INTRODUCTION
Virtual design and planning simplify treatment, especially when complex multi-phase care has been planned. Utilization of 3D printing allows the fabrication of provisional restorations during the same appointment as prep and design, yielding same-day aesthetic provisionals without needing to wait for fabrication by an outside lab. When provisional crowns are required to be present for months as other treatment is completed, such as the osseointegration of implants, the durability of the provisional material is important. If provisionals chip or fracture during that extended period of use, the patient gets frustrated, and the practitioner has to attempt to repair or remake them, increasing chair time and making treatment less efficient. The utilization of a high-strength aesthetic material also allows the patient to “test-drive” the aesthetics of the provisionals and permits modifications in the final restorations that satisfy the patient’s aesthetic desires. Novel 3D printing resins, such as OnX Tough (SprintRay), enable rapid fabrication of durable provisional restorations for such applications. A case is presented here illustrating complex treatment involving orthodontics to better position the teeth and placement of 3D printed long-term provisionals in preparation for implant placement.
CASE REPORT
A 69-year-old female patient presented for consultation, expressing a desire to improve the aesthetics of her smile and replace her missing bilateral maxillary molars. Full-mouth radiographs were taken and evaluated (Figure 1). Decay was noted on the right second premolar (tooth No. 4) with no apparent pulpal involvement, and no apical pathology was noted radiographically. The right first premolar (tooth No. 5) had a PFM crown present with recurrent decay on the distal. Deep decay with pulpal involvement was noted on the right canine (tooth No. 6), with most of the coronal tooth structure affected. A midline diastema was noted between the central incisors, and facial flaring of the laterals and centrals was present. The left canine (tooth No. 11) was missing most of its coronal tooth structure, and pulpal involvement was noted on the radiograph with no apical pathology present. The left mandibular first molar (tooth No. 19) was missing most of the coronal tooth structure with no pulpal exposure noted.
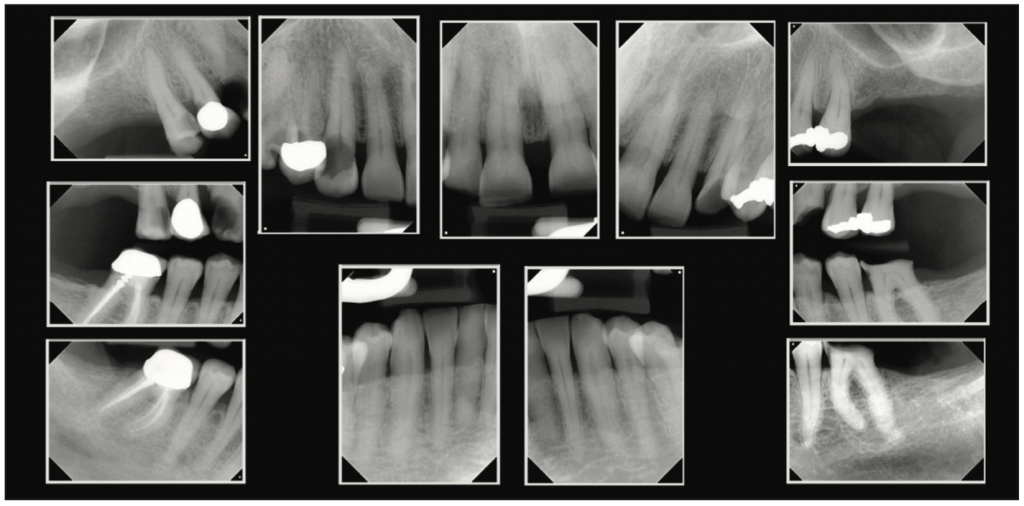
Figure 1. Radiographs at the initial consultation demonstrating issues in the maxillary arch that the patient wished to address.
The patient returned to discuss treatment options and was presented with a detailed plan for the maxillary arch. This included endodontic treatment of the maxillary canines bilaterally, caries removal on tooth No. 4 with a resin core buildup, removal of the old crown on tooth No. 5, and crown preparations on both right premolars. Provisional splinted crowns would be placed on teeth Nos. 4 and 5 with orthodontic brackets embedded in the provisional crown resin. Brackets would be placed on the maxillary arch from second premolar to second premolar, and hyper-eruption of the canines would be performed bilaterally, along with uprighting of the centrals and laterals to close the diastema and better position the teeth aesthetically. Following orthodontic repositioning, the maxillary teeth would be prepared for crowns, and provisional crowns would be placed to provide improved aesthetics to the patient’s smile in preparation of implant placement in the molar area bilaterally. The patient was informed she would be in those provisional restorations for an extended period of time (6 or more months) as the implants integrated, at which time final restorations would be initiated for the entire arch. The patient agreed to the treatment plan after any questions she had were answered.
