The American Association of Endodontists (AAE) recently sent a letter to all state governors and health departments urging them to recognize endodontists as emergency healthcare providers when N95 masks and other personal protective equipment (PPE) are distributed.
The AAE noted that endodontists treat dental emergencies that become life-threatening if untreated. Also, the AAE said, endodontists engage in emergency care in high-aerosol environments and mitigate the burden on medical and hospital emergency departments.
For example, a 12-year-old boy from Baltimore named Diamonte Driver died after an untreated infected molar resulted in an abscess that spread to his brain in 2007.
In 2011, a 24-year-old Cincinnati resident died of an untreated tooth infection. And in 2017, a 26-year-old truck driver died of a tooth infection that had only been treated with pain medication.
The conditions that led to these deaths are the very same emergency conditions that endodontists treat effectively in the dental practice, the AAE said, as dental emergencies become life-threatening emergencies if they aren’t treated properly.
According to the ADA’s definition, endodontics is concerned with the morphology, physiology, and pathology of the human dental pulp and periradicular tissues, the AAE said, specifically the treatment of diseases and injuries of the pulp and associated periradicular regions.
“Put simply, endodontists treat pulpal conditions often produced as a result of untreated decay, often exhibiting with abscessed pulp, and often experienced as severe pain,” said Keith V. Krell, DDS, MA, MS, president of the AAE.
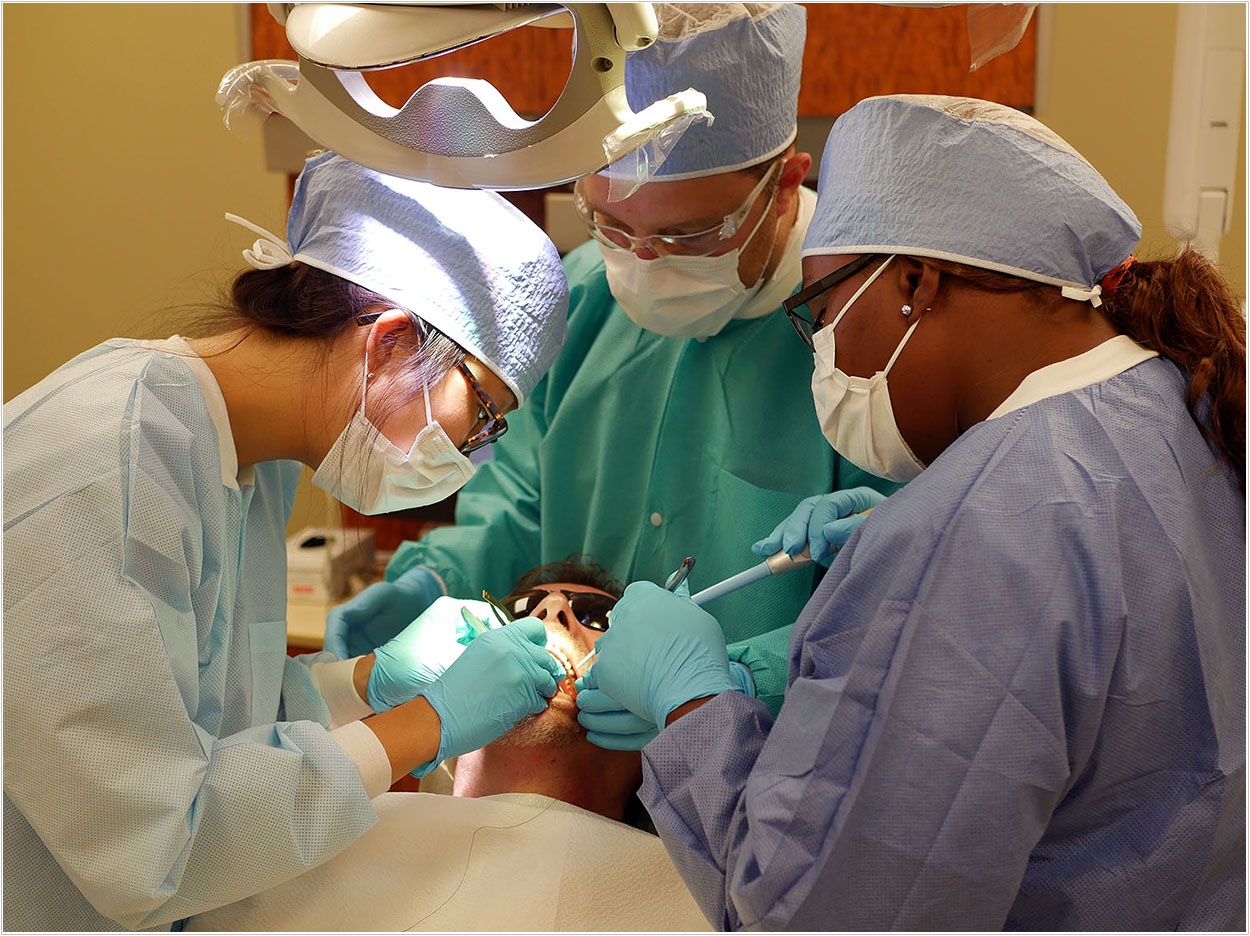
Endodontic treatment includes surgical and nonsurgical therapies, both of which require the use of a high-speed drill that creates aerosols that can transmit the COVID-19 coronavirus, according to the Centers for Disease Control and Prevention.
“These aerosols are necessary in emergency dental care but require N95 masks for protection of the dentist and staff,” Krell said.
The AAE said that there were 2.2 million emergency department visits for dental issues in the United States in 2016, or one every 14 seconds, according to the ADA. The top two dental conditions resulting in emergency department visits in 2009 were dental decay (41.8%) and abscesses (37.4%), which are most effectively treated by endodontists, the AAE said.
“Today, with the need for emergency departments to focus their limited resources on the COVID-19 pandemic, avoidable dentally related emergency department visits are especially problematic,” Krell said.
“Dentists, especially endodontists, must serve as the first point of contact for dental emergencies if we are collectively going to minimize the burden on the limited capacity of emergency departments,” Krell said.
“Moreover, by helping patients with dental emergencies through telehealth or emergency office visits that respect social distance, these patients avoid becoming agents and recipients of transmission of the coronavirus in emergency departments where social distance is a challenge,” Krell said.
“For the reasons explained here, it is critical for ensuring the safety of patients and for protecting valuable emergency department resources and staff that endodontists be included as essential emergency healthcare providers for distribution of necessary N95 masks and other PPE,” Krell said.
Related Articles
Q&A: COVID-19 Treatment With AAE President Dr. Keith V. Krell
AAE Guidelines Separate Emergency and Non-Emergency Treatment
Endodontics Emergencies Peak During COVID-19 Outbreak












