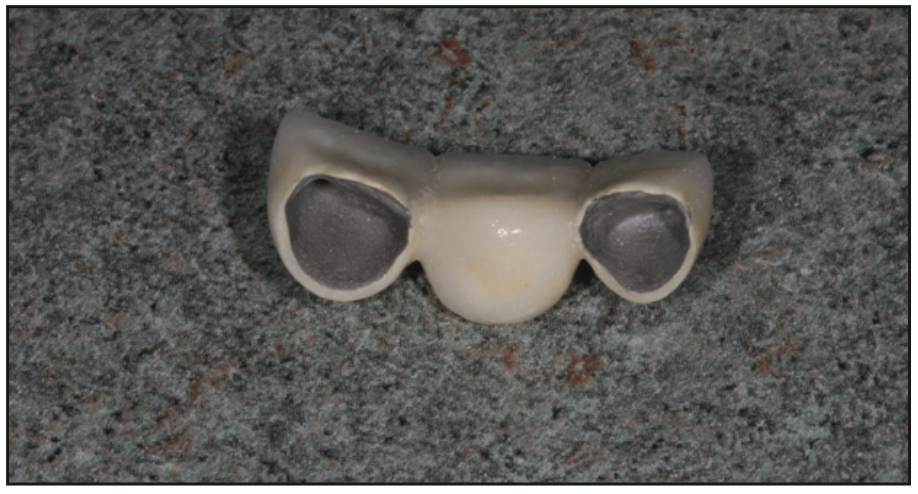
For the anterior fixed bridge, slightly more axial reduction (approximately 1.5 mm) was needed for the new porcelain-to-gold (PFG) fixed bridge. In comparison to porcelain veneer margins, the heavy chamfer abutment margins were placed 1.0 mm subgingival to create a natural-appearing emergence profile7 (Figure 4). To reduce darkening along the facial margin of the abutments, a porcelain shoulder was incorporated along the margin of the final PFG bridge. This would make the final result appear natural.
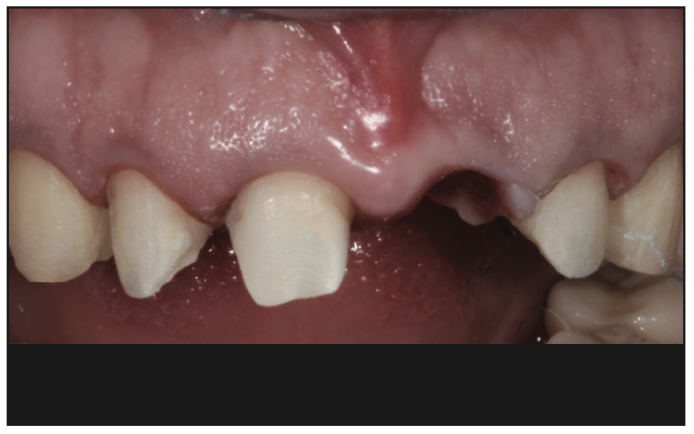
Along the pontic site of the bridge, the gingival tissue needed to be aesthetically refined to create a natural-appearing gingival emergence profile. State-of-the-art methods for minimally invasive soft-tissue surgical correction were done along the pontic site with the use of laser-assisted dentistry. With a thorough understanding of the dento-gingival complex, predictable correction of gingival tissue can be addressed.8,9 A high degree of precision with an ovate pontic can be attained with a dental laser.10,11 Using an Er,Cr:YSSG