
What do you get when you combine today’s successful, evidence-based gingival grafting techniques with the healing benefits of platelet-rich plasma (PRP)? I present alloderm reverse tunneling (ART), a proprietary approach to addressing gingival recession, mucogingival defects, and nonprotective, thin tissue biotypes.
ART combines aspects of sulcular manipulation of the gingiva and vestibular tunneling to facilitate access, improve tissue mobilization, and create ease of graft insertion without harming the overlying tissues. The addition of PRP to the graft material has been suggested to accelerate soft-tissue wound healing, promote revascularization of the surgical wound, and facilitate patient recovery.
The Background
Past treatment modalities for the correction of gingival recession stem from the subepithelial connective tissue graft, first described by Langer and Langer in 1985.1 Their technique involved vertical incisions, a partial thickness flap, and procurement of the subepithelial layer of connective tissue grafts (SECTG) for root coverage. Variations in this technique have been proposed such as Nelson’s replacement of the partial thickness flap with a full thickness dissection.2
Around the same time, Raetzke introduced the envelope technique, whereby a partial thickness envelope or pouch around the involved teeth was created to accommodate a free SECTG without the need for vertical incisions.3 In 1994, Allen modified Raetzke’s technique by introducing the tunnel or supraperiosteal envelope technique to address multiple adjacent recession defects.4 Variations of this procedure include Santarelli et al’s single vertical incision tunnel technique and Mahn’s tunnel approach using a full thickness dissection with vertical incisions.5,6
With the introduction of an acellular dermal matrix (Alloderm [LifeCell]), root coverage outcomes using this extracellular matrix of freeze-dried cadaver tissue have been shown to be equivalent to those with palatal connective tissue.7-10 The current manufacturer’s protocol for the use of Alloderm is the alternate papilla tunnel method, as described in a 2005 journal article.11
The advantages of this technique over the previous tunneling method include better access for pouch creation, tissue mobilization, and graft insertion with the use of an alternating incised papillae design. The intact papillae in the surgical region are also tunneled without separation to stabilize the wound and prevent tissue retraction.
Published in 2012, Chao introduced the pinhole surgical technique, a novel approach to root coverage, performed through incisions of 2 to 3 mm in diameter made by a No. 12 scalpel in the alveolar mucosa.12 Further features of this technique include a full thickness tunnel performed through the pinhole access points, inclusion of at least 4 papillae into the pouch design, and stabilization of the flap with Bio-Gide (Geistlich Biomaterials) bioresorbable membranes, which eliminate the need for suturing.
In 17% of cases (21 of 121 total sites), Alloderm was used without specifying the indication for its use. However, no significant differences were noted when comparing the results between the use of bioresorbable membranes and Alloderm in the study.12
The ART Technique
The ART technique represents a combination of key features contained within the previously described gingival grafting protocols. Highlights of this proprietary technique include the following:
- Application of PRP (partitioned blood containing patient-derived growth factors) to facilitate wound healing, enhance graft/flap stabilization, and improve recovery times with minimal postoperative symptomology;
- Simplified surgical armamentarium consisting mainly of a curved/flexible blade, a double-end titanium-nitride composite instrument or equivalent for tunneling (11 mm long/1.8 mm wide working blade), a SUB-O Gracey curette (Hu-Friedy) or equivalent for advancing the tunnel, a 15 UNC periodontal probe (Hu-Friedy) to verify dissection and continuity of the pouch, and a Castroviejo needle holder (Hu-Friedy) for suturing;
- Bidirectional tunneling of the gingival tissues to improve tunnel creation, tissue mobility, and graft insertion while minimizing nicks, tears, and perforations to the free gingival margins, gingival vent entry points in the alveolar mucosa, and overlying native tissues (the term “reverse” tunneling implies performing the flap dissection in the opposite direction, in the context that it is either being compared to sulcular or vestibular tunneling methods);
- Maximum access to the subgingival environment through multiple entry points, which allows for optimal navigation through challenging biotypes and non-uniform bony architecture and around anatomical limitations within the surgical region;
- Ease of insertion of the grafting material (Alloderm) via suture anchoring to the graft material, sulcular threading of the suture, and graft advancement by way of the suture leading the Alloderm through the tunneled preparation (a single papilla may be incised at the furthest point of the surgical region to accommodate the width component of the graft through the first gingival sulcus).
