INTRODUCTION
One of the most common questions asked by general practitioners and specialists alike is: “How do I obturate the root canal system?” With many techniques and materials available to the practitioner, it can be difficult to know which system is the right one for both you and your patient’s tooth. Not all root canal systems are amenable to obturation with the same technique, just as not every canal can be shaped with the same file system. The degree of curvature, anatomical variations (c-shaped canals), and root maturity (open apices) play an important role in one’s selection of shaping, irrigation, and obturating techniques. With that being said, most practitioners develop their “go-to” technique. For many endodontists, our go-to technique is warm vertical condensation, either by the traditional method or continuous wave.
Preceding obturation of the root canal system is cleaning, shaping, and irrigation. These steps are critical to eliminate both pulpal remnants and microbial contamination while creating a suitable space to accept the root canal filling material. A well-prepared canal allows both instruments and filling material to be delivered to the most apical extent of the canal system so that the filling material can be compacted to create a good apical seal. Practitioners who are diligent in creating well-shaped and well-irrigated canal systems will find that quality obturation will be more easily obtainable regardless of their “go-to” technique.
The importance of quality obturation cannot be overemphasized in its contribution to successful treatment outcomes. Some have attempted to diminish its importance, suggesting that coronal microleakage through a poor-quality coronal restoration is the true final determinant of success or failure.1,2 They argue that the quality of the final restoration is more important than that of the obturation. However, this notion was challenged by Ricucci et al,3 as they looked at the histological and microbiological status of endodontically treated teeth that had been exposed to caries and the oral environment for prolonged periods of time. They studied teeth with poor-quality restorations for a period of at least 3 years, and found that well-prepared and well-filled root canals resisted bacterial penetration even when subjected to long-standing exposure to caries, restoration fracture, or the loss of coronal coverage altogether.3 This study demonstrated the importance of filling the root canal system completely in 3 dimensions. That’s the type of obturation that practitioners should strive for with their go-to technique. The goal of effective obturation should be, despite being subjected to constant bacterial challenge (for years), to create an impenetrable seal which prevents bacteria from reaching the periapical tissue and causing apical periodontitis. For many general dentists and endodontists, this goal is easily obtainable through warm vertical condensation.
Warm Vertical Condensation
Warm vertical condensation was first introduced in the 1960s as an effective and efficient way to obturate root canals.4 Like other techniques in dentistry, warm vertical condensation has become much improved in 50 years. Gone are the days of heating pluggers until they were cherry-red and plunging them into the canal. Not only was this more time consuming, but this technique was also alarming to the patient.
Later, heat sources (or downpack devices) were introduced that could heat a plugger to 200° in seconds, at the push of a button. Almost instantly gutta-percha was thermoplasticized and became moldable, allowing the practitioner to compact and adapt it to the irregular shape of the root canal system. Additionally, injectable backfill devices were introduced. These allowed practitioners to heat and inject softened gutta-percha into canals at the push of a button or the pull of a trigger. These new devices represented a huge leap forward in technology and became widely adopted by endodontists and general practitioners alike. Still, room for improvement remained, as many of the current devices were hampered by cords, irregular and excessive heating, and less-than-ergonomic designs.
Recently, a new obturation system was introduced (elementsfree dual-obturation unit [Kerr Endodontics]) that allows both downpack and backfill capabilities in a cordless design. The downpack unit features a 360° activation ring so that it can be easily activated from any position, digital control for temperature accuracy, and heats to 200°C in less than half a second and with an adjustable heating range of 100°C to 400°C. What makes it uniquely innovative is that it’s the first cordless backfill unit with motorized extrusion of gutta-percha, thereby decreasing hand fatigue and increasing delivery precision. Finally, aerogel insulation surrounds the heating element, which helps to protect your patient from excessive heat at the tip of the unit.
Three retreatment cases are presented that were completed by 3 different practitioners evaluating the elementsfree dual-obturation unit. All 3 practitioners utilized their own go-to technique, showing the versatility of the unit. Each practitioner will elaborate on the advantages that the elementsfree unit provided that contributed to the success of each respective case.
CASE REPORTS
Case 1 (Eric Pacheco, DDS)
An adult male patient presented with pain and edema in the mandibular right anterior. The patient reported that the pain and swelling had been present for 2 days. He was unable to bite or place pressure on tooth No. 26, and he had pain when touching the tooth and surrounding tissues. An oral examination of the area showed Class I mobility of No. 26, with sensitivity to vertical and lateral pressure. Cold tests produced no response.
