INTRODUCTION
Legal proceedings have a large financial impact and consume a considerable measure of management time and energy, only to sometimes end in the dismal loss of a lawsuit. In some cases, the outcome has resulted in not being able to purchase future malpractice insurance at all. Now, more than ever, it is critical to develop appropriate and effective risk management strategies.
Excellence in dental care includes the performance of thorough and comprehensive extraoral and intraoral examinations. There are many advantages to your practice, including the obvious in reducing your malpractice risk. A comprehensive oral cancer examination serves as the most effective mechanism for protecting your patients’ health, and reducing exposure to claims against you for failing to diagnose properly and may even be a procedure that literally involves saving lives. Every dental examination, including recare appointments, should include the evaluation of tissues for early warning signs (abnormalities) of oral cancer or other mucosal pathologies.
A survey conducted by the ADA revealed that only 15% of patients reported having an oral cancer examination during a routine dental appointment.1 A survey conducted and presented at the 2006 annual session of the American Dental Hygienists’ Association reported that of 1,505 subjects surveyed, only 453 reported having been examined for oral cancer. Overall, 506 indicated that they did not have an examination, and 532 were not certain whether or not an oral cancer examination was performed.2 Unfortunately, the reality is that even though the professional community understands the critical importance of performing the examination, often there is a disconnect in the actual application.
Even when oral cancer screening is part of an examination, many patients remain unaware that it has been performed. It is imperative that the dental patient be informed that you are doing a thorough and comprehensive screening examination, which includes screening for oral cancer. Failing to educate our patients further contributes to the perception that this examination is being overlooked. Furthermore, failing to perform a routine oral cancer screening has unintentionally placed the responsibility on the dental patient to bring the presence of an oral lesion to our attention; often this occurs at the later stages.
Also, of particular interest is that failure to diagnose or delayed diagnosis of oral cancer is the number 2 cause of dental malpractice in the United States; and is among the highest of any type of dental malpractice claim. The average claim is settled for approximately $1,000,000, with the average age of claimants being in their early 40s. One should take note that it is one of the hardest suits to defend against.3 It is not only within the professional standards of practice to refer a suspicious finding, it is an obligation. Suggesting that an abnormal clinical finding was an oversight or did not seem to warrant further investigation would not provide a strong defense in a court of law.
EXTRAORAL AND INTRAORAL EXAMINATIONS
The following is a concise overview of the components of the extraoral and intraoral examination. It stresses a systematic and consistent approach to these examinations. (The order of the examination steps as described herein, is the systematic sequencing that the author uses. The order of the examination steps may vary depending individual clinician-determined protocols.)
Systematic Extraoral Examination
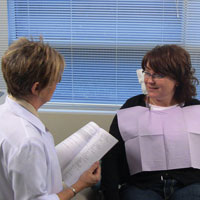
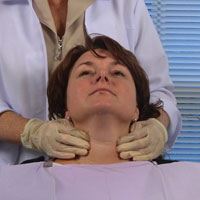
A review and assessment of the systemic health and pharmacological status of the patient is always done prior to any dental examination. The extraoral examination continues with observation of the head and neck, as well as observation of the sound of the patient’s voice and eye movements commencing from when the patient is first seated in the treatment room (Figure 1). Hoarseness in the voice may warrant further investigation if it has been persistent, since this may be an indication/suspicion of a growth within the larynx/oropharynx. Abnormal breathing may be a sign of anxiety or fatigue. Pupil size may signify a reaction to drugs or state of emergency as well as an indication of a disease state or inflammatory presence. The appearance of the face is further evaluated noting any asymmetry, swelling or discoloration. Inspection of the skin includes the color, texture, the presence of eruptions or swellings, or any abnormal growth. Observe all areas of exposed skin, paying particular attention to areas behind the ears and the back of the head and neck. Most people will have freckles, birthmarks, or moles; irregularities or a change in the shape, edge, color, and/or size can be a warning sign of skin cancer thus warranting further investigation.
