The Clinical Rationale Behind Fully Guided Third Molar Tooth Bud Ablation
Clinical management of third molars has remained largely unchanged for the past 100 years. Practitioners’ only choices are to surgically intervene prophylactically or address issues after symptoms become evident. In the presence of pathology, the latter approach is painful and costly. Unfortunately, both approaches pose considerable surgical risk. As a result, general practitioners refer more than 80% of third-molar surgeries to specialists.
With the evolution of guided implant placement, dentists have an opportunity to reimagine how they manage third molars. Recent research by TriAgenics describes a new preventive care procedure called fully guided third-molar tooth bud ablation (3TBA). A one-minute, minimally invasive thermal treatment, 3TBA has been shown to irreversibly induce third-molar agenesis in extensive animal trials.
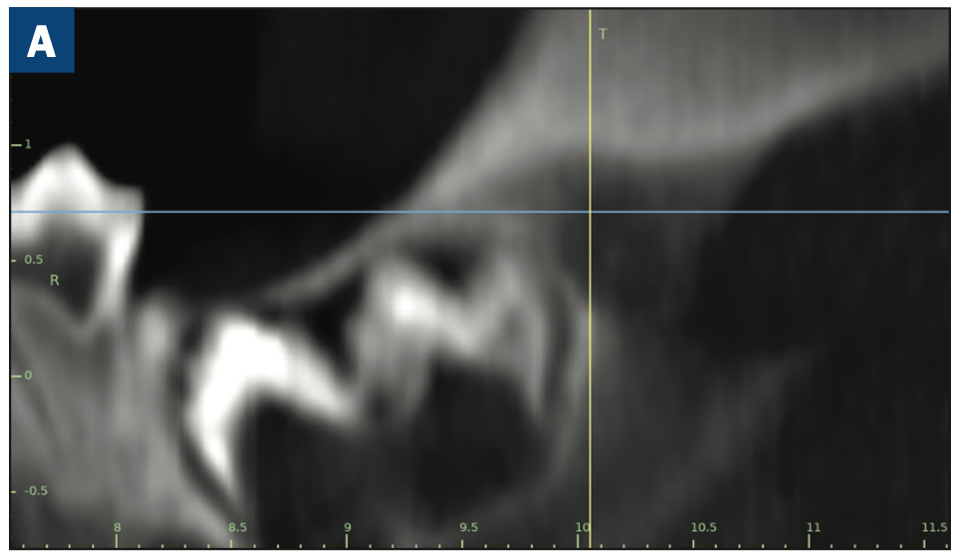
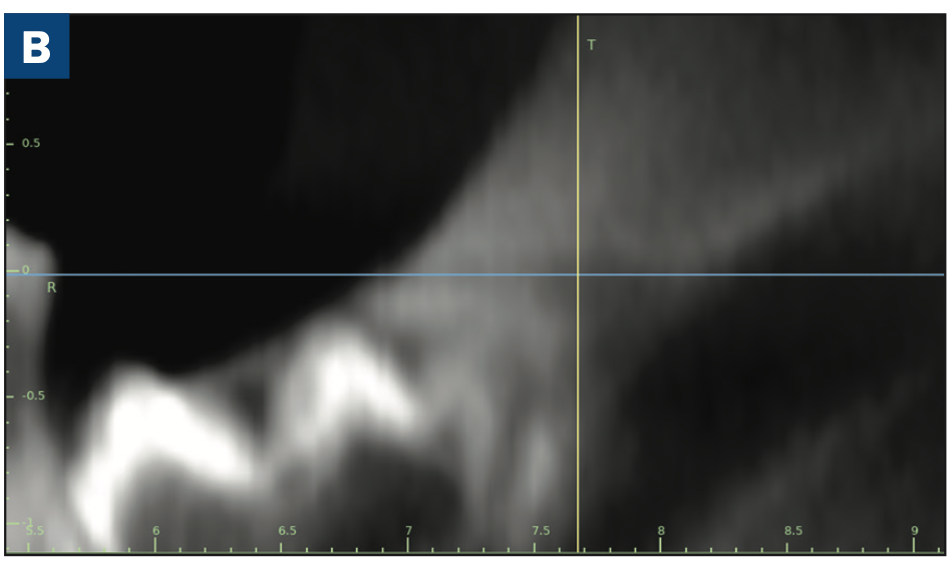
As reported in the April 2023 issue of Journal of Oral and Maxillofacial Surgery, complete molar agenesis was achieved in 100% of TriAgenics’ 3TBA procedures using micro-ablation treatment cycles of 60 seconds or less. Radiographic and histological assessment indicated no presence of treated tooth bud tissue 28 days following 3TBA treatment. Figure 1a shows a typical one-day, pre-operative image of a targeted tooth bud. Figure 1b shows 28-day, post-operative healing results. Histological evaluation at 28-days post 3TBA treatment confirms the presence of complete bony infill with trabecular new bone growth and no detectable viable tooth bud tissue.
