Kenneth A. Malament, DDS, MScD, discusses his professional expertise and candid perspectives related to all-ceramic dental material options.
Dr. Malament, in addition to your position as a clinical instructor at Tufts University School of Dental Medicine (TUSDM), and even more importantly to our GP readers, you are a busy clinician. How does being a practicing Board Certified Prosthodontist and postgraduate continuing education professor shape your view of dentistry?
Dr. Malament: I have been a clinical professor in the Department of Postgraduate Prosthodontics at TUSDM for more than 25 years and teach a course each week on the clinical management of simple and complex prosthodontic care. This course provides a significant exposure to modern material science, with an emphasis on dental ceramics. As a past president of the American Board of Prosthodontics, I have had the privilege of examining candidates since 2001 and learning from many of the most skilled and knowledgeable individual examiners in prosthodontics and dentistry. My mentors and professors always emphasized that continued learning and teaching was the most important part of a career. I have practiced prosthodontics since 1977 and created a full dental laboratory with master dental technologists, and I can clearly say that I have learned more from my dental laboratory team than I have taught them as a practitioner. One may believe that a specialist in dentistry should be an expert on the cutting edge of knowledge in materials and techniques; this thought would be incorrect. The graduate prosthodontic education taught and examined by the board is set by the ADA and is based on experienced, excellent clinical care. The education emphasizes treating patients with comprehensive care and with an interdisciplinary approach. We teach our residents the value of teamwork, and I believe prosthodontists everywhere are the most knowledgeable and talented dental professionals to consult and help guide GPs with complex care.
 |
 |
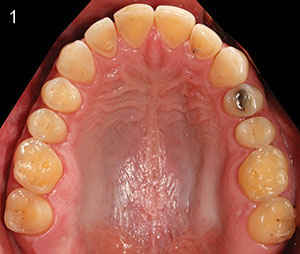
| Figures 1 and 2. The patient presented unhappy with the aesthetic results and smile. A loss of vertical dimension due to erosion and wear had occurred over the years. |
 |
 |
| Figures 3 and 4. Partial-coverage tooth preparations. |
 |
 |
| Figures 5 and 6. Partial-coverage lithium disilicate (IPS e.max [Ivoclar Vivadent]) restorations 2 weeks after being luted to the teeth after enamel acid etching, GLUMA dentin placement, and dentin bonding. |
I created a database 36 years ago of more than 7,600 all-ceramic restorations with 27 different confounding variables. Besides writing papers on the survival of the different all-ceramic restorations, I learned from my own experience what may be successful and under what conditions the restorations may survive best. I also learned from Professor Sigmund Socransky that to develop meaningful information, one must study at least 500 restorations over 5 years to have reasonable statistical significance.
To further elaborate on what shapes my vision of care today and tomorrow, I should add that I attend many academy meetings where I learn much from my colleagues’ work and their observations. In my dental career, nothing has shaped me more than continuing education.
 |
| Figure 7. The patient presented unhappy with her aesthetic results and smile. Over the years, there had been loss of vertical dimension of occlusion (VDO) due to wear. |
What are some of the clinically relevant trends that you are seeing related to current dental material options?
Dr. Malament: Today, there is more of an emphasis on ceramics than ever before, as they do not degrade over time in the same manner that resin restorations can. The ever-improving CAD/CAM technologies allow dentists to create restorations more quickly and with improving precision. Digital impressions are accurate, and the data has the potential to create a restoration that will fit more precisely than restorations made with any of the different impression materials, stone dies, investment materials, and casting techniques. As always, proper tooth preparations and any required tissue retraction must be acceptable. With each passing year, CAD/CAM technology is improving with the introduction of more precise milling machines that can self-calibrate and replace worn drill bits automatically. CAD/CAM restorations can be milled today in blocks or in discs where many restorations can be made, and the material costs are not significant. There is work being done now to develop a lithium disilicate disc, and, if this can be accomplished, the use of this excellent and etchable glass ceramic will have an even greater use in clinical dentistry. Removable, complete dentures are made today with CAD/CAM technology, as well as millable metals or forms that can be layered and sintered into metal. Since 3-D printing continues to develop, in time, this technology will allow for the creation of master casts and dies, wax patterns, resin restorations, and maybe even zirconia all-ceramic restorations. Great work is being done in this area. Today, most restorations are made in milling centers or by small labs that can afford the new and excellent CAM/CAM machines. It is important to remember that technology is improving in this field at a logarithmic rate and, due to wear, new machines are required to be purchased within only a few years. It must be remembered that great dentistry is about the dental materials applied more than it is about the technology that is used in the process. CAD/CAM or 3-D printing can make the process easier and faster, but there will always be the highest need for great technologists. These individuals will design restorations and custom finish them to the most optimal aesthetic results. Those results and the long-term survival of these restorations will always define “success.”
