INTRODUCTION
There are very few milestones in my career that changed my entire trajectory and method of practice. Designing my own cases in-house digitally would have to be at the top of that list. I can think of numerous reasons why having a full in-house digital workflow will benefit a practitioner, his or her patients, and the lab/ceramist. This article will take you along my path.
As patients present to our practice for cosmetic consults, they often have an idea of what they want their smiles to look like but cannot explain things in dental terms. They usually have no idea of the steps it will take to achieve a result and are often surprised. And as the practitioner, I have to explain that it will take me some time just to develop a plan and figure out how many teeth might be involved. Having digital design software in-house gives me the tools to show patients proposed outcomes chairside at the consultation appointment. This is a huge benefit from the traditional methods of sending a case to a lab to design and having a patient wait weeks to see a mockup.
With current software, patients have the ability to see a digital rendition of their smiles and what the results will look like, depending on how many teeth they decide to incorporate, within a few minutes. This increases patient communication and, in turn, patient acceptance, all while reducing turnaround time and cost. But what does it take to simplify this process and complete a digital design chairside at the consultation appointment? All that is needed to showcase the design is a full-face photo (Figure 1) and an intraoral scan of the patient (Figure 2). The software will merge both (Figure 3) to begin the design process.

Figure 1. A full-face photo of the patient was captured and brought into exocad.
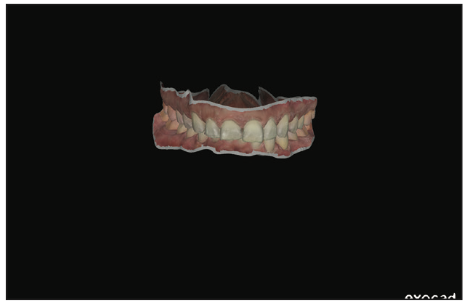
Figure 2. An intraoral scan of the patient was captured and brought into exocad.
Figure 3. The intraoral scan and full-face photo of the patient were aligned and merged together in exocad software to facilitate facially driven treatment planning.
CASE REPORTS
Case 1
A 43-year-old patient arrived at my practice after she completed Invisalign treatment (Align Technology) at an orthodontic office (Figures 4 and 5). She was unhappy with her smile and was interested in veneers.
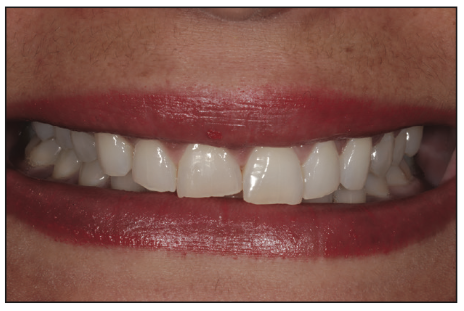
Figure 4. Close-up smile photo of the patient’s then-existing condition.
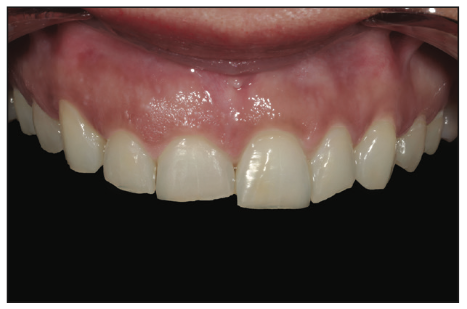
Figure 5. Magnified photo of the patient’s existing teeth, preoperatively.
She was focused on the 6 anterior teeth, but I realized that more teeth might have to be involved in order to obtain what I thought would create the best outcome. With a simple full-face photo and an intraoral scan of the patient (iTero [Align Technology]), I merged the data into the digital design software (exocad) and instantly began to show the patient what her smile could look like. It was emphasized that the result depended on the number of restorations. The software showed the 2 options in 2D and 3D side by side (Figure 6).
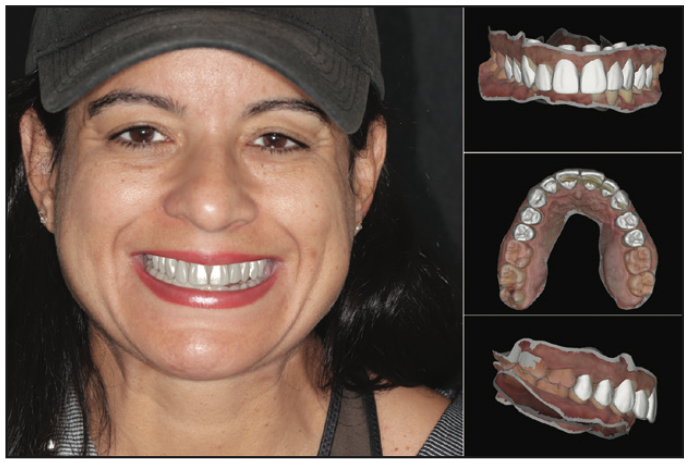
Figure 6. Initial digital wax-up design superimposed on the patient’s face to help plan proper proportions, midline, and overall aesthetics.