Case Studies
In the first case, a 46-year-old female patient presented with moderate recession in the aesthetic zone. She was considering veneers at the time of consultation and was interested in evening out the gingival zeniths of her teeth prior to any planned restorative work. As a busy business consultant with a heavy work schedule, she was concerned with any inconveniences after gum recession treatment that might impact her ability to work and travel for business. The ART gingival grafting technique was proposed due to its minimal recovery time with no downtime from work (Figures 1 to 4).
 |
 |
|
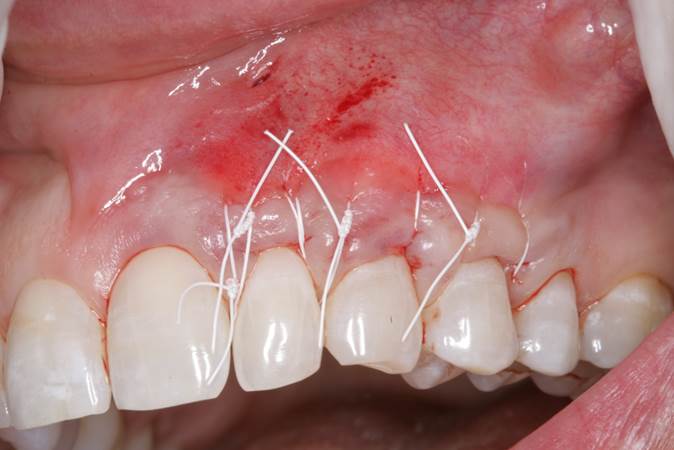
Figure 2. Immediate postop of the alloderm reverse tunneling (ART) gingival grafting technique, showing sling suturing with 4-0 polytetrafluoroethylene (PTFE) sutures and a gingival vent in the alveolar mucosa above tooth No. 10. |
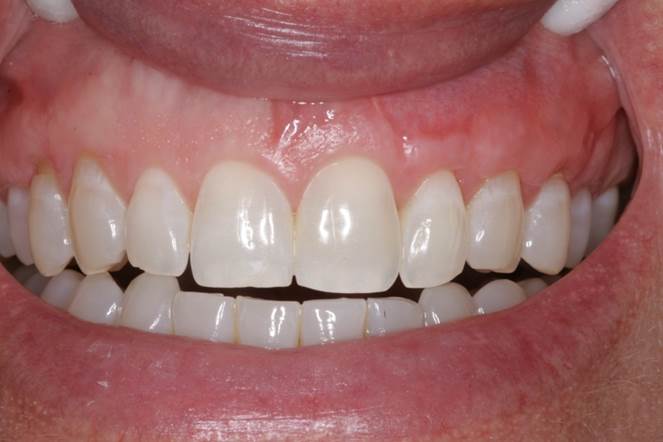
Figure 3. Retracted view of the postop result after 6 months of healing, showing full root coverage of the recession defects. |
 |
|
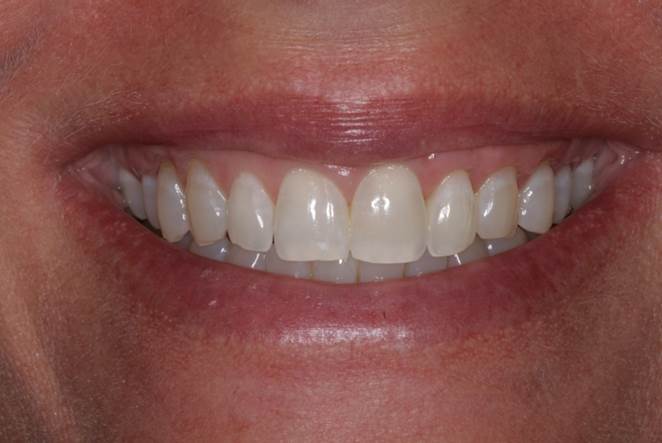
Figure 4. The patient’s smile photo after 6 months of healing, showing proportional gingival characteristics in the anterior maxillary region. |
In the second case, a 32-year-old male patient presented with moderate recession on his canines and premolars. He was stressed about gum changes occurring at such an early age and was afraid of losing his teeth. He had heard several horrible accounts of gum grafting from the roof of the mouth by family members and friends, so he was seeking an alternative treatment option that did not involve the use of his own tissues. The ART gingival grafting technique was suggested as a great alternative therapy to conventional palatal gum grafting. This patient was relieved to hear that no secondary surgical site was needed and the outcome would be highly aesthetic (Figures 5 to 10).
