
The percent of general practices providing intravenous (IV) sedation services still remains low. However, the increase in blood-derived products for hard- and soft-tissue regenerative treatment has increased the number of general dentists and specialists drawing patient blood during treatment.
Most dentists don’t think that drawing blood can place them on the wrong side of a malpractice suit, landing them in the witness chair desperately trying to defend themselves. Although drawing blood is a common medical procedure, dentists do not get training in it at the undergraduate level and may only be exposed to it in post graduate residencies or through continuing education.
The Risks of Drawing Blood
Yet there is limited information concerning documented complications of venipuncture. The most common of these complications involves injuries leading to paresthesia and forearm pain after phlebotomy to the venipuncture area due to medial antebrachial cutaneous nerve damage.
As may occur with administration of local anesthetic intraorally to achieve an inferior alveolar nerve (IAN) block, where the IAN may be injured, injuries to the medial antebrachial cutaneous nerve are relatively rare but may be a serious complication of drawing blood from the arm. Nerve damage from an improperly administered blood draw can result in a condition known as claw hand.
Also known as ulnar claw or spinster’s claw, claw hand is an abnormal hand position that develops due to a problem with the ulnar nerve. A hand in the ulnar claw position will have the fourth and fifth fingers extended at the metacarpophalangeal joints and flexed at the interphalangeal joints. Patients with this condition can make a full fist, but when they extend their fingers, the hand posture is referred to as claw hand. The ring and little finger usually can not fully extend at the proximal interphalangeal (PIP) joint.
This can become a debilitating injury and, if left untreated, may result in loss of ability to use the arm. A New York Times reporter had this complication in 2006 and wrote about how a routine blood draw led to her developing claw hand and how it had to be managed.
The Lack of Training
According to The Washington Post, unlike other medical skills, in many states phlebotomy does not require specialized training and goes largely unregulated. Many medical personnel performing phlebotomy procedures have received little training, leading to incorrect administration of blood draws and injuries to patients. Even an experienced phlebotomist can sometimes have trouble finding or isolating a vein.
The Clinical & Laboratory Standards Institute constitutes the body of knowledge on the subject from which the standard of care can be derived. Unfortunately, dentists do not know the standard of care for phlebotomy. Dental schools are not training dentists in how to draw blood, and most dentists do not invest in educating themselves.
There are recognized and effective methods to prevent nerve injury by appreciating the details and the anatomical features of the peripheral arteries, nerves, and veins of the arm. The recommended order of vein selection also needs to be followed. To prevent the needle from being inserted too deeply, shorter needles may be used.
Probing is a very dangerous procedure that must be avoided, but re-direction of the needle is acceptable if it is performed once per venipuncture. It also is critical to ask patients before venipuncture whether they have experienced a previous nerve injury or other conditions like a mastectomy that require modified techniques.
