INTRODUCTION
Dental caries have long represented a significant oral health issue for children and adults. However, in the 1980s, the prevalence of coronal caries in children steadily and gradually declined within segments of the population, following the implementation of fluoride supplements and toothpastes, increased public oral health education, and application of dental sealants.1 Since they were first utilized in dental offices in the 1970s, dental sealants have been effective in caries prevention.
Sealants, which act as a barrier and are typically applied onto the premolars and molars where decay is most likely to develop, may be resin-based or glass ionomer cement. They have been proven to be effective in preventing pit and fissure caries,2 as well as caries on the occlusal surfaces of permanent molars and in high-risk cases.3 Throughout the years, sealants have been implemented into public programs as a way to reach children of low socioeconomic status who are most susceptible to—and often have high instances of—caries. Studies regarding retention rates and clinical benefits of community sealant programs conducted by county health departments determined that children who received sealants had a 71% successful retention rate and considerable protection from occlusal decay up to the fifth grade.4 Other studies indicated that sealants are more effective when placed in patients with established risk factors for occlusal caries,5 while other studies suggested that knowledge gaps remained regarding the costs and benefits of sealing low- versus high-risk populations.6-8
That may partially explain why the success of early sealants was a gray area. A cost-benefit and cost-effectiveness analysis regarding preventive dental programs within a hypothetical community examined 4 popular dental preventive programs—community water fluoridation, school water fluoridation, weekly school-based mouthrinses, and school-based sealants—to evaluate maximum caries reduction during a 20-year period. The analysis revealed that community water fluoridation was the most cost effective and beneficial, while school-based dental sealants resulted in negative net benefits.9
Further, some past studies evaluating the use and effectiveness of placing sealants on first and second permanent molars in children during a 5-year period indicated that sealant placement was only minimally beneficial in preventing carious lesions.5,10 Therefore, there has been a lack of agreement amongst clinicians regarding the benefits and use of caries-preventive agents, including sealants.11
The low incidence of dental sealant use is a direct result of a lack of public awareness and patient education, as well as a disproportionate reimbursement for sealants by third-party insurers.12 In 1988, the average percent of patients 18 years old and younger receiving dental sealants was only 18.7%, and many dental patients were not receiving sealants at all.13 This trend continued throughout the years, even though the ADA widely advocated the use of dental sealants as a recommended component to maintaining good oral health.2
In fact, children who do not receive sealants have greater odds of developing carious lesions and needing restorative dental care in the future, costing the healthcare system more money in the long term.14 Perhaps that explains why research regarding caries risk assessment and the use of preventive techniques in children aged 6 to 18 years found that dental sealants and in-office fluoride are the most frequently used caries preventive regimens.11
Currently, new and improved dental sealants are available that are beneficial and cost-effective. They reflect an evolution in which sealants have advanced to become more cost-effective, and research now suggests that properly placed and retained sealants can decrease the occurrence of carious lesions and prevent restorative costs.
Characteristics of Dental Sealants
The earliest generations of sealants were vulnerable to fissures, bubbles, and failure to adapt to dentition, which contributed to earlier wear. As a result, they required replacement over time, which is an essential component of caries prevention to avoid bacterial infiltration that can lead to carious lesions. Early sealants typically lasted 6 months to a year.15
First- and second-generation sealants demonstrated a low viscosity and a high resistance to flow, causing the material to run over the margins of the tooth and other surfaces. These sealants were usually clear and resembled caries in subsequent x-rays. Additionally, early generations of sealants were also moisture incompatible and required application in a dry environment to prevent contamination and sealant failure caused by a weakened sealant bond.
Third-generation sealants showed improvements but were still problematic. These sealants were more viscous and easier to handle and, as a result, the sealant remained on the tooth surface until it was light-cured. However, research showed that LED or halogen lights were insufficient for curing 2-mm-thick opaque or high-filler-loaded sealants, potentially causing microleakage and insufficient microhardness.16
Adhesion is one of the most important features of a dental sealant. Studies have shown self-adhesive sealants do not have as defined an etching pattern as etch-and-rinse adhesives.17 A pretreatment conditioning protocol with an appropriate acid is necessary to obtain adequate penetration of a sealing material.18 Newer generations of sealants can be cured in a moist environment and do not require complete drying of the tooth surface after etching. This is possible due to the hydrophilic agents that today’s sealants contain.
Today, dental professionals have sealant materials that are easy to apply, long-lasting and durable, radiopaque for subsequent dental procedures, and contain fluoride. The process of sealing teeth has been simplified with the introduction of syringes with disposable tips that allow clinicians to apply the sealant directly to the pits and fissures of the tooth surface. Sealants today can last up to 5 or 10 years if regularly cared for after application.15 This is facilitated by modern technology that permits dentists to view risk factors and monitor sealant application and overall retention.19 Additionally, contemporary sealants are radiopaque, making dental procedures easier; radiolucent materials could mimic caries in subsequent radiographs and, therefore, be problematic.