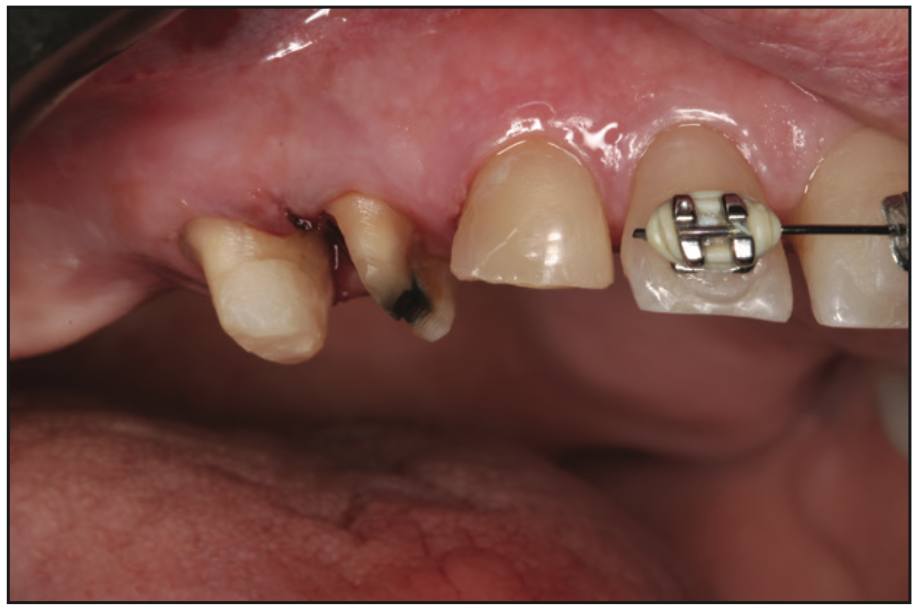
Figure 2. The defective crown on the first premolar and decay on the second premo- lar were removed with placement of a core buildup before crown preparations were refined on the premolars.
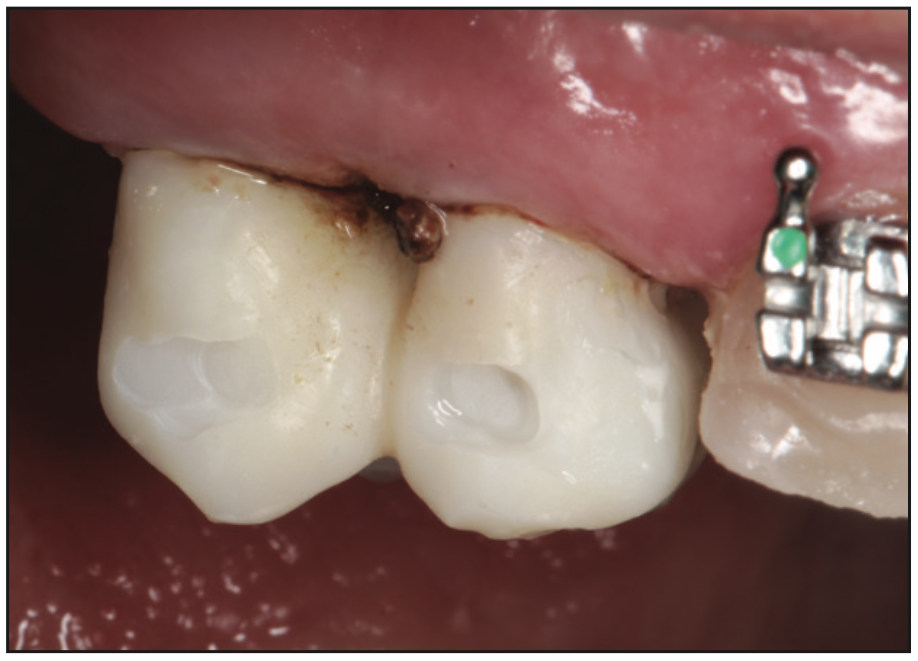
Figure 3. Splinted provisional crowns were printed with OnX resin bleach (SprintRay) with areas on the buccal for placement of orthodontic brackets to aid in the orthodontic treatment.
Endodontic treatment was initiated and completed on the canines. The decay was removed from tooth No. 4, a resin core buildup was completed using ParaCore dual-cure resin core material (COLTENE), and the tooth was prepared for a crown. The old PFM crown was removed from tooth No. 5, and the crown preparation was refined to remove any caries present (Figure 2). Teeth Nos. 4 and 5 were intraorally scanned with a CS 3700 scanner (DEXIS) and imported into exocad (exocad America). Splinted provisional crowns were designed with an area on the buccal of each to accept embedding an orthodontic bracket into the resin. The provisional crowns were then printed on a SprintRay Pro55 S printer (SprintRay) using OnX resin (SprintRay). The printed crowns were tried on the premolars intraorally and then cemented with Temp-Bond (Kerr Corporation) (Figure 3). Orthodontic brackets were luted into the provisional crowns with Transbond XT Light Cure Paste Adhesive (3M) and applied to the other teeth on the maxillary arch. An archwire was placed, connecting the brackets from second premolar to second premolar (Figures 4 and 5).
