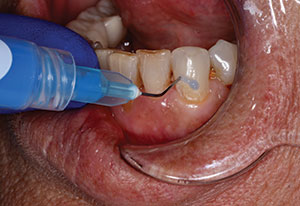
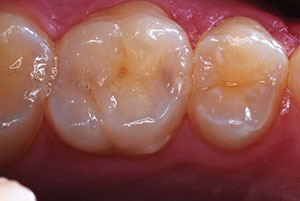
A dimensionally accurate impression is one of the primary determinants for a precise fitting indirect restoration. The clinical success of the indirect restoration requires a precise working model and thus depends upon the accuracy of the final impression.1 The use of custom fabricated trays with elastomeric impression materials can improve the accuracy of the working model.2 There are a myriad of materials and techniques available for custom tray fabrication, including autopolymerizing and heat-activated acrylic resins, thermoplastic resins, and visible light-cured resins. The techniques for custom tray fabrication also vary and range from direct intraoral techniques to indirect laboratory procedures on a primary model.
CONSIDERATION FACTORS FOR FABRICATION AND UTILIZATION OF THE CUSTOM IMPRESSION TRAY
Visible light-cured resins exhibit dimensional stability immediately after curing, thus allowing immediate clinical use after fabrication.5,12 Research indicates that autopolymerizing acrylic resins should be fabricated 24 hours before the impression procedure.5,13 The dimensional stability of elastomeric impression materials is considered to depend on the bulk of material which is the distance from the inner surface of the tray to the surface of the impression.4,14,15 Elastomeric impression materials are considered most stable when they have a uniform thickness of 2 to 4 mm.16 Incorporating dental and/or tissue stops can provide a uniform impression material thickness of approximately 2 to 4 mm.17,18
 |
 |
|
Figure 1. Evaluate the stone model for potential undercuts and design the form and dimension of the tray. Diagram with a margin liner pencil the boundaries of the wax spacer (red), borders of the custom tray (blue) and the occlusal stops (blue). |
Figure 2. Heat and adapt layers of base plate wax to the diagnostic model to obtain a 2 to 4 mm thickness following the predetermined guide marks. Occlusal stops are made with a scalpel blade (No. 12 disposable Bard Parker) and positioned to provide a tripod-like stability. |
 |
 |
 |
|
Figures 3a to 3c. The light-cured material is applied over the spacer and carefully adapted to the pre-determined design. After adapting the material to the anticipated boundaries, the excess material is excised using a scalpel blade (No. 12 disposable [Bard Parker]). (a) A central handle and detachment wings are shaped and contoured. (b,c) These posterior lateral detachment wings provide axial traction for a uniform removal of the tray. |
 |
 |
|
Figures 4a and 4b. After an air barrier coating (Triad air barrier coating [DENTSPLY]) is applied over the tray material, the custom tray is placed in the light-curing unit and undergoes 2 polyme rizations of 5 minutes each. |
Adapting the visible light-cured resin material directly over the wax spacer may leave a wax residue remaining in the tray. This residue contamination can interfere with adhesion of elastomeric impression materials to the impression tray. Even a small release of the impression material can cause a distortion in the impression, so this is critical. Surface cleaning of the tray using boiling water, pressurized steam and/or a wax remover is suggested. Another recommended method involves burnishing tin foil over the wax spacer.19
 |
 |
|
Figures 5a and 5b. The polymerized custom tray, while still on the diagnostic model, is immersed in boiling water for several minutes. The spacer wax is removed and the air barrier is applied to the internal surface of the tray and placed in the light-curing unit for an additional 5 minutes to cure the interior surface. After pressure steaming the internal surface, a wax remover is applied to the internal surface of the tray to remove any residual wax residue. |
 |
 |
|
Figure 6. The tray is evaluated on the diagnostic model and any sharp edges or irregularities are smoothed with a tungsten carbide bur (H251Q [Brasseler USA]). To improve retention of the impression material, perforations are made with a carbide bur (H379 [Brasseler USA]). |
Figure 7. Completed visible light-cured custom tray. |
 |
 |
|