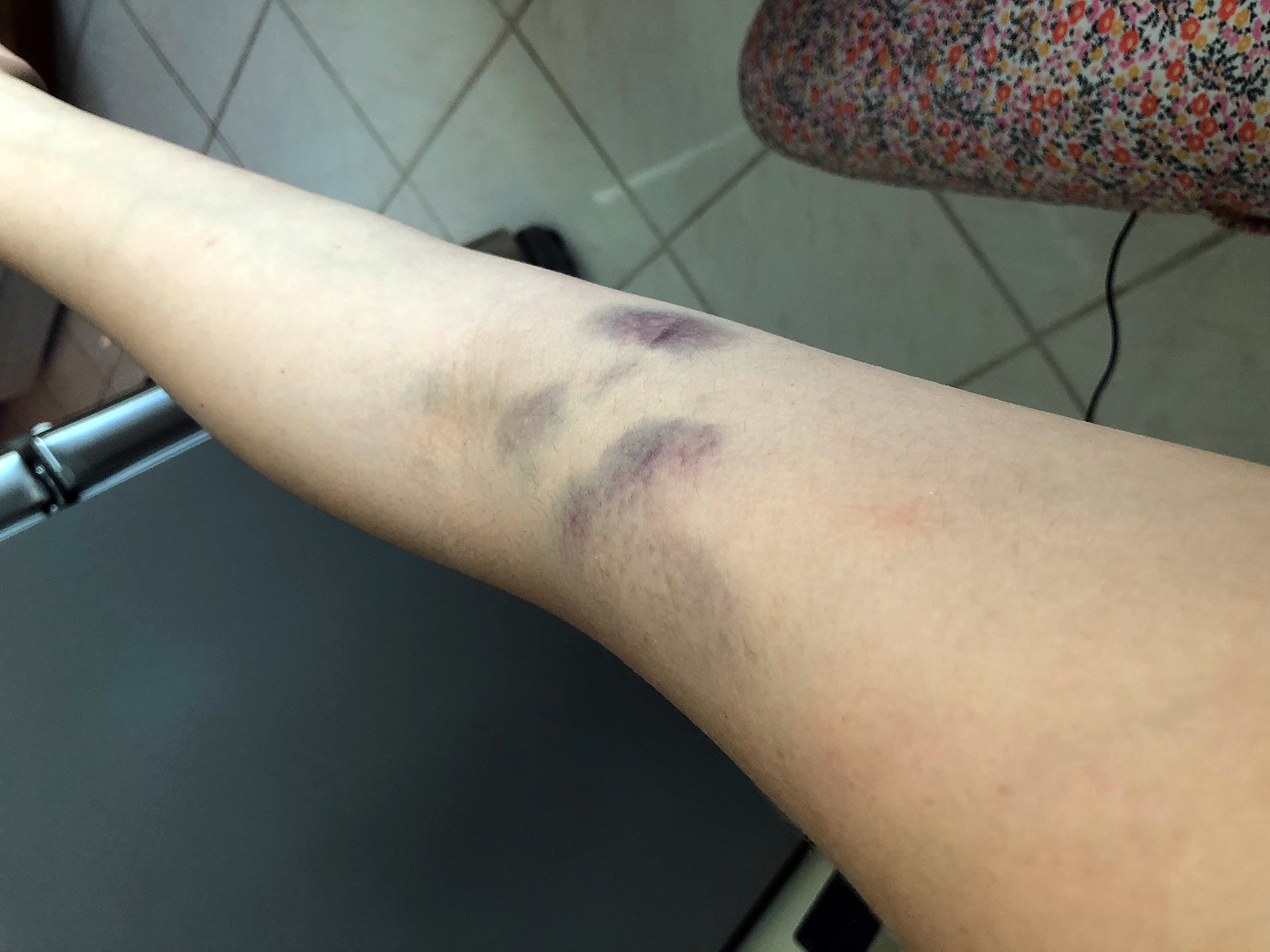 |
| Figure 2: Hematoma resulting from trauma to the blood vessel during blood drawing shown several days following phlebotomy. |
A phlebotomist can miss the vein and pierce a nearby nerve instead, causing shooting pain or paralyzing damage to the affected arm. Other types of injury may occur when the needle entirely passes the vein and punctures an artery or bruises the vein, which can cause major internal bleeding and result in a hematoma (Figure 1 and 2). Phlebotomy patients may be injured not directly from the needle itself, but they may faint and lose consciousness as a result of anxiety related to the overall experience and injure themselves in the resulting fall.
Guarding Against Liability
The risk of a nerve injury can never be completely eliminated. But when an injury occurs, establishing liability for the injury rests on the plaintiff’s attorney, who will attempt to find error in the way the procedure was performed and evaluate the medical professional’s training.
The biggest factor in avoiding phlebotomy complications is getting proper hands-on training in these procedures. Additionally, knowing the anatomy of the arm and how to manage complications should they arise can assist in limiting liability for those dental practitioners drawing blood from their patients.
Nerves passing the antecubital area may not be visible or palpable. It’s crucial that those who are performing venipunctures know the anatomy of the antecubital fossa. Medical professionals performing venipunctures particularly need to know where the nerves and the arteries lie in relation to the acceptable veins for venipuncture in this area.
Dentists and specialists who routinely perform venous punctures should obtain some sort of certification or continuing education from a valid source. This will give them more confidence in their routine venipuncture procedures, and they will have a better sample every time. It also will help to keep them and their patients safe from unnecessarily complications and litigation.
Dr. Javid received his doctorate of dental surgery from the dental school at the University of Southern California (USC) and is a former member of the USC advanced education in general dentistry faculty. He also is a Diplomat of the International Congress of Oral Implantology, a Fellow of the California Implant Institute, an Associate Fellow of the World Congress Laser Institute, a clinical phlobotomy technician, a member of the Biolase advisory board, medical director of DIO Implant, a DIO Navi investigator, CEO of the Doctor Smile Dental Group, CEO of the Southbay Implant Institute, and a member of the Community’s Child board. His practice is limited to implant dentistry, full-mouth reconstruction, and laser dentistry. He can be reached at doctorkayvonjavid@gmail.com.
Dr. Kurtzman is in private general practice in Silver Spring, Md, and is a former assistant clinical professor at the University of Maryland, department of endodontics, prosthetics, and operative dentistry. He has earned Fellowships in the AGD, American College of Dentists, International Congress of Oral Implantologists (ICOI), Pierre Fauchard Academy, and Academy of Dentistry International, as well as a Mastership in the AGD and ICOI and a Diplomate status in the ICOI and American Dental Implant Academy. He has lectured internationally and has published more than 585 articles. He can be reached at drimplants@aol.com.
Related Articles
Full-Arch Zirconia Screw-Retained Prosthesis
New Technique Simplifies Bone Graft Procedures











