Periodontal surgery is one of the most common treatment modalities for periodontal disease. The disease, which is the leading cause of tooth loss, occurs due to the reaction of the host to different bacterial antigens and results in the loss of periodontia. Preserving or improving this periodontia the supporting osseous level, ligament apparatus, cementum is the goal. Unfortunately, and commonly, post-surgical sensitivity can compromise this goal by allowing, during the healing phase, a newly established and unremoved nidus of bacteria to accumulate due to lack of proper hygiene, thus thwarting the purpose of periodontal surgery.
Periodontal surgery involves many different facets and techniques. Regenerative and cosmetic techniques are recent encouraging surgical modes of treatment. Other commonly used surgical techniques include crown lengthening, apically repositioned flaps, growing enamel, gingival grafts including root coverage as well as regenerating new keratinized tissue, and mucogingival flap surgery.1–11 All of these surgical procedures and techniques share a common goal of trying to restore the health of the periodontia, preventing further destruction of soft and hard tissue from localized bacteria and its effects, and aiding the patient’s ability to perform local hygienic methods to access and remove the initiating and offending bacteria, while achieving the best aesthetic result. No systemic method, such as a vaccine, has yet been made practical to eliminate periodontal disease, although one is envisioned for the future.
Periodontal surgery procedures also share a common postoperative side effect, that of sensitivity. Sensitivity is a common, unpleasant reaction to temperature change and touch. It may persist for varying periods of time and produce varying degrees of annoyance. It is frequently glossed over as a side effect, and surgical patients complaints may be ignored or overlooked. However, ignoring this postoperative side effect may have frustrating consequences for the practitioner, as this healing phase of the procedure is an integral step to achieving the goal of a healthy periodontia.
During the surgical phase, the practitioner achieves complete control of pain and sensation with local anesthetic and other analgesic aids. When the surgery is completed, sensation returns. A dressing is frequently utilized, but when it is removed, the surface is exposed. Sensitivity will frequently cause a postoperative patient to avoid cleaning the area of surgery during this healing phase. If the patient cannot adequately keep the area clean during this time, the offending bacteria may start to accumulate once again. Therefore, the healing phase must be carefully monitored for proper cleaning by the practitioner as well as the patient.
Since it is difficult for the dentist to keep the area clean in the critical time after surgery, the responsibility must shift to the patient. Initially, the area may be so sensitive to heat and cold, as well as to touch, that the patient is hesitant and may be reluctant to clean this area thoroughly, as he or she may be uncomfortable with the pain accompanying this phase. Confidence in the dentist may be compromised or strained at this juncture. Patients may resent the occurrence of postoperative sensitivity and blame the practitioner.
Another consequence of sensitivity is that the patient tends to avoid functional use of the surgical side, thus placing undue physiologic pressure on the opposite side. This may affect normal occlusal functioning. Sensitivity may also cause a patient to negatively alter his or her diet and therefore compromise proper nutritional intake, again, with a possible resultant negative effect on healing.
Until now there has been no consistent satisfactory application to compensate for this discomfort. Commercially available rinses that might have been recommended during this phase have drawbacks. They may or may not be effective, and some leave unsightly stains.
This article presents a case in which a new, fluoride-containing varnish was used to address the problem of postoperative sensitivity.
MATERIAL
Duraphat (Colgate Professional) is a viscous, varnish-type product that has been FDA-approved for treatment of dental sensitivity.12-15 The material appears to have the ability to greatly lessen or eliminate a patients immediate postsurgery sensitivity when applied during periodontal surgery.
Duraphat should be applied during the periodontal surgery phase, before the tissue is sutured into the desired position, and before the dressing is placed. Applying it in this manner has resulted in patients experiencing minimal postoperative sensitivity.
CASE PRESENTATION
A 55-year-old woman was referred for periodontal treatment as well as treatment planning and suggested sequential order of treatment. She knew that she had dental problems, but she wanted to look better at the same time. Her maxillary and mandibular left sides had previously been treated periodontally and prosthetically (full-coverage crowns). Her maxillary right side had not been retreated and would need new prosthetics as well, and teeth Nos. 2 to 6 had existing full-coverage crowns (in place for 20 years). There was class III and IV bone loss with periodontal pockets 5 to 7 mm in depth. She reported that the prior postoperative phase of periodontal treatment (maxillary and mandibular left side) had been very uncomfortable for her, and that she had experienced painful sensitivity after surgery was completed and the dressing removed. She was bothered so much by the temperature changes and the hypersensitivity to touch, especially when brushing her teeth, that she avoided appointments to take care of the maxillary right side for more than a year.
After team discussions with the restorative dentist, the patient, and myself, and proper sequential planning, the accepted course of treatment was periodontal surgery on the maxillary right side, including crown-lengthening techniques, to be followed prosthetically with new, full-coverage crowns replacing the existing crowns.