laser (Waterlase iPlus [BIOLASE]), a soft-tissue surgical procedure was performed to create this new emergence profile12,13 (Figure 5). Using an erbium laser results in minimal to no bleeding, less wound contraction, and less pain compared to a traditional approach.14
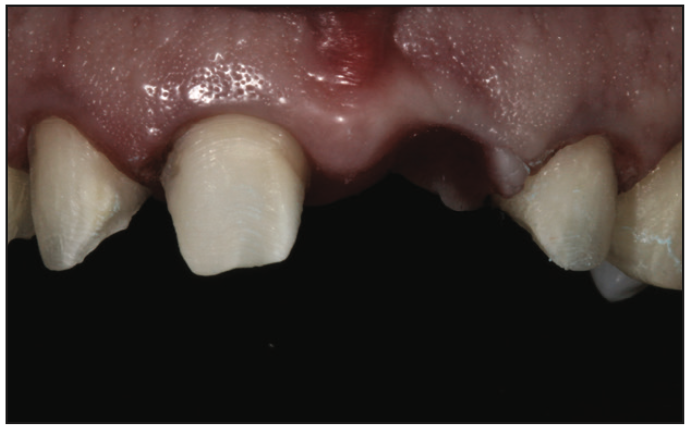
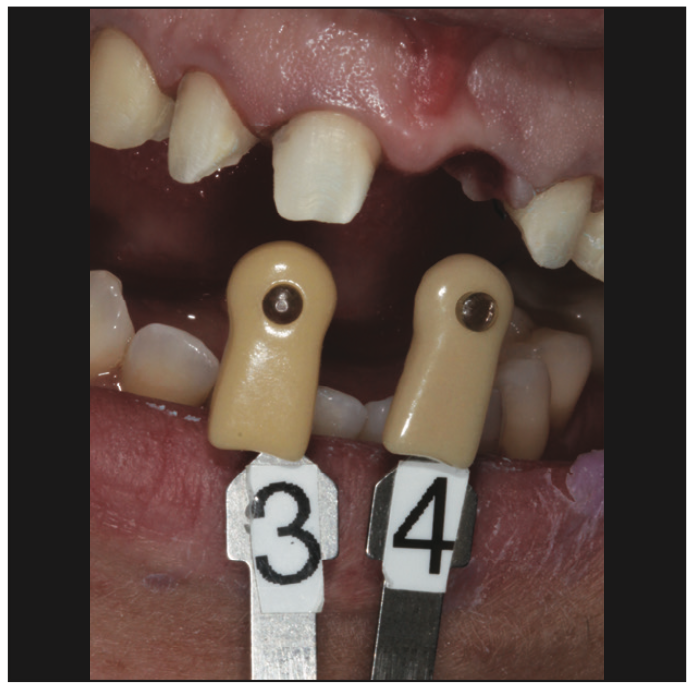
Aesthetic temporary prototype veneers (TurboTemp 3 [Zest Dental Solutions]) and a bridge were hand sculpted. The temporary prototypes were designed to support the healing gingival tissue, meet the aesthetic expectations of the patient, and dial in the proper occlusal guidance (Figure 7).
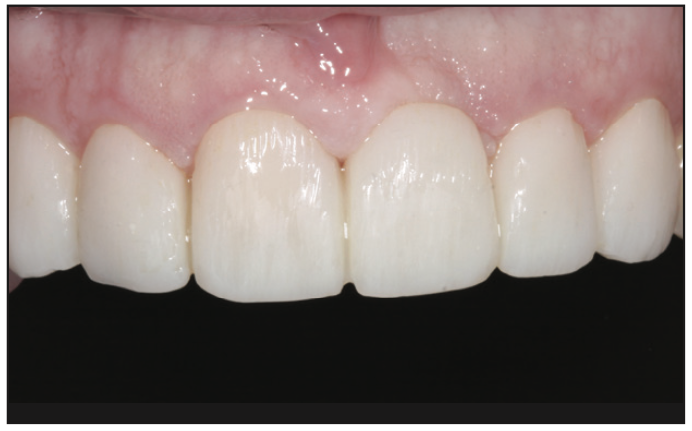
Meeting the patient’s aesthetic expectations is particularly important as the success of the case always needs to meet the aesthetic vision of the patient. In comparison to using a computer software for aesthetic development of the case, artistic time was spent with the patient blending the correct contours, proportions, and color shading to maximize her facial balance and facial aesthetics.16,17 Artistic hand sculpting was used to