 |
 |
| Figure 1a. The Bioclear Anterior Matrix Kit. Figure 1b. The Smile Design Gauge (Bioclear), front and back views. There are 5 grids based on 5 different central incisor widths. The incisor height is based on an 80% width-to-length ratio of the maxillary central incisor. A blank sixth side is for contrast photos of anterior sextants. |
INTRODUCTION
Anterior Aesthetic Dilemmas: Peg Laterals and Diastemata
Undersized maxillary lateral incisors and diastemata in the maxillary arch are anatomical anomalies that present little functional concern but greater aesthetic concerns. The prevalence of undersized laterals in the general population is 4.6%, with females affected more than men.1 The prevalence of maxillary midline diastemata has been reported to range from 1.6% to 25%, depending on developmental age and race.2 The traditional treatment options are indirect ceramic restorations or direct composite bonding. For adolescents and young adults, direct composite bonding is more common.
Traditional Treatment Options
For financial and physiologic concerns, direct composite restorations would seem reasonable for young patients. The procedure can be performed in a single visit, without the incurrence of lab fees, and is generally less costly. Direct composite restorations generally require no tooth reduction, which is ideal for young patients. Indirect ceramic restorations typically require multiple visits and have associated lab fees. The potential for continued passive eruption into the late teens to the early 20s presents the risk of restorative margin exposure, revealing an unaesthetic demarcation between tooth and restoration. Also, the potential need for tooth reduction and the risk for accelerated abrasive wear of the opposing dentition may be a concern.
Industry bias considers porcelain restorations to be the epitome of aesthetic treatment of anterior teeth. Direct composite restorations are often considered a compromised choice. For young patients, such a compromise is deemed clinically reasonable and practical. However, direct chairside procedures pose more challenges in controlling the final restorative outcome. Direct composite restorations are typically “free-handed,” even if a palatal matrix is used. Gingival overhangs often lead to hygiene difficulties and associated inflammatory responses. Layered composite restorations can be quite aesthetic; however, the technique requires skill and artistry. Most clinicians lack sufficient opportunities to practice and maintain the skills necessary to consistently achieve aesthetic outcomes with layering techniques.
Direct composite restorations are often too translucent, stained, and poorly finished and also have unhealthy gingival contours, poor proportions, and/or asymmetries. Initially, the patient may be happy with the outcome because a worse aesthetic issue was conquered. However, as restorations begin to deteriorate and patients’ aesthetic sensibilities mature, they may become self-conscious of their smiles. Clinicians may consider direct composite bonding as a reasonable solution until the patient can “upgrade” to a more “definitive” porcelain restoration. However, during an important psychosocial developmental stage, the embarrassment and negative impact on confidence generated by an unaesthetic smile can be significant.
The Bioclear Method
In this article, the Bioclear Method is proposed as a third option. The Bioclear Method is not traditional direct composite bonding. Hand-layered composite is prone to incorporation of seams and voids that contribute to structural weakness, overhangs, pitting, and staining of the restoration. According to the Department of Polymer Technology at the Royal Institute of Technology in Stockholm, knit lines in polymers (similar to seams in hand-manipulated composites) may result in a significant reduction in fracture resistance. Monolithic forms have better integrity and strength than hand-layered forms, as seen with ceramics. The Bioclear Method is a direct overmolding technique where heated composite resin is injected into anatomic matrices, resulting in a tooth shrink-wrapped in a monolithic form.
The Bioclear Method can create strong, void-free, stain-resistant restorations with incredible shine retention; infinity margins; and smooth, convex subgingival contours when done well. Unlike porcelain restorations, Bioclear restorations fit around the tooth. There is no need to sacrifice tooth structure for the restoration to fit. In addition, the possibility of a near imperceptible restorative margin, mostly on enamel, avoids concerns of a subgingival cement gap at the margin that can occur with porcelain restorations. Rejuvenation with the Bioclear Method offers an aesthetic treatment alternative to porcelain at a minimal biologic cost. It also offers a more robust, long-term treatment option compared to traditional composite bonding.
Chairside Smile Design
A common technique for planning and executing direct treatment of anterior aesthetic cases is the use of a diagnostic wax-up and putty matrix to create a palatal shelf. The advantages are an ability to preview the final outcome and an ability to create a one-walled custom palatal matrix. The disadvantage is the additional laboratory time and costs involved in doing a “bench top smile design.”
The Bioclear Matrices are anatomic forms for the mesial, distal, and gingival contours of a tooth (Figure 1a). The matrices create a smooth Mylar finish of these contours that previously could not be polished. This is especially critical in the subgingival areas for tissue health. The labial, palatal, and incisal walls are easily shaped and polished for a customized restorative outcome. Because the system precludes the need for a diagnostic wax-up to create a custom matrix, the method has incorporated “chairside smile design.” This offers the advantage of diagnostic planning done with clinical photography instead of time-consuming study models and diagnostic wax-ups.