In the past, we had to create a preliminary wax-up, which took a lot of time by both me and, often, a laboratory. There were also costs involved that would be passed on to the patient. The reduced cost is not the only big win in providing in-house digital designing at the practice. The patient ultimately decided on 10 veneers based on her digital design. But the excitement with digital didn’t end there. Utilizing digital in-house provides numerous advantages. To start, the software has the ability to toggle between different tooth shapes with a click of a button to see which shape best suits a patient’s facial structure (Figure 7). You can also see the thickness of the proposed restorations to visualize how much tooth structure will need to be prepared for desired results (Figure 8). This often can be a huge driving force for the patient to seek orthodontics prior to the treatment to put teeth in an ideal position that will allow for a purely additive case. There was a discrepancy in this patient’s gingival heights, so it was noted that aesthetic crown lengthening would help facilitate a better outcome in this case. The teeth were virtually crown-lengthened first, and an aesthetic crown-lengthening guide would be designed and 3D printed to ensure the proper contours on the day of surgery (Figure 9).
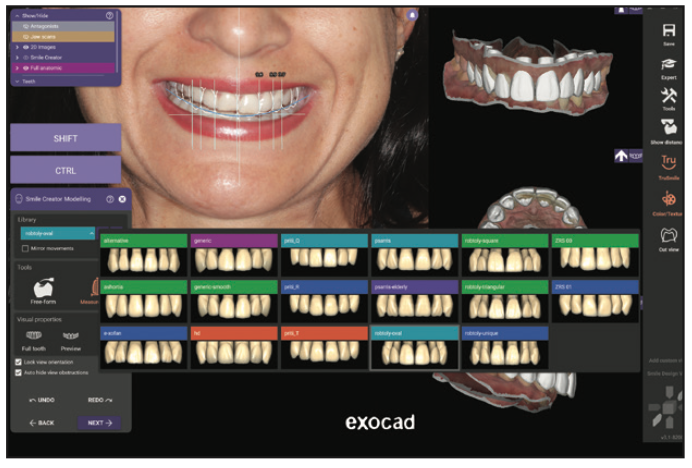
Figure 7. Utilizing exocad’s extensive tooth libraries to select shapes that best suited the patient’s facial structure and desired results.
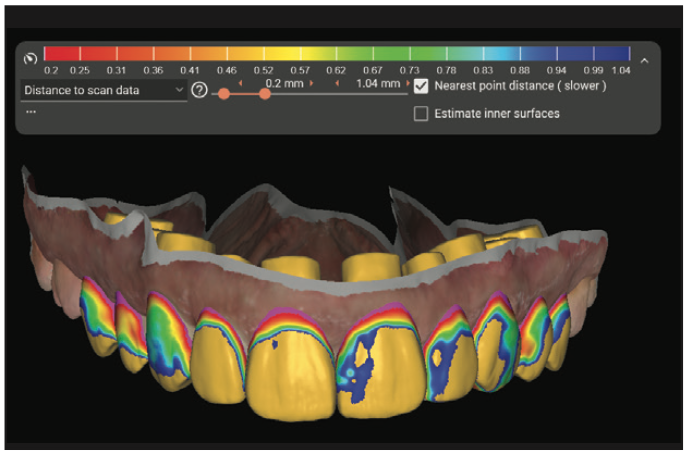
Figure 8. The software provides a user with the ability to see the thickness of the wax-up (and, therefore, final restorations) to determine how much tooth structure will need to be prepared for each case.
