Advances in medical imaging, computer-aided design (CAD), and computer-aided manufacturing (CAM) are changing the traditional processes used in dentistry. Cone beam computed tomography (CBCT) along with laser and light imaging systems provide precise, 3-dimensional information about our patients. This data is as accurate as conventional techniques and can be sent via the Internet to any individual involved in the patient’s treatment. This information can also be used to manufacture any number of dental devices used in patient treatment.1-3
Electron beam melting (EBM) is a new method of creating fully dense dental devices in titanium. This new technology has the potential to transform the way dental rehabilitation is accomplished by integrating the treatment process to produce dental devices directly from digital information. Custom dental implants and dental restorations can be manufactured with this process. EBM is an additive fabrication process that uses a high-power electron beam to selectively melt 0.05- to 0.1-mm thick layers of titanium metal powder (Figure 1). Successive layers of powder are deposited, and the electron beam selectively melts the surface of each layer to create a 3-D part. This process makes it possible to manufacture fully dense titanium structures.4
 |
|
Figure 1. Arcam electron beam melting system (Arcam AB). |
 |
|
Figure 2. CAD model of the surface that contacts tissue and connects to the dental implants (left). Actual titanium part created from the CAD file with the EBM process (right). |
ELECTRON BEAM MELTING
Most dentists are familiar with stereolithography; this additive manufacturing process is used to create medicalmodels, surgical drill guides, and the parts used in the Invisalign (Align Technology) manufacturing process. Each stereolithography part is built a layer at a time by selectively curing a liquid photopolymer with a laser. EBM creates parts in a similar way by selectively melting titanium powder in a vacuum chamber. Each layer represents a cross-section of the CAD model of the dental prosthesis. Each successive layer of titanium is melted to the previous one with the electron beam, and the unmelted powder provides support for the device during the building process. Once the part is complete, excess titanium power is removed and the device is ready for machining. The completed part is fully dense5 but not as precise as the original CAD model (Figure 2). Generally, the process occurs over a 24-hour period of time, and currently available machines can create 12 to 15 frameworks per cycle.
NUMBER CONTROLLED (NC) MILLING
 |
|
Figure 3. Milled titanium surface (left) and polished titanium surface (right). |
The titanium part must now be milled to precise tolerances to fit accurately to dental implants and to have a shape that is hygienic and aesthetic. A 5-axis mill is used to machine the surface and to create holes for the retentive screws. Figure 3 illustrates the machined surface after the initial tool paths, and the polished surface with laboratory analogues attached. The occlusal surface of the titanium part must also be milled and then covered with a pink opaque surface to improve the aesthetics of the completed prosthesis.
The CAD design for the part has titanium struts that extend into the artificial teeth to increase the strength and retention of the processed teeth. The virtual design for the position of artificial teeth and the titanium substructure is created by imaging the patient’s provisional restoration and making any necessary changes (Figure 4). NC milling can create a very precise surface, but some aspects of the metal substructure can only be created with EBM; these include the unique retentive surface of EBM titanium and the undercut areas that cannot be milled. EBM parts also require much less time to mill since the parts are a “near net” shape after they come out of the EBM machine and only require the outer 50 to 150 µm surface to be removed. Conventional milling starts with a large blank of titanium metal that must be reduced with numerous tool paths to create the shape of the metal substructure.
VIRTUAL TREATMENT PLANNING
 |
|
Figure 4. Virtual design of prosthesis (left) and opaque metal substructure (right). |
 |
|
Figure 5. Virtual treatment plan and clinical view of implant placement. |
Cone beam CT is commonly used to plan for implant treatment. Generally the 3-D rendering of bone is used to determine the proper placement and size of dental implants and to create a computer generated drill guide with stereolithography. In addition to the implants, it is also possible to plan for the actual restoration prior to implant placement. This provides the benefit of knowing how much restorative space is available for restorative materials and the proper contours that are needed for good aesthetics and hygiene. This 3-D model of the implants, bone, restoration, and drill guide can easily be sent to the referring dentist or surgeon via the Internet to coordinate treatment and provide excellent communication.6 Any object that can be visualized from the CT data or can be scanned directly can be joined in virtual space to create a composite computer model. The model (Figure 5, left) joins CT data with virtual implants, artificial teeth, and the shape of the drill guide into one composite 3-D image. This makes it possible to ideally plan the position of dental implants (Figure 5, right).