Based on animal trials, the 3TBA procedure in humans will be as fast and simple. Designed for children ages 6 to 12, fully guided 3TBA involves accurate positioning of a 3TBA micro-ablation handpiece using a 3TBA guide. Positioning of the 3TBA micro-ablation handpiece tip is predetermined with 0.1 mm planning resolution. The full-arch 3TBA guide is first seated onto patients’ teeth. The disposable 3TBA micro-ablation handpiece is then fully seated into the 3TBA guide, as shown in Figure 2. If an osteotomy is required, a 2-mm bone drill can be used to enable complete insertion of the 3TBA handpiece.
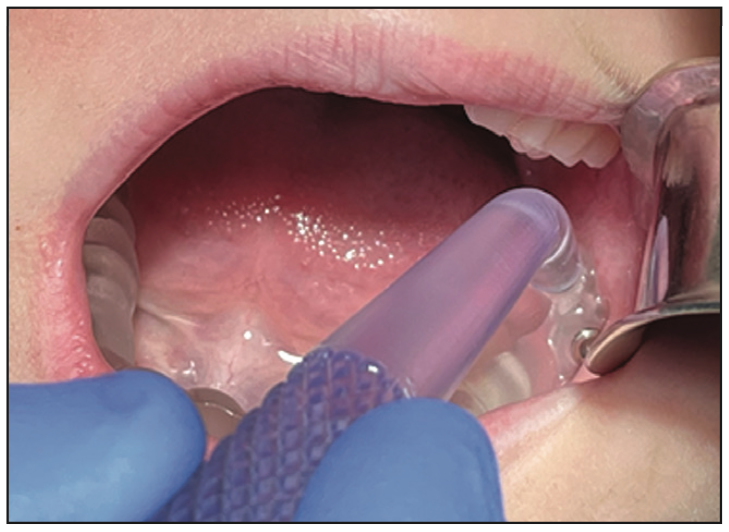
Figure 2. The mock 3TBA handpiece inserted into a full-arch 3TBA guide as part of a pilot human trial.
A predetermined microwave energy dose of one minute or less in duration would be delivered through the 3TBA handpiece using a proprietary microwave generator. After delivering the energy dose, the 3TBA handpiece is immediately removed and treatment is complete. The only post-op evidence of treatment in animals was a small puncture (Figure 3), which was not detectable 7 days following 3TBA treatment.
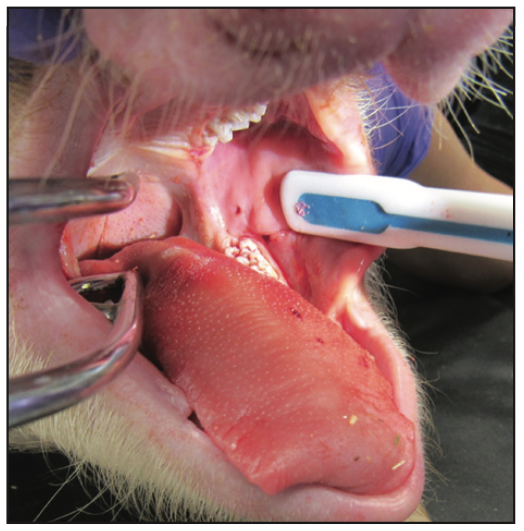
Figure 3. Immediate post-op view showing the small punc- ture made by the 3TBA micro-ablation handpiece in a porcine animal study.
