INTRODUCTION
Almost all dentists have been faced with the challenge of rehabilitating an existing dental prosthesis. Patients, sometimes medically compromised, who request that their current restorations be maintained “just a while longer,” can pose quite a dilemma. Furthermore, the financial limitations in today’s economy are making this challenge become more commonplace. This may be impossible to address when the restoration is functionally compromised. Replacement, or fabrication, of an entirely different type of prosthesis is usually necessary. However, when the restoration is functionally stable and an aesthetic deficiency is present, there are several options available.
Periodontal status of the supporting abutments may also be a consideration. When the long-term prognosis of the involved teeth is guarded, a new restoration involving these teeth should not be considered. Frequently, conversion from a fixed to removable prosthesis is recommended. In this case, a properly informed patient may prefer to delay this option and choose to maintain the current restoration despite the long-term uncertainty. Dental implants are frequently an ideal choice. However, finances, patient health, and whether the patient smokes, are compromising factors.
 |
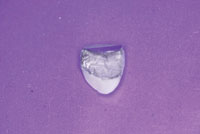 |
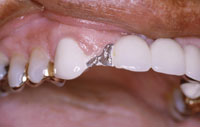
| Figure 1. Fractured porcelain on pontic of 6-unit anterior PFM bridge. | Figure 2. The PFM overcasting as fabricated by the dental laboratory technician. |
 |
|
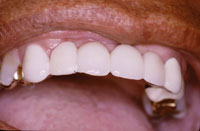
Figure 3. The overcasting cemented in place. |
With current advances in adhesive technology, aesthetic enhancement of an older restoration is often a viable possibility. This is especially true with PFM fixed partial dentures. Case studies demonstrating the use of porcelain laminate veneers and small PFM overlays have been described in the1-4 literature (Figures 1 to 3). Direct composite resin has frequently been described as a useful material for direct repair of porcelain fractures.5-7 The porcelain-to-composite bond is strong, stable, and reliable.8,9 The key to success is the availability of adequate surface area interproximally to ensure an optimally strong bond for the connectors.10 Adhesive retention may be enhanced with wings, slots, or grooves.11,12
This clinical article will demonstrate the use of a variety of techniques in conservative aesthetic rehabilitation of a compromised fixed prosthesis.
CASE REPORT
Diagnosis and Treatment Planning
A male patient presented with a chief complaint of an unattractive smile with several dark areas (Figure 4). A significant fixed prosthodontic restoration had been placed 20 years ago. The existing restorations of concern were a 4-unit fixed bridge extending from teeth Nos. 3 to 6, single-unit crowns on teeth Nos. 7 and 8, and a 3-unit fixed bridge extending from teeth Nos. 9 to 11. Except for tooth No. 7, there was no mobility present. However, the current periodontal bone support was significantly compromised. This individual was a smoker of almost 40 years. He had undergone a variety of different smoking cessation therapies at several points in his life. Unfortunately, there has been no long-term success and he continues to smoke about one pack of cigarettes per day. Despite encouragement, he did not anticipate attempting to again quit smoking in the near future.
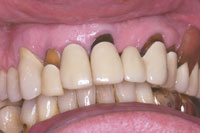 |
| Figure 4. Pretreatment view depicting numerous aesthetic deficiencies. |
Tooth No. 7 had 90% bone loss, and exudate was present in the periodontal pocket. This tooth required extraction. The remaining abutments had approximately 50% bone loss. Considering this patient’s smoking habit and uncertain periodontal support, fabrication of new fixed restorations were not warranted. The patient was informed that a removable prosthesis would eventually be necessary. He requested a short-term, aesthetic solution. One that he hoped would “last a few more years.”
Description of Treatment
It was discussed that tooth No. 7 would have to be extracted due to the advanced bone loss and active infection. A removable appliance was considered as an alternative. However, a resin-bonded pontic was preferred by the patient. The technique used to bond and repair porcelain intraorally would be the foundation for this segment of the rehabilitation.
In the initial appointment, restoration of the abfraction lesions of abutment teeth Nos. 9 and 11 and build-out of the pontic on No. 10 were completed. Two appointments to create a preparation and bond a porcelain pontic for No. 7 followed.