INTRODUCING A NEW SEALANT WITH HYDROPHILIC CHEMISTRY
UltraSeal XT hydro (Ultradent Products) is a highly filled (53%) and light-curable pit and fissure dental sealant. This sealant is also radiopaque, methacrylate based, and thixotropic. It also contains diurethane dimethacrylate, triethylene glycol dimethacrylate, and methacrylic acid.
UltraSeal XT hydro’s adhesive properties increase the bond strength of the material to the enamel, enhancing marginal retention and reducing microleakage. The thixotropic nature of the material, combined with its hydrophilic chemistry, prevents sealant failure by chasing moisture deep into the pits and fissures of the tooth on a microscopic level. This prevents moisture-related sealant failures common with earlier generations of hydrophobic sealants. Additionally, the traditional step of pretreating teeth with a drying agent is eliminated, resulting in faster and more efficient procedures.
The sealant’s fluorescent properties enable visual verification of the sealant’s margins under a UV black light, making it easier to verify and view marginal retention at the time of placement and at subsequent examinations. The chemical composition contains and releases fluoride, so no additional treatments are necessary. UltraSeal XT hydro is available in 2 shades: Opaque White (clear) and Natural (tooth-colored material), and is applied using a syringe and Inspiral Brush tip (Ultradent Products).
Unlike previously introduced sealants, UltraSeal XT hydro seals to and is retained by dentition for long-term results, similar to its UltraSeal XT plus predecessor.20 Additionally, it is free of bisphenol A (BPA), as tested by an independent third-party laboratory that confirmed levels of less than 0.00000% BPA.21
CASE REPORT
Diagnosis and Treatment Planning
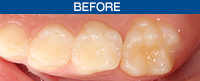
A 9-year-old female presented with deep pits and fissures. Upon examination, it was determined that application of a hydrophilic sealant would be the best course of preventive treatment (Before Image).
 |
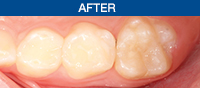 |
| Before Image. Preoperative photo. | After Image. Postoperative photo. |
Clinical Protocol
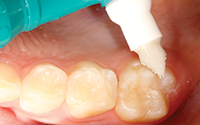
The brush tip was attached to the Ultra-Etch etchant syringe containing 35% phosphoric acid solution. The Inspiral Brush tip was attached to the UltraSeal XT hydro syringe for later application of the sealant. The fissures of the teeth were cleaned using a microetcher (Ultradent Products) (Figure 1). The selected teeth were isolated with cotton rolls in order to avoid saliva contamination (Figure 2).
 |
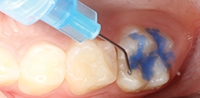 |
| Figure 1. The tooth was cleaned with plain pumice. | Figure 2. Ultra-Etch 35% phosphoric acid solution (Ultradent Products) was placed for 20 seconds. |
 |
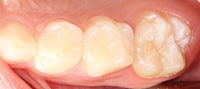 |
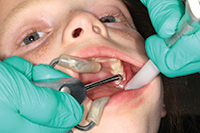
| Figure 3. The teeth were thoroughly rinsed and dried. | Figure 4. Properly etched teeth should have a frosty appearance. |
 |
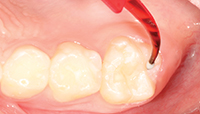 |
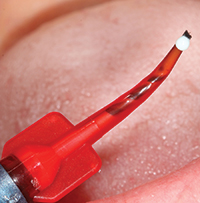
| Figure 5. A small drop of UltraSeal XT hydro (Ultradent Products) was expressed. | Figure 6. Application was done using a painting action, followed by light agitation with the brush tips. |
 |
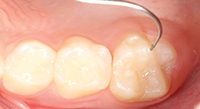 |
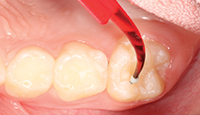
| Figure 7. Resin was applied to deep fissures (avoid pooling) and light-cured. | Figure 8. Margins were checked and the occlusion adjusted, as needed. |
Etchant was applied to the fissures of the teeth for 20 seconds (Figure 3). The teeth were thoroughly rinsed with a water spray unit and dried with an air-abrasion unit (Figure 4). It was necessary to repeat the etch-and-rinse step in cases where sodium bicarbonate was being used.
Prior to applying the sealant, a small drop of UltraSeal XT hydro was expressed onto the Inspiral brush tip (Figure 5). In order to prevent premature polymerization of the dental sealant, the overhead light was redirected, and the sealant was applied using a painting action, followed by light agitation (Figures 6 and 7).