 |
 |
|
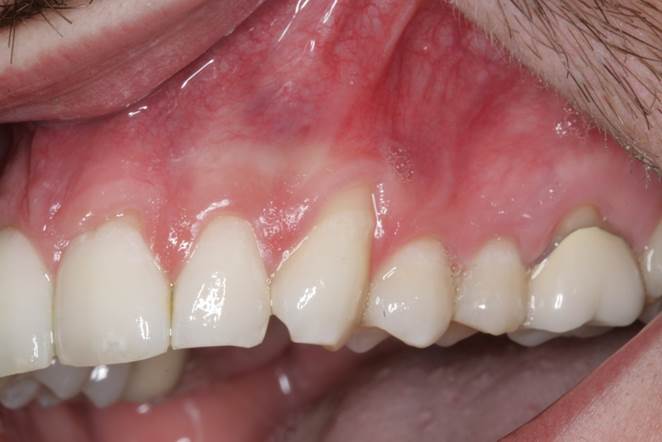
Figure 5. Pre-op presentation of a 32-year-old male, showing mild to moderate recession on teeth Nos. 9 and 11 with minimal keratinized tissue at the canine region. |
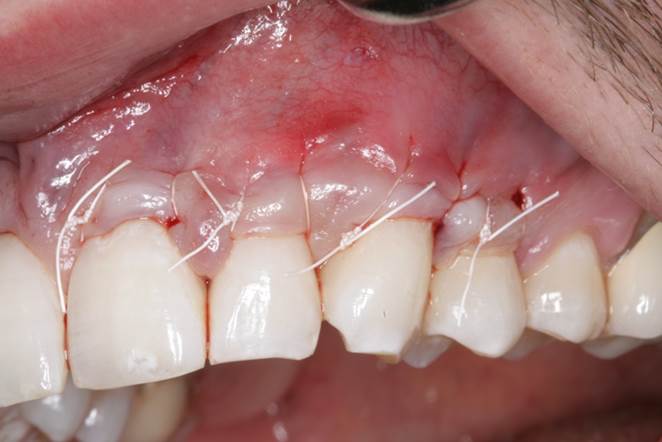
Figure 6. Immediate postop photo of the ART gingival grafting technique showing sling suturing with 4-0 PTFE sutures and a gingival vent in the alveolar mucosa above tooth No. 11. |
 |
 |
|
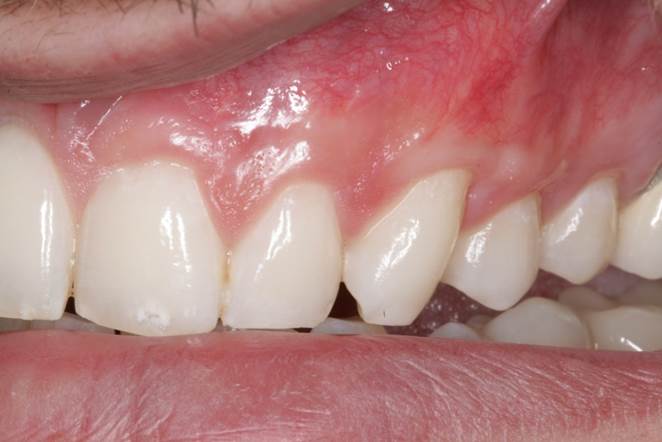
Figure 7. Retracted view of the postop result after 6 months of healing, showing full root coverage of the recession defects. |
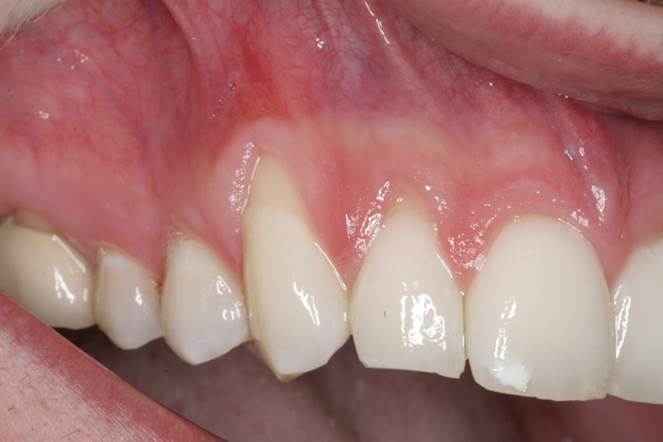
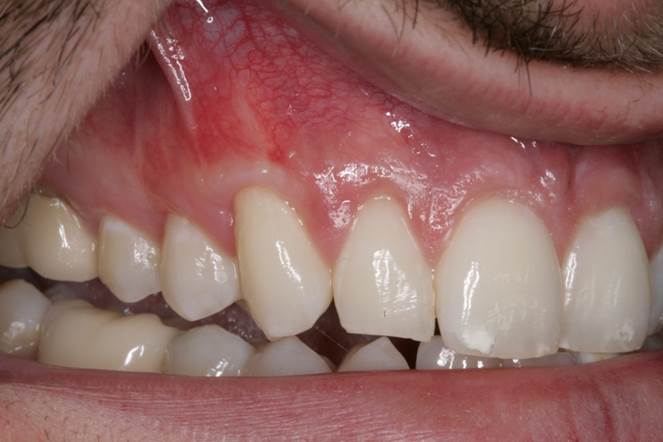
Figure 8. Pre-op presentation of the same 32-year-old male, showing mild to moderate recession on teeth Nos. 5 to 7 with minimal keratinized tissue at the canine region. |