accentuate the contours of her temporary prototypes to match her personality, lip curvature, and unique facial features (Figure 8). This valuable time spent with the patient leads to no guesswork in the aesthetic aspects of the final restorations.18,19
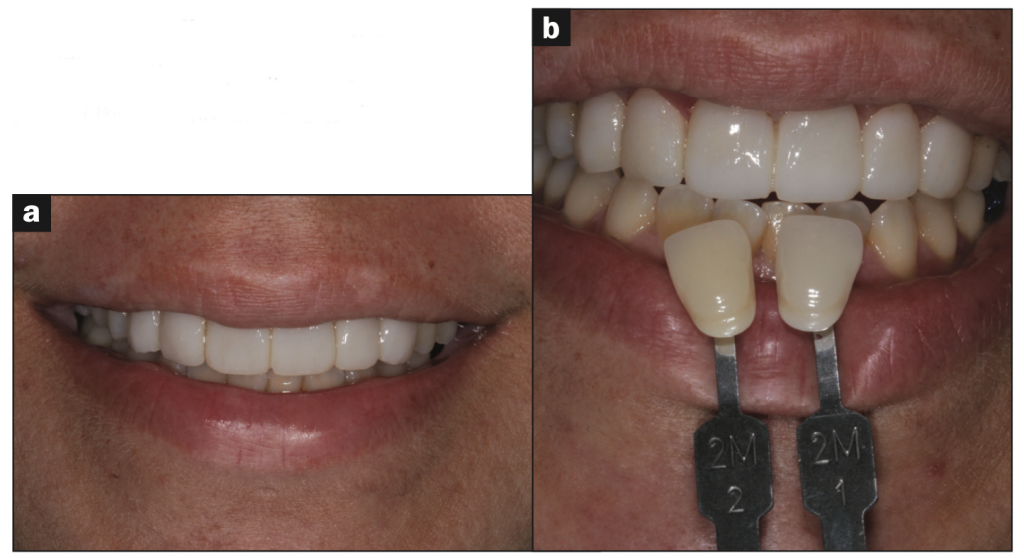
Along with the lab prescription, a customized color map and texture map was sent, so the ceramic artist was able to artistically create the final porcelain veneers and aesthetic anterior PFG bridge using the temporary prototypes as a guide (Figures 9 and 10). After receiving the aesthetic restorations from the ceramic lab, they were evaluated to ensure the new porcelain restorations would meet the patient’s aesthetic expectations.20,21
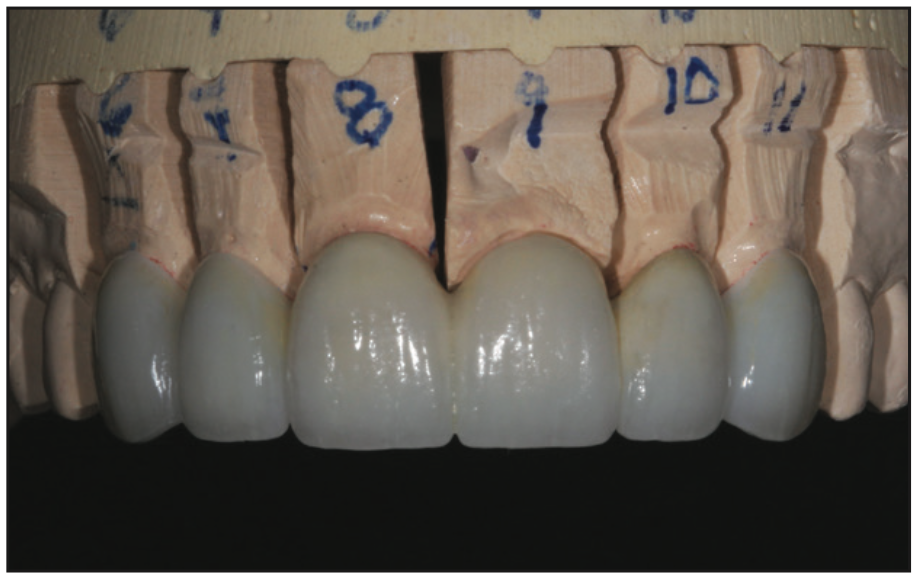
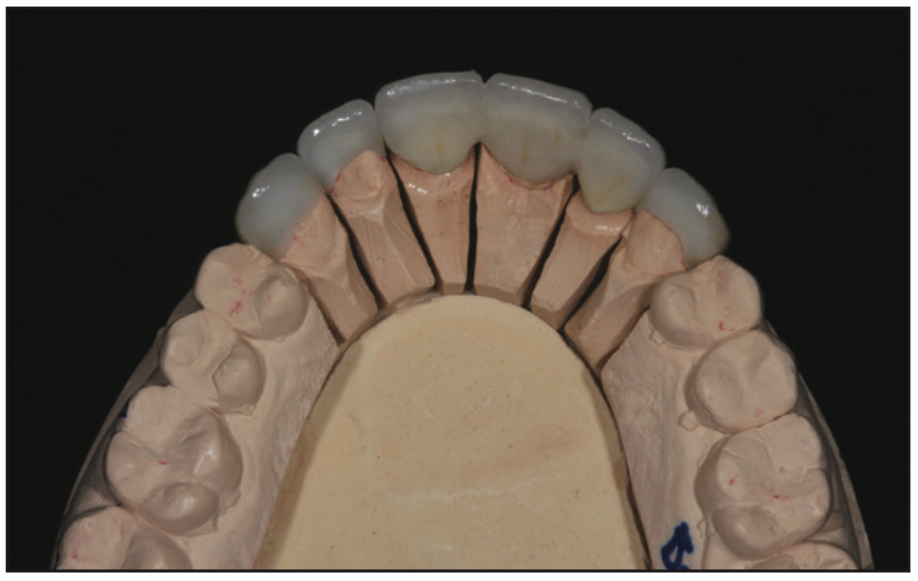
Try-in and Final Bonding of the Final Restorations
At the seat appointment, the temporary prototypes were removed and the surfaces were cleaned with a plain flour of pumice slurry using an ICB rotary brush (ICB Brush [Ultradent Products]). Optimal gingival tissue healing was seen as a result of high-quality marginated temporaries and proper hygiene maintenance during this provisional period (Figures 11 and 12).