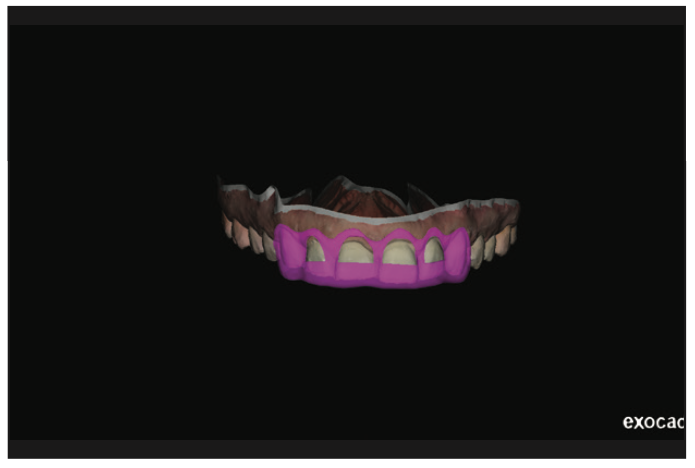
Figure 9. Virtual crown lengthening was completed, and a crown lengthening guide was designed and fabricated to utilize on prep day.
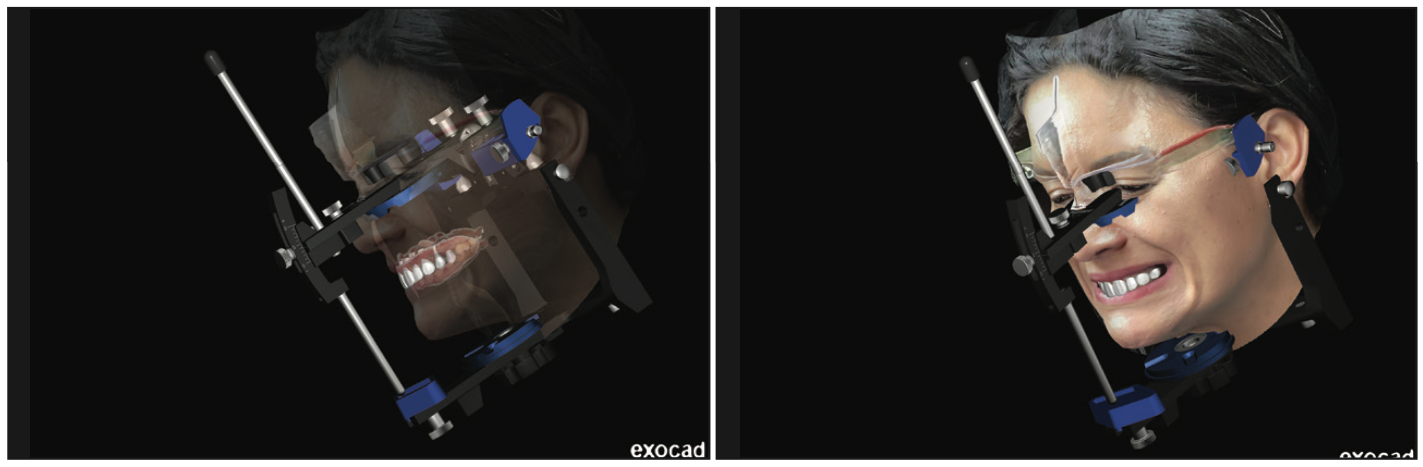
Figure 10. A face scan and virtual articulator were utilized to ensure proper orientation of the wax-up as well as adaptation to occlusion.
Once the wax-up teeth are set on the jaw scan, the next ideal step is to mount them on a virtual articulator. This ensures that the dynamic movements of the patient can be respected in the design. At this time in planning, if there are concerns with alignment, facial orientation, and side profile view, a face scan can be created (Figure 10). With this multilayer approach, we have the ability to ensure optimal accuracy, correct canted smiles, and compensate for any jaw alignment discrepancies.
Using the design software, you can once again show the final outcome to the patient and, when approved, fabricate the definitive wax-up (Figure 11). This wax-up can be converted into numerous beneficial components to facilitate the ease of prep day. It is utilized to create a prep guide to ensure only the minimal tooth structure is reduced when actually preparing (Figure 12). The software can then take the wax-up and create a model for shell temporaries (Figure 13). This workflow, which can be done in under an hour, is an extraordinary time saver. Proceeding on this digital path, the shell temporaries were printed on a SprintRay Pro55 printer utilizing Bego Varseo Resin (Figure 14) and were perfectly applied in a short time. The predetermined gingival architecture and the predesigned preps made this all happen. Before this workflow, there were a few unknowns, and a lot of time was spent creating the temporaries with matrices and flowing in temporary resins. There were also long finishing times.
