INTRODUCTION
Air abrasion (Accelerated Particle Ablation [APA]) has been accepted for years in dentistry for many applications. It is used daily by a large number of dentists and their clinical teams for removing cement from crowns and preparing surfaces for crown-and-bridge and prosthetic repairs. These routine uses are only a small sample of what really can be done with the APA systems available today. There was a renaissance of APA in dentistry 20 years ago, but this seemed to fall by the wayside as dentistry focused more on comprehensive care and aesthetic renovations. Now that the economy has taken a downturn, APA is poised for a second renaissance. Patients are now looking for “meat and potato” dentistry to get them through these financially risky times, and they will probably demand more elective care once the economy improves. Reportedly, one of the main reasons for abandoning the use of APA in the preparation of teeth was the overspray of dry aluminous oxide particles. It was difficult to contain all the dry particles, even with the assistant using high-volume evacuation, and thus dusty surfaces were created in the operatory. J. Tim Rainey and his associates found that focusing water spray on the stream of aluminous oxide particles would hold this overspray down to a minimum, and a side benefit to employing this technique was that one could cut deeper into the tooth structure with less discomfort.
A new version of a well-established air-abrasion unit, the PrepStart (Danville Materials), was recently introduced. This enhanced unit provides a circumferential halo of water that is picked up by the aluminous oxide particle stream, thereby solving the overspray issue. By controlling the amount of water, particle beam, and air pressure, teeth can be comfortably and conservatively restored.
BIOMIMETICS: MINIMALLY INVASIVE TECHNIQUES
Biomimetics (mimicking nature) is a new buzzword in dentistry, and employing this concept is made easier with the minimally invasive removal of mainly the diseased tissues with APA preparations. Preparations in cavitated teeth should remove only the cavitated tooth structure so that we can restore the tooth back to nearly 100% of the strength of the virgin tooth. APA allows the clinician to easily remove tissue from the cavitated areas, removing diseased tissues and leaving a solid microtextured tooth structure for bonding.
 |
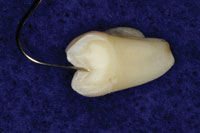 |
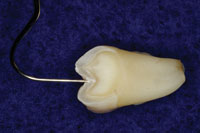
| Figure 1. Cross section of tooth showing a new sharp explorer and carious lesion. | Figure 2. Accelerated Particle Ablation (APA) preparation with sharp explorer showing the extent of tooth removal. |
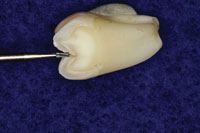 |
|
Figure 3. A 330 carbide bur shown superimposed over the APA preparation. |
Figure 1 shows a cross section of a tooth that has been tested with a Diagnodent (KaVo) at a measured level of 39. Figure 2 shows the same tooth with APA preparation, and Figure 3 shows a comparison to the profile of a 330 bur that many of us were taught to use in dental school pediatric clinics. In order to be more conservative, many dentists have moved to smaller burs like the 330. However, as the photo demonstrates, there is still much more tooth structure removed with these burs or even the new fissurotomy burs.
Another side benefit of APA is that it minimizes any unintentional trauma to the quite fragile enamel surfaces. Rotary instruments (even electric handpieces) lose their concentricity, resulting in eccentric movements that create enough trauma to the enamel to fracture it at the surface when using carbide burs. These fractures radiate from the cavosurface margins of the preparation and can compromise the bond to enamel. By diagnosing and treating teeth early, the future need for larger restorations can be reduced. Diagnodents and other nontraumatic diagnostic tools allow clinicians to identify areas of cavitations earlier to allow us to treat at these early stages.
The following cases are used to illustrate the early treatment of cavitated lesions and how APA can be used to treat active lesions with biomimetic techniques.