Have your patients remove their eyeglasses to make certain there are no hidden growths or developments that would have otherwise gone unnoticed. The areas along the hairline and under the eyeglasses will require tactile palpation in order to discern or identify any swellings/growths.
 |
 |
|---|---|
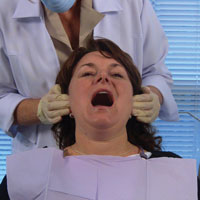
| Figure 1. Initial observation of head and neck, speech, and eye movements. | Figure 2. Examination of the temporomandibular joint. |
 |
 |
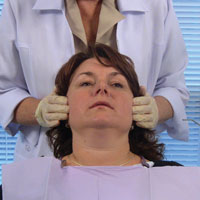
| Figure 3. Bilateral palpation of parotid salivary glands. |
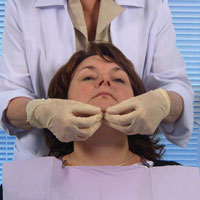
Figure 4. Bilateral palpation of submental nodes. |
 |
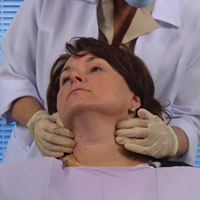 |
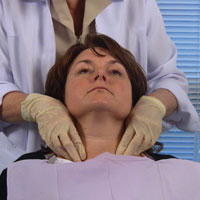
| Figure 5. Bilateral palpation of submandibular nodes. | Figure 6. Bilateral palpation of cervical lymph nodes. |
 |
|
| Figure 7. Bilateral palpation of supraclavicular nodes. | Figure 8. Bilateral palpation of occipital nodes. |
 |
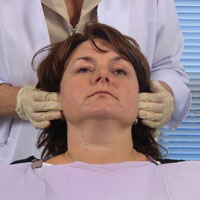 |
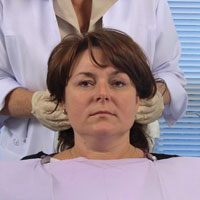
| Figure 9. Bilateral palpation of postauricular nodes. | Figure 10. Bilateral palpation of preauricular nodes. |
Next is the examination of the temporomandibular joint, utilizing a bilateral examination technique (Figure 2). This is accomplished by placing your finger pads over the joint just anterior to the ear; instructing the patient to open and close as well as move the jaw to the left and right; checking for any limitations or deviations upon opening, subluxation, any tenderness, sensitivity or any noises such as a grating, clicking, or popping.
The next area to be examined is the parotid salivary glands (Figure 3). The extraoral palpation of the parotid salivary glands is best examined using a bilateral technique, employing light pressure and placing fingers at the angles of the mandible over the parotid glands. Compare the bilateral findings for symmetry. Normal parotid glands are not palpable and exhibit no tenderness. Abnormal salivary glands may be painful, swollen, and indurated.
The lymph nodes are examined next with the clinician behind the patient and the patient’s chin slightly elevated. Areas of particular concern in a systematic examination can be found in the Table.
It is important to inform the patient as to the relevance of the examination of the lymphatics of the head and neck before commencing this portion of the extraoral examination. In addition, one should indicate what areas of the head and neck will be examined. Due to the diverse multiculturalism that exists within our patient population, we must be culturally aware and sensitive to the different possible comfort levels of our patients.
Evaluation of the lymph nodes is done by a gentle rolling motion of the fingers, using the bilateral palpation technique. Note any enlargement, tenderness, lack of mobility, hardness, or asymmetry. If enlargement is detected, the examiner should determine the mobility and consistency of the nodes. Enlargement or lymphadenopathy may be attributed to either an infectious or inflammatory process or a malignant neoplasm. Clinical characteristics can help discern the difference.
In the broadest clinical terms, the enlarged node, if related to infection, is most often soft, freely movable, and painful. Also, the patient may have presented with an infection (or presence of inflammation) and may occasionally possess some knowledge of the etiology. Malignant neoplasm related nodes are normally fixed, particularly in the later stages, and they are generally not painful. One could compare the consistency of an infection related node to a blueberry or pea, whereas a malignant neoplasm related node is normally firmer in consistency, like a stone.