To obtain complete molar agenesis, the diameter of the spherical zone of ablation is predetermined with 0.1-mm planning resolution. Accurate positioning of the 3TBA handpiece, combined with precise control of the ablation zone diameter, results in thermo-coagulation of the entire third molar tooth bud with no meaningful damage to tissues outside the bony crypt of the tooth bud (Figure 4).
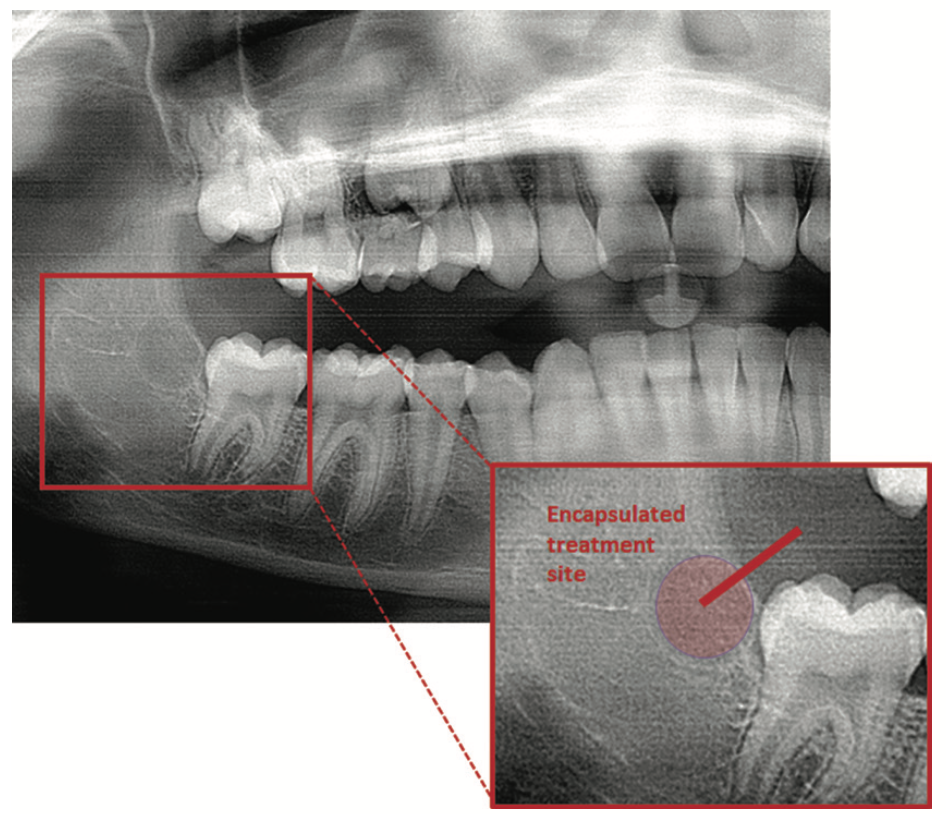
Figure 4. The predetermined spherical zone of ablation results in complete thermocoagulation of the tooth bud with no meaningful damage to tissues outside the bony crypt of the tooth bud.
The most exciting aspect of minimally invasive 3TBA will be dramatically improved outcomes, which are simply unattainable using conventional surgical means. Based on animal trial data, there will be no recovery time nor any of the many painful complications that normally follow surgical removal of third molars. The zone of tissue ablation has no exposure to the oral cavity. As a result, there will be no possibility of painful dry sockets and there will be virtually no risk of immediate or delayed onset infections.
For more information, visit the website located at triagenics.com.