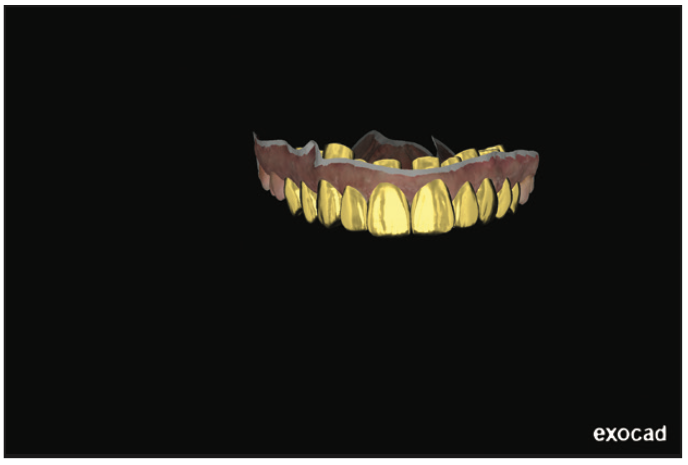
Figure 11. The final wax-up design.
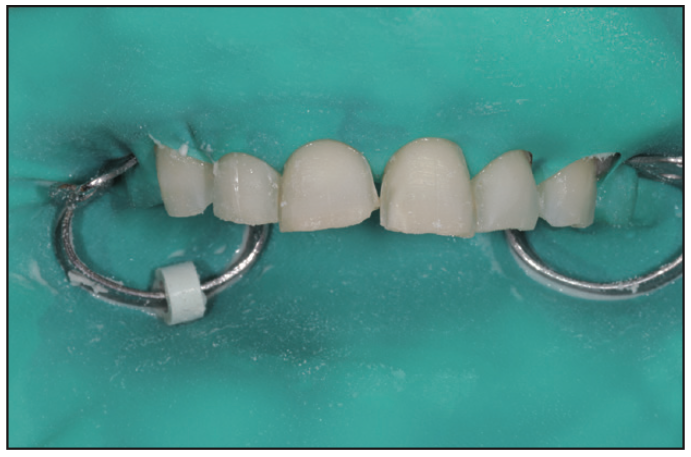
Figure 12. Minimal preparations were completed based off the design and reduction guide.
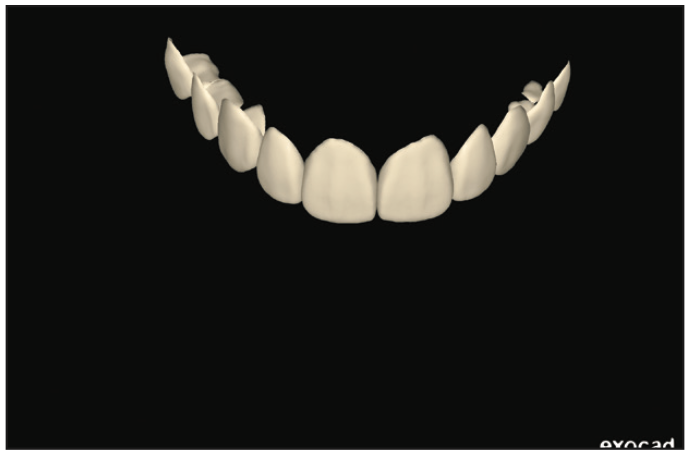
Figure 13. The final wax-up design was converted into shell temporaries digitally.
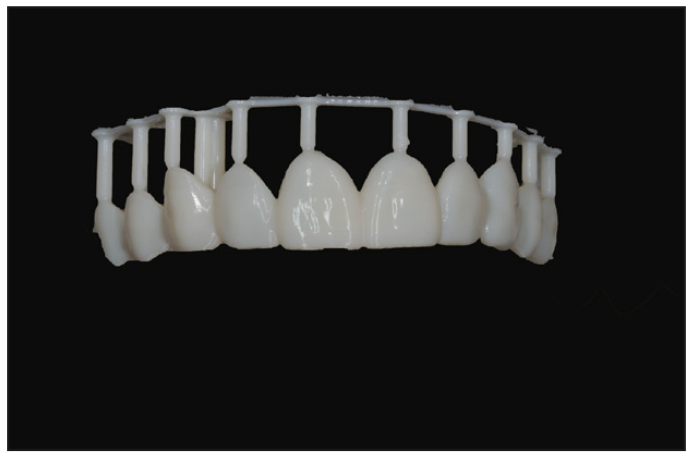
Figure 14. The printed shell temporaries were printed on a Pro55 (SprintRay) using Bego Varseo Resin.
