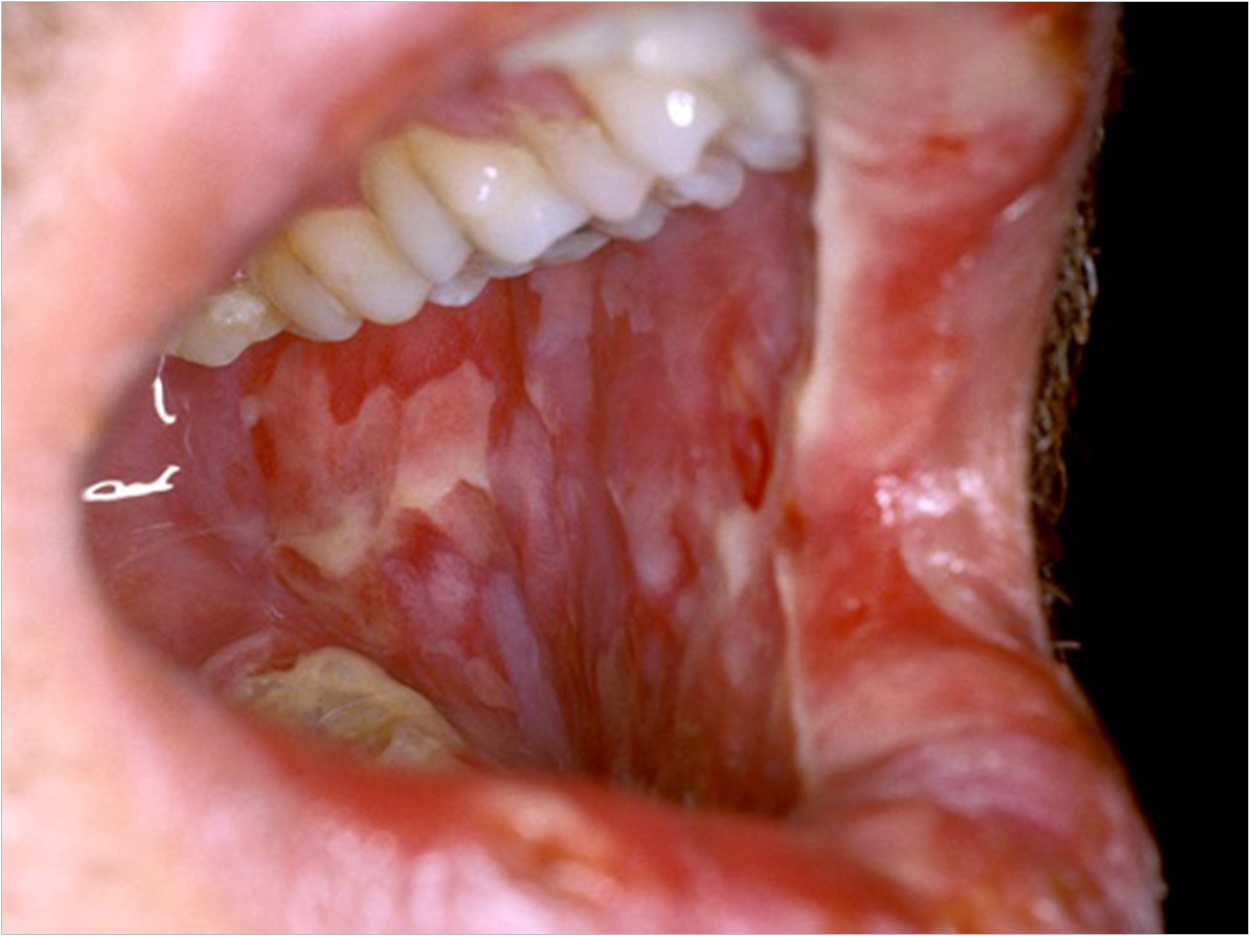
Researchers at the University of Connecticut School of Dental Medicine say they are a step closer to understanding the root causes of oral mucositis that occurs after chemotherapy, with direct evidence that the oral microbiome could influence its clinical course.
Oral mucositis, a common side effect of chemotherapy, is triggered by chemotherapeutic drugs breaking down the mucous membrane lining the mouth. This breakdown induces the painful lesions.
“Oral mucositis due to chemotherapy can impact the delivery of optimal cancer treatment,” said Patricia Diaz, DDS, MS, PhD, associate professor in the Department of Oral Health and Diagnostic Sciences and the study’s lead investigator.
“These uncomfortable oral lesions can be associated with clinically significant pain in patients and impact their ability to eat. In extreme cases, a patient’s risk of bloodstream infections is elevated, and they are at increased length and cost of hospitalization,” said Diaz.
While this chemotherapy complication has not been widely researched, it has been suggested that the oral microbiome plays a role in inducing the responses that lead to mucositis. Diaz’s study tracked 49 patients receiving treatment for cancers not located in the mouth during one chemotherapy cycle.
The researchers found that oral mucositis is associated with detrimental changes in the oral microbiome. Patients who developed the most severe oral mucositis lesions showed suppression of beneficial mouth bacteria and outgrowth of harmful ones.
However, it remains unknown if the oral microbiome itself is disrupted during the chemotherapy. Further research studies are needed to understand which specific microbiome components are detrimental and in what manner they affect the oral mucosa’s ability to withstand a chemotherapy challenge, the researchers said.
The findings also can shed light on new preventive approaches to stop the lesions from developing, the researchers said. As of now, some evidence suggests that an antimicrobial mouth rinse such as chlorhexidine has some benefits in preventing chemotherapy-associated mucositis, but Diaz says more research is needed to develop more effective preventive measures.
“We need to design more targeted preventive strategies aimed at these detrimental microorganisms,” said Diaz. “Since chemotherapeutics are the primary cause of mucosal injury, it is also likely that these microbiome-targeted therapies need to be combined with other treatments to prevent cell death and inflammation at the oral mucosa.”
The study, “Chemotherapy-Induced Oral Mucositis Is Associated With Detrimental Bacterial Dysbosis,” was published by Microbiome.
Related Articles
Topical Anesthetic Improves Oral Mucositis Pain Treatment
Timing of Radiation Treatment Can Improve Oral Mucositis Symptoms
Grant to Support Research Into Light Therapy for Treating Oral Pain












