INTRODUCTION
In today’s economy, we are finding more and more patients presenting with severe dental problems ranging from multiple tooth decay to advanced generalized periodontitis, because they have put off dental treatment either due to fear of discomfort or fear of cost. The major reason for finally presenting to the office is because they just can’t withstand the pain anymore or the infection has gotten so bad that it will affect their overall health. For the practioner, it is very difficult to treatment plan when there are so many dental issues to address while trying to stay within the patient’s dental awareness, time frame, and budget. Practicing in Michigan, I have personally found many of these patients need full-mouth extractions because their teeth have been affected by extensive caries and periodontal disease to the extent that no other treatment is possible. This could be due to neglect, poor oral hygiene, genetic dental malformations, hereditary issues, or unhealthy dietary consumption. Before full-mouth extractions are implemented into a patient’s treatment plan, a definitive plan must be examined and reviewed to offer the patient several options of oral rehabilitation.
The initial portion of these complex treatment plans focuses on eliminating the infections so that the patient is relieved of acute or chronic pain. Unfortunately, due to the severity of these cases, the treatment of full-mouth extraction is the only option.
However, most dental providers may choose to refer these full-mouth extraction cases due to patient fear of the surgery or the possibility of complications. Having a technique of extracting teeth with less risk of complications is a more desired approach for many practitioners. This article will describe the processes involved from diagnosis and treatment planning to full-mouth extractions and restoration.
Having all one’s teeth extracted definitely has a huge psychological impact on the patient because of the fear of pain of the procedure, fit or look of the final prosthesis, function of the reconstruction, and cost of treatment. However, not addressing the issue can affect the general health of the patient. So keeping view of all these concerns, there are certain conditions where full-mouth extraction is indicated and cannot be ignored.
 |
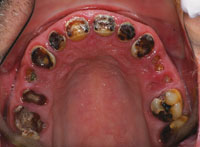 |
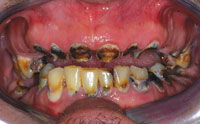
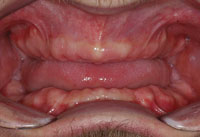
| Figure 1. Preoperative retracted view. | Figure 2. Occlusal view of maxillary arch. |
 |
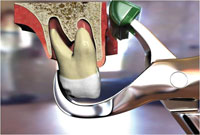 |
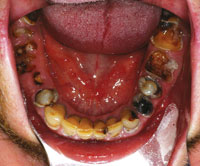
| Figure 3. Occlusal view of mandibular arch. | Figure 4. Illustration of the positioning of the Physics Forceps (Golden Dental Solutions) (upper first molar). |
 |
 |
| Figure 5. Positioning of Physics Forceps for a broken down tooth (lower molar). | Figure 6. Extraction of 32 teeth in 15 minutes. |
Periodontal Problems
When every step has been taken, utilizing modern periodontal therapy and surgery, to treat or delay periodontal disease without improvement, then the only treatment may be partial or full-mouth edentulation. Otherwise, the disease affects supporting structures of teeth, causing their destruction along with the health of the patient by raising the risk to heart disease. It is important to note that when these teeth are already excessively loose from infection, then they must be extracted to prevent further progression of the disease into bone, which could lead to problems of denture construction or strategic implant placement.
Extensive Caries
When the extent of decay is far beyond proper restoration with a good prognosis, then it may be best to remove these teeth with the delivery of a complete set of dentures to initially control the pain and infection followed by implant reconstruction. After many decades of improvements in oral health, tooth decay is still on the rise. Much of the blame can be placed on today’s diet consisting of fast food, soda pop, sport drinks, juices, and energy drinks. Another factor that comes to mind is aging baby boomers who are living longer. A majority of these patients may be taking medications that are causing severe drying in the mouth (xerostomia) that results in a high caries rate, or simply they are unable to brush and floss properly because of hand dexterity issues.