IDEAL AESTHETICS
 |
|
Figure 6. Tooth wax-up (left) and clinical view of finished prosthesis (right). |
 |
|
Figure 7. Preoperative (left) and post-treatment views (right). |
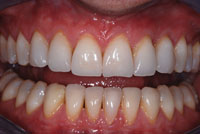
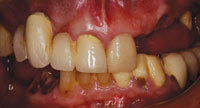
Generally, ideal aesthetic results are possible for patients who will have all their teeth removed (Figures 6 and 7). Since the pretreatment vertical dimension and tooth position are known from initial imaging, it is possible to select the correct virtual tooth for a given patient and to position the teeth with the proper spatial relationship to the patient’s lips, natural head position, and midline. Virtual treatment planning can determine the ideal position for restorative components, and by using computer-generated drill guides it is possible to create the best environment for the manufacture of the final restoration using advanced techniques. This same technique can be used to make fixed maxillary restorations with excellent aesthetics, speech, and contours.
CHANGING DEMOGRAPHICS
Over the past 50 years the percentage of patients wearing dentures has been dramatically reduced due to improved dental techniques and preventive care. Unfortunately, although the percentage of people without teeth has been reduced, the aging babyboom generation is large and their life expectancy continues to lengthen. This means that more patients will require dentures or a more ideal aesthetic treatment such as fixed implant-retained prosthetics. New techniques such as EBM provide an excellent alternative to conventional dentures, and are a very aesthetic, predictable, and cost-effective alternative to conventional dental treatment.
CONCLUSIONS
The present process of diagnosis and treatment in dentistry is undergoing a dramatic transformation. The highly successful methods of treatment developed in the last century are being replaced by new more accurate, efficient, and cost-effective technologies. As we begin the 21st century, medical and dental use of digital imaging, computer-aided design, additive manufacturing, milling, and the Internet will improve the quality of care, improve communication, and reduce costs.
References
- Schmitt SM. “Output”: the final step in digital diagnosis and treatment. Academy News: quarterly publication of Academy of Osseointegration. 2004;15:1,8-9.
- Schmitt SM. Dental lab technology in the digital age. J Dent Technol. 2001;18:18-21.
- Schmitt S, Shirley J, Jones J. Digitally designed denture attachments. Collaborative Techniques. 2003;3:4-6.
- Winder J, Bibb R. Medical rapid prototyping technologies: state of the art and current limitations for application in oral and maxillofacial surgery. J Oral Maxillofac Surg. 2005;63:1006-1015.
- Cormier DR, West H, Harrysson O, et al. Characterization of thin walled Ti-6Al-4V components produced via electron beam melting. Solid Freeform Fabrication Proceedings. 2004:440-447.
- Schmitt S. Virtual diagnostics using cone beam CT. Dent Today. 2006;25:90-91.
Dr. Schmitt received his DDS degree from the University of Minnesota, School of Dentistry in 1975. He earned his specialty certificate in prosthodontics in 1982 from the Wilford Hall United States Air Force Medical Center, San Antonio, Tex, and his masters of science degree in prosthodontics from The University of Texas Health Science Center at Houston, Dental Branch. Prior to his retirement from the Air Force, Dr. Schmitt was chairman of the Department of Prosthodontics and program director for Graduate Prosthodontics at Wilford Hall USAF Medical Center. He also served as consultant to the USAF Surgeon General for prosthodontics. Dr. Schmitt has lectured throughout the United States and Europe and has published numerous articles in refereed journals. He is a Diplomat of the American Board of Prosthodontics, a Fellow of the American and International College of Prosthodontics, and President of Dental Implant Technologies. He can be reached at (210) 587-6857 or sschm11977@aol.com.
Dr. Harrysson is a member of the faculty in the Industrial Engineering Department at North Carolina State University, Raleigh, NC. He has been one of the leaders in the development of direct metal fabrication of implants and prosthetics and can be reached at (919) 513-0220 or harrysson@ncsu.edu.