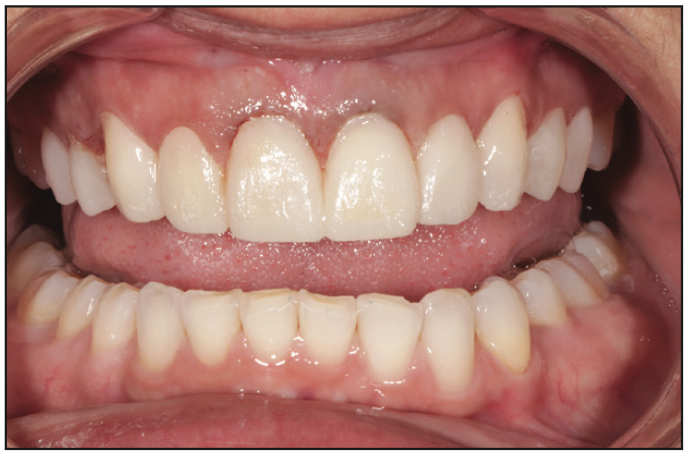
Figure 15. The printed shell temporaries were cemented in the mouth at the end of the prep appointment.
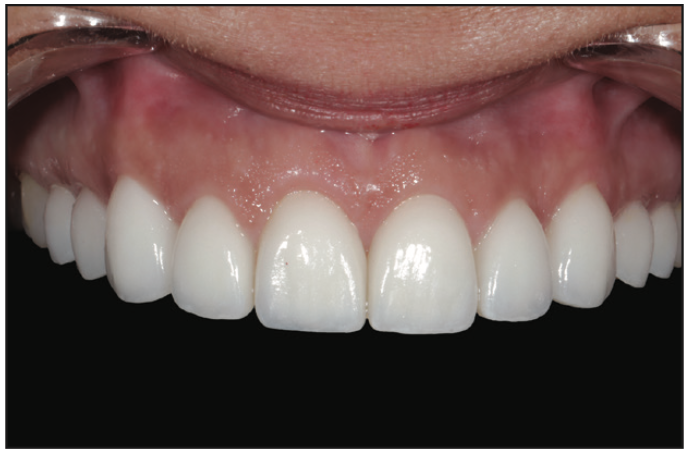
Figure 16. The final ceramics that were replicated off of the digital wax-up.
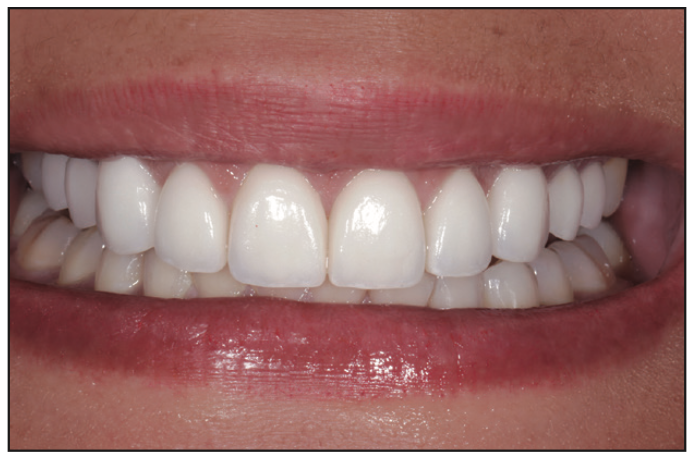
Figure 17. The patient’s end results of 10 ceramic veneers.
Once the patient left with shell temporaries (Figure 15), the entire design project created was sent to the ceramist to be replicated into porcelain veneers. This increases lab communication exponentially as well as the accuracy of the final ceramics in being replicas of the approved temporaries. The final ceramics were inserted (Figures 16 and 17) and approved by the patient—all while reducing turnaround time, increasing patient and lab communication, and reducing the cost to the patient.
Case 2
The notion that digital design software is reserved for large cosmetic cases or full-mouth reconstructions couldn’t be further from the truth in my practice. In fact, I would be bold to say that I utilize design software at my practice more so for my everyday dentistry cases than for smile makeovers. No matter what type of dentistry we are inclined to practice, whether it be cosmetic or “bread-and-butter” or implant dentistry or orthodontically and airway-driven, we can all relate to the patient who shows up to our office from an emergency call with a broken front tooth. These types of emergencies no longer intimidate me. Whether it’s going to be a direct or indirect restoration, the ability to confidentially mirror a central tooth to match its contralateral tooth has become one of my favorite digital workflows.