 |
 |
|
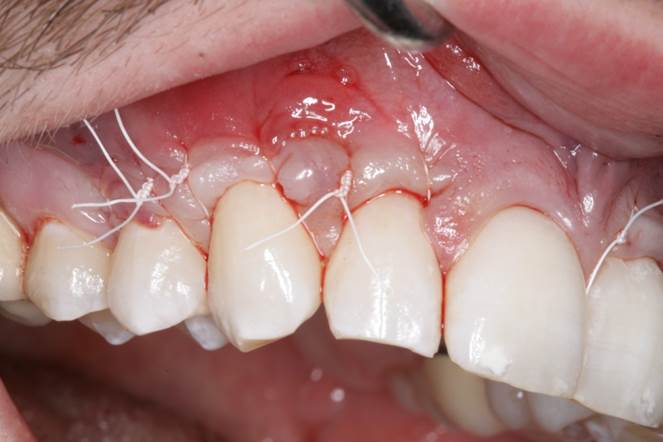
Figure 9. Immediate postop photo of the ART gingival grafting technique showing sling suturing with 4-0 PTFE sutures and a gingival vent in the alveolar mucosa above teeth Nos. 6 and 7. |
Figure 10. Retracted view of the postop result after 6 months of healing, showing full root coverage of the recession defects. |
In the third case, a 39-year-old male patient presented with moderate recession in the aesthetic zone and was very apprehensive about proceeding with any type of corrective gum grafting. He was interested in newer techniques available for the treatment of gum recession that would be painless in approach with minimal recovery time. The ART gingival grafting technique was recommended to fulfill his preferences and establish appropriate root coverage on the affected teeth (Figures 11 to 13).