When a patient has been diagnosed by the dentist that he or she needs full-mouth extractions and no other alternatives are available, then most of the anxiety in the patient’s mind is on how the full-mouth extractions will be carried out by the dentist or oral surgeon, how much pain and suffering he or she will have to undergo, and how will the definitive restoration, whether denture or implant prosthesis, look and function.
CASE REPORT
Diagnosis and Treatment Planning
A young man in his late 30s presented to the practice dissatisfied with the appearance of his smile. He commented that he was experiencing constant sensitivity to hot and cold as well as tenderness to biting. He also mentioned that he could feel some broken portions of tooth structure causing food to be trapped, resulting in swelling in his gum tissue.
Initial diagnostic evaluation consisted of a series of digital images with study models, a panoramic x-ray, and a full set of radiographs. Upon clinical examination, it was very evident that the patient had gross decay in his whole dentition as well as localized advanced periodontal disease in the posterior regions (Figure 1). Overall health of these teeth was severely compromised with poor prognosis (Figures 2 and 3). Upon examination of the radiographs, it was clearly obvious that he needed to have all his teeth extracted. Although he denied any drug use, the patient did admit to smoking 2 packs of cigarettes per day and drinking a 2 liter bottle of Mountain Dew soda every day. All risks, benefits, and alternatives were reviewed with the patient regarding his diagnosis and treatment plan.
To develop a treatment plan and to determine if the vertical dimension could be increased, a diagnostic wax-up was fabricated. Based on information gathered from the initial consult, it was determined that all his teeth (Nos. 1 to 16 and Nos. 17 to 32) should be removed, the maxillary and mandibular alveolar ridges leveled and then grafted with immediate placement of removable maxillary and mandibular dentures. It was also determined that aesthetics and function could be further enhanced later on (4 to 6 months) with the placement of dental implants once the grafted areas had healed. The final treatment plan would consist of fixed PFM bridges for each arch after proper healing as long as it fit the patient’s budget.
Advantages of full-mouth extractions in a single visit include: the number of appointments is reduced, local anesthesia has to be given in only one visit, and the patient doesn’t have to go through the procedure multiple numbers of times. A disadvantage of full-mouth extractions in a single visit is that the patient has to face the aesthetic and functional problems associated with a period of complete edentulism. However, considering the pain and infection this patient was suffering, it was most advantages to do full-mouth extractions in one seating.
 |
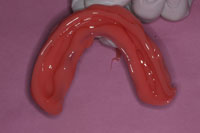 |
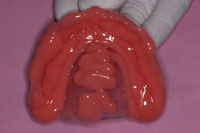
| Figure 7. Maxillary soft reline. | Figure 8. Mandibular soft reline. |
 |
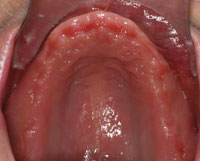 |
| Figure 9. Postoperative retracted view. | Figure 10. Healed maxillary arch. |
 |
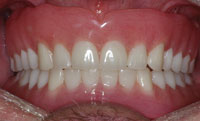 |
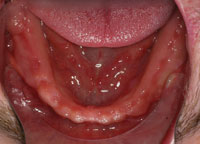
| Figure 11. Healed mandibular arch. | Figure 12. Retracted view of maxillary and mandibular dentures. |
Extractions
If all the teeth have to be extracted in a single visit, then anesthesia is given in all regions of mouth, and the teeth are extracted in a particular order. Since the patient is sedated utilizing an intravenous infusion pump, it is necessary to keep the patient’s mouth open using a mouth prop. For this reason, I routinely extract teeth in quadrants starting from the upper left to the upper right and then down to the lower right and lower left. This way we can keep the patient’s mouth open while working in a consistent sequence, saving time.
One set of instruments that I have personally found that make my extractions more effective and efficient are the Physics Forceps (Golden Dental Solutions). The Physics Forceps act simply like a Class I lever, where only one force is applied with the beak on the lingual aspect of the tooth. Once the beak is placed, the bumper is placed on the alveolar ridge at the approximate location of the mucogingival junction to balance the beak. The beak grasps the tooth, while the bumper is the fulcrum to provide leverage and stability for the beak and wrist movement.