Figure 8. Evaluation of the custom tray in the patient’s mouth for proper extension, stability and orientation. |
Figure 9. A thin layer of adhesive is applied to the internal surface of the tray and should extend several millimeters beyond the borders of the tray. The adhesive is allowed to dry for at least 15 minutes prior to the impression procedure. |
 |
 |
 |
|
Figures 10a to 10c. A precise, predictable, and dimensionally accurate elastomeric impression is obtained using a visible light-cured custom tray (a,b). Cross-sectional view of the custom impression tray, illustrating a uniform thickness of material throughout the tray (c). |
It is essential that the impression material be securely attached to the tray, especially during removal of the set material from the oral cavity. Surface preparation of the custom tray can significantly affect the retention of the impression material and can improve adhesion between impression material and tray. Methods for improving retention/adhesion include: perforating or roughening of the custom tray surface with tungsten carbide burs and application of adhesive solutions.20,21
FABRICATION AND UTILIZATION OF THE VISIBLE LIGHT-CURED CUSTOM IMPRESSION TRAY
The main objective in tray construction is to provide a rigid tray for retention of the impression material. The aforementioned consideration factors can provide insight into the optimal fabrication and utilization of the custom tray. A visible light-cured resin material (Palatray XL [Heraeus Kulzer]) was selected for its rigidity, high dimensional stability, ease of manipulation, and unrestricted working time. Also, this material provides the ability to be ideally contoured prior to curing, thus eliminating prolonged finishing times. Other visible light-cured resins include Individo Lux (VOCO), Triad (DENTSPLY International), and Fastray LC (Bosworth Products).
References
- Terry DA, Leinfelder KF, Geller W. Aesthetic & Restorative Dentistry: Material Selection & Technique. Stillwater, Minn: Everest Publishing Media; 2009.
- Gordon GE, Johnson GH, Drennon DG. The effect of tray selection on the accuracy of elastomeric impression materials. J Prosthet Dent. 1990;63:12-15.
- Bomberg TJ, Hatch RA, Hoffman W Jr. Impression material thickness in stock and custom trays. J Prosthet Dent. 1985;54:170-172.
- Eames WB, Sieweke JC, Wallace SW, et al. Elastomeric impression materials: effect of bulk on accuracy. J Prosthet Dent. 1979;41:304-307.
- Thongthammachat S, Moore BK, Barco MT II, et al. Dimensional accuracy of dental casts: influence of tray material, impression material, and time. J Prosthodont. 2002;11:98-108.
- Johnson GH, Craig RG. Accuracy of addition silicones as a function of technique. J Prosthet Dent. 1986;55:197-203.
- Wassell RW, Ibbetson RJ. The accuracy of polyvinyl siloxane impressions made with standard and reinforced stock trays. J Prosthet Dent. 1991;65:748-757.
- Burns J, Palmer R, Howe L, et al. Accuracy of open tray implant impressions: an in vitro comparison of stock versus custom trays. J Prosthet Dent. 2003;89:250-255.
- Ceyhan JA, Johnson GH, Lepe X, et al. A clinical study comparing the three-dimensional accuracy of a working die generated from two dual-arch trays and a complete-arch custom tray. J Prosthet Dent. 2003;90:228-234.
- Millstein P, Maya A, Segura C. Determining the accuracy of stock and custom tray impression/casts. J Oral Rehabil. 1998;25:645-648.
- Mitchell JV, Damele JJ. Influence of tray design upon elastic impression materials. J Prosthet Dent. 1970;23:51-57.
- Ogle RE, Sorensen SE, Lewis EA. A new visible light-cured resin system applied to removable prosthodontics. J Prosthet Dent. 1986;56:497-506.
- Goldfogel M, Harvey WL, Winter D. Dimensional change of acrylic resin tray materials. J Prosthet Dent. 1985;54:284-286.
- McCabe JF, Storer R. Elastomeric impression materials. The measurement of some properties relevant to clinical practice. Br Dent J. 1980;149:73-79.
- Valderhaug J, Fløystrand F. Dimensional stability of elastomeric impression materials in custom-made and stock trays. J Prosthet Dent. 1984;52:514-517.
- Phillips RW, Skinner EW. Skinner’s Science of Dental Materials. 8th ed. Philadelphia, Pa: WB Saunders Co; 1982:149-150.