The Smile Design Gauge (Bioclear) is a 6-sided contraster, of which 5 sides have a golden proportion grid based on 5 central incisor widths (Figure 1b). The widths range from 8.0 to 10.0 mm in 0.5-mm increments. The golden proportionality is not universal for all dental arches. The recurring esthetic dental (RED) proportions have been proposed to customize the proportionality, from 60% to 80%, to the patients’ physical type.3 The author has designed the gauge to serve as a visual tool. The purpose of the grid is not to function as an absolute rule in making a clinical case fit within the golden proportion; rather, the grid serves as a multifunctional tool, enabling the clinician to visualize the mesial-to-distal projection and symmetry of the smile based upon the central incisor width. As a visual tool, the grid can aid the clinician in adjusting the smile proportionality to achieve a conservative and aesthetic outcome (Table 1).
 |
CASE REPORTS
Case 1: A Peg Lateral Case
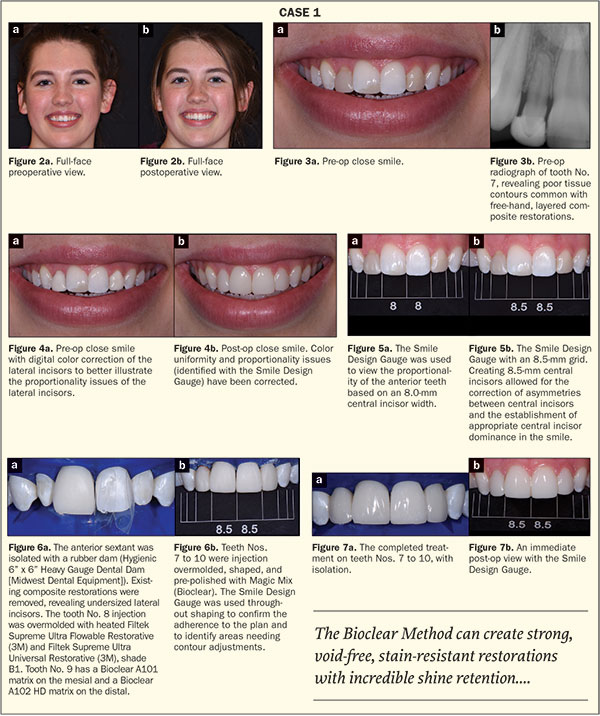
A 17-year-old female patient presented with undersized maxillary lateral incisors. She disliked the discolored composite restorations done 2 years prior (Figure 2). Other aesthetic detractors observed were a midline cant causing asymmetry of central incisors, a lack of central incisor dominance due to wide lateral incisor restorations, and unhealthy gingival contours (Figures 3 and 4). The Smile Design Gauge was used for diagnostic planning and treatment execution (Figures 5 to 7). After viewing the proportionality of the smile based on an 8.0-mm versus an 8.5-mm central incisor, it was decided that an 8.5-mm central incisor proportion would allow for appropriate central incisor dominance and lateral incisor proportions.
The case was restored with Scotchbond Universal Adhesive (3M) and Filtek Supreme Ultra Flowable Restorative (3M) and Filtek Supreme Ultra Universal Restorative (3M), shade B1.
Case 2: A Diastema Case
A 48-year-old male patient presented with multiple diastemata in the maxillary anterior sextant. His primary goal was to close the spaces and improve the aesthetics of his smile with minimal tooth structure removal (Figures 8 and 9). The Smile Design Gauge was again used for diagnostic planning and treatment execution (Figures 10 to 12). The 9.0-mm and 9.5-mm proportions were considered. It was decided that the 9.0-mm proportion would work best to maintain closer-to-ideal central incisor width-to-length ratios. The 9.0-mm grid was then evaluated at the center of the midline diastema and the center of the facial midline to assess if the facial and maxillary midline discrepancy could be corrected.
The case was restored with Scotchbond Universal Adhesive and Filtek Supreme Ultra Flowable and Universal Restoratives, shade A1.
 |
IN SUMMARY
Chairside smile design and the Bioclear Method of injection overmolding anteriors offers a third option for aesthetic treatment. The advantages of direct composite restorations (single-visit treatment, lesser financial cost, and preservation of tooth structure) are combined with the advantages of porcelain (better strength, integrity, and aesthetics). With this option, the patient does not have to compromise aesthetics, restorative longevity, or tooth structure. The preservation of tooth structure maintains all treatment options for the future. With the increase in average patient life span and improved dental maintenance, the Bioclear Method is an attractive and conservative treatment alternative for patients.
References
- Citak M, Cakici EB, Benkli YA, et al. Dental anomalies in an orthodontic patient population with maxillary lateral incisor agenesis. Dental Press J Orthod. 2016;21:98-102.
- Abu-Hussein M, Watted N. Maxillary midline diastema—aetiology and orthodontic treatment—clinical review. IOSR Journal of Dental and Medical Sciences. 2016;15:116-130.
- Ward DH. Using the RED proportion to engineer the perfect smile. Dent Today. 2008;27:112-117.
Dr. Kim maintains a full-time practice in Tacoma, Wash, and Bellevue, Wash. She is also co-director of and full faculty at the Bioclear Learning Center International in Tacoma, where she develops new curriculum and teaches. She can be reached via email at jihyonkim@bioclearmatrix.com.
Disclosure: Dr. Kim has a financial interest in Bioclear’s Smile Design Gauge.
Related Articles
Full-Mouth Black Triangle Treatment Protocol
Are Curriculums in Need of an Update?
Composite Versus Porcelain, Part 2: The 360° Composite Resin Veneer