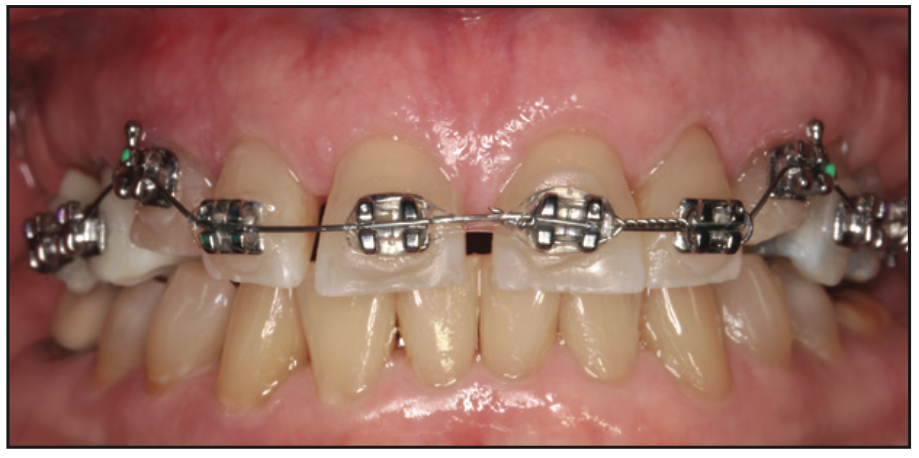
Figure 4. Archwire was placed between the printed provisional crowns on the right premolars to the left premolars to initi- ate orthodontics to tip the centrals and laterals lingually and extrude the canines bilaterally.
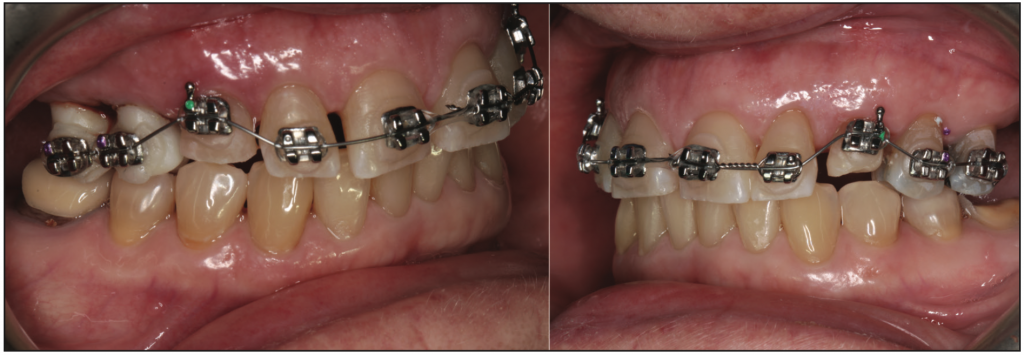
Figure 5. Lateral views of the orthodontic brackets and archwire on the right and left at the initiation of orthodontics in the maxillary arch.
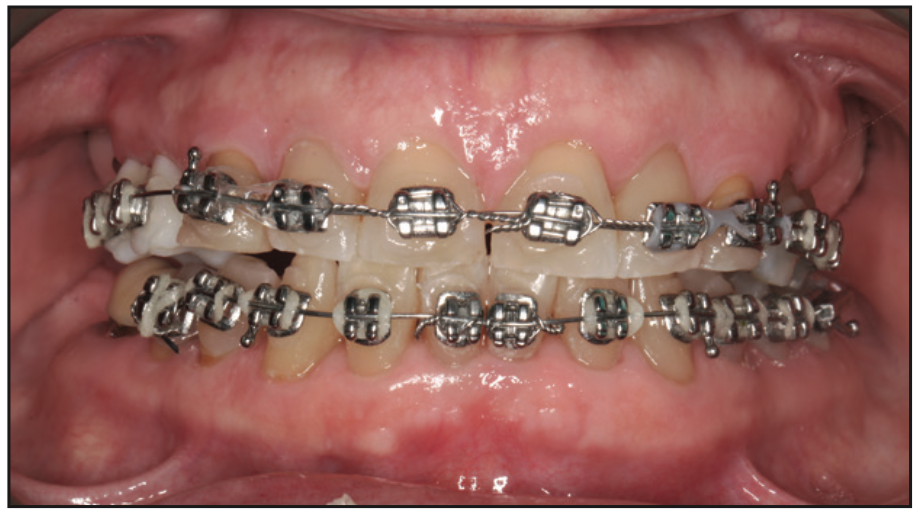
Figure 6. Facial view at the completion of orthodontics with closure of the diastema in the anterior maxilla and coronal positioning of the canines bilaterally.