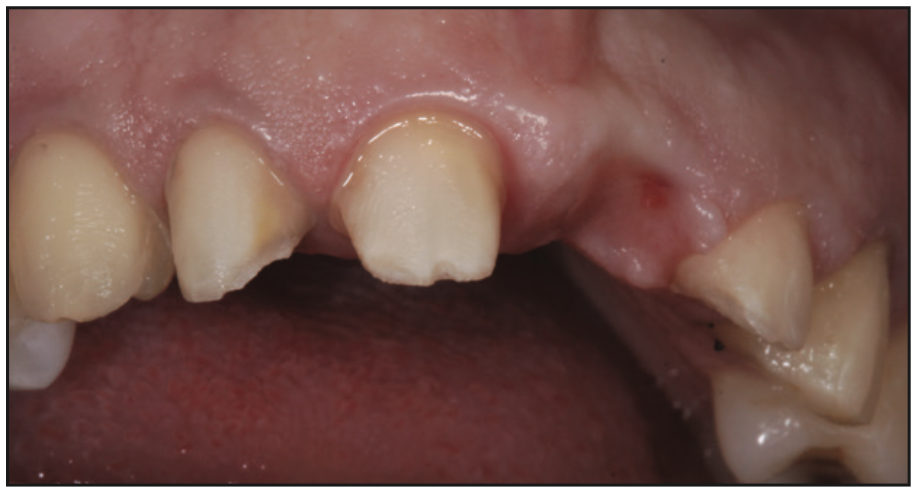
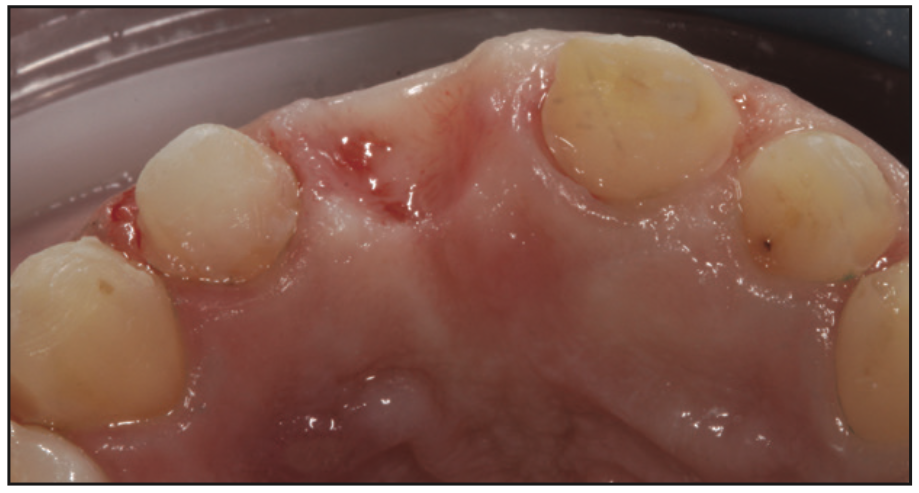
The new porcelain veneers and bridge were tried in to evaluate overall fit, aesthetic contours, interproximal contacts, and gingival embrasures. Additionally, an intimate fit of the pontic of the bridge to the ovate pontic site was verified (Figure 13). Next, the external coloration of the veneers to the PFG bridge was particularly scrutinized to be sure the final aesthetic appearance would have uniform external color blending. Porcelain veneer try-in pastes (Choice 2 Try-In Pastes [BISCO]) were used to assess this uniformity.
After acceptance of the try-in phase by the patient, the porcelain veneers were cleaned and prepared with a ceramic etch and then silanated with a silane coupling agent (BIS-SILANE [BISCO]). After air-drying, a thin layer of porcelain-bonding resin (Porcelain Bonding Resin [BISCO]) was placed along the intaglio surface of the veneers to further optimize adhesive strength.22