Next, submental and submandibular nodes should be examined carefully. With the patient’s head back slightly, first examine the submental nodes (Figure 4). Instruct the patient to bite together lightly and place the tongue into palatal vault. This results in a tensing of the mylohyoid muscle, allowing for easier palpation of submental glands. Moving posterior toward the angle of the mandible and palpating directly below the line of the mandible are the submandibular glands (Figure 5).
Another area to examine are the cervical nodes; both superficial and deep nodes. This set forms a complex chain of numerous nodes. Instruct the patient to turn the head in order to reposition the sternocleidomastoid muscle for ease of palpation and better access of both the superficial/deep cervical nodes (Figure 6).
The supraclavicular nodes are palpated next, found superior to the clavicle in the hollow area or supraclavicular fossa directly above the collarbone (Figure 7). They drain a part of the thoracic cavity and abdomen. Virchow’s node is a left supraclavicular node, which receives the lymph drainage from most of the body (especially above the abdomen) via the thoracic duct; this node may serve as an early site of metastasis for various malignancies.
The next nodes to be palpated are the occipital nodes (Figure 8). These are associated with the occipital artery at the posterior base of the skull. Using a bilateral technique, palpation is done directly below the base of the occipital bone. Reclining the patient’s head to the front, exposing the occipital area may facilitate better access for palpation of the occipital nodes.
The posterior auricular, or postauricular, nodes are next in the systematic order of lymph node palpation and are usually 2 in number (Figure 9). The anterior auricular or preauricular nodes are from one to 3 in number and lie immediately in front of the tragus (Figure 10). Both pre- and postauricular nodes’ efferent vessels drain into the superior deep cervical nodes.
The thyroid gland, normally not detected by palpation, is examined next.
An abnormal gland could be indurated, enlarged on one or both sides, or contain palpable nodes. When using bilateral palpation, palpation is done on both sides of the gland, noting any nodules or masses (Figure 11). Instruct your patient to swallow, which in turn will elevate the thyroid gland; allowing for an abnormality to become more apparent. Asymmetrical movement of the thyroid cartilage during swallowing might indicate that the gland is fixed to underlying tissues. If the patient is obese, it may be easier to palpate this area positioned behind the patient, having him or her turn the head toward the examining side. Suspicious thyroid gland findings should be referred to your patient’s physician for further evaluation.
Systematic Intraoral Examination
It is best to follow a systematic and consistent approach when performing the intraoral examination. The following is a suggested 7-step systematic approach:
Step 1: Inspect the lips with the patient’s mouth both closed and open. The lips should have a normal/well-defined vermilion border and be even in coloration. Use the method of bidigital palpation to note any swelling, indurations or observed texture or color change (Figure 12). Documentation when dryness and/or unclear demarcation of lip vermillion and skin exist should be noted as “lip at risk” to flag the area for subsequent examinations. Also examine for loss of vertical dimension manifested often on labial commissures with the outcome being angular cheilitis. Further investigation to determine the causative factor behind the loss of vertical dimension would be warranted. Reinforce the need for sunblock protection, especially related to those patients who ar
e active outdoors and have prolonged exposure to sunlight. Sunblock protection for the lips has had a positive effect on reducing the number of cancers related to the lip.
Step 2: Inspect the labial mucosa using a visual and tactile method (Figure 13). This is accomplished with the patient’s mouth partially open, allowing examination of the labial mucosa and sulcus of the maxillary and mandibular vestibule and frenum.
Step 3: Inspect the buccal mucosa using visual inspection and tactile palpation (Figure 14). This is best accomplished by using a bidigital palpation technique with the thumb placed against the buccal mucosa simultaneously with external palpation, noting any change in pigmentation, texture or diminished mobility or other abnormalities of the mucosa. Inspect the parotid gland from the intraoral aspect at this time as well as palpating both the maxillary tuberosities and retromolar pads.
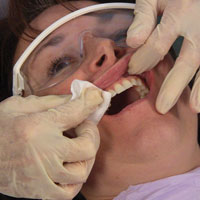
Step 4: Examine the gingival tissues. Observe attached and free gingiva on both arches, assessing for normal color and contour using digital palpation. Use a 2-x-2 gauze to dry the tissues to provide an enhanced assessment (Figure 15).
