|
INTRODUCTION
The options for treatment of patients experiencing pain associated with temporomandibular dysfunction (TMD) have dramatically increased over the past decade. Regardless of the treatment philosophy utilized, most begin with a removable mandibular positioning device or orthotic to begin therapy. The rationale behind the use of a removable orthotic is based in the concept of alleviating the patient’s pain, stabilizing painful muscles and joints, and to begin establishing a physiological arc of closure, vertical dimension, and occlusal scheme prior to moving on to more definitive, possibly invasive, treatment.
The role of accurate full-arch impressions and a proper bite registration (at the desired treatment position) is tantamount. Inaccurate preliminary casts created from impressions that exhibit voids, pulls, or drags, or from distorted impressions made from materials that exhibit poor tear strength, elastic deformation, and dimensional instability, must be rejected. So, every inaccuracy allowed to slip by with the preliminary models and bite registration can parlay into errors that will hinder reaching any definitive treatment goals.
Bite Registration Materials
A bite registration material must be able to accurately reproduce the exact intermaxillary relationship. Inaccuracies during bite registration can lead to incorrect contouring of the occlusal surfaces by the dental laboratory team, resulting in many time-consuming adjustments of the restoration by the dentist.
A bite registration material should be able to be easily dispensed onto the occlusal surfaces of the teeth, having enough flow to encompass the occlusal one third of each tooth; however, all bite registration materials must be fluid enough to not deflect or impede the path of closure into the desired occlusal position. Ideal bite registration materials should also have sufficient flexibility to be removed from the mouth without permanent elastic deformation, yet polymerize to a final hardness that permits easy trimming of any excess material. Materials used for bite registrations taken in the patient’s existing centric occlusion (maximum intercuspation) typically require the least amount of working time in that no mandibular manipulation, or other form of jaw positioning, is required prior to material polymerization. When alterations to the patient’s occlusal relationship are being made, the ideal working time is dependent on the time required to reach the precise mandibular position.
There are many bite registration materials available to clinicians today (ie, wax, cold-cure acrylics, bis-acrylics, and addition-curing silicones). The latest bite registration material is the addition-curing silicones (A-silicones). These materials are vinyl polysiloxane (VPS) impression materials that have been chemically altered to make them ideal for use as bite registration materials. All A-silicones are dispensed from a dual-barreled cartridge via a spiral tip, assuring proper mix ratios of catalyst and base. Depending on the brand, A-silicones vary in wetability, flexibility, brittleness (during removal from undercuts as well as during trimming), consistency and handling, and length of working time from mix to set. Some dental manufacturers offer a choice of working times within the same brand so that clinicians can avoid stocking different brands for the variety of clinical situations common to most dental offices.
Preliminary Impression Materials
Historically, there have been many commercially available materials that can be used for preliminary impressions for diagnostic casts and study models (ie, alginate [reversible hydrocolloid], polyether, and VPS).
Ideally, materials designed for taking preliminary impressions must be highly accurate, easy to dispense at precise catalyst/ base ratios, and be sufficiently elastomeric to be removed from the mouth without deformation. They should also have sufficient tear strength to endure being pulled from interproximal embrasures and beneath fixed-bridge pontics. Since is it quite common in TMD therapy for preoperative models to be sent directly to dental laboratories, they must be able to be disinfected and durable enough to be poured multiple times, remaining accurate and available for repouring during the course of treatment. Full-arch impressions need enough working time to fill a full-arch tray and be seated in the mouth, yet not require uncomfortably long set times while in the mouth. Lastly, since impression materials typically used for preliminary models are also used to make impressions for many other clinical procedures, the ideal impression material should be affordable.
Traditionally, many dentists were taught to use alginates for preliminary impressions. Many dentists simply find the “feel” of alginate to be ideal for full-arch preliminary impressions; however, despite these attractive advantages, the physical properties and working characteristics are extremely technique sensitive. Exact powder/water ratios are easily abused and erratic mixing can lead to errors in flow, air entrapment, dimensional stability, and tear strength in the mouth. Because alginate materials are water-based, they are highly subject to evaporation over time and must be poured immediately to be accurate. Further frustration can come from not removing the stone casts from the alginate while they are still hydrated, which may result in model fracture, and repours are not possible.
Some dentists choose to use modern polyether and VPS materials when making preliminary impressions. These materials require no hand mixing, are easily dispensed and are quite capable of creating highly accurate, elastomerically-stable impressions that can be disinfected and sent to the dental laboratory and poured multiple times. They are significantly more expensive to use than alginate, and depending on the physical properties and viscosity of the particular brand used, these may exhibit more flow than desired for the typical full-arch impressions used for preliminary models. Some have a displeasing taste and can take up to 4 minutes to set, which is time consuming and uncomfortable for patients.