In preparing the PFG bridge restoration, the intaglio surface was micro-etched (MicroEtcher II [Zest Dental Solutions]), then 2 coats of primer (Z-Prime Plus [BISCO]) were placed for 5 minutes and dried thoroughly. Using a primer helps facilitate the chemical bonding of the restoration to the luting resin cement23 (Figure 14).
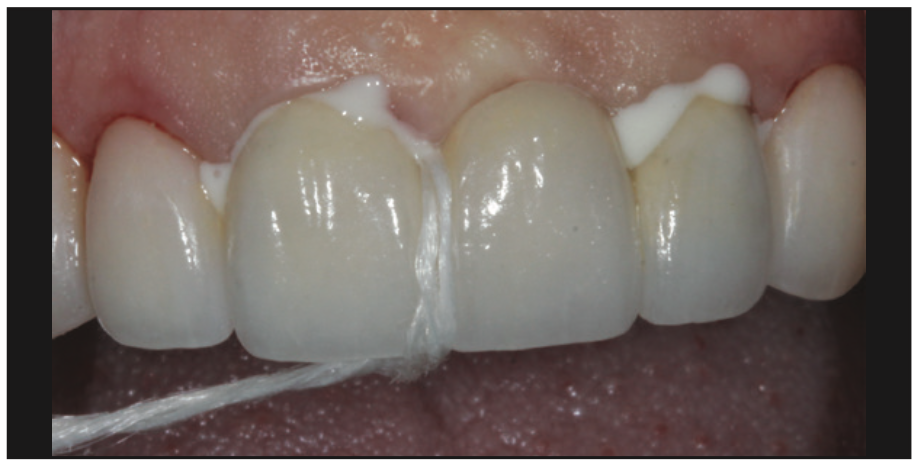
To reduce gingival crevicular fluid contamination, a thin gingival cord (4-0 suture cord [Patterson Dental]) was gently tissue-packed for all teeth. In the final bonding of the veneers, plain flour of pumice was used for final cleansing of the prepped surfaces. Next, chlorhexidine gluconate (Cavity Cleanser [BISCO]) was used as an initial disinfectant. A 32% phosphoric acid (Select HV Etch w/BAC [BISCO]) was placed on the enamel using a selective-etch technique for 20 to 30 seconds, then rinsed off thoroughly. A desensitizer (MicroPrime G [Zest Dental Solutions]) was swabbed for 20 seconds prior to placing the dental adhesive (ALL-BOND UNIVERSAL [BISCO]). Several layers of this adhesive were thinly placed, blown thin, and light-cured along all surfaces (Figure 15).