CASE 1
 |
 |
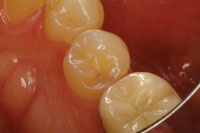
| Figure 4. (Case 1) Preoperative photo (mirrored view) of a distalocclusal carious lesion, with an intact distal marginal ridge, on tooth No. 20. |
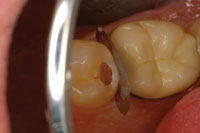
Figure 5. APA preparation after all caries were removed. |
 |
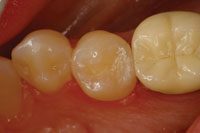 |
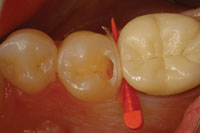
| Figure 6. A matrix and wedge was placed to keep bonding materials away from the adjacent teeth. | Figure 7. Immediate photo of the finished distalocclusal filling (Filtek Supreme Plus [3M ESPE]), after occlusal adjustment. |
This case involved tooth No. 20, which appeared to need a straightforward occlusal filling (Figure 4). A Diagnodent reading of 45 was noted in the distal pit, and radiographs hinted of some deeper involvement. Upon preparation with APA, the cavitated lesion extended down the distal aspect of the enamel and perforated distally just below the area of contact interproximally (Figure 5). The peripheral rim of enamel crossing the marginal ridge was undamaged, so a traditional proximal box was not developed; instead, a tunnel-type preparation was utilized. The tooth was prepared entirely using the APA technology. The peripheral rim of enamel gives strength to the tooth, making preservation of this structure important to the long-term success of a restoration. The area was isolated, then a matrix and wedge were placed (Figure 6). The preparation was etched with 35% phosphoric acid and a bonding resin was applied (PQ1 [Ultradent Products]). Then, the restoration was completed using a nanofilled composite resin (Filtek Supreme Plus [3M ESPE]) (Figure 7).
CASE 2
 |
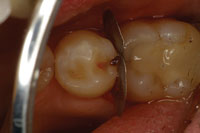 |
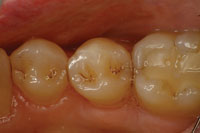
| Figure 8. (Case 2) Preoperative photo of caries associated with a distal fracture in tooth No. 20 (mirrored view). | Figure 9. Initial preparation with APA utilizing a metal matrix to protect adjacent interproximal surfaces and soft tissues. |
 |
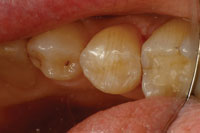 |
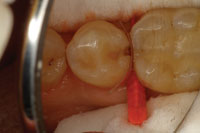
| Figure 10. The tooth was isolated and a matrix and wedge placed. The finished APA preparation is shown. | Figure 11. Immediate photo of the finished minimally invasive Class II composite resin restoration. |
This case illustrates a very common problem that we see every day in our practices. In tooth No. 20, there was a fracture of the peripheral rim of enamel, and decay had migrated through the enamel fracture and started to demineralize the dentin through this crack (Figure 8). Many times, we fail to diagnose these lesions until the enamel of the occlusal surface is undermined and the enamel collapses into the undermined lesion from the forces of occlusion. In this case, the crack through the marginal ridge was starting to demineralize the walls of the crack and stains appeared, so a visible diagnosis was made early. Respecting the adjacent tissues, a small slot preparation was created by dissecting down through the crack with APA and strong magnification. The preparation was extended, following the crack, to the cervical dentin enamel junction (DEJ) where the fracture had terminated (Figure 9). Lateral spread of the lesion stopped just inside the dentin. As there was no lateral spread of the lesion along the interproximal DEJ, the preparation was maintained with a slot design, and the area was isolated and restored (Figures 10 and 11).