The buccal gingiva and labial vestibule were moderately edematous and tender to palpation. Adjacent teeth showed no pain to percussion or lateral pressure. Periapical radiographs showed No. 26 with periapical radiolucency, prior endodontic treatment, and a PFM restoration. Moderate bone loss of the mandibular anterior dentition can be seen on the radiographs. Probing depths did not exceed 3 mm. The previously completed endodontic treatment appeared to be significantly short of the apical foramen (Figure 1).
CASE 1
|
After profound anesthesia was obtained under rubber dam isolation, a No. 20 stainless steel hand file and K3 rotary files (Kerr Endodontics) were used to remove the existing gutta-percha while No. 20 Hedstrom files were utilized to remove any residual sealer or gutta-percha attached to the canal walls.
The working length was determined by an electronic apex locator (Elements Diagnostic Unit [Kerr Endodontics]). Twisted File (TF) rotary NiTi files (Kerr Endodontics) were used to instrument to one third short of working length. Following apical gauging with hand files, canal shaping was continued with TF files. The canal was instrumented to a No. 30-.06 rotary file to working length. Purulent exudate continued to drain into the canal at the completion of instrumentation, and UltraCal (Ultradent Products) calcium hydroxide paste was placed as an interappointment medicament. The patient was prescribed Augmentin 500 mg, taken by mouth every 12 hours for 7 days.
At the final appointment, the canal was re-instrumented, re-irrigated, and dried with paper points. A 30-.06 gutta-percha cone was placed in the canal, and the fit was verified with a periapical radiograph. The master cone was removed, EndoREZ sealer (Ultradent Products) was applied to the canal walls, and a 30-.06 gutta-percha cone was re-inserted. The elementsfree downpack unit with .06 heat plugger was used to downpack the master cone to 4 mm from the working length, the gutta-percha was condensed with a hand plugger with light finger pressure. The elementsfree backfill unit was used to dispense the heated gutta-percha into the canal and also to backfill the canal to the cemento-enamel junction. This was condensed with hand pluggers using light finger pressure. A periapical radiograph was used to verify an adequate obturation.
The access opening was cleaned of excess sealer and etched for 15 seconds with 37% phosphoric acid. G-ænial Bond (GC America) was applied and light cured for 10 seconds. Composite resin was placed and the access opening sealed (Figure 2).
Case 2 (Garry L. Bey, DDS)
An adult female, with a history of pain, was referred for evaluation and retreatment of tooth No. 12 (Figure 3). Tooth No. 12 had root canal therapy completed approximately 3 months prior to being seen in our office. Upon initial examination, an angled preoperative intraoral digital radiograph showed that this maxillary first bicuspid possessed 3 roots. The mesiobuccal (MB) and palatal canals appeared to have been filled close to the radiographic apex. The obturation material in the distobuccal (DB) canal was limited to the coronal third of the root (Figures 4 and 5).
A CBCT scan of the left maxilla was performed with the Kodak 9000 (Carestream Dental) limited field of view at 76 μm and confirmed the presence of an unfilled DB root with a well-circumscribed periapical radiolucency present.
CASE 2
|
Access was made through the existing temporary restoration under rubber dam isolation. The gutta-percha from all 3 canals was removed using hand and rotary instruments. The canals were instrumented to a size .04/35 TF used in a TF Adaptive motor (Kerr Endodontics). A sterile cotton pellet was placed in the pulp chamber and the access cavity was sealed with Cavit W (3M). The patient was prescribed Amoxicillin 500 mg, 3 times daily.
At the second appointment, the apical preparation sizes were enlarged to a size 45 and 50 LightSpeed LSX file (Kerr Endodontics) for the buccal canals and the palatal canal, respectively. Final irrigation using EndoVac (Kerr Endodontics) was performed using 5.25% sodium hypochlorite (NaOCl), followed by 17% ethylenediaminetetraacetic acid (EDTA), and a final rinse of 5.25% NaOCl. The canals were then dried and obturated using the continuous wave of condensation technique with the cordless elementsfree dual-obturation unit (Figure 6).
Case 3 (Trent Lally, DDS, MSD)
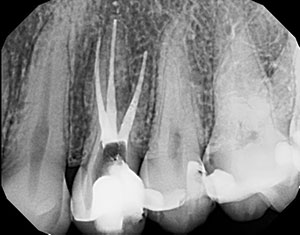
An adult female was referred by a prosthodontist who noted a periapical radiolucency associated with the MB root of tooth No. 14. The patient had the root canal therapy completed 8 years prior and was going to have the PFM crown replaced. The tooth was acutely sensitive to percussion at this time. No tenderness was reported upon buccal and palatal palpation. The tooth exhibited normal physiologic mobility, and probing depths ranged from 2 to 3 mm with little bleeding on probing. The tooth was nonresponsive to cold (Figures 7 to 9).