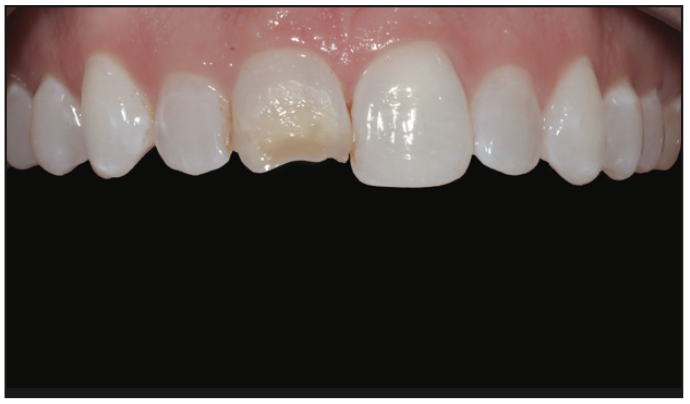
Figure 18. A magnified view of a patient’s fracture as she presented at office.
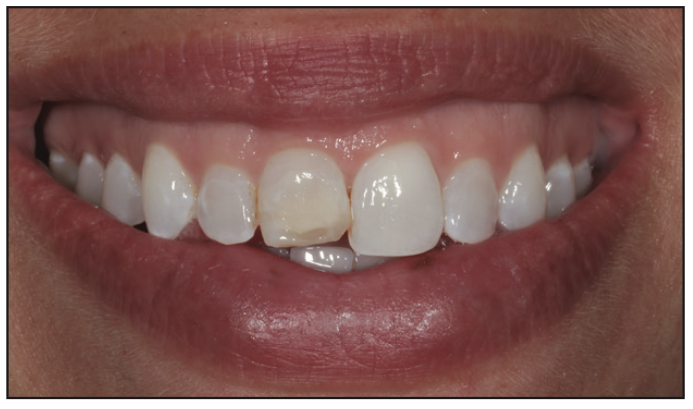
Figure 19. Patient’s pre-op photo.
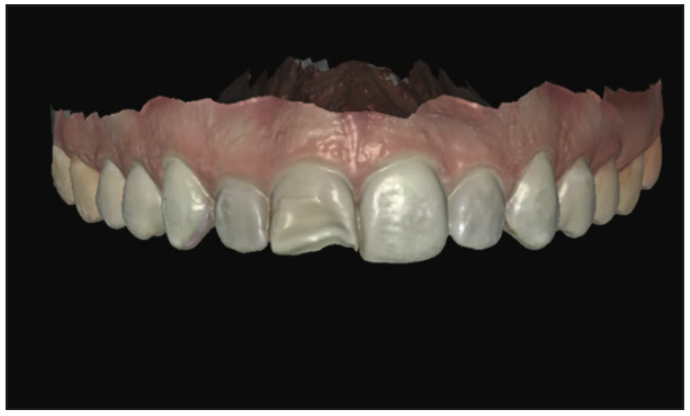
Figure 20. An intraoral scan of the patient was captured and brought into exocad.
A new 26-year-old patient called our practice on a Monday morning, frantically stating that she broke her front tooth (Figures 18 and 19). If she had been a current patient at our practice, I would have been able to utilize an existing intraoral scan of her teeth to 3D print a cast. We started by scanning her existing teeth in their condition with our iTero 5D scanner (Figure 20) and taking that scan straight to exocad design software.
Once the scan was in the software, the contralateral tooth (No. 9) was mirrored digitally into the No. 8 position (Figures 21 and 22).
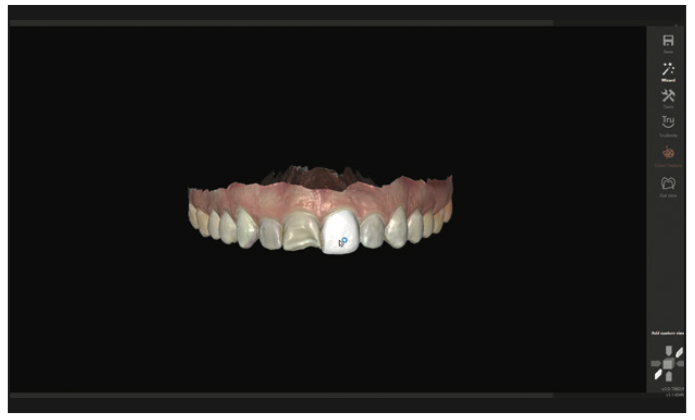
Figure 21. Tooth No. 9 was digitally copied in exocad.