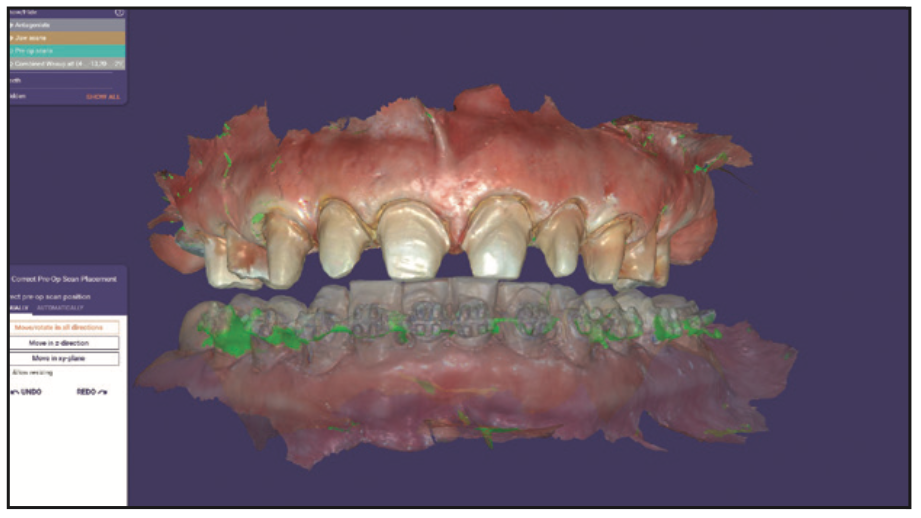
Figure 7. Intraoral scan of the arches with a CS 3700 scanner (Carestream Dental) following crown preparation of the teeth in the maxillary arch, which was then imported into exocad.
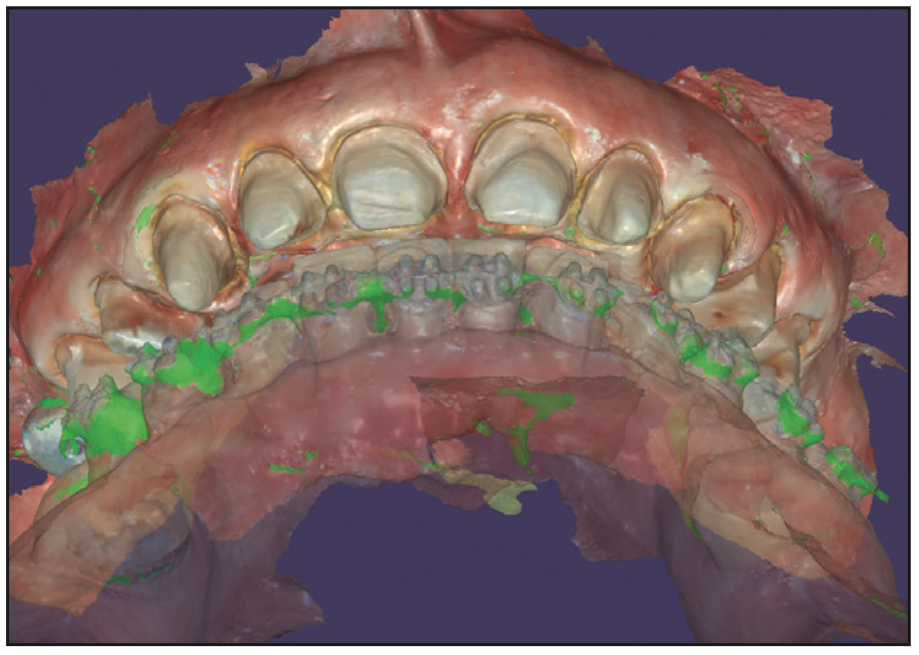
Figure 8. View of the scanned arches in occlusion after crown preparation, demonstrating sufficient occlusal clearance for the planned restorations.
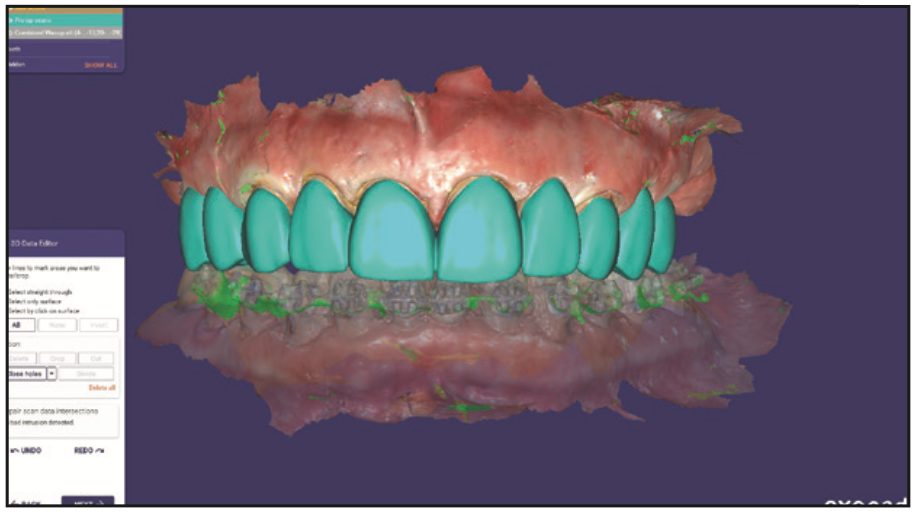
Figure 9. Virtual design of the planned maxillary provisional crowns.