One clinical and 2 off-angle periapical radiographs were taken to evaluate the tooth. A periapical radiolucency was noted on the root of No. 13 and the MB root of tooth No. 14. A small radiopaque mass was noted in the apical 2 mm of the MB canal of tooth No. 14. The off-angle radiograph was inconclusive on the presence of a MB2 canal (Figure 10).
CASE 3
|
A small-volume CBCT scan was taken. The CBCT image showed the obturation material was off-center in the oval MB canal, indicating the possibility of a missed MB2 canal. However, a missed canal could not be definitively identified on the CBCT.
The tooth was diagnosed as being previously treated with symptomatic apical periodontitis. Due to the radiopaque obstruction in the MB canal and the presence of a post in the palatal canal, an apicoectomy was recommended for tooth No. 14. However, due to the patient’s past experience with the procedure, she declined, and nonsurgical retreatment was chosen. The risks, benefits, and treatment options were reviewed with the patient and an informed consent was obtained (Figure 11).
Anesthesia was obtained and the tooth was isolated using a rubber dam. The crown was removed and ultrasonic instruments were utilized to remove the post from the palatal canal. The previous obturation material was removed using a combination of Gates Glidden burs, K3XF NiTi rotary instruments (Kerr Endodontics), and K-files.
The MB2 was located, and working lengths were determined with the Elements Diagnostic Unit and confirmed radiographically. The obstruction in the MB canal could not be bypassed at this appointment. The canals were shaped using K3XF instruments. The buccal canals were finished to size 35 and the palatal canal to a size 55 master apical file, and 5.25% NaOCl and 17% EDTA was used as an irrigant throughout the procedure using a side-vented needle. Calcium hydroxide was placed as an interappointment medicament. The tooth was temporarily restored with resin modified glass ionomers (RMGIs) over a cotton pellet (Figures 12 to 14).
At the second treatment appointment, the obstruction in the MB canal was bypassed using small K-files and finished to a size 35. Final irrigation was completed using 5.25% NaOCl followed by 17% EDTA to remove the smear layer. A final rinse of 5.25% NaOCl was utilized and the canals dried with paper points. K3XF master gutta-percha cones were selected to match the master apical files. The cones were inserted to the full working length and exhibited apical tugback upon removal. Kerr Pulp Canal Sealer (Kerr Endodontics) was applied to the master cones and seated into the canals. The .10 tapered Buchanan Heat Plugger (Kerr Endodontics) in the elementsfree cordless downpack unit set at 200°C was used to sear off the cones at the orifice and were vertically condensed using hand pluggers. The .10 taper, 0.8 taper, 0.6 taper pluggers were used in sequential order to incrementally downpack and thermoplasticize the gutta-percha to within 3 mm of the apex. Vertical condensation was completed with hand pluggers after each increment. Two- to 3-mm increments of gutta-percha were injected into the canals using the elementsfree backfill unit set at 200°C and vertically condensed until the canals were completely 3-dimensionally obturated. The chamber was cleaned using isopropyl alcohol and dried. A cotton pellet was placed and the tooth was temporarily restored using RMGI.
DISCUSSION
Endodontic retreatment presents clinicians with many challenges, several of which are evident in these 3 cases. Prior to applying one’s go-to obturation technique, several hurdles need to be jumped, starting with a comprehensive preoperative examination and imaging.
CBCT is quickly becoming an important part of this preoperative assessment. CBCT images have been shown to be particularly useful in identifying reasons why the original attempt at root canal therapy was not successful.5 These 3-D images can detect missed canals, additional roots, previously unrecognized periapical lesions, and bone loss patterns associated with cracks.5 Cases 2 and 3 employed the use of CBCT to visualize and identify previously uninstrumented canal space. Both clinicians were able to direct a large portion of their efforts to addressing these canals, both of which were likely what led to the original treatment to be unsuccessful.
Following a proper preoperative assessment, treatment is initiated. Sometimes large metal posts or other obstructions must be removed in order to obtain access to the canals, as demonstrated in Case 3. This is most often accomplished with ultrasonic instruments. Once the canal space has been identified, practitioners have to remove the previous root canal filling. The root canal system is then reinstrumented and disinfected. In Case 1, the clinician was able to improve the previous root canal therapy by instrumenting the apical 2 mm of the canal system, a previously uninstrumented portion of the canal that likely harbored residual micro-organisms. In Cases 2 and 3, each was able to identify and clean the missed canals that were identified in the preoperative CBCT. This left all 3 practitioners with fully shaped and properly irrigated canal systems that were primed for their go-to obturation technique.