The exposed, discolored dentin surfaces were roughened with a coarse round carbide bur (801 018 [KOMET USA]) and the superficial staining removed. The adjacent porcelain surface was prepared with a very light bevel. The beveled porcelain was etched with hydrofluoric (HF) acid for 5 minutes and the dentin was conditioned with 37% phosphoric acid for 15 seconds. A silane porcelain primer (BIS-SILANE [BISCO]) was applied to the beveled porcelain surface. A light-cured bonding agent (ALL-BOND 3 [BISCO]) was applied to both porcelain and dentin. A composite resin opaquing agent was applied as a thin coat to the dark-colored dentin and exposed metal collar of the prosthesis (Figure 5). This material handles similar to a flowable resin. An opaque masking agent (CLEARFIL ST OPAQUER [Kuraray]) is necessary as restorative composite resin has some degree of translucency, allowing the dark discoloration to negatively affect the aesthetics of the restoration. After the opaquer was light-cured, the restoration was built to full contour, finished, and polished.
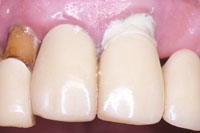 |
| Figure 5. Flowable resin opaquer (Clearfil Majesty Esthetic [Kuraray]) applied to darkened root surfaces. |
The space between the pontic and edentulous ridge was then addressed. A variety of manufacturers have created porcelain repair systems such as CLEARFIL Porcelain Repair Kit (Kuraray), Porcelain Prep Kit (Pulpdent), and Porcelain Repair Kit (BISCO). These systems frequently demonstrate statistically similar shear bond strengths. Many of the specimens exhibit cohesive fracture in the porcelain.13 The undersurface of the pontic was roughened with a coarse diamond bur (849L [KOMET USA]). The porcelain surface to be built out was then etched with HF acid and silanated. HF acid and silanating agents are available in many porcelain repair kits or kits designed for bonding of all-ceramic restorations. It is important to follow the manufacturer’s recommendations and protect the gingival tissues from the caustic HF acid with a conventional rubber dam or a syringable dam material (OraSeal or OpalDam [Ultradent Products]).
Proper silanation may be the most important step in achieving a strong, reliable bond.14-16 Depending on the manufacturer’s recommendation, etching times will vary from 20 seconds to 10 minutes. The concentration of HF acid varies between 5% and 10%.8 Silane primers have a carbon chain that presents an SiO2 group in a functional end. The functional end bonds to the porcelain, allowing the free carbon chain to bond to the resin.8
 |
 |
|
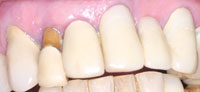
Figure 6. Completed resin restorations masking darkened root surfaces and pontic build-out. |
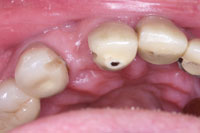
Figure 7. Flattened proximal surfaces and slot preps ready to receive the bonded pontic. |
The pontic was primed with unfilled resin (ALL-BOND 3) and lengthened with composite resin (CLEARFIL MAJESTY Esthetic [Kuraray]) to better approximate the edentulous ridge. In this case an opaquer was not necessary. The undersurface of the resin build-out was polished with composite finishing strips (Sof-Lex finishing and polishing strips [3M ESPE]). All the composite surfaces were coated with a clear resin sealant (BisCover LV [BISCO]) to develop a glaze-like surface. In one appointment, several dark, unaesthetic spaces were eliminated (Figure 6).
At the second appointment, tooth No. 7 was removed. The porcelain surfaces of the abutment teeth were first prepared to create flat, parallel proximal surfaces for bonding the laboratory-fabricated pontic. Slot preparations were then created to enhance retention and facilitate proper positioning (Figure 7). A vinyl polysiloxane (VPS) impression (Imprint 3 VPS [3M ESPE]) was made and sent to the dental laboratory for fabrication. Several options were considered for this pontic, including composite resin, ceramic, and PFM.
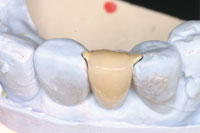
A PFM was chosen for several reasons. Using the same materials as the adjacent teeth offered the best aesthetic match. This type of restoration ensures maximum strength. Finally, the dental laboratory technician could easily create a restoration with a maximum of etchable and bondable porcelain surface area. The precise fit of the restoration created by the technician was evident upon return from the laboratory (Figure 8).