The patient was seen on a regular basis to check and adjust the orthodontics as required, and at 5 months of treatment, orthodontics had been completed with extrusion of the canines bilaterally and uprighting of the laterals and centrals with the closure of the midline diastema (Figure 6). The orthodontic wire and brackets were removed from the teeth on the maxillary arch. The maxillary teeth were prepared for crowns and scanned with a CS 3700 scanner, and the file was imported into exocad (Figure 7). The occluded virtual arches were evaluated to confirm adequate occlusal clearance for the design of the provisional restorations (Figure 8). Virtual crowns were designed in the software with second-premolar-to-second-premolar splinting of the remaining teeth on the arch (teeth Nos. 4 to 13) (Figure 9). This was designed to lock the teeth in the established position that resulted from orthodontic treatment. The virtual provisional splinted crowns were laid out in DentalCAD 3.0 Galway (exocad) software to be printed on the SprintRay Pro55 S printer in OnX resin (Figure 10). The virtual provisional restoration was placed in the virtual build platform in preparation for 3D printing (Figure 11). After printing on the SprintRay Pro55 S printer with OnX resin, the restoration was removed from the unit with supports attached to the build platform (Figure 12). The supports were removed with a bur, and the areas were polished to complete the provisional restoration for intraoral insertion (Figures 13 and 14).

Figure 10. Layout of the crowns to be printed, with a full-arch provisional restoration from second premolar to second premolar.
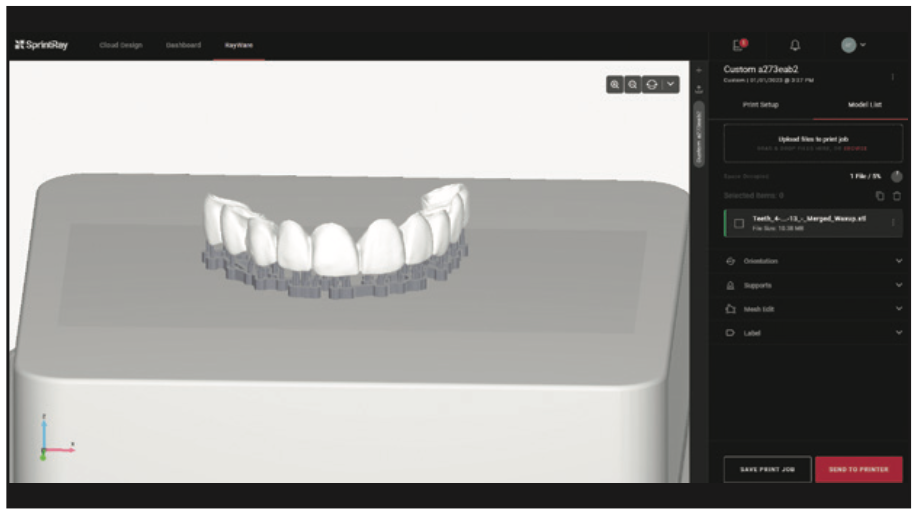
Figure 11. Virtual setup of the provisional to be printed on the build platform in the software.
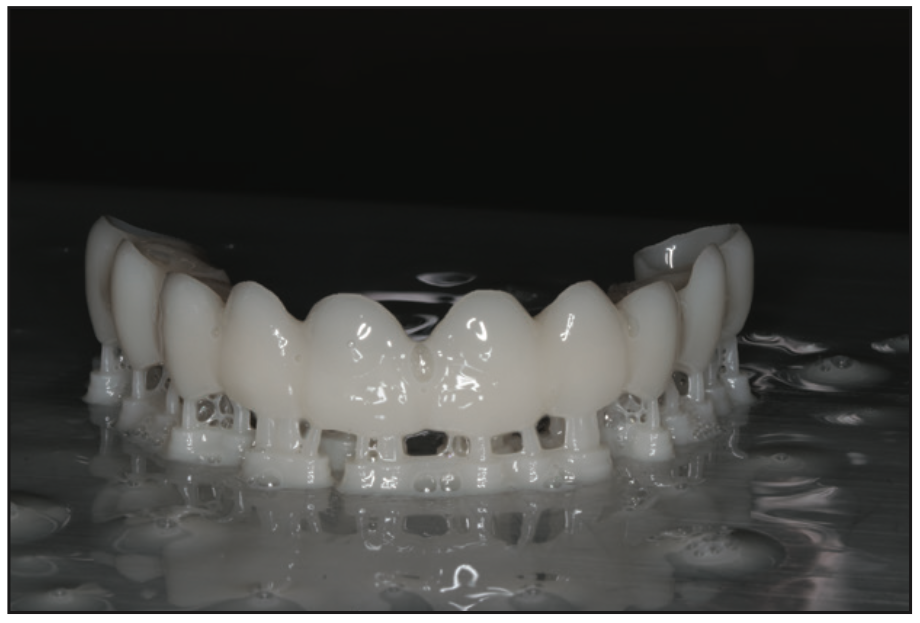
Figure 12. After printing, the OnX Tough (SprintRay) resin provisional restoration was completed with supports on the build platform.
