
A member of the Dental Resource Program of America’s ToothFairy, Holly Jorgenson, RDH, of Let’s Smile, Inc., delivers a virtual presentation on oral health to students in Minnesota. Although more children received educational services than in years past, less received screenings, sealants, and fluoride varnish applications due to restrictions on school-based dental programs.
Last month, the World Health Organization (WHO) acknowledged that preventive dental care and the treatment of tooth decay are vitally important when they added fluoride, glass ionomer cement, and silver diamine fluoride to their list of essential medications. Why would the WHO be concerned about oral health when it seems that COVID-19 should be the focus?
According to a recent study conducted by the British Dental Association and published in the British Dental Journal, after excluding older or obese subjects, Covid patients with poor oral health are more likely to experience severe and/or longer lasting symptoms. It stands to reason then, that improving oral health is part of the strategy to reduce the impact of Covid. The problem is, people who are at higher risk of developing severe cases of Covid–people of color and those living below the poverty level–also face extra barriers to access dental care.
Before the pandemic, school-based dental programs were proven to be an effective strategy to help children living in low-income homes and rural communities get preventive care and connect them and their families to a dental home. Research shows that screenings, sealants, fluoride varnish, and oral health education received through school-based programs reduced cavities by 50%. As the pandemic lingers on, the children who benefited from these school-based programs are facing barriers to care once again.
“Most people dealt with delays in dental care for a short time while dental offices were shut down or only offering emergency treatment. We’re 19 months into this pandemic and many of the children who depend on school-based dental programs are still waiting in many cases,” said Jill Malmgren, Executive Director of America’s ToothFairy, a nonprofit organization that provides resources for safety-net dental clinics and organizations delivering preventive services to underserved communities.
The organization has been keeping a close eye on the impact the coronavirus shutdowns have had on children who need dental services the most, and the community organizations that are struggling to provide the care they need.
Through their Dental Resource Program (DRP), 64 nonprofit dental clinic members in 25 states receive dental supplies and equipment, educational materials, and grants to support the delivery of care. 82% of DRP members provide care through school-based programs.
“42% of our member safety net clinics report that the majority of their patients receive dental care at school–that’s as many as 450,000 kids,” Malmgren explained. “It’s only a snapshot of safety-net clinics across the U.S. At this time, only 18% of our members have access to schools at the same level that they had before Covid.”
According to a survey of its member clinics, America’s ToothFairy reports that 63% of its members have some access to schools, but not at the same level as before. While 14% are still not allowed to visit schools to provide essential dental services. Clinics with unrestricted access were more likely to be in rural areas in states like South Carolina, Minnesota, and West Virginia, while those in more urban areas in states like California are more likely to have limited access or are completely cut-off from school settings.
Even in states like Missouri, where clinics can access students at school, coordination has become more complicated.
“The biggest challenge is that the school nurses are overburdened with Covid-related problems, such as contact tracing and managing quarantines,” one clinic responded in the survey. “Our capacity is already reduced, plus we are trying to do more to lessen the burden on nurses. Several of our larger districts have chosen not to participate in our school-based screening program this year, which will significantly reduce the number of students receiving screenings and care coordination as well as preventive fluoride treatments.”
Overall, since 2019, America’s ToothFairy has seen a 25% reduction in the number of kids who received fluoride varnish and sealants, and a 27% drop in the number of kids who were screened for emergent dental needs through their program partners–numbers that do not sit well with Ms. Malmgren.
“While this has been a very challenging and frustrating time, we are encouraged by the creative ways our Dental Resource Program member clinics have found to reach kids with oral health education through virtual presentations and small-group instruction,” Malmgren pointed out. “In fact, last year our members reached more kids than ever mostly due to educational outreach. Oral health education is important, and is a major component of our mission, but it’s not a substitute for dental services. Kids still need screenings and preventive treatments.”
Another obstacle for school-based programs is concern from school personnel and parents that receiving dental treatment at school is too risky during the pandemic.
“Our first school event is scheduled for late October,” a clinic in Minnesota noted in their survey response. “We are anticipating a lower participation rate… We have sent communication home with families to share the safety measures we have set in place to assure families know that dental care is safe to receive in a school setting.”
It is important to note that dental care providers were already practicing strict infection control protocols before Covid. The clinics that oversee school-based programs have implemented more precautions in addition to their existing safety protocols such as the use of additional PPE (which can be difficult to procure) and restricting the number of students who receive services in the same spaces.
“We have always implemented safety first while treating patients; however, we had to implement a few changes to go that extra mile to make everyone feel safe,” a member from Missouri reported. “Prior to Covid, our teams could go inside the schools to retrieve children from their classrooms. Now many schools would prefer that their staff assist in this area. The number of children that we would normally service daily has changed to continue practicing the social distancing requirements.”
To overcome these additional barriers, DRP members are going out of their way to deliver care to kids in need. A clinic located in Vermont cannot enter schools but has worked with the school system to coordinate transportation to bring students to their facility during school hours.
Another from New Jersey delivered “Tooth Brushing Stations” kits to schools for children with developmental disabilities, to reinforce daily oral hygiene routines for the students and their aides. Still others reported moving their services to Head Start programs or The Boys and Girls Club locations.
Malmgren is confident their program members could do much more with more resources.
“We are inspired every day by the optimism and dedication of our member clinics,” she said. “They are working with reduced budgets and staff, limited access to supplies and PPE, roadblock after roadblock, and still they come up with such creative work-arounds because they care so very much about these kids. They could do exceedingly more, and we could do so much more for them,with support from the dental community.”
For more information about America’s ToothFairy and the resources they provide to safety-net clinics and community oral health organizations, visit AmericasToothFairy.org.
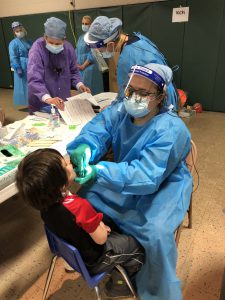
A student from Central Community College Dental Hygiene program in Hastings, NE applies sealant to a young child’s teeth.
ABOUT THE AUTHOR
Jan Badger is the Communications Manager for America’s ToothFairy. She can be reached at communications@ncohf.org.