 |
| Figure 8. Maximum Interdigitation Position (centric occlusion) at a decreased VDO. |
 |
| Figure 9. Laterotrusive (working) excursion. All the posterior teeth are hitting in all excursive movements. |
Based upon your own clinical experience, in terms of long-term observations and data gathered in your own practice, can you please share your latest findings related to all-ceramics? What is the relevance of your latest findings to the everyday GP reading this interview?
Dr. Malament: As I have described, the database I created 36 years ago studying different all-ceramic restorations, and the effects that 27 different, confounding variables may have on long-term survival, have a profound impact on the way scientists and dentists understand how ceramics survive over a long time.1-5 To date, the most successful ceramic is the IPS e.max lithium disilicate glass ceramic material (Ivoclar Vivadent). This glass ceramic is the most versatile and can function and survive even at thicknesses of 0.5 mm as a complete- or partial-coverage restoration. It has excellent light absorption and reflection properties that can be enhanced with fluorapatite veneering ceramics that are unlikely to chip in function. The ceramic can be translucent or more opaque, allowing technicians, if they desire, to stratify color to develop in depth color that is stable over time.
In an article in the Journal of Prosthetic Dentistry titled “Ten-Year Survival of 1960 Pressed e.max Lithium Disilicate Monolithic and Bilayered Complete Coverage Restorations,”5 it was concluded that e.max pressed lithium disilicate restorations can survive successfully: “Seven failures were recorded for the 1960…units placed, providing a [crude percent] failure estimate of 0.003. The 7 failures occurred during a cumulative monitoring period of [5,112.6] years, providing an estimated failure risk of 0.14% per year.”5 The e.max survival statistics clearly demonstrate there is minimal chance of fracture with restorations anterior to the bicuspids and that molars have a very low percentage of fracture as well. “The failure rate for complete coverage restorations for each tooth in both arches….[finds that] regardless of mandibular or maxillary placement, incisor restorations had no failures.”5 There was no statistically significant difference in the survival of acid-etched, pressed e. max restorations related to type of monolithic or bilayered physical structure, tooth position, sex, or age.5
The ceramic has a glassy component, allowing it to be etched and then silaned to create a good attachment between tooth structure and the ceramic. This is important because it limits micromotion that can break the seal and have a restoration come out and also minimizes crack growth that may fracture the ceramic.
 |
 |
| Figure 10. Maxillary full-coverage tooth preparations. | Figure 11. A digital pantograph (Cadiax) was used to record the patient’s posterior determinants and to set a fully adjustable articulator. The registration allowed a visualization of the condylar movements and timing. |
 |
 |
| Figure 12. After the new VDO had been determined and captured in the full-mouth provisional restoration, the dimension was maintained using a leaf gauge. The guided centric relation (CR) was recorded. | Figure 13. A full white wax-up can either be made by hand or digitally fabricated. This is tried in to examine tooth position, shape, length, and occlusal planes. Most important is that this is tried in so that the patient can feel and preview the form to approve and give us permission to finish the work. Wax, as opposed to resin, can be very easily adjusted. |
What is the importance of selecting the right dental material options and in understanding and perfecting the appropriate techniques (ie, preparation design, isolation, bonding-cementation, finishing-polishing, and occlusion) and skill levels to predictably achieve long-term clinical success with all-ceramic materials?