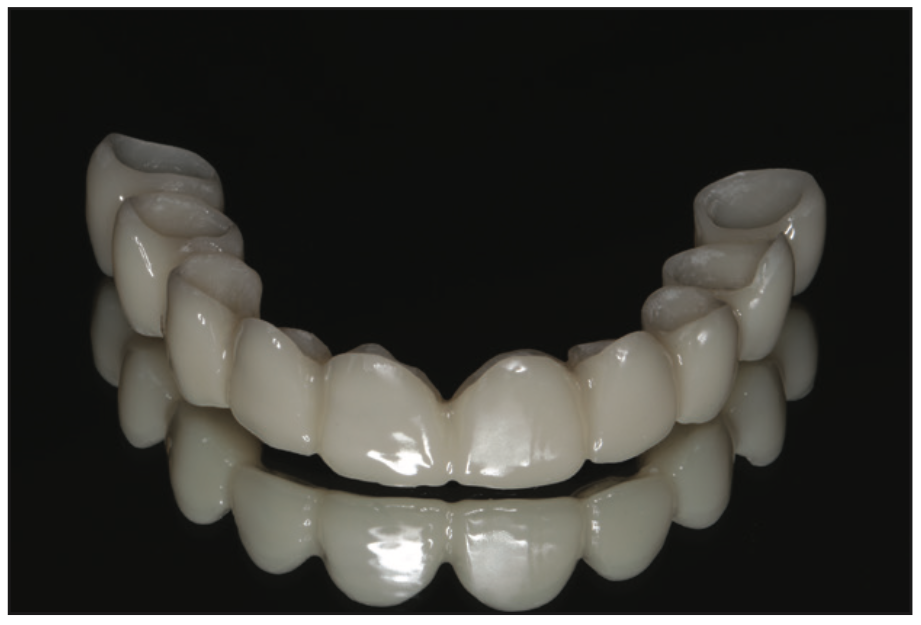
Figure 13. View of the buccal/facial surface of the full-arch OnX Tough printed provisional restoration.
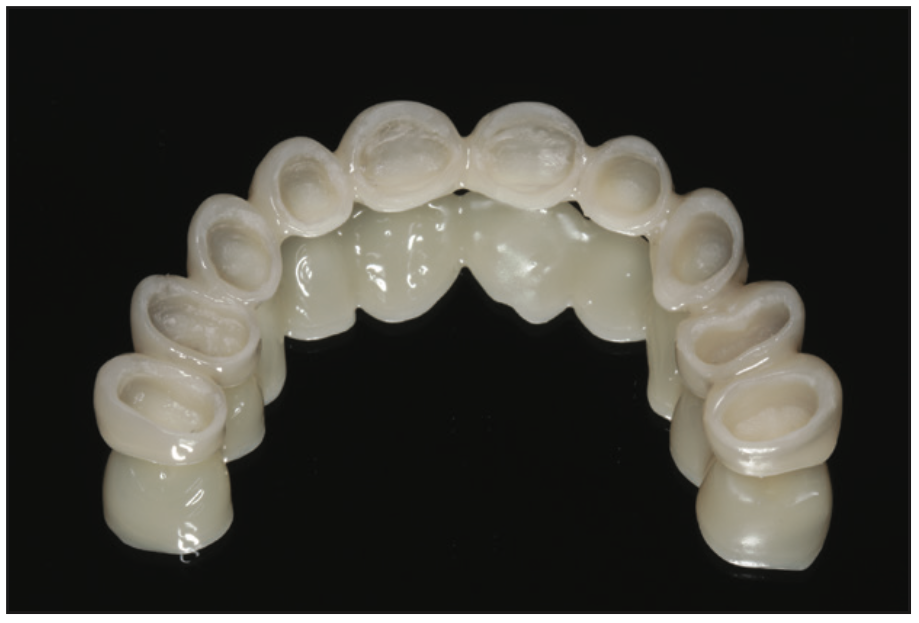
Figure 14. View of the internal surface of the full-arch OnX Tough printed provisional restoration.
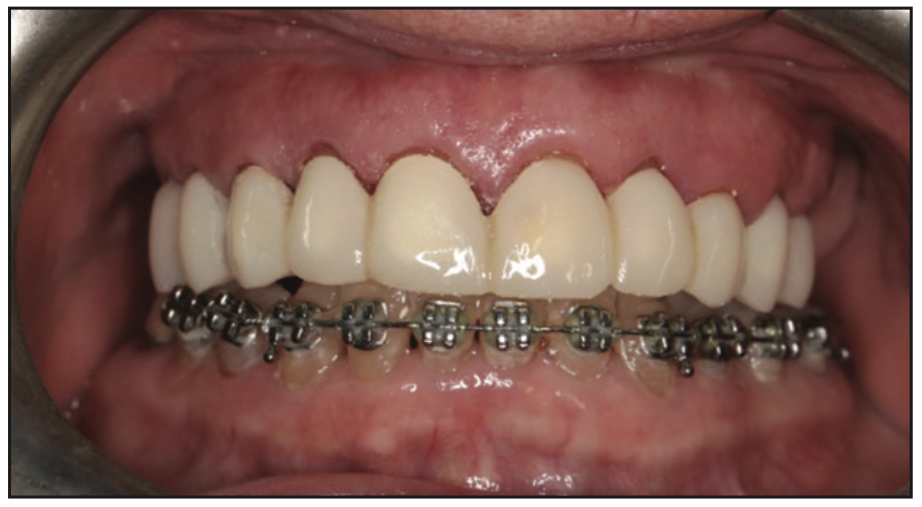
Figure 15. Trying in the splinted full-arch provisional restorations on the prepared teeth from second premolar to second premolar and in occlusion.