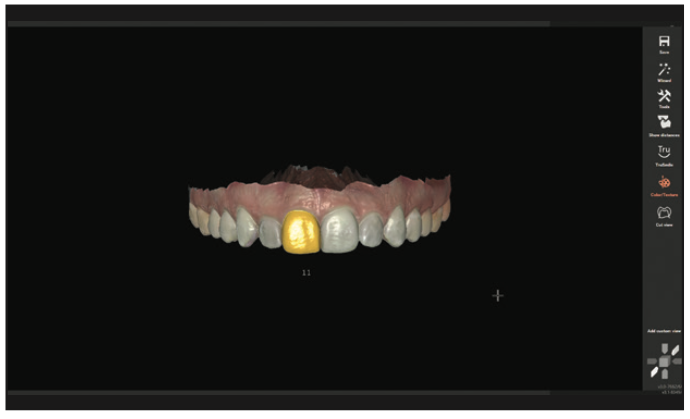
Figure 22. The tooth No. 9 digital copy was then mirrored in the No. 8 position.
A model then takes 40 minutes to 3D print utilizing Die and Model Tan 2 Resin on a Pro95 S printer (SprintRay) (Figure 23). The patient can opt to wait or return for the restorative part of the procedure. The cast was utilized to create a lingual matrix out of PVS to aid in a lingual shelf for a direct composite (Figure 24).
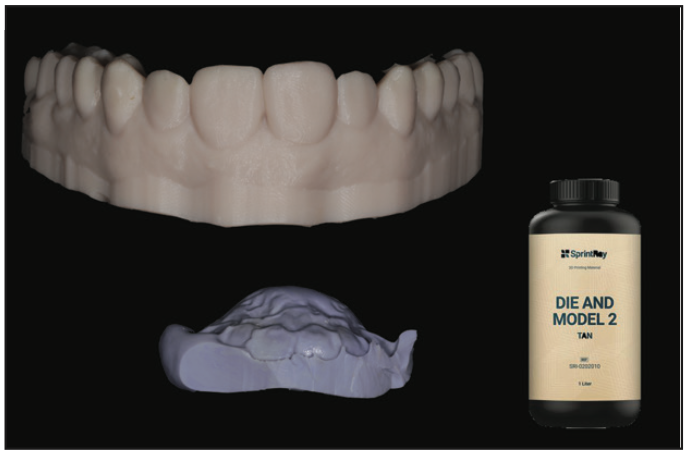
Figure 23. A model of the new wax-up was 3D printed.
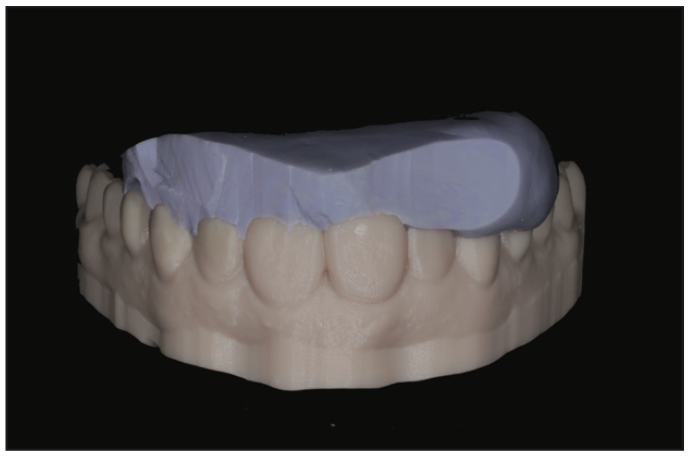
Figure 24. A PVS lingual matrix was fabricated against the wax-up model.
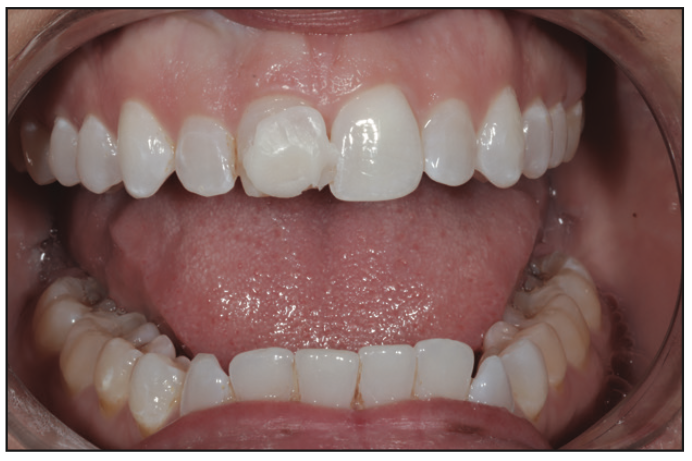
Figure 25. Composite was placed to evaluate the thickness of the dentin shade needed to mask the discolored tooth.