Recently, some dental manufacturers have released impressions materials specifically designed to serve as what could be called an “alginate substitute.” The primary purpose of these materials is to render more accurate, elastomerically-stable, tear resistant impressions than traditional alginate, with many of the already mentioned advantages of polyether and VPS materials.
CASE REPORT
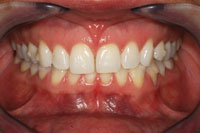
A 38-year-old woman presented with the chief complaint of moderate to severe myofacial pain and frequent migraine-type headaches, particularly in the left temporalis area. The patient was actively engaged in clear aligner orthodontic therapy and noted that though she had occasional headaches and joint pain before, her symptoms had become worse as orthodontic therapy progressed (Figure 1). A complete intraoral and head and neck exam was performed and a comprehensive TMD/myofacial pain questionnaire was completed.
 |
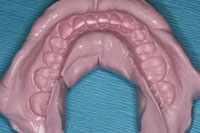 |
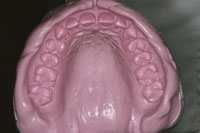
| Figures 5 and 6. Views of the maxillary and mandibular full-arch impressions. |
Preliminary Impressions
Accurate full-arch impressions suitable for occlusal assessment and ultimately for the fabrication of a neuromuscular orthotic can be difficult to capture. Because of the variables involved in mounting a neuromuscular case, several anatomical landmarks must be captured to the teeth themselves. The full hamular notch beyond the maxillary tuberosity region must be captured in the event that the hamular-incisive papilla plane is needed to orient the maxillary cast. The anatomical details of the palate must be represented in the impression if a cranial base transfer is necessary. Precise replication of the occlusal anatomy, the circumference of every tooth and the soft tissue surrounding the teeth is mandatory to fabricate a neuromuscular orthotic to assure proper fit and exact occlusal position of the oriented casts at the myocentric bite.
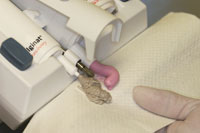
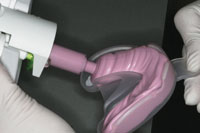
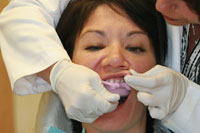
A medium viscosity, addition-curing, elastomeric VPS (alginate substitute) material (Silginat [Kettenbach LP]) was chosen because of its accuracy and dimensional stability, even after multiple pours. In addition, it exhibits an ideal consistency, flow, and ability to distend the soft tissue in the buccal and lingual corridors to capture the required soft-tissue landmarks. The material is dispensed from the Plug & Press Dispenser (Kettenbach LP) efficiently into an impression tray at the precise rate and catalyst/base ration (Figures 2 and 3), and it has the consistency and flow of traditional alginate materials, but is far more dimensionally stable with fewer voids. With a total set time of 3 minutes and a thixotropic consistency that flows under pressure (it does not run spontaneously into the pharyngeal cavity), it is an excellent choice for patient comfort when taking full-arch preliminary impressions (Figure 4). In this case, the detailed and anatomically accurate impressions were nearly void-free, and minimal drags and pulls were evident (Figures 5 and 6).
 |
 |
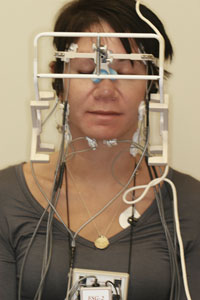
| Figure 7. After a thorough exam, a complete computer-assisted neuromuscular scan was performed. |
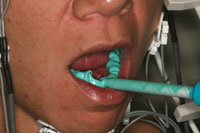
Figure 8. This A-siliconebite registration material (Futar [Kettenbach LP]) with an adequate working time of one minute and 30 seconds (1:30), flowed evenly and smoothly onto the patient’s teeth. |
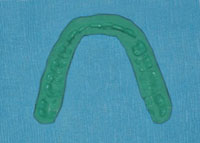 |
| Figure 9. The bite registration, shown after properly trimming with a lab scalpel and confirmation of the neuromuscular position. |
 |
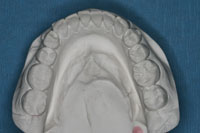 |
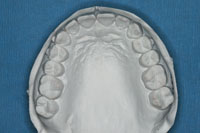
| Figures 10 and 11. Maxillary and mandibular full-arch models. Note the accurate detail of the not only the teeth but soft and hard tissues. While this vinyl polysiloxane (VPS) alginate substitute material (Kettenbach LP) is significantly more affordable than most traditional VPS or polyether crown and bridge impression materials, it still generated the extremely accurate casts that were required for this TMD case. |
 |
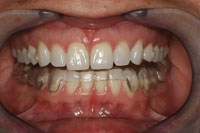 |
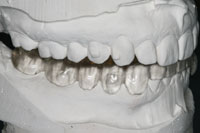
| Figure 12. The neuromuscular orthotic on the mounted models. | Figure 13. The seated and adjusted orthotic. |
Computer-Assisted Neuromuscular Assessment
Next, the patient was scheduled for a comprehensive neuromuscular evaluation using a computer-assisted jaw tracking device (Figure 7). Preoperative electromyography (EMG) tracings revealed hypertonic muscle activity, particularly in the left temporalis region with dominance over the masseter muscles and early muscle fatigue on clenching. Electrosonographic tracings during repetitive opening and closing revealed either adhesions or posterior displaced articular disks bilaterally upon closing, with bone to bone contact on opening. Jaw tracking scans revealed 3 mm of deviation to the left upon opening, limited lateral movement and sagittal tracings revealed dyskinesic (irregular) and bradykinesic (slow or protective) closure patterns congruent with the EMG and electrosonographic data. This data was collected and stored to serve as a baseline to be compared with post-treatment assessment. The patient underwent one hour of closely monitored transcutaneous electrical neural stimulation (TENS) in which cranial nerves V and VII were stimulated as well as the primary elevator muscle groups and the postural muscles of the cranium.