The sealant was light-cured using the VALO LED curing light (Ultradent Products) on standard mode for 10 seconds. It is recommended that clinicians and patients wear UV protective eyewear when the sealant is light-cured to prevent injuries (Figure 8).
The sealant margins were examined with a black light lens (VALO Black Light Lens [Ultradent Products]) to visually verify marginal retention. The occlusion was then examined and appropriately adjusted (After Image).
IN SUMMARY
Sealant placement remains an integral component of preventive dentistry. UltraSeal XT hydro is an innovative dental sealant that is easy to use, cost-effective, and clinically proven to help prevent the formation of cavities in pit and fissure areas.
References
- Rozier RG, Beck JD. Epidemiology of oral diseases. Curr Opin Dent. 1991;1:308-315.
- ADA Council on Access, Prevention and Interprofessional Relations; ADA Council on Scientific Affairs. Dental sealants. J Am Dent Assoc. 1997;128:485-488.
- Ahovuo-Saloranta A, Hiiri A, Nordblad A, et al. Pit and fissure sealants for preventing dental decay in the permanent teeth of children and adolescents. Cochrane Database Syst Rev. 2008 Oct 8;(4):CD001830.
- Dorantes C, Childers NK, Makhija SK, et al. Assessment of retention rates and clinical benefits of a community sealant program. Pediatr Dent. 2005;27:212-216.
- Dennison JB, Straffon LH, Smith RC. Effectiveness of sealant treatment over five years in an insured population. J Am Dent Assoc. 2000;131:597-605.
- Mejàre I. Indications for fissure sealants and their role in children and adolescents. Dent Update. 2011;38:699-703.
- Feigal RJ, Donly KJ. The use of pit and fissure sealants. Pediatr Dent. 2006;28:143-150.
- Feigal RJ. The use of pit and fissure sealants. Pediatr Dent. 2002;24:415-422.
- Niessen LC, Douglass CW. Theoretical considerations in applying benefit-cost and cost-effectiveness analyses to preventive dental programs. J Public Health Dent. 1984;44:156-168.
- Burt BA. Fissure sealants: clinical and economic factors. J Dent Educ. 1984;48(suppl 2):96-102.
- Riley JL, Richman JS, Rindal DB, et al. Use of caries-preventive agents in children: findings from the Dental Practice-based Research Network. Oral Health Prev Dent. 2010;8:351-359.
- Lam A. Increase in utilization of dental sealants. J Contemp Dent Pract. 2008;9:81-87.
- Cohen L, LaBelle A, Romberg E. The use of pit and fissure sealants in private practice: a national survey. J Public Health Dent. 1988;48:26-35.
- Dasanayake AP, Li Y, Kirk K, et al. Restorative cost savings related to dental sealants in Alabama Medicaid children. Pediatr Dent. 2003;25:572-576.
- Tripodi D, Filippakos A, Piattelli A, et al. Wear of dental sealing materials using the replication technique. Eur J Paediatr Dent. 2011;12:95-98.
- Duangthip D, Ballungpattama S, Sitthisettapong T. Effect of light curing methods on microleakage and microhardness of different resin sealants. J Dent Child (Chic). 2011;78:88-95.
- Perdigão J, Sezinando A, Gomes G. In vitro sealing potential of a self-adhesive pit and fissure sealant. Quintessence Int. 2011;42:e65-e73.
- Markovic D, Petrovic B, Peric T, et al. The impact of fissure depth and enamel conditioning protocols on glass-ionomer and resin-based fissure sealant penetration. J Adhes Dent. 2011;13:171-178.
- Braz AK, Aguiar CM, Gomes AS. Evaluation of the integrity of dental sealants by optical coherence tomography. Dent Mater. 2011;27:e60-e64.
- Boksman L, Carson B. Two-year retention and caries rates of UltraSeal XT and FluoroShield light-cured pit and fissure sealants. Gen Dent. 1998;46:184-187.
- Fleisch AF, Sheffield PE, Chinn C, et al. Bisphenol A and related compounds in dental materials. Pediatrics. 2010;126:760-768.
Ms. Brinker is a certified dental assistant and an international speaker and published author. She and her husband Erik are the owners of a new publication called Contemporary Product Solutions. She is past faculty member at the Dawson Academy and Spear Education. An active member of the American Academy of Cosmetic Dentistry (AACD), Ms. Brinker is the first auxiliary to sit on the AACD board of directors. She is a member of the E4D Clinical Operations Operators group and had extensive input for the certified dental designer certification. Since 2009, she has been selected as one of Dentistry Today’s Leaders in Continuing Education. She was also selected as one of Dental Products Report’s 25 Most Influential Women in Dentistry and Dr. Bicuspid’s Dental Assistant Educator of the year for 2012. She can be reached at shannon@cpsmagazine.com.
Disclosure: Ms. Brinker was compensated by Ultradent Products for writing this article.









