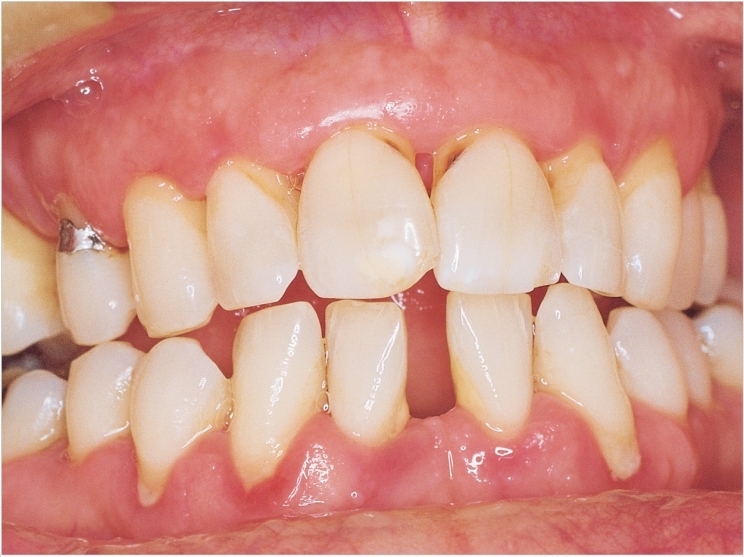
As researchers continue to probe the links between oral and systemic health, independent studies in Europe and the United States underscore the potential connections between periodontitis and various forms of cancer, with a particular look at how oral bacteria may trigger onset of the disease.
Bacteria and Cancer
Researchers at the University of Helsinki, the Helsinki University Hospital, and the Karolinska Institutet have investigated the role of bacteria that cause periodontitis in developing oral and certain other cancers as well as the link between periodontitis and cancer mortality on the population level.
Their work has proven for the first time, the researchers said, the existence of a mechanism on the molecular level through which Treponema denticola (Td) also may have an effect on the onset of cancer. The primary virulence factor of Td, the Td-CTLP proteinase, also occurs in malignant tumors in the gastrointestinal tract such as pancreatic cancer.
The CTLP enzyme can activate the enzymes that cancer cells use to invade healthy tissue (pro-MMP-8 and pro-MMP-9). At the same time, CTLP also diminishes the effectiveness of the immune system by, for example, inactivating molecules known as enzyme inhibitors.
In another study, the researchers proved on the population level that periodontitis is linked with cancer mortality, with an especially strong link to mortality caused by pancreatic cancer. Some 70,000 Finns took part in the this 10-year follow-up study.
“These studies have demonstrated for the first time that the virulence factors of the central pathogenic bacteria underlying gum disease are able to spread from the mouth to other parts of the body, most likely in conjunction with the bacteria, and take part in central mechanisms of tissue destruction related to cancer,” said Timo Sorsa, a professor at the University of Helsinki.
The researchers concluded that a low-grade systemic inflammation related to periodontitis facilitates the spread of oral bacteria and their virulence factors to other parts of the body. They noted that the prevention and early diagnosis of periodontitis are very important for patients’ oral health and their overall wellbeing.
“In the long run, this is extremely cost-effective for society,” Sorsa said.
More Correlations
The American study used data from comprehensive dental exams performed on 7,466 participants from Maryland, Minnesota, Mississippi, and North Carolina as part of their participation in the Atherosclerosis Risk in Communities (ARIC) study who were followed from the late 1990s until 2012. During the follow-up period, 1,648 new cancer cases were diagnosed.
The research team found a 24% increase in the risk of developing cancer among participants with severe periodontitis compared to those with mild to no periodontitis at baseline. Among patients who had no teeth, which can be a sign of severe periodontitis, the increase in risk was 28%. The highest risk was observed in cases of lung cancer, followed by colorectal cancer.
Subgroup analyses found that subjects with severe periodontal disease had more than double the risk of developing lung cancer than those with no or mild periodontitis. Subjects who were edentulous at baseline had an 80% increase in risk of colon cancer, which is consistent with prior findings. Subjects who had never smoked but had severe periodontitis saw a twofold higher risk than those who had never smoked with no or mild periodontitis.
“This is the largest study addressing the association of gum disease and cancer risk using dental examinations to measure gum disease prior to cancer diagnosis,” said first and corresponding author Dominique Michaud, ScD, professor of public health and community medicine at the Tufts University School of Medicine.
“Additional research is needed to evaluate if periodontal disease prevention and treatment could help alleviate the incidence of cancer and reduce the number of deaths due to certain types of cancer,” said Michaud.
Michaud noted that the findings were particularly interesting in light of research, including a recent study in Science, that determined that colorectal cancer tissues include bacteria that are present in the mouth, including bacteria that have been associated with periodontal disease.
The researchers also uncovered a small increase in the risk of pancreatic cancer in patients with severe periodontitis. Although not significant statistically, the association has not been seen in other studies. They accounted for the impact of smoking as well, since smoking increases the risk of periodontal disease as well as lung and colon cancers.
“When we looked at data for the people who had never smoked, we also found evidence that having severe periodontal disease was related to an increased risk of lung cancer and colorectal cancer,” said Elizabeth Platz, ScD, deputy chair of the department of epidemiology at the Johns Hopkins Bloomberg School of Public Health and co-leader of the Cancer Prevention and Control Program at the Johns Hopkins Sidney Kimmel Cancer Center.
The researchers found the ARIC data especially useful because unlike most research linking gum disease and cancer risks, periodontitis cases were determined from dental examinations performed as part of the ARIC study rather than participants’ self-reports of the disease. The dental exams provided detailed measurements of the depth of the pocket between the gum and tooth in several locations in the mouth.
The ARIC data also included Caucasian and African-American participants. While the researchers found no links between increased risk of breast, prostate, or blood/lymphatic cancer and periodontitis, the link between periodontitis and increased cancer risk was weaker or not apparent in African-American participants from the ARIC study, except in cases of lung and colorectal cancer.
According to the researchers, additional work is necessary to understand cancer-site specific and racial differences in their findings. They also caution that the study was limited in size for subgroup analyses and less common cancers. However, they noted, the findings do suggest the need for further study. Furthermore, the study points to the importance of expanding dental insurance to more individuals, they said.
“Knowing more about the risks that come about with periodontal disease might give more support to having dental insurance in the way that we should be offering health insurance to everyone,” Platz said.
Further Reading
The first European study, “Treponema Denticola Chymotrypsin-Like Proteinase May Contribute to Orodigestive Carcinogenesis Through Immunomodulation,” was published by the British Journal of Cancer.
The second European study, “Periodontitis and Cancer Mortality: Register-Based Cohort Study of 68 273 Adults in 10-year Follow-up,” was published by the International Journal of Cancer.
The American study, “Periodontal Disease Assessed Using Clinical Dental Measurements and Cancer Risk in the ARIC Study,” was published by the Journal of the National Cancer Institute.
Related Articles
Different Microbiomes May Cause Gingivitis and Periodontitis
Oral Bacteria Tied to Esophageal Cancer
Periodontal Disease Increases Lung Cancer Risks