For all 3 porcelain veneers (Nos. 6, 7, and 11), a light-cured luting resin cement (Choice 2 translucent luting resin cement [BISCO]) was placed, positioned, and tack-cured for 2 seconds along the incisal edge. After gentle flossing through all the proximal contacts, most of the excess luting resin cement was removed. Then all veneers were light-cured simultaneously along all surfaces. After final light-curing, the margins of the veneers were cleaned using a curved scalpel blade (#12 Bard-Parker [Aspen Surgical]). Then the margins were finished with finishing burs (H50A.FG.010 and 8379.FG.012) (Figure 16). Finally, a Ceramic Polishing Kit (4533C.RA [Komet USA]) was used to create a final beautiful luster on the case.
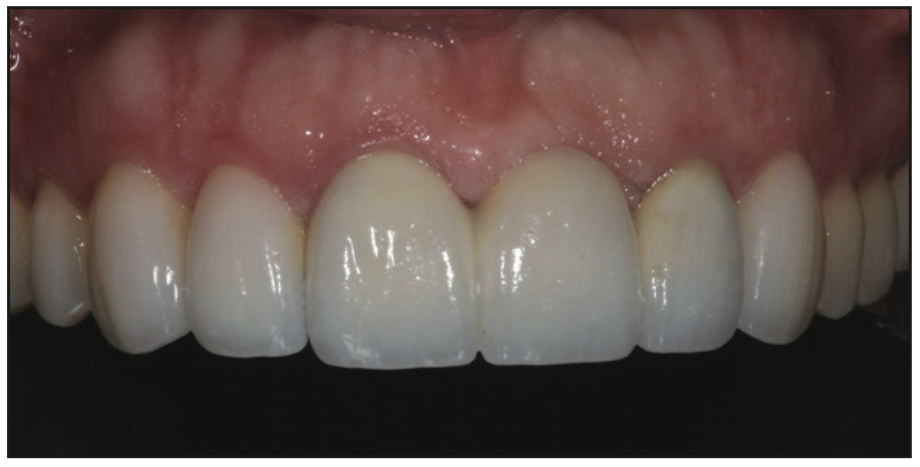
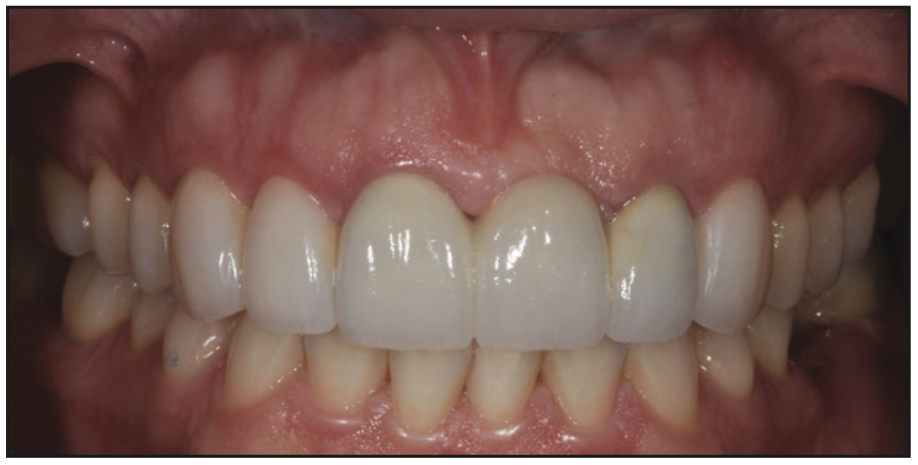
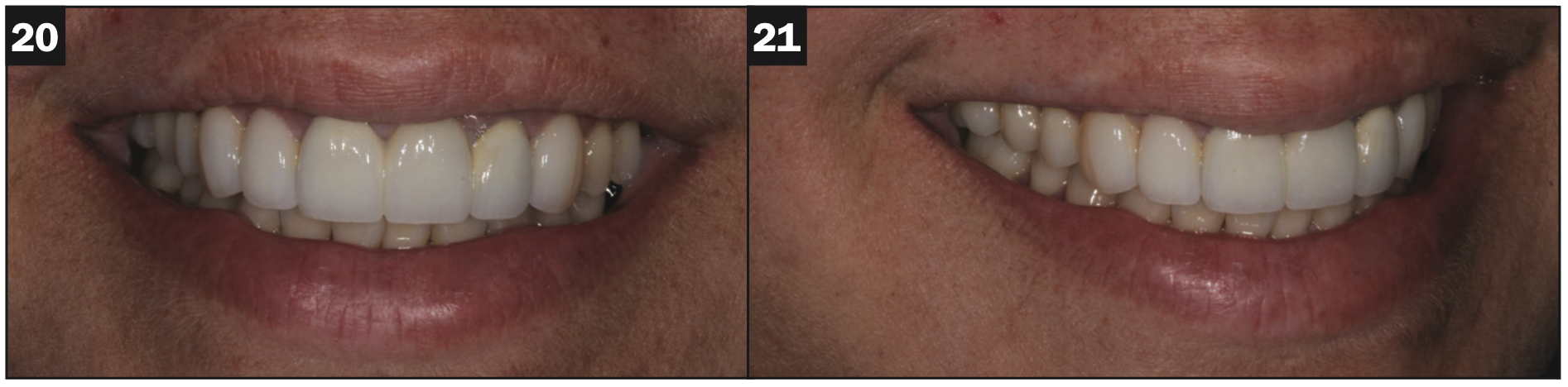
In the final placement of the PFG bridge, a self-adhesive luting cement (TheraCem [BISCO]) was used. With positive pressure, the bridge was placed on the abutment teeth, and excess cement was allowed to extrude (Figure 17). The margins were tack cured for a few seconds. This allowed the excess cement to semi-set so it could be easily peeled off. Because of the unique properties of TheraCem, simple removal of excess cement was performed along the interproximal surfaces and under the pontic site with floss. Additional flossing and margin cleanup were done to complete the procedure (Figure 18). The final result of indirect mixed-media cosmetic cases can be very successful aesthetically with long-term success (Figures 19 to 21).
CONCLUSION
In practicing cosmetic dentistry, there are many different procedures performed. The clinician needs to understand the different details to perform indirect, mixed-media cosmetic dental treatment well. Although these cases are much more complex, by incorporating this method into cosmetic dental treatment, the clinician can reduce unnecessary tooth preparation, become minimally invasive, and achieve long-term results.
REFERENCES
1. Chiche G, Kokich V, Caudill R. Diagnosis and treatment planning of esthetic problems. In: Pinault A, Chiche G, eds. Esthetics in fixed prosthodontics. Quintessence; 1994;33-52.
2. Garguilo AW, Wentz FM, Orban B. Dimensions of the Dentogingival Junction in Humans. J Periodontology. 1961;32:261–7. doi:10.1902/jop.1961.32.3.261
3. Okuda W. Smile design 2.0: evolving from our past to be successful in treating the modern cosmetic patient. Gen Dent. 2016;64(1):10–3.