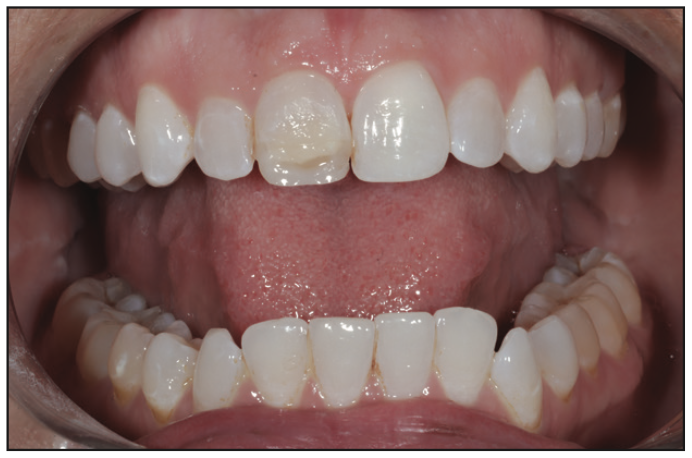
Figure 26. The initial lingual layer was placed on the PVS matrix and then transferred to the tooth to establish the framework of the shape.
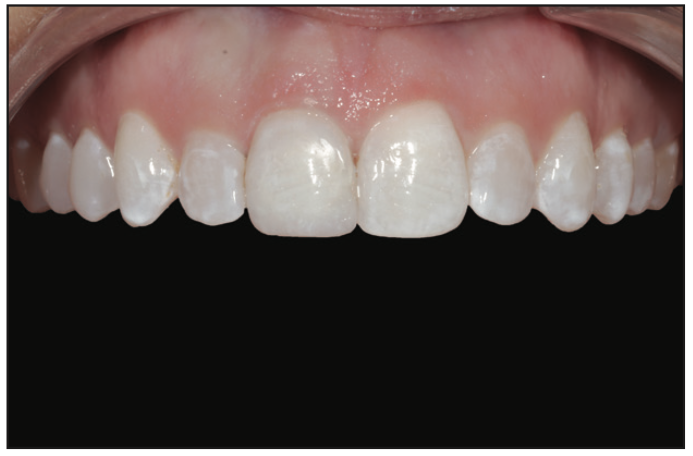
Figure 27. The completed case with IPS Empress Direct composites (Ivoclar) and Cosmedent stains.
A shade-match photo was taken to determine the enamel and dentin shades. In this case, I was evaluating the thickness of the dentin shade needed to mask the discolored tooth (Figure 25). Next, a PrepStart microabrasion unit (Zest Dental Solutions) was utilized. The tooth was selective-etched (enamel only) with 30% to 40% phosphoric acid. A bonding agent, Adhese Universal (Ivoclar), was then applied throughout the tooth surface. The initial lingual layer was placed on the PVS matrix to provide the framework for the composite and then placed on the tooth and bonded (Figure 26). The case was completed utilizing a layered composite method with IPS Empress Direct composites in shade B1 dentin and Bleach enamel (Ivoclar), along with white and low-chroma stains (Cosmedent) (Figure 27). The restoration was polished, and she left extremely happy and stated that it looked like her original smile again.
CONCLUSION
I have found that the implications for digital are broad and hugely outweigh the benefits of the traditional analog methods. When done properly, it can provide huge wins for the patients, practitioners, and laboratories. I believe so much in the impact that digital has had in my office that I decided not to hide my digital lab in the back like we are accustomed to but display it front and center when patients enter our office (Figure 28). This has produced another level of patient engagement and interest in the technology and services I am providing daily in my practice. With all that digital has to offer, it is rapidly becoming the key player in modern day dental practices.

Figure 28. Dr. Tadros’ digital consultation room that also houses all her digital machines and computer software.
ABOUT THE AUTHOR
Dr. Tadros owns a boutique, fee-for-service private practice in South Florida. She is a Kois Center graduate and an accredited member of the American Academy of Cosmetic Dentistry. She holds Fellowship status in the AGD as well as in the International Congress of Oral Implantologists. She is a key opinion leader and lecturer for digital dentistry, including for exocad, SprintRay, and VHF. Outside of her practice, she is the founder of Exocad Elite, a training continuum, where she teaches a series of workshops to other dentists and staff on digital designing and workflows. She will also be teaching 2 upcoming courses at the Kois Center on Digital Dentistry. She was selected as one of the Top 50 Global Digital Women of the Year (2022) as well as Digital Educator of the Year (2022). She can be reached at dianatadrosdds@gmail.com.
Disclosure: Dr. Tadros reports no disclosures.