The splinted full-arch provisional crowns (teeth Nos. 4 to 13) were tried in to assess fit on the preparations (Figure 15). The aesthetics and occlusion were evaluated (Figures 16 and 17). The patient was shown a mirror to evaluate her improved smile, and she expressed that she was happy with the aesthetics. The provisionals were luted with Temp-Bond temporary cement. It was decided at a later appointment to optimize the aesthetics of the provisionals by changing to a lighter shade at the patient’s request and, as they would be worn for an extended period, to redo them in the stronger OnX Tough resin. Utilizing the same virtual design, slight modifications were made to the design in the software to improve the shapes of the teeth. The provisionals were reprinted in OnX Tough resin and then luted with Premier Implant Cement resin cement (Premier Dental) in clear shade. The OnX Tough resin yielded an acceptable aesthetic result for the patient (Figures 18 and 19). The patient would be in the provisional crowns for 6 or more months to allow placement of implants at the maxillary first molars bilaterally and to allow them to osseointegrate before being restored. During that period, the splinted provisional crowns would hold the maxillary teeth in a stable position and prevent anterior flaring.
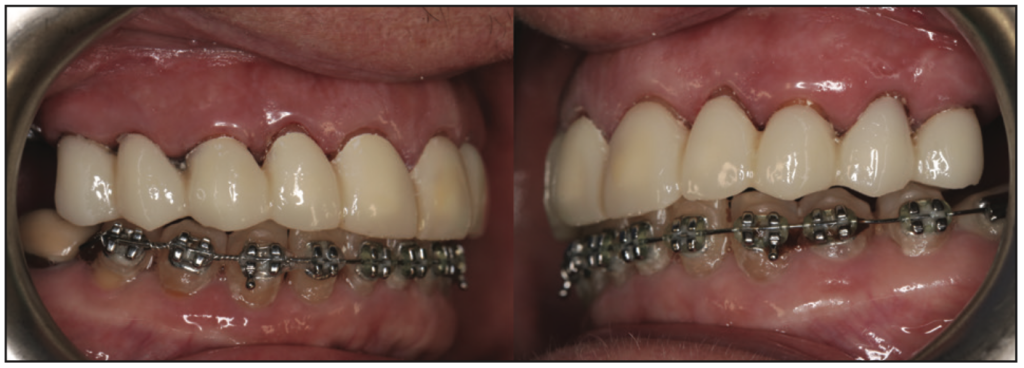
Figure 16. Lateral views of the occluded maxillary provisional restorations.
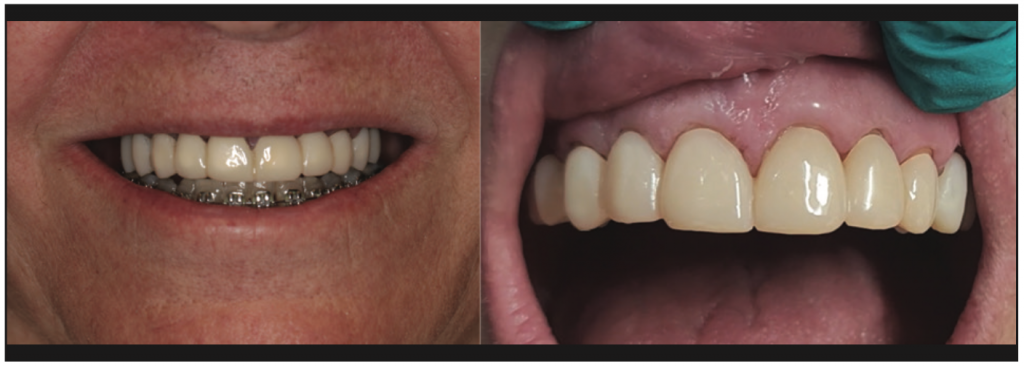
Figure 17. Facial views of the provisional restorations utilizing OnX at the time of placement and 2 months later.