 |
 |
|
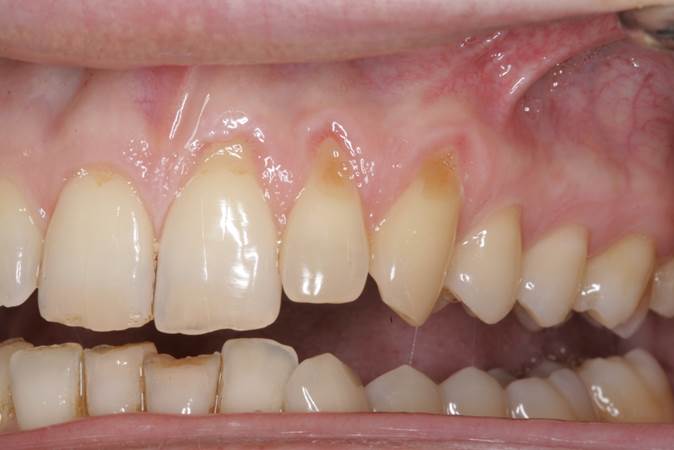
Figure 11. Pre-op presentation of a 39-year-old male, showing moderate recession on teeth Nos. 9 to 11 with notable cosmetic concerns that affect his smile. |
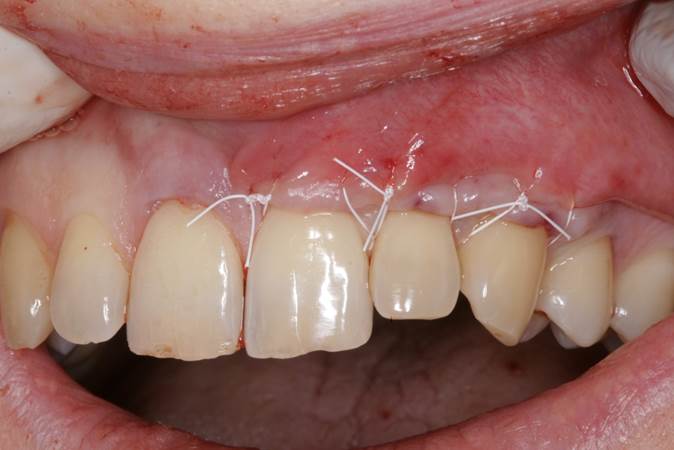
Figure 12. Immediate postop photo of the ART gingival grafting technique, showing sling suturing with 4-0 PTFE sutures (gingival vent not visible in the photo). |
 |
|
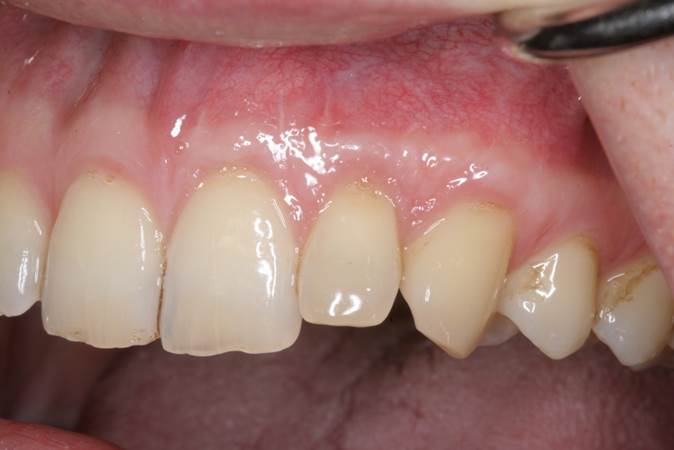
Figure 13. Retracted view of the postop result after 6 months of healing, showing full root coverage of the recession defects. |
Conclusion
Since the emergence of periodontal therapies aimed at treating exposed root surfaces and tissue insufficiency, gingival grafting techniques have continued to evolve and have improved dramatically since their inception. Different approaches have developed, along with minor changes and alterations, to existing treatment protocols.