 |
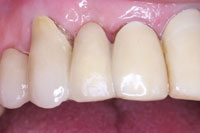 |
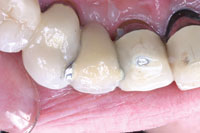
| Figure 8. PFM pontic on the laboratory model. | Figure 9. Restoration bonded in place with a dual-cured resin cement (DUOLINK [BISCO]). |
 |
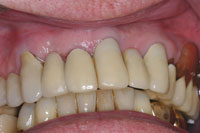 |
| Figure 10. Palatal view of new pontic. | Figure 11. Intraoral view of completed aesthetic enhancement. |
 |
|
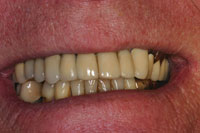
Figure 12. Extraoral view of completed aesthetic enhancement. |
The opposing surfaces were etched with HF acid (PORCELAIN ETCHANT 9.5% HF [BISCO]) and silanated. Light-cured bonding agent (ALL-BOND 3) was applied to the treated surfaces and the restoration seated into place with a dual-cured composite resin cement (DUO-LINK [BISCO]). Excess resin was removed, the restoration finished with diamond burs (858EF, 379EF [KOMET USA]), polishing points (diamond composite polishers [KOMET USA]), and a diamond polishing paste (Luster Paste [Kerr]). The rehabilitation nicely resembled a new restoration (Figures 9 to 12).
Again, the patient was informed that this should be considered a transitional rehabilitation of his anterior prosthesis. We discussed that staining due to smoking would compromise the aesthetics of the composite material over time. The potential for dislodgement of the bonded pontic was discussed if heavy occlusal forces were applied. Finally, periodontal maintenance was stressed as the most important factor in maintaining his “like new” restoration.
SUMMARY
It is not always possible to simply replace a defective restoration in every clinical situation. In certain cases, replacement of a restoration may not be an acceptable choice. As this case demonstrated, it is possible to replace a lost tooth, mask a discoloration, and add to existing porcelain restorations. Adhesive bonding chemistry has allowed dentists to become innovators in restoration and rehabilitation of a compromised restoration.
References
- Herwig L. Minimally invasive porcelain repair using high-strength, wrapped aesthetic veneers. Dent Today. 2006;25:86,88.
- Mancuso A. Salvaging a porcelain/metal bridge with a bonded porcelain-fused-to-metal overcasting. Gen Dent. 2003;51:456-457.
- Galiatsatos AA. An indirect repair technique for fractured metal-ceramic restorations: a clinical report. J Prosthet Dent. 2005;93:321-323.
- Yanikoglu N. The repair methods for fractured metal-porcelain restorations: a review of the literature. Eur J Prosthodont Restor Dent. 2004;12:161-165.
- Ahmad I. Salvaging fractured porcelain crowns with a direct composite repair technique. Pract Proced Aesthet Dent. 2002;14:233-238.
- Kurtzman GM, Schneider AL. A technique for repair of a fractured porcelain-fused-to-metal bridge. Dent Today. 2006;25:94-95.
- Latta MA, Barkmeier WW. Approaches for intraoral repair of ceramic restorations. Compend Contin Educ Dent. 2000;21:635-639,642-644.
- Reston EG, Filho SC, Arossi G, et al. Repairing ceramic restorations: final solution or alternative procedure? Oper Dent. 2008;33:461-466.
- Terry DA, Leinfelder KF, Trajtenberg CP. Simplifying the luting procedure. Dent Today. 2007;26:130, 132-135.
- Heymann HO. The Carolina bridge: a novel interim all-porcelain bonded prosthesis. J Esthet Restor Dent. 2006;18:81-92.
- Hagiwara Y, Matsumura H, Tanaka S, et al. Single tooth replacement using a modified metal-ceramic resin-bonded fixed partial denture: a clinical report. J Prosthet Dent. 2004;91:414-417.
- Wyatt CC. Resin-bonded fixed partial dentures: what’s new? J Can Dent Assoc. 2007;73:933-938.
- Knight JS, Holmes JR, Bradford H, et al. Shear bond strengths of composite bonded to porcelain using porcelain repair systems. Am J Dent. 2003;16:252-254.
- Della Bona A, Anusavice KJ, Hood JA. Effect of ceramic surface treatment on tensile bond strength to a resin cement. Int J Prosthodont. 2002;15:248-253.
- Filho AM, Vieira LC, Araújo E, et al. Effect of different ceramic surface treatments on resin microtensile bond strength. J Prosthodont. 2004;13:28-35.
- Moharamzadeh K, Hooshmand T, Keshvad A, et al. Fracture toughness of a ceramic-resin interface. Dent Mater. 2008;24:172-177.
Dr. Rada received his DDS from the University of Illinois College of Dentistry and completed a general practice residency at Loyola University. He is currently an associate clinical professor in the Department of Oral Medicine and Diagnostic Sciences at UIC and maintains a private practice in LaGrange, Ill, focusing on restorative and aesthetic dentistry, as well as dentistry for special needs patients and hospital dentistry. He can be reached at (708) 482-3636 or at bobr759@sbcglobal.net.
Disclosure: Dr. Rada reports no conflicts of interest.