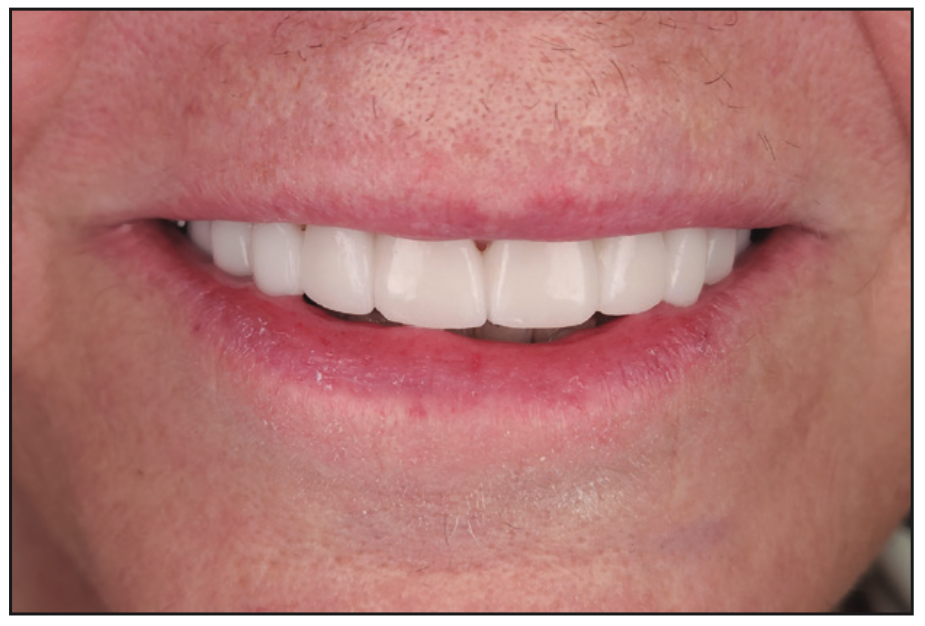
Figure 18. Restorations were remade in OnX Tough resin demonstrating better shade aesthetics to meet the patient’s desire for whiter teeth and more natural anatomy.
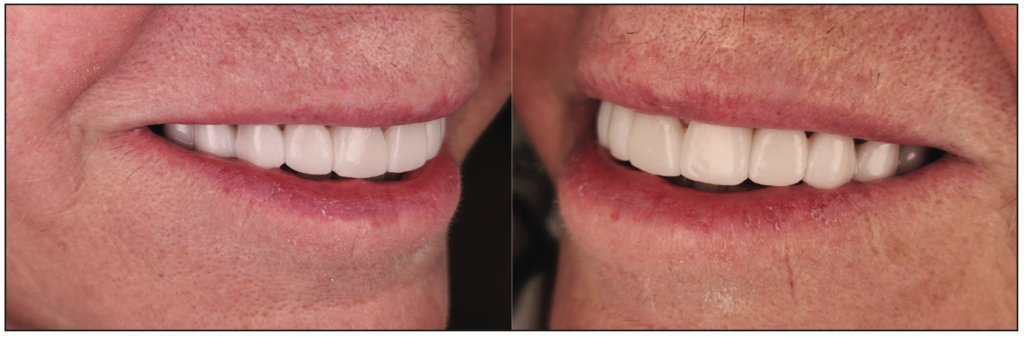
Figure 19. Lateral views of the patient’s smile demonstrating improved aesthetics with the provisional restorations using OnX Tough.
CONCLUSION
Complex dental treatment often involves treatment over an extended period of time while phases of care are being completed. This is especially true when implants will be included in treatment and time is needed for osseointegration before the final restorative phase can be initiated. When orthodontics will also be part of the treatment plan, and the remaining teeth in the arch will receive crowns upon completion of orthodontics, provisional restorations will be a key part of the treatment plan. Utilization of an aesthetic, strong provisional material allows the placement of provisionals that are aesthetic and will hold up well during the extended period of treatment time until final restorations can be placed. Digital planning, with intraoral scanning and virtual design of the provisional restoration, aids in this process, shortening the time that would be required compared to the traditional fabrication of provisionals at a lab. Digital 3D printing allows fabrication of those provisionals while the patient is in the chair and should be considered as a treatment option for the practitioner.
ABOUT THE AUTHORS
Dr. Ferguson has taught implant dentistry for the last 30 years and has lectured nationally and internationally. His lecture topics have included treatment planning, case selection, simple and complex surgical placement and restoration, advanced bone grafting and bone graft materials, use of CT and surgical guides, hygienic maintenance, and management of complications and failures. Dr. Ferguson has been instrumental in bringing low-cost 3D printing technology to dentistry and developing digital workflows for implant placement, restorative dentistry, and clear aligner orthodontic therapy. He has developed and implemented implant training programs and hands-on bone grafting courses, including at Implant Educators Academy—a 6-month implant live surgery continuum at the University of Florida. He maintains a private practice with his wife, Dr. Katherine Ferguson, in Davie, Fla, emphasizing digital dentistry and dental implants. He can be reached at drferguson@aol.com.
Dr. Kurtzman is in private general dental practice in Silver Spring, Md, a former assistant clinical professor at the University of Maryland in the department of restorative dentistry and endodontics, and a former American Academy of Implant Dentistry Implant MaxiCourse assistant program director at the Howard University College of Dentistry. He has lectured internationally on the topics of restorative dentistry, endodontics, implant surgery, prosthetics, removable and fixed prosthetics, and periodontics and has published more than 800 articles globally as well as several e-books and textbook chapters. Dr. Kurtzman has been honored to be included in Dentistry Today’s Leaders in CE listings annually since 2006. He can be reached at dr_kurtzman@maryland-implants.com.
Disclosure: The authors report no disclosures.