Once the instrument is properly placed, pressure is slowly applied using only wrist movement applying a steady and gentle pressure toward the buccal. Approximately within 30 to 60 seconds the internal force or “creep” will build up, allowing the bone to slowly expand and the periodontal ligament to release at which point the tooth will disengage from its socket (known as the “pop”) (Figure 4). Once the tooth has disengaged from the socket, the instrument has completed its task and another instrument of choice (eg, rongeurs) or your fingers can be utilized to remove the tooth. If the tooth is severely broken down (Figure 5), the tooth may be relieved with a bur on the lingual aspect, so that the beak of the Physics Forceps may engage a solid portion of the tooth.
Once the teeth in each quadrant were removed (Figure 6), any sharp areas of the alveolar crest were leveled and bone grafting material placed in the sockets to further enhance preservation of the ridge. The soft tissue was trimmed and sutured from quadrant to quadrant. Once all 4 quadrants were completed, the sutures were inspected to ensure there were no excessive sutures remaining to prevent them from being pulled during the soft reline procedure.
Relining Procedure
Routinely, I prefer to use a vinyl polysiloxane (VPS) soft reline material that that will not degrade in a short amount of time and that works well when relining immediately after extractions (such as Soft Reline [GC America]). Usually, I will start with the upper immediate denture and verify that there are no undercuts before applying the adhesive on the internal aspect of the denture. Once verified, I will place the adhesive, allow it to dry for a few minutes, and then fill the soft reline material in the internal aspect and borders of the immediate denture (Figure 7). The same process will be followed for the lower denture (Figure 8).
Postoperative Instructions
At this point the patient had already been in recovery, awake and alert when doing the reline procedure. He was instructed not to remove his denture for the first 24 hours and to return the following day for another check to make sure the fit, aesthetics, and phonetics were appropriate. Follow-up appointments were scheduled for one-, 3-, and 4-month recall visits. If a new reline was necessary at those appointments, the same protocol for a soft reline was followed.
Fabrication and Delivery of the Definitive Prostheses
Four months postoperatively the areas had healed very well (Figure 9). From the occlusal view, it was very evident that the patient had sufficient width for implant in the future in both maxillary and mandibular ridges (Figures 10 and 11). At this point, a Panorex x-ray was taken to visualize bone integration in the areas that had been grafted. Utilizing the immediate dentures as custom trays, impressions were taken using a medium body VPS impression material (Take One Advance [Kerr]). The laboratory was instructed on what the patient desired for tooth shade, shape, and contour. Within a week, the final dentures were completed and delivered (Figure 12). The patient was so pleased with the final outcome that he is currently saving up to have implants placed in both upper and lower arches with corresponding fixed bridges.
CONCLUSION
Within your practice, a time may come where you, the dental provider, will encounter a patient who might need full-mouth extraction due to severe decay or infection. Having the ability to perform full-mouth extractions in a fast, predictable, and atraumatic way for the patient and the dental team will help eliminate stress for everyone. Using a process that takes advantage of efficient Class I lever principles, as well as biochemical properties while conserving bone and soft tissue will ensure more efficiency and effectiveness. The techniques discussed in this article should allow the general dental practitioner the opportunity to offer more services under one roof.
Dr. Nazarian maintains a private practice in Troy, Mich, with an emphasis on comprehensive and restorative care. He is a Diplomate in the International Congress of Oral Implantologists. His articles have been published in many of today’s popular dental publications. Dr. Nazarian is the director of the Reconstructive Dentistry Institute. He has conducted lectures and hands-on workshops on aesthetic materials and dental implants throughout the Untied States, Europe, New Zealand, and Australia. Dr. Nazarian is also the creator of the DemoDent patient education model system. He can be reached at (248) 457-0500 or at aranazariandds.com.
Disclosure: Dr. Nazarian reports no disclosures.