- Brown D. Factors affecting the dimensional stability of elastic impression materials. J Dent. 1973;1:265-274.
- Ortensi L, Strocchi ML. Modified custom tray. J Prosthet Dent. 2000;84:237-240.
- Johnston JF, Phillips RW, Dikema RW. Modern Practice in Crown and Bridge Prosthodontics. 3rd ed. Philadelphia, Pa: WB Saunders Co; 1971:181.
- Maruo Y, Nishigawa G, Oka M, et al. Tensile bond strength between custom tray and elastomeric impression material. Dent Mater J. 2007;26:323-328.
- Abdullah MA, Talic YF. The effect of custom tray material type and fabrication technique on tensile bond strength of impression material adhesive systems. J Oral Rehabil. 2003;30:312-317.
- Cho GC, Donovan TE, Chee WW, et al. Tensile bond strength of polyvinyl siloxane impressions bonded to a custom tray as a function of drying time: Part 1. J Prosthet Dent. 1995;73:419-423.
Dr. Terry is a clinical assistant professor in the Department of Restorative Dentistry and Biomaterials, at the University of Texas Health Science Center Dental Branch at Houston. He is a member and the US vice president of International Oral Design. Dr. Terry is the founder and CEO of design Technique International and the Institute of Esthetic and Restorative Dentistry. He maintains a private practice in Houston, Tex. Dr. Terry is an editorial member of numerous peer-reviewed scientific journals and has published over 230 articles on various topics in aesthetic and restorative dentistry. He has authored the textbooks Natural Aesthetics with Composite Resin and Aesthetic & Restorative Dentistry: Material Selection & Technique. He has lectured internationally on various subjects in restorative and aesthetic dentistry. He can be reached at (281) 481-3483 or via e-mail at dterry@dentalinstitute.com.
Disclosure: Dr. Terry reports no conflicts of interest.
Mr. Tric is a master ceramist and specializes in the many facets of porcelain aesthetic restorations on both natural teeth and osseointegrated implants. He is a member of Oral Design International and currently owns and operates a dental laboratory and an educational center for Oral Design in Elmhurst, Ill. He serves on the editorial board of Spectrum and has authored numerous scientific articles on ceramic layering techniques and aesthetic dentistry. He is a consultant in the area of new product development and clinical testing of materials for dental manufacturers and laboratories. Mr. Tric has lectured and given hands-on courses to dentists and technicians throughout the United States and Europe. He can be reached via e-mail at oliviertric@ameritech.net.
Disclosure: Mr. Tric reports no conflicts of interest.
Dr. Blatz graduated and received an additional Doctorate as well as a postgraduate certificate in Prosthodontics from the University of Freiburg, Germany. He is currently a professor of Restorative Dentistry and Chairman of the Department of Preventive and Restorative Sciences at the University of Pennsylvania School of Dental Medicine. Dr. Blatz is a Diplomate of the German Society of Prosthodontics and Material Sciences. He is an editorial board member of numerous peer-reviewed scientific dental journals. He is a member of multiple professional organizations, including the European Academy of Esthetic Dentistry and OKU Honor Dental Society. Dr. Blatz has published and lectured extensively on various facets of restorative dentistry, implantology, and dental materials. He can be reached at (215) 573-3959 or via e-mail at mblatz@dental.upenn.edu.
Disclosure: Dr. Blatz reports no conflicts of interest.
Dr. Burgess graduated from Emory University School of Dentistry and completed graduate training at the University of Texas Health Science Center in Houston. He completed a General Practice Residency and a General Dentistry Residency in the Air Force. He is currently the assistant dean for Clinical Research and the director of the Biomaterials Graduate Program at the University of Alabama in Birmingham. Dr. Burgess maintains a part-time private practice in Birmingham, Ala. Dr. Burgess reviews for 4 dental journals, is the author of more than 300 journal articles, textbook chapters and abstracts, and has presented more than 800 continuing education programs internationally. He is an active investigator on clinical trials evaluating posterior composites, adhesives, fluoride releasing materials, impression materials, and Class V restorations. He can be reached at (205) 996-5796 or via e-mail at jburgess@uab.edu.
Disclosure: Dr. Burgess reports no conflicts of interest.