Step 5: Inspect all surfaces of the tongue. The tongue is a very high-risk area for oral cancer as well as for candida infections. Candida infections can be an indication of an underlying systemic disease. The tongue should be examined thoroughly using both visual and tactile methods. Visual inspection alone is inadequate in its ability to identify early changes to the mucosal surface of the tongue. It is best to follow a systematic approach when inspecting the tongue, commencing with examination of the dorsum, then lateral borders and concluding with the ventral surface.
The dorsum is the first area of the tongue to be examined. Ask the patient to protrude the tongue, moving from side to side, noting any abnormality of mobility or restriction of movement. With the patient’s tongue at rest, and mouth partially open, inspect and palpate the dorsum of the tongue to detect any swelling or fixed mass (Figure 16).
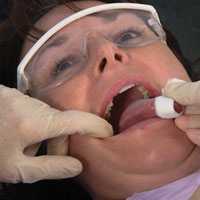
Following inspection of the dorsum, examine the lateral borders. A common site for oral cancer is on this lateral aspect of the tongue. With retraction of the cheek, inspect the left and right lateral margins of the tongue. Handling the tip of the tongue with a piece of gauze will assist full protrusion and will aid examination of the more posterior aspects of the tongue’s lateral borders, including the lingual tonsils (Figure 17). With the tongue fully protruded (held and manipulated forward and side by side by the clinician for optimal visual access), inspect the posterior aspect and base of tongue using digital palpation along the lateral borders to identify any changes in tissue texture or consistency, noting any swelling/induration. If detected, compare with the opposing lateral border. Be suspicious of an abnormality that is unilateral.
The last area of the tongue to be examined is the ventral surface. Instruct the patient to touch the roof of the mouth with the tip of the tongue (Figure 18). This will allow full inspection of the ventral surface of the tongue. Digitally palpate the ventral surface of the tongue to aid in any detection of growths, swelling or area of tenderness, as well as any color or texture changes. Observe for any asymmetry, comparing one side to the other.
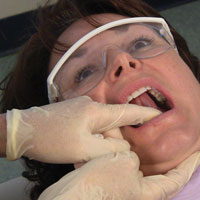
Step 6: Examine the floor of the mouth carefully, keeping in mind that this is another highly vulnerable area that requires close and thorough inspection. Areas are easily hidden from visual inspection. With the tongue still elevated, inspect the floor of the mouth for changes in color, texture, swellings, or other surface abnormalities. Using bimanual palpation, compress the floor of mouth against the opposite hand (Figure 19). This is the only effective way to identify any area of firmness or mass as well as locating any feeling of tenderness.
Step 7: Inspection of the oropharynx and palatal tissues. Check the entire area of the oropharynx, examining the tonsil region including the uvula, tonsillar pillars, and palatine tonsils for presence, color, size, or any noted abnormalities. When examining the oropharynx, it is best to depress the tongue down toward the floor of the mouth using either a tongue blade or the back of the mouth mirror while instructing the patient to take a deep breath and hold or say “ah” (Figure 20). This method enables the clinician to gain better visual access of the oropharynx area. The soft palate should be visually examined next, accompanied by digital palpation of the hard palate, noting any asymmetries, swelling or mucosal changes.
ADJUNCTIVE SCREENING METHODS
The purpose of this article is to provide a pathway of decision making rather than an endorsement of a specific order of examination or the use of specific screening devices. There are a number of adjunctive screening technologies that are available and continue to emerge in the dental marketplace. It is vitally important to recognize that adjunctive screening technologies can provide valuable additional information (beyond the visual and tactile examination process) for further evaluation/assessment. A definitive diagnosis is obtained through a surgical biopsy to either rule out a malignancy or establish another diagnosis. This can sometimes be done in conjunction with other special testing methods.