Dr. Malament: Each clinical condition requires different considerations as to what dental material will work best to provide structural support, aesthetics, and resistance to fracture and chipping. All dental restorations, whether gold, metal-ceramic (ie, PFM), or all-ceramic, need to be checked with a fit checker to ensure proper contact and marginal seal with the tooth. With individual crowns, lithium disilicate ceramics have become the standard of excellence as they resist fracture and are etchable and very aesthetic. Metal-ceramic crowns are more expensive and labor intensive. Depending on the level of artistic and technical ability, they may be aesthetically more unpredictable, and feldspathic porcelain has a clear history of chipping. Crowns made with zirconia have improved significantly, but its physical properties are dependent on the quality of the zirconia used. There are many off-label and poor-quality zirconia ceramics sold, chosen due to low prices, and these materials should not be used. Dentists should know who manufactured the zirconia that they will use and some of its physical properties. Quality zirconia disks are, by themselves, not expensive. Ceramics produced by isostatic pressing from major manufacturers should always be considered first, as these will perform significantly better. The color properties of the new generation zirconia ceramics (such as IPS e.max ZirCAD Prime [Ivoclar Vivadent]) have fused together 3Y-TZP that has high strength with 5Y-TZP that, although lower strength is more translucent, allows the production of an all-ceramic with excellent aesthetics and strength. The 5Y-TZP has 650 MPa strength and will resist fracture. By blending the 2 zirconia forms to create a more translucent form, the use of zirconia is more prevalent today than ever before. The problems remain that many restorations are coming out after cementation and, furthermore, the time to dislodgment is unpredictable.
 |
| Figure 14. Resin-bonded, individual full-coverage e.max restorations, principally monolithic with micro-layering done for aesthetic effects, in CR and in protrusive. |
 |
| Figure 15. The completed restorations in CR. |
With complex bridges and implant reconstructions, zirconia made with a CAD/CAM titanium substructure is an excellent and predictable restoration. Some laboratories cement implant components to zirconia frames, and, with this poor technique, there is a probability that they can be dislodged and the zirconia suprastructure can fracture. Metal ceramics with complex care may still be the standard of care.
Although it is desirable to use individual, all-ceramic crowns for aesthetic reasons, in some patients, contact areas open up, teeth continue to move down occlusally, and—in the worst scenario—individual teeth snap off at the gingiva. One of the tenets of placing a periodontal prosthesis is to splint together many, if not all, teeth together. This minimizes tooth mobility and many of the problems just stated. Understanding advanced prosthodontics and periodontics is most helpful in guiding the choice of dental materials.
 |
| Figure 16. The completed restorations in protrusive. |
 |
| Figure 17. Maxillary and mandibular occlusal views of the final lithium disilicate full-coverage restorations. |
When we observe preparations in dental laboratories, we are still not witnessing the expected growth in minimally invasive dentistry, despite the fact that quite a few modern composite and all-ceramic materials allow for more thoughtful prep design that saves tooth structure. Knowing that, along with placing a fairly high number of partial-coverage lithium disilicate restorations, what are your comments and recommendations to the majority of clinicians who seem to find it easier or “safer” to deliver full-crown restorations instead of more minimally invasive partial-coverage restorations?
Dr. Malament: Minimally invasive dentistry has been around a very long time. For generations, the gold onlay was the ideal standard of care for most operative dentistry. A gold onlay strengthens a tooth and does not degrade over time, and it is an ideal restoration to improve occlusion. The ceramic veneer, assuming the bonding of the ceramic is mostly to enamel, has been a significant restoration since the 1970s. With the etchable lithium disilicate ceramic, partial-coverage restorations can more easily and predictably be a part of modern treatment.6 A great advantage of this type of restoration, because it is etchable, is that the bond and cement strength to both dentin and enamel is a significant improvement over zinc phosphate or conventional glass ionomer cements. These restorations reinforce the tooth complex without extensive occlusal coverage as was required for gold restorations. The survival statistics now being reviewed and processed for a new journal submission are excellent. Dental school faculties are not teaching the onlay preparation as effectively as was done in the past; therefore, clinicians are not comfortable doing them in their practices. Another point is that many teeth considered for minimally invasive dentistry already have large existing restorations and decay. Many of these teeth would be better treated with full-coverage restorations to minimize tooth fractures.