Today’s techniques represent the highest evolution of our treatment approaches offered to patients in the dental setting. Through surgical innovation, we will continue to refine our methods and materials in the area of these periodontal therapies.
ART is just one of many contemporary variations of previously described gingival grafting techniques. And through this progressive manner, the field of periodontics continues to modernize and transform its treatment approaches for the benefit of a growing patient population.
References
- Langer B, Langer L. Subepithelial connective tissue graft technique for root coverage. J Periodontol. 1985;56:715-720.
- Nelson SW. The subpedicle connective tissue graft. A bilaminar reconstructive procedure for the coverage of denuded root surfaces. J Periodontol. 1987;58:95-102.
- Raetzke PB. Covering localized areas of root exposure employing the “envelope” technique. J Periodontol. 1985;56:397-402.
- Allen AL. Use of the supraperiosteal envelope in soft tissue grafting for root coverage. I. Rationale and technique. Int J Periodontics Restorative Dent. 1994;14:216-227.
- Santarelli GA, Ciancaglini R, Campanari F, et al. Connective tissue grafting employing the tunnel technique: a case report of complete root coverage in the anterior maxilla. Int J Periodontics Restorative Dent. 2001;21:77-83.
- Mahn DH. Treatment of gingival recession with a modified “tunnel” technique and an acellular dermal connective tissue allograft. Pract Proced Aesthet Dent. 2001;13:69-74.
- Aichelmann-Reidy ME, Yukna RA, Evans GH, et al. Clinical evaluation of acellular allograft dermis for the treatment of human gingival recession. J Periodontol. 2001;72:998-1005.
- Novaes AB Jr, Grisi DC, Molina GO, et al. Comparative 6-month clinical study of a subepithelial connective tissue graft and acellular dermal matrix graft for the treatment of gingival recession. J Periodontol.2001;72:1477-1484.
- Paolantonio M, Dolci M, Esposito P, et al. Subpedicle acellular dermal matrix graft and autogenous connective tissue graft in the treatment of gingival recessions: a comparative 1-year clinical study. J Periodontol. 2002;73:1299-1307.
- Tal H, Moses O, Zohar R, et al. Root coverage of advanced gingival recession: a comparative study between acellular dermal matrix allograft and subepithelial connective tissue grafts.J Periodontol. 2002;73:1405-1411.
- Cummings LC, Kaldahl WB, Allen EP. Histologic evaluation of autogenous connective tissue and acellular dermal matrix grafts in humans. J Periodontol. 2005;76:178-186.
- Chao JC. A novel approach to root coverage: the pinhole surgical technique. Int J Periodontics Restorative Dent. 2012;32:521-531.
Dr. Reganato is a diplomate of the American Board of Periodontology and a private practice periodontist in the Chicagoland area. Previous educational institutions include the New York University College of Dentistry for his DDS degree, Long Island Jewish Medical Center for his chief residency appointment, University of Alabama at Birmingham (UAB) and Birmingham Veterans Affairs Medical Center for his dual residency degree in periodontology, and UAB Graduate school for his master’s in clinical dentistry. He can be reached at perio.tutor@gmail.com.
Related Articles
California’s Brightest Students Shine at Table Clinic Competition
Basics of Platelet-Rich Fibrin Therapy
AlloDerm: An Effective Alternative to Palatal Donor Tissue for Treatment of Gingival Recession