The elementsfree system is a dual-cordless unit that employs both a downpack device and a motorized backfill device. Cases 1 and 2 used the device for a continuous wave technique of warm vertical condensation. Both clinicians selected one of the many System B Heat Pluggers (Kerr Endodontics) that best matched the apical preparation, taper, and curvature of each canal. This allowed them to activate and plunge the tip to within 3 to 4 mm of the apex. This maximized condensation forces filling material and sealer to move into all areas of the root canal, including lateral canals, fins, and isthmuses.
The elementsfree cordless backfill device was then used to deliver warm gutta-percha to the most apical extent of the canal and filled in one or 2 increments. The backfill device needle was then placed in the canal in contact with the condensed gutta-percha and allowed to soften the gutta-percha. Once softened, the gutta-percha was dispensed into the canal. This eliminated the possibility of voids at the junction of the downpack and the backfill. The fill was then condensed at the orifice level using hand pluggers.
Case 3 is particularly interesting because it could have easily been treated with an apicoectomy of the MB root and placement of a root-end filling. The root-end filling would have encompassed both the MB1 and the unfilled MB2 canal. However, the patient limited our options to orthograde nonsurgical retreatment. Not only did a large metal post have to be removed, but also the small metal fragment that obstructed the canal had to be bypassed. Bypassing the metal fragment ensured that an irregularity was formed in the most apical portion of the root canal system, making an ideal habitat for bacteria to reside if left unfilled.
Because of this, a more traditional incremental approach to warm vertical obturation was implemented instead of a continuous wave technique (as seen in Cases 1 and 2). It’s been shown that an incremental downpack and an incremental backfill are able to obturate canal irregularities in the last 3 mm of the canal system more predictably.6 However, the traditional incremental approach has been difficult to perform with previously motorized extruder backfill units because it has been difficult to control the amount of gutta-percha being extruded into the canal. It has been the lead author’s experience that the gutta-percha would continue to be extruded once the activation button was released. The new elementsfree unit seems to have corrected this, and one can accurately extrude 2 to 3 mm of gutta-percha at a time without fear of overfilling the canal. With each canal filled exactly to the orifice level, there’s no need to go back and “clean up” and level off the obturation.
CLOSING COMMENTS
Until now, cordless backfill units were only available in what could be called “gun-style” units. These units required a handle to be squeezed, which could possibly lead to hand fatigue. The motorized extrusion by the backfill unit can lead to less hand fatigue during a busy day at the office. Additionally, the digital temperature and extrusion rate control allows practitioners to set their preferred settings for use during treatment. This way, they can “feel” the canal being backfilled. Finally, the aerogel insulation that surrounds the heating element protects the patient. Past units would easily overheat, and the shielding units have been known to come off.
We found the elementsfree unit ideal for clinicians looking to add warm vertical condensation to their practice. The cordless units can easily be moved among treatment rooms. Multiple pluggers are available to fit canals of varying shapes and sizes.
References
- Ray HA, Trope M. Periapical status of endodontically treated teeth in relation to the technical quality of the root filling and the coronal restoration. Int Endod J. 1995;28:12-18.
- Tronstad L, Asbjørnsen K, Døving L, et al. Influence of coronal restorations on the periapical health of endodontically treated teeth. Endod Dent Traumatol. 2000;16:218-221.
- Ricucci D, Gröndahl K, Bergenholtz G. Periapical status of root-filled teeth exposed to the oral environment by loss of restoration or caries. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;90:354-359.
- Schilder H. Filling root canals in three dimensions. Dent Clin North Am. November 1967:723-744.
- Patel S, Dawood A, Ford TP, et al. The potential applications of cone beam computed tomography in the management of endodontic problems. Int Endod J. 2007;40:818-830.
- Perry C, Kulild JC, Walker MP. Comparison of warm vertical compaction protocols to obturate artificially created defects in the apical one-third. J Endod. 2013;39:1176-1178.
Dr. Lally graduated from the University of Detroit Mercy School of Dentistry in 2012. He then completed an endodontic residency program at Louisiana State University School of Dentistry, where he earned his specialty certificate in endodontics in 2014. Upon completion of the endodontic program, he joined Valley Endodontic Specialty Group in Tucson, Ariz. He can be reached via email at tlally01@gmail.com.
Disclosure: Dr. Lally reports no disclosures.
Dr. Pacheco is a 2005 graduate of the University of Missouri-Kansas City School of Dentistry and practices in Albuquerque, NM. He can be reached at epacheco@comfortdental.biz.
Disclosure: Dr. Pacheco reports no disclosures.
Dr. Bey is in private practice in New York and New Jersey, specializing in endodontics. After graduating from Syracuse University with a BS in biology, he received his DDS degree from the New York University College of Dentistry. He lectures extensively and can be reached via email at rockendo@aol.com.
Disclosure: Dr. Bey conducts courses and lectures for which he receives honoraria from Kerr Dental.