4. Morley J, Eubank J. Macroesthetic elements of smile design. J Am Dent Assoc. 2001;132(1):39-45. doi:10.14219/jada.archive.2001.0023
5. Spear F. Facially generated treatment planning: a restorative viewpoint. Paper presented at: 11th Annual American Academy of Cosmetic Dentistry Scientific Session; May 1995; Orlando.
6. Nixon RL. Chairside manual for porcelain bonding. BV Videographics; 1987.
7. Rufenacht C. Fundamentals of esthetics. Quintessence Publishing; 1990.
8. Kois JC. Altering gingival levels: the restorative connection part 1: biologic variables. J Esthe Dent. 1994. 6(1):3-9. doi:10.1111/j.1708-8240.1994.tb00825.x
9. Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11:29-38. doi:10.1111/j.1600-0757.1996.tb00180.x
10. Venkatasubramanyam A, Sigtia S, Sheth E, et al. Laser-assisted natural gingival profile creation of an ovate pontic site. J Dent Lasers. 2017;11:29-32. doi:10.4103/jdl.jdl_5_17
11. Mhatre S, Ram SM, Shah N. Modified ovate pontic design for immediate anterior tooth replacement. J Contemp Dent. 2012;2:64-68. doi:10.5005/jp-journals-10031-1013
12. Hari Iyer V, Manali SR. Interdisciplinary approach using diode laser for esthetic management of missing anterior teeth. Int J Laser Dent. 2013;3:24–8. doi:10.5005/jp-journals-10022-1032
13. Ernesto L. Lasers assisted crown lengthening procedures in the esthetic zone: contemporary guidelines and techniques. Contemp Esthetics. 2007;42–9.
14. Dyer BL. Minimally invasive osseous crown lengthening procedure using an erbium laser: clinical case and procedure report. J Cosmetic Dent. 2008;23(4):84-91.
15. Sieber C. Voyage: visions in color and form. Quintessence Publishing; 1994.
16. Ubassy G. Shape and color: the key to successful ceramic restorations. Quintessence Publishing; 1993.
17. Okuda W. An innovative approach to complex cosmetic dentistry. Dent Today. 2018:70–3.
18. Muia PJ. Esthetic restorations: improved dentist-laboratory communication. Quintessence Publishing; 1993.
19. Crispin BJ. Contemporary esthetic dentistry: practice fundamentals. Quintessence Publishing; 1994.
20. Snyder T. Modern aesthetic mixed restorative case. Dent Today. 2014;335):131-135.
21. Ochoa P. Solving aesthetic challenges with mixed restorations. Dent Today. 2021;40(2):42–45.
22. Suh BI. Principles of adhesive dentistry: a theoretical and clinical guide for dentists. Aegis Publication; 2013.
23. Chen L, Suh BI, Brown D, et al. Bonding of primed zirconia ceramics: evidence of chemical bonding and improved bond strengths. Am J Dent. 2012;25(2):103–8.
ABOUT THE AUTHOR
Dr. Okuda is a past national president (2002 to 2003) and an accredited member of the American Academy of Cosmetic Dentistry (AACD). He is also a fellow of the International College of Dentists and the International Congress of Oral Implantologists. In 2014, Dr. Okuda achieved his Accredited Fellowship with the AACD. He is currently the aesthetic dentistry expert to the National Dental Expert Advisory Board of the AGD. He has also been the aesthetic columnist of the AGD’s General Dentistry publication for the last 9 years. Over the last 28 years, Dr. Okuda has been a keynote and featured speaker on cosmetic and restorative dentistry at numerous conferences and universities. For the last 16 years, Dr. Okuda was one of Dentistry Today’s Leaders in Continuing Education. He is the co-founder of the Give Back a Smile National Charitable Foundation. He may be reached at okudacosmeticdentistry.com, on Facebook @drwynnokuda, or on Instagram @drokuda.
Disclosure: Dr. Okuda reports no disclosures.