When lesions are found that are highly suspect, the need for a referral becomes evident. Adjunctive screening devices can serve as a critical component in our decision making, particularly those that aid identification of an abnormal finding before it becomes visible under traditional white light examination.
 |
 |
|---|---|
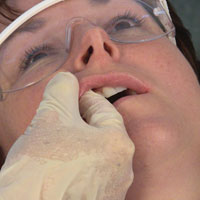
| Figure 11. Bilateral palpation of the thyroid gland. | Figure 12. Bidigital palpation of lips. |
 |
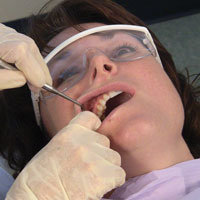 |
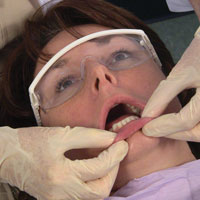
| Figure 13. Palpation of the labial mucosa. | Figure 14. Examination of buccal mucosa. |
 |
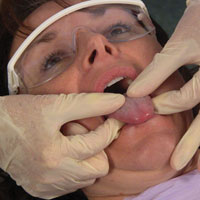 |
| < strong>Figure 15. Examination of the gingival tissues. | Figure 16. Palpation of dorsum of tongue. |
 |
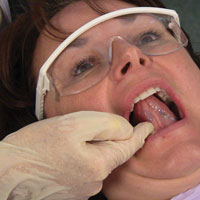 |
| Figure 17. Examination of lateral borders of tongue. | Figure 18. Palpation of the ventral surface of the tongue. |
 |
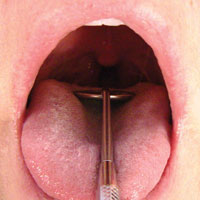 |
| Figure 19. Bimanual palpation of floor of mouth. | Figure 20. Examination of oropharynx and palatal tissues. |
Many epithelial lesions typically start below the surface of the tissue, at the basement membrane, and can remain occult until they reach the surface, making earlier discovery more challenging. There are a number of light-based detection systems used to enhance visualization techniques. One must be careful to not be pulled into the marketing rhetoric rather than evidence-based research and scientific data. The weakest science involves tissue reflectance.
A technique referred to as direct fluorescence visualization is supported by a strong body of scientific evidence related to its inherent ability to detect cancers and high-risk lesions including occult or nonapparent lesions or areas.4 This technique has a long history of use in other body sites such as the cervix, lungs, and colon.
Direct fluorescence visualization works on the premise of the ability of human tissue to fluoresce due to naturally occurring fluorophores in oral mucosa under excitation with a specific wavelength and intensity. By utilizing special optical filters, the clinician is able to immediately view different fluorescence patterns in the oral tissue to help differentiate between normal and abnormal cellular activity. When normal tissue is exposed to the blue excitation light, it will emit an apple-green glow. As dysplasia begins to develop, there is a breakdown in the stroma and specifically in the connective tissue or collagen cross-links coupled with a reduction in the naturally occurring fluorophores greatly diminishing the ability of the tissue to fluoresce. This allows for real-time feedback of an irregular dark area, presenting a stark contrast to the surrounding tissue that appears as an apple-green glow.
The advantages of the examination are its relative ease in implementation and patient comfort. The examination is noninvasive and does not involve any additional rinses or dyes. It also provides photo documentation for means of evaluation, referral and management.
| Are We Limiting Our Professional Standard of Care for Diagnosis? |
|
Ronald C. McGlennen, MD References
Dr. McGlennen is the chief medical officer of OralDNA Labs, a leading provider of salivary diagnostic tests such as the OraRisk HPV Test to the dental profession, and a subsidiary of Quest Diagnostics Incorporated. Dr. McGlennen is board certified in anatomic and clinical pathology, and also board certified by the American Board of Medical Genetics, with a specialty in clinical molecular genetics. He is internationally recognized as an expert in Molecular Biology and Genetics. He can be reached at (952) 942-0671, via e-mail at [email protected] or at access-genetics.com. Disclosure: Dr. McGlennen serves as the medical director of OralDNA Labs Inc, which offers testing for salivary diagnostics. He is president and medical director of Access Genetics, which sells materials and consultative support to OralDNA Labs, Inc. |
Vital staining of a mucosal lesion using pharmaceutical grade 1% tolonium chloride or toluidine blue (referred to as TBlue) is an adjunctive aid as a tissue marker that has been utilized for more than 40 years. TBlue is applied to the tissue and then decolorized. The decolorization is done with reapplication of the acetic acid. The dye has an affinity for nuclear material with a high DNA or RNA content which supports its selective concentration in dysplastic or malignant cells within the oral epithelium.