The periodontal surgical techniques included apically repositioned flaps as well as crown-lengthening techniques, designed to improve access to allow the patient to keep the area cleaner in the future and to allow the restorative dentist adequate access to solid tooth structure to perform correct prosthetic work. The periodontal disease had caused bone loss, thereby exposing a portion of the roots. There was no sensitivity before the surgical intervention because the diseased tissue of the periodontal pockets still surrounded the exposed roots. The roots were not clinically visible. Therefore, the diseased tissue was preventing sensitive stimulation of the root. After successful treatment, her roots would still be visibly and unaesthetically exposed until tissue maturation. The possibility of sensitivity was a significant issue. She had a positive attitude about waiting until the crowns could be placed at the proper time, but was apprehensive because of the uncomfortable postoperative period from her previous experience.
 |
 |
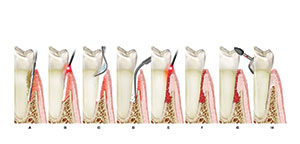
| Figure 1. Illustration showing the maxillary right quadrant with an adequate zone of pinkish-white keratinized gingival demarcated from the bluish-purple-colored alveolar mucosa by the mucogingival junction. Note the depth of the periodontal probe denoting the perio-pocket. | Figure 2. Mucogingival flap reflected revealing the exposed roots, alveolar bone present, and the relationship of exposed roots to the CEJ and enamel. |
 |
|
Figure 3. The orange-yellow-colored Duraphat covers the exposed roots and crest of the alveolar bone. |
Figures 1 and 2 illustrate what we were to do and how we prevented her postoperative sensitivity. Figure 3 illustrates the Duraphat being placed in the appropriate area. It is applied to the desired level by painting on the orange-colored paste, which is adherent even in a moist environment, prior to suturing the tissue. Duraphat adheres to the area of the tooth where it is easily applied with the supplied disposable brush.
Duraphat is derived from several rosins. It contains a shellac mastic and colophonium, which impact stickiness, and saliva does not interfere with its placement. This product is an alcohol-based ethanol. As the alcohol evaporates, the sticky rosins adhere to the surface. It forms a coating on the surface, and the dentinal tubules are blocked. Similar to the theoretical action of sodium fluoride clogging the open tubules with calcium fluoride, Duraphat has an immediate effect by coating the surface, and a longer-lasting clogging effect.
 |
 |
| Figure 4. Previously reflected mucogingival flap now sutured in the apically repositioned level covering the bone, while Duraphat is still covering the exposed roots as well as under the flap. | Figure 5. The buccal view of the maxillary right posterior area Nos. 2 to 6 with temporaries. |
 |
 |
| Figure 6. The palatal aspect of the same area. Notice the adequate zone of keratinized epithelium. | Figure 7. Occlusal aspect showing the temporaries removed, illustrating an inadequate amount of tooth structure to place correct restorations. |
 |
 |
| Figure 8. Palatal view of the palatal mucogingival flap revealing the recession of the roots and the amount of bone loss due to the perio disease. | Figure 9. Buccal aspect of the upper right area showing the osseous level with the exposed root. |
 |
 |
| Figure 10. Buccal view showing the osseous level, exposing the root, now covered with Duraphat. | Figure 11. Buccal view showing the apically repositioned flap sutured at the appropriately chosen level covering the osseous level, exposing the root, now covered with Duraphat as well. |
The maxillary right posterior teeth from Nos. 2 to 6, which had existing full-coverage crowns, were now provided with temporary crowns. The patient had acknowledged the need for new crowns. She also was informed that after the periodontal surgery, the gingiva would be a different height, and there would be visual exposure of the roots. Figure 5 shows a buccal view and Figure 6 the palatal view of the temporary crowns in place. There is an adequate zone of keratinized gingiva, but it was unattached (periodontal probing showed pockets of 5 to 7 mm in the area). The need for crown-lengthening surgery plus pocket removal with an apically repositioned flap technique appears necessary in Figure 7, even from an occlusal aspect. Figures 8 and 9 show the buccal and palatal reflected mucogingival flaps, denoting the effects of the disease in the extensive exposure of the roots as well as the obvious bone loss. The accretions were removed, the roots were planed, and the bone treated before the Duraphat was painted on the appropriate areas (Figure 10). The tissue was then sutured to the appropriate level to cover the osseous crest, thus exposing the roots visually (Figure 11). Gauze pads were used to compress the buccal and palatal aspects of the wound site briefly after suturing. Then a periodontal dressing (COE-PAK Automix NDS [GC America]) was placed on the area for a 1-week period. Prescriptions for an antibiotic and an analgesic had previously been given to the patient, so she had them at the time of surgery. Instructions on the use of the prescribed medication were reviewed once again.