Bite Registration Technique
Regardless of occlusal philosophy or TMD management philosophy, altering a patient’s interocclusal relationship requires a highly accurate bite registration. Depending on the technique used, recording an exact bite relationship requires a material that has the appropriate elastomeric properties and working time to permit the desired position to be recorded. In neuromuscular dentistry, the myocentric bite is based on quantitative analysis of computer-generated scans and the patient receives TENS along a myocentric trajectory from isotonic rest. In this particular case, an A-silicone material (Futar [Kettenbach LP]) was chosen because, in the author’s opinion, it has the ideal working time and physical properties for taking a neuromuscular bite. This material exhibits minimum resistance as the patient bites together, preventing any displacement. Furthermore, it accurately reproduces the details of the occlusal surfaces and its fully polymerized state exhibits a hard but easily trimmed texture. It possesses many of the physical properties of a definitive crown and bridge impression material and has impressive permanent dimensional stability, virtually eliminating the risk of deformation. With a dispensing time of 30 seconds and a set time in the mouth of 90 seconds, this A-silicone material is an excellent choice for bite registrations that require time for mandibular positioning (Figure 8).
Several bites were taken, ultimately trimmed with a lab scalpel, and reseated in the mouth to cross-check the accuracy and reduced muscle activity. A properly trimmed final bite was used in mounting the models on which the mandibular neuromuscular orthotic was fabricated (Figure 9).
Working Models and Orthotic Fabrication and Delivery
The impressions and neuromuscular bite registration were then sent to the dental laboratory team, and they poured and mounted the models (Figures 10 and 11). Figure 12 shows the neuromuscular orthotic on the mounted models. Note the knife edge detail of the teeth, embrasures, and gingival tissues, as well as the fit of the orthotic on the mandibular model and the proper bite alignment created from the A-silicone bite registration.
The patient was scheduled for a one-hour appointment to have the orthotic seated in the mouth. Fit and alignment were assessed and after 45 minutes of TENS therapy, the patient was seated in an upright position and the final adjustments of the bite (orthotic) were checked (Figure 13).
CONCLUSION
The role of accurate full-arch impressions and bite registrations in the treatment of TMD pain is extremely important. While numerous impression and bite registration materials are available, the benefits of VPS alginate substitutes and A-silicone bite registration materials, such as those described herein, have been illustrated.
Dr. Blank graduated from the Medical University of South Carolina, College of Dental Medicine in 1989, and maintains a full-time private practice in Rock Hill, SC, where he emphasizes complex restorative reconstruction and cosmetic enhancement procedures. He holds an adjunct instructor post in the Department of General Dentistry at Medical University of South Carolina, College of Dental Medicine, and has authored dozens of clinical manuscripts on a variety of clinical techniques and materials. He is a Fellow in the Academy of Comprehensive Esthetics, and an active member of the International Association for Dental Research, the Academy of Operative Dentistry, the American Academy of Cosmetic Dentistry, the Pierre Fauchard Academy, the American Dental Association, and the Academy of General Dentistry. Dr. Blank has lectured throughout the United States, Europe, and in 9 countries in Asia, and holds US Patent for a composite finishing instrument and is the creator of the C.E.B.L. Technique for direct veneer layering. He can be reached at jblank@comporium.net or at carolinasmilecenter.com.
Disclosure: Dr. Blank reports no disclosures.