Dental technicians are perfecting the lithium disilicate veneer restoration to improve the color properties by building more translucency into a thin veneer. These veneers are being created using CAD/CAM technology. Lithium disilicate ceramic veneers are easier to fabricate for the technician, are etchable and significantly stronger than feldspathic ceramics, and are now becoming the standard.
With all the growth in materials, techniques, and evolving treatment modalities, we are expecting young dental graduates to learn so much more and in the same amount of time as we did 20 to 30 years ago. Is the time currently devoted to the average dental curriculum enough to adequately prepare to be a knowledgeable and high-quality dentist? What role could academia play in better preparing young graduates to take an evidence-based and more minimally invasive approach to dental care? Do you feel we may reach a point, as with physicians, that dental residencies become a required step in the dental career?
Dr. Malament: The undergraduate and graduate dental curricula are very challenged to provide the best and most meaningful education to our students. What is taught is set by an ADA Council and by the educators themselves. As so much is changing every year, and because new equipment is expensive and wears out with time, the challenge to educate students about cutting-edge technologies is nearly impossible. As I have previously mentioned, all educators today emphasize the importance of continuing education and finding mentors who can guide persons through all the many, and often complex, questions that will arise.
References
- Malament KA, Socransky SS. Survival of Dicor glass-ceramic dental restorations over 14 years: Part I. Survival of Dicor complete coverage restorations and effect of internal surface acid etching, tooth position, gender, and age. J Prosthet Dent. 1999;81:23-32.
- Malament KA, Socransky SS. Survival of Dicor glass-ceramic dental restorations over 14 years. Part II: effect of thickness of Dicor material and design of tooth preparation. J Prosthet Dent. 1999;81:662-667.
- Malament KA, Socransky SS. Survival of Dicor glass-ceramic dental restorations over 16 years. Part III: effect of luting agent and tooth or tooth-substitute core structure. J Prosthet Dent. 2001;86:511-519.
- Malament KA, Socransky SS. Survival of Dicor glass-ceramic dental restorations over 20 years: Part IV. The effects of combinations of variables. Int J Prosthodont. 2010;23:134-140.
- Malament KA, Natto ZS, Thompson V, et al. Ten-year survival of pressed, acid-etched e.max lithium disilicate monolithic and bilayered complete-coverage restorations: performance and outcomes as a function of tooth position and age. J Prosthet Dent. 2019;121:782-790.
- Malament KA, Margvelashvili M, Natto ZS, et al. Ten-year survival of pressed, acid-etched e.max lithium disilicate monolithic and bilayered partial coverage restorations: performance and outcomes as a function of tooth position. J Prosthet Dent. In press.
Dr. Malament received his DDS degree from the New York University College of Dentistry and a specialty certificate and Masters (MScD) degree from the Boston University Henry M. Goldman School of Dental Medicine. He has a full-time practice limited to prosthodontics in Boston that includes a dental laboratory with master dental technicians. Dr. Malament is past president of the American Board of Prosthodontics, a clinical professor at Tufts University, and a course director in Tufts University’s postgraduate department of prosthodontics. He is past president of the Academy of Prosthodontics, Greater NY Academy for Prosthodontics, and Northeastern Gnathological Society, and is currently the vice president of the American Academy of Esthetic Dentistry. He is a Fellow of the American College of Prosthodontists, the Academy of Prosthodontics, the Greater New York Academy of Prosthodontics, and the Northeastern Gnathological Society. He is also an active member of many dental organizations, including the International College of Prosthodontists, the American Academy of Fixed Prosthodontics, the American Academy of Esthetic Dentistry, the Academy of Osseointegration, the Northeastern Prosthodontic Society, and the American Equilibration Society. Dr. Malament was on the research and development teams for 2 well-known ceramic products and developed instrumentation used in clinical practice. He is a consultant to 3 journals, has published significantly in the dental literature, and has frequently lectured about prosthodontic topics involving ceramics, implants, and periodontics. He can be reached at kenmalament@mac.com.
Disclosure: Dr. Malament reports no disclosures.
Related Articles
Reflections on Modern Dental Ceramics
Removing All-Ceramic Restorations With Lasers
All-Ceramics and Tooth Alignment Create a New Smile