CASE 3
 |
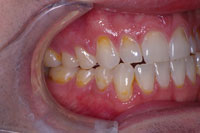 |
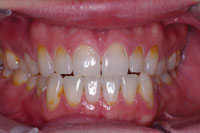
| Figure 12. (Case 3) Preoperative anterior view of the eroded and carious teeth. | Figure 13. Right lateral preoperative view. |
 |
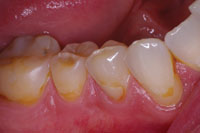 |
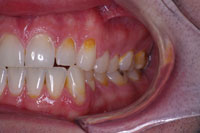
| Figure 14. Left lateral preoperative view. |
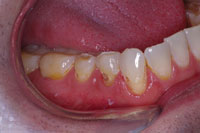
Figure 15. Closeup of the eroded teeth and failed restorations. |
 |
 |
|
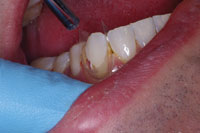
Figure 16. APA preparation demonstrating minimal tissue trauma. |
Figure 17. Isolation was secured and a matrix was applied on each tooth (Contour Strip [Ivoclar Vivadent]) as they were restored. |
 |
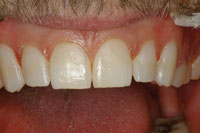 |
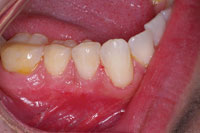
| Figure 18. Immediate photo of the finished lower right quadrant restorations, showing little gingival trauma and natural emergence profiles. |
Figure 19. Close-up photo of the completed cervical restorations. |
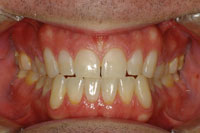 |
| Figure 20. Retracted view of the final restorations at 18 months. |
This case is much more complex than the ones presented above. It illustrates how APA can be used to provide beautiful restorations in a severely broken down mouth (Figures 12 to 14). This particular patient presented to our office with an extraordinary fear of dentistry and consequently had not been to the dentist in 15 years. The intraoral examination revealed active caries and a heavily worn dentition with severe attrition and erosion. Nutritional and preventive dental counseling were provided, and a stabilization restorative plan was embarked upon. The active carious lesions were removed, and the patient’s desire was to cover over the deep erosions to homogenize the anterior tooth color. APA preparations once again removed active lesions only (Figures 15 and 16), and then the areas of anterior aesthetics were surface-textured with APA to improve the bond. These prepared areas were then isolated with Con-tour Strips (Ivoclar Vivadent), and restored one by one (Figure 17). The Contour Strips allowed us to matrix and isolate simultaneously, creating a very biocompatible emergence profile within the periodontal sulcus. This surface that is fabricated against the mylar Contour Strip results in a surface that is smoother than even well-polished composite. Before and immediate postoperative photos (Figure 18) demonstrate that minimal tissue trauma was imparted using these techniques, and that a biomimetic result was accomplished very conservatively (Figures 19 and 20).
CLOSING COMMENTS
These 3 cases help to illustrate a few of the clinical uses of APA. In the author’s opinion, with dentistry moving toward minimally invasive and biomimetic procedures, APA is poised to become the treatment of choice in cases like those presented in this article. The recent modifications to the older dry-delivery systems make it easier for practitioners to accept and use this modality with confidence. Identifying cavitated lesions early and treating them with minimally invasive preparations and composite resin restorations will create beautiful, long-lasting biomimetic restorations.
Dr. Malterud, a 1983 graduate of the University of Minnesota School of Dentistry, practices general dentistry in St. Paul. He is a faculty member of the University of Minnesota Continuing Dental Education Department. His practice focuses on comprehensive cosmetic dentistry, incorporating minimally invasive dental procedures. His passions in these areas have allowed him to lecture internationally. He trained at the Pankey Institute and completed the entire curriculum of its educational continuums on comprehensive dentistry, and he has received Mastership in the AGD. He is an active member of the ADA and its state and local components, and he is currently the immediate past president of the Minnesota AGD. He chairs the AGD’s Dental Education Council. He can be reached at mark@drmalterud.com.
Disclosure: Dr. Malterud reports no conflicts of interest.