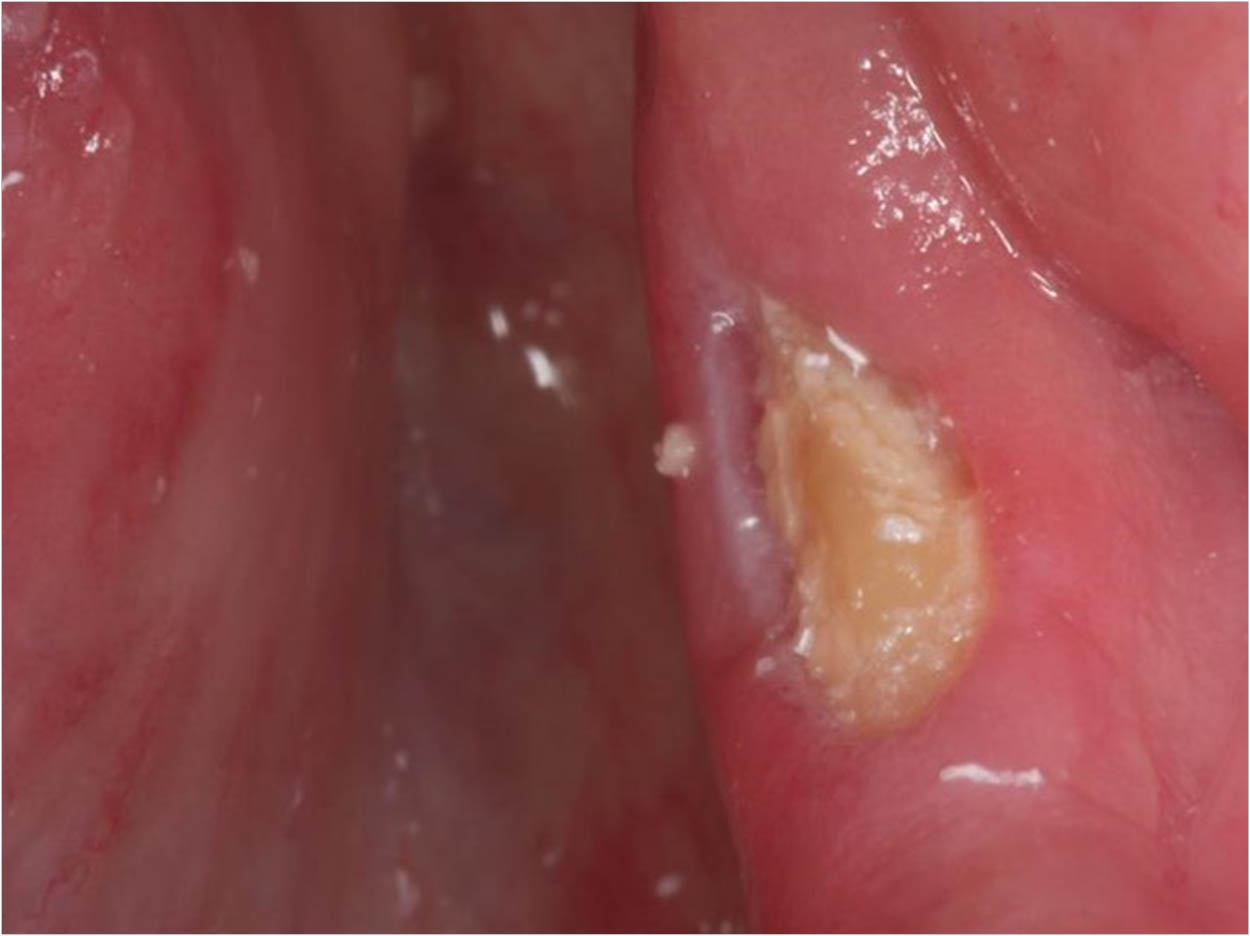
Researchers in California report a breakthrough to prevent damage to the jaw, a side effect suffered by some people undergoing treatment for cancer or osteoporosis. They call it an important step toward a cure for osteonecrosis of the jaw, a rare side effect caused by drugs commonly used to combat bone loss.
Osteonecrosis causes severe and persistent inflammation, leading to loss of bone from the jaw. It has no effective prevention or cure. Though small, the researchers say, the risk deters people from taking drugs needed to fight bone cancer or prevent fractures due to loss of bone density. The researchers also hope to adapt the successful animal experiment to treat the condition in people.
“This is a condition that has been excruciatingly painful and difficult to treat for more than a decade,” said Charles McKenna, PhD, a professor of chemistry at the University of Southern California (USC) Dornsife College of Letters, Arts, and Sciences and adjunct professor of pharmacology and pharmaceutical sciences in the USC School of Pharmacy. “We think our new approach may provide hope for the future.”
For years, bisphosphonates (BPs) have been used to treat metastatic bone cancer patients and to maintain bone density in osteoporosis patients. They include a range of compounds that can stick to bone like Velcro, the researchers say. But when used in high doses in the cancer clinic, BPs sometimes cause necrosis in the jaw. It often occurs after a tooth is removed, the gap doesn’t heal, and the jaw begins to deteriorate.
The condition is very rare at the lower BP doses used to combat osteoporosis, but many patients avoid the drugs out of fear of their side effects. The National Osteoporosis Foundation estimates incidence of osteonecrosis of the jaw due to BPs to be between 1 in 10,000 and 1 in 100,000 people annually. The risk is higher, about 3% of patients, in the BP dose used to treat cancer, McKenna said.
Yet the researchers say that more and more osteoporosis patients are willing to take their chances with the disease rather than risk the side effects. Surveys have shown the recent trend in reduced hip fractures among postmenopausal women may be reversing due to BP drug aversion, the researchers report.
“The fear factor of this condition has led to severe underuse of bisphosphonates for osteoporosis, so much so that we’re seeing a rise in hip fractures in elderly people, aversion to bisphosphonates in oncology clinics, and liability concerns in the dental office,” McKenna said.
To solve the problem, the researchers used a different inactive BP compound that could be used locally in the mouth to push the BP drug from the jawbone while leaving undisturbed the useful drug in the rest of the skeleton.
“Think of it as a way to fight fire with a fire,” McKenna said.
The researchers used mice to test different BPs attached to fluorescent dyes. One color label coded the BP zoledronate, which is administered systemically to treat osteoporosis and cancer, while a different color labeled “rescue BP” coded a BP compound with similar bone affinity but no biological activity.
The researchers discovered that rescue BP injected into the jaw removed most of the BP drug that caused the jawbone tissue damage, clearing the way for the animal’s natural healing process to repair the extraction site. The researchers note, however, that the new technique isn’t ready for clinical use in human beings.
BioVinc, which provided funding for the study via a National Institutes of Health small business grant, will advance the treatment to commercial clinical use. Several of the authors of the study have a financial interest in the company, which specializes in bone-targeted therapeutics and diagnostics. McKenna is the company’s academic founder.
The study, “Rescue Bisphosphonate Treatment of Alveolar Bone Improves Extraction Socket Healing and Reduces Osteonecrosis in Zoledronate-Treated Mice,” was published by Bone.
Related Articles
An Oral Bisphosphonate Dilemma
PRF Proves Effective in 15-Year Retrospective Study
Oral Complications Rarely Follow Osteoporosis Treatment