The “brush test” (previously known as the oral brush biopsy) is part of the diagnostic process rather than the discovery process, as it further examines an already visible clinical finding. Further limitations of a brush test refer to the fact that only individual cells are examined, thus eliminating the opportunity to evaluate in their proper tissue relationships. A positive result must be followed with a full-thickness biopsy (can be either incisional or excisional) in order to further determine the extent and nature of the disease process.
Our task is simply to discover, not diagnose, an abnormal clinical finding. There are several data points to consider which are enhanced by the use of adjunctive screening devices such as:
- Has the tissue become friable, exophytic, indurated, etc?
- Does the tissue manifest a loss of autofluorescence?
- Is the tissue picking up tolonium chloride?
- Has the lesion existed for more than 14 days?
- Is there an absence of an identified etiology?
|
WHAT DOES THE FUTURE HOLD?
A closer look at molecular biology, specifically genomics and proteomics through examination of the saliva may be the breakthrough to deriving rich genetic information. In a major step towards earlier diagnosis of oral cancer, Wong5 (University of California’s Los Angeles School of Dentistry) has identified 5 biomarkers for the disease utilizing salivary diagnostics.5 The possibility of a simple saliva test for oral cancer has moved one step closer to reality. Determining genetic predisposition and examination of direct behavior of cellular activity will add a new dimension to screening. This will enable more people to be moved toward accelerated monitoring by means of sifting through huge populations, resulting in a revolutionary change in disease management.
CONCLUSION
Consider the quote by Charles Darwin, who was the first of evolutionary biologists and certainly no stranger to change, “It is not the strongest of the species that survives, nor the most intelligent, but the one most responsive to change.” We have, as a professional community, every opportunity to write our own success stories related to opportunistic screening and to be a catalyst for change. As a wise family friend once wrote in my autograph book in my teenage years, “Your life is like a path of snow; walk carefully for every step will show.” The power is within your own hands to impact this insidious disease and change the face of oral cancer. It is your practice, your legacy, and your responsibility.
Acknowledgement
All photographs and accompanying video appear with permission from the Canadian Dental Hygienists’ Association. Additional practice resources to support the endeavors of the professional community to elevate oral cancer awareness are available through the Web site cdha.ca and the online course, “Oral Cancer Awareness—4 Life Saving Minutes: The Extraoral and Intraoral Examination.” The author also wishes to acknowledge Brian Hill, the founder of the Oral Cancer Foundation (oralcancerfoundation.org) for his insight and direction in development of this article.
References
- Horowitz AM, Drury TF, Goodman HS, et al. Oral pharyngeal cancer prevention and early detection. Dentists’ opinions and practices. J Am Dent Assoc. 2000;131:453-462.
- Hein C, Kunselman B, Frese P. Preliminary findings of consumer-patient’s perceptions of dental hygienists’ scope of practice/qualifications and the level of care being rendered. American Dental Hygienists’ Association Annual Session, Orlando Fla, June 21 to 28, 2006.
- Bregman JA. Early oral cancer detection: Why you? Why n
ow? oralcancernews.org/wp/early-oral-cancer-detection-why-you-why-now. Accessed on: February 19, 2010. - Poh CF, Zhang L, Anderson DW, et al. Fluorescence visualization detection of field alterations in tumor margins of oral cancer patients. Clin Cancer Res. 2006;12:6716-6722.
- Wong DT. Salivary diagnostics powered by nanotechnologies, proteomics and genomics. J Am Dent Assoc. 2006;137:313-321.
Ms. Jones is an international speaker for the profession of dental hygiene and the owner of RDH CONNECTION, a consulting and training company dedicated to excellence in quality dental hygiene education. Having a career that has spanned over 3 decades, Ms. Jones’ experience has encompassed clinical practice, education, international lecturing, and is published internationally. She has been appointed to serve on the advisory board for Dentistry Today and is one of Dentistry Today’s 2011 Leaders in Dental Consulting. She can be reached via e-mail at [email protected] or at the Web site rdhconnection.com.
Disclosure: Ms. Jones reports no disclosures.