One week later the dressing and sutures were removed, and the mouth was lavaged. There was no sensitivity or discomfort, and the oral hygiene instructions were reviewed and demonstrationed once again. If desired, the Duraphat can be applied again at this point. However, this should be done only if necessary, and in this case it was not needed.
 |
 |
| Figure 12. The upper right, healed properly with the keratinized epithelium now attached gingivally and the roots able to be maintained with good hygiene and no sensitivity. |
Figure 13. The palatal view of the same. |
 |
 |
| Figures 14 and 15. The completed restorative prosthetics of full-coverage from the buccal and palatal views. |
Eight weeks later the tissue had matured, allowing the patient to maintain her oral hygiene and thus protect the future health of the area. The roots, although visually exposed, caused no sensitivity or discomfort to the patient. Figures 12 and 13 show the buccal and palatal aspect of the healed area with the temporaries still present. The extent of the periodontal pocket depth and bone loss can be visualized. The final prostheses in place can be seen in Figures 14 and 15.
SUMMARY AND CONCLUSIONS
Responding to the patients uncomfortable reaction following certain periodontal surgery procedures, notably the sensitivity to temperature and touch, has been a source of frustration to both the practitioner performing the surgery as well as the patient. This case demonstrates the placement of an easily applied desensitizing paste (Duraphat) at the time of surgery, which enables the patient to avoid uncomfortable sensitivity after the dressing has been removed and allows the patient to return to good oral hygiene practices quickly, thereby avoiding new accumulation of bacteria. It also prevents further periodontal destruction, which is the purpose of the periodontal treatment.
This presentation and diagrammatic explanation demonstrate placing this topical paste during the surgery, just before suturing. This particular paste is easy to place, and ease of placement is not inhibited by moisture in the affected area. The desensitizing effect for the immediate postoperative period provides comfort for the patient and helps to maintain trust between the dentist and the patient.
Acknowledgment
The author would like to thank J. Ziezel, E. Burger, and Dr. T. Volpe in the preparation of this article.
References
1. Nabors CL. Repositioning the attached gingiva. J Periodontol. 1954;25:38-39.
2. Grupe HE, Warren RF Jr. Repair of gingival defects by a sliding flap operation. J Periodontol. 1956;27:92-95.
3. Friedman N. Mucogingival surgery. Tex Dent J. 1957;75:358-362.
4. Ariaudo AA, Tyrrell HA. Repositioning and increasing the zone of attached gingiva. J Periodontol. 1957;28:106-110.
5. Lang NP, Loe H. The relationship between the width of keratinized gingiva and gingival health. J Periodontol. 1972;43:623-627.
6. Hoexter DL. Surgical techniques for a winning smile. Dent Today. Jun 1994;13:46-49.
7. Staffileno H. Palatal flap surgery: mucosal flap (split thickness) and its advantages over the mucoperiosteal flap. J Periodontol. 1969;40:547-552.
8. Hoexter D. Growing enamel. Dent Today. Dec 1995;14:56-57.
9. Lindhe J, Nyman S. Alterations of the position of the marginal soft tissue following periodontal surgery. J Clin Periodontol. 1980;7:525-530.
10. Carnio J, Miller PD Jr. Increasing the amount of attached gingiva using a modified apically repositioned flap. J Periodontol. 1999;70:1110-1117.
11. Hoexter DL. Cosmetic periodontal surgery, part 2: using a variations of gingival graft techniques. Dent Today. Nov 1999;18:110-115.
12. Clark DC, Hanley JA, Geoghegan S, et al. The effectiveness of a fluoride varnish and a desensitizing toothpaste in treating dentinal hypersensitivity. J Periodontal Res. 1985;20:212-219.
13. Clark RE, Papas AS. Duraphat vs. Extra Strength Aim in treating dentinal hypersensitivity. J Dent Res. 1992;71(special issue):628.
14. Papas AS, Clark RE. Accrued desensitization with repeated Duraphat treatment of dentinal hypersensitivity. J Dent Res. 1995;74, 74, 134.
15. Gaffar A. Treating hypersensitivity with fluoride varnishes. Compend Contin Educ Dent. 1998;19:1088-1097.
Dr. Hoexter is director of the International Academy of Dental Facial Esthetics and is clinical professor of periodontics at Temple University. He received his degree from Tufts University, where he was also an adjunct professor of periodontics. He is a diplomate (implantology) of the ICOI, the American Society of Osseointegration, and the American Board of Esthetic Dentistry. Dr. Hoexter has lectured and published nationally/internationally and has been awarded 11 fellowships. He is in a private practice limited to periodontics, implants, and aesthetics in New York City, and can be reached at (212) 355-0004 or drdavidlh@aol.com.