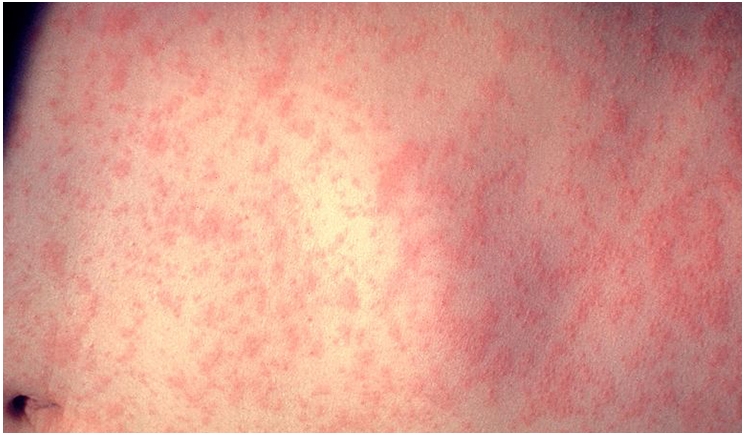
The United States is now experiencing its largest outbreak of measles in 20 years. For the most part it was believed that the chance of a measles outbreak in the United States had been eliminated thanks to the measles, mumps, and rubella (MMR) vaccine. Unfortunately, some parents have been reluctant to get their children vaccinated. Couple this with people entering the country unvaccinated and exposed to measles, we now see outbreaks across the country.
According to the Centers for Disease Control and Prevention:
- About one in four people in the United States who get measles will be hospitalized.
- One out of every 1,000 people with measles will develop brain swelling, which could lead to brain damage.
- One or two out of 1,000 people with measles will die, even with the best care.
- Women exposed to measles while pregnant are at risk of possible birth defects or spontaneous abortion.
Given the infectivity of measles, just one patient in a waiting room with measles will expose everyone in the area, and the virus can linger for up to two hours after the ill person leaves. This can be any waiting room, dorm, school, church, home, or your practice. Public health policy usually dictates that people exposed to a suspected measles case may be quarantined until their measles vaccination can be determined.
What does this mean for dental practitioners? In keeping with many medical practices in areas of outbreaks, many patients with a rash and fever are not being allowed in waiting rooms and are instead being seen in an outside isolated area. Dental practices should be aware that an infected measles victim can be a child or an adult. Good infection control will not prevent the spread of the virus because it can linger in the air long after the victim leaves.
So what can we do?
The following suggested guidelines will help guide your decisions.
First, if you are not in an area of infection, then you should continue patient care as usual with proper infection control procedures. But be on the lookout for patients with runny nose, coughing, malaise (flu-like symptoms but not flu season), any small white spots in the palate, and rash on exposed areas. In some cases, measles presents with oral lesions known as Kopliks spots that are a precursor to full blown measles. With Koplik spots and a skin rash, you may want to stop treatment and discuss these symptoms with your patient. You may also need to follow up with your local public health department.
Second, work with your local health department to see what precautions should be followed.. Questions to be asked would include:
- Is measles in our area?
- Who do I contact if I suspect a measles case?
- Where do I send a measles case if suspected?
Finally, if your practice is in a measles area, you should let patients know if they are symptomatic with a fever and rash that they need to reschedule. A good idea would be to confirm all patients to see if someone may need to be rescheduled. The real problem is a situation where you have a suspected case in your practice. You will need to contact your local health department because the status of your practice may be affected by decisions from your public health department.
As dentists, we are concerned about the health and well-being of our patients. Being aware of the devastation of measles and our patients’ health helps make us a part of any effort to protect the public’s health.
Dr. Williams graduated from the University of Tennessee College of Dentistry in 1982 with subsequent service of 30 years in the United States Navy Dental Corps, where he was the Public Health Emergency Officer for Navy Region Midwest. He is currently an associate professor at the Midwestern University College of Dental Medicine-Illinois. He also is a member of the Skokie (Illinois) Board of Health. He is a member of the ADA, serves as a national spokesperson for the Academy of General Dentistry, and holds board certified status in the American Board of General Dentistry. Dr. Williams is also a Fellow in the American College of Dentists, International College of Dentists, and Academy of Dentistry International. Dr. Williams received his Masters in Public Health in 2017. He can be reached at [email protected].
Related Articles
Oregon Bill Allows Dentists to Administer Vaccines
Ensure Best Practices for Infection Control in Your Dental Office
Disinfectant Wipes Kill 44 Different